Ats-Brief-1.Pdf (154.3Кб)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Methylphenidate Hydrochloride
Application for Inclusion to the 22nd Expert Committee on the Selection and Use of Essential Medicines: METHYLPHENIDATE HYDROCHLORIDE December 7, 2018 Submitted by: Patricia Moscibrodzki, M.P.H., and Craig L. Katz, M.D. The Icahn School of Medicine at Mount Sinai Graduate Program in Public Health New York NY, United States Contact: [email protected] TABLE OF CONTENTS Page 3 Summary Statement Page 4 Focal Point Person in WHO Page 5 Name of Organizations Consulted Page 6 International Nonproprietary Name Page 7 Formulations Proposed for Inclusion Page 8 International Availability Page 10 Listing Requested Page 11 Public Health Relevance Page 13 Treatment Details Page 19 Comparative Effectiveness Page 29 Comparative Safety Page 41 Comparative Cost and Cost-Effectiveness Page 45 Regulatory Status Page 48 Pharmacoepial Standards Page 49 Text for the WHO Model Formulary Page 52 References Page 61 Appendix – Letters of Support 2 1. Summary Statement of the Proposal for Inclusion of Methylphenidate Methylphenidate (MPH), a central nervous system (CNS) stimulant, of the phenethylamine class, is proposed for inclusion in the WHO Model List of Essential Medications (EML) & the Model List of Essential Medications for Children (EMLc) for treatment of Attention-Deficit/Hyperactivity Disorder (ADHD) under ICD-11, 6C9Z mental, behavioral or neurodevelopmental disorder, disruptive behavior or dissocial disorders. To date, the list of essential medications does not include stimulants, which play a critical role in the treatment of psychotic disorders. Methylphenidate is proposed for inclusion on the complimentary list for both children and adults. This application provides a systematic review of the use, efficacy, safety, availability, and cost-effectiveness of methylphenidate compared with other stimulant (first-line) and non-stimulant (second-line) medications. -

Substance Abuse and Dependence
9 Substance Abuse and Dependence CHAPTER CHAPTER OUTLINE CLASSIFICATION OF SUBSTANCE-RELATED THEORETICAL PERSPECTIVES 310–316 Residential Approaches DISORDERS 291–296 Biological Perspectives Psychodynamic Approaches Substance Abuse and Dependence Learning Perspectives Behavioral Approaches Addiction and Other Forms of Compulsive Cognitive Perspectives Relapse-Prevention Training Behavior Psychodynamic Perspectives SUMMING UP 325–326 Racial and Ethnic Differences in Substance Sociocultural Perspectives Use Disorders TREATMENT OF SUBSTANCE ABUSE Pathways to Drug Dependence AND DEPENDENCE 316–325 DRUGS OF ABUSE 296–310 Biological Approaches Depressants Culturally Sensitive Treatment Stimulants of Alcoholism Hallucinogens Nonprofessional Support Groups TRUTH or FICTION T❑ F❑ Heroin accounts for more deaths “Nothing and Nobody Comes Before than any other drug. (p. 291) T❑ F❑ You cannot be psychologically My Coke” dependent on a drug without also being She had just caught me with cocaine again after I had managed to convince her that physically dependent on it. (p. 295) I hadn’t used in over a month. Of course I had been tooting (snorting) almost every T❑ F❑ More teenagers and young adults die day, but I had managed to cover my tracks a little better than usual. So she said to from alcohol-related motor vehicle accidents me that I was going to have to make a choice—either cocaine or her. Before she than from any other cause. (p. 297) finished the sentence, I knew what was coming, so I told her to think carefully about what she was going to say. It was clear to me that there wasn’t a choice. I love my T❑ F❑ It is safe to let someone who has wife, but I’m not going to choose anything over cocaine. -

XANAX® Alprazolam Tablets, USP
XANAX® alprazolam tablets, USP CIV WARNING: RISKS FROM CONCOMITANT USE WITH OPIOIDS Concomitant use of benzodiazepines and opioids may result in profound sedation, respiratory depression, coma, and death [see Warnings, Drug Interactions]. Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Follow patients for signs and symptoms of respiratory depression and sedation. DESCRIPTION XANAX Tablets contain alprazolam which is a triazolo analog of the 1,4 benzodiazepine class of central nervous system-active compounds. The chemical name of alprazolam is 8-Chloro-1-methyl-6-phenyl-4H-s-triazolo [4,3-α] [1,4] benzodiazepine. The structural formula is represented to the right: Alprazolam is a white crystalline powder, which is soluble in methanol or ethanol but which has no appreciable solubility in water at physiological pH. Each XANAX Tablet, for oral administration, contains 0.25, 0.5, 1 or 2 mg of alprazolam. XANAX Tablets, 2 mg, are multi-scored and may be divided as shown below: 1 Reference ID: 4029640 Inactive ingredients: Cellulose, corn starch, docusate sodium, lactose, magnesium stearate, silicon dioxide and sodium benzoate. In addition, the 0.5 mg tablet contains FD&C Yellow No. 6 and the 1 mg tablet contains FD&C Blue No. 2. CLINICAL PHARMACOLOGY Pharmacodynamics CNS agents of the 1,4 benzodiazepine class presumably exert their effects by binding at stereo specific receptors at several sites within the central nervous system. Their exact mechanism of action is unknown. Clinically, all benzodiazepines cause a dose-related central nervous system depressant activity varying from mild impairment of task performance to hypnosis. -

Meth/Amphetamine Use and Associated HIV: Implications for Global Policy and Public Health
International Journal of Drug Policy 21 (2010) 347–358 Contents lists available at ScienceDirect International Journal of Drug Policy journal homepage: www.elsevier.com/locate/drugpo Review Meth/amphetamine use and associated HIV: Implications for global policy and public health Louisa Degenhardt ∗,1, Bradley Mathers 2, Mauro Guarinieri 3, Samiran Panda 4, Benjamin Phillips 5, Steffanie A. Strathdee 6, Mark Tyndall 7, Lucas Wiessing 8, Alex Wodak 9, John Howard 10, the Reference Group to the United Nations on HIV and injecting drug use National Drug and Alcohol Research Centre, University of New South Wales, Sydney, NSW 2052, Australia article info abstract Article history: Amphetamine type stimulants (ATS) have become the focus of increasing attention worldwide. There are Received 29 May 2009 understandable concerns over potential harms including the transmission of HIV. However, there have Received in revised form 30 October 2009 been no previous global reviews of the extent to which these drugs are injected or levels of HIV among Accepted 24 November 2009 users. A comprehensive search of the international peer-reviewed and grey literature was undertaken. Multiple electronic databases were searched and documents and datasets were provided by UN agencies and key experts from around the world in response to requests for information on the epidemiology of use. Keywords: Amphetamine or methamphetamine (meth/amphetamine, M/A) use was documented in 110 countries, Methamphetamine Amphetamine and injection in 60 of those. Use may be more prevalent in East and South East Asia, North America, South HIV Africa, New Zealand, Australia and a number of European countries. In countries where the crystalline Injecting form is available, evidence suggests users are more likely to smoke or inject the drug; in such countries, Epidemiology higher levels of dependence may be occurring. -

Evidence-Based Guidelines for the Pharmacological Management of Substance Abuse, Harmful Use, Addictio
444324 JOP0010.1177/0269881112444324Lingford-Hughes et al.Journal of Psychopharmacology 2012 BAP Guidelines BAP updated guidelines: evidence-based guidelines for the pharmacological management of substance abuse, Journal of Psychopharmacology 0(0) 1 –54 harmful use, addiction and comorbidity: © The Author(s) 2012 Reprints and permission: sagepub.co.uk/journalsPermissions.nav recommendations from BAP DOI: 10.1177/0269881112444324 jop.sagepub.com AR Lingford-Hughes1, S Welch2, L Peters3 and DJ Nutt 1 With expert reviewers (in alphabetical order): Ball D, Buntwal N, Chick J, Crome I, Daly C, Dar K, Day E, Duka T, Finch E, Law F, Marshall EJ, Munafo M, Myles J, Porter S, Raistrick D, Reed LJ, Reid A, Sell L, Sinclair J, Tyrer P, West R, Williams T, Winstock A Abstract The British Association for Psychopharmacology guidelines for the treatment of substance abuse, harmful use, addiction and comorbidity with psychiatric disorders primarily focus on their pharmacological management. They are based explicitly on the available evidence and presented as recommendations to aid clinical decision making for practitioners alongside a detailed review of the evidence. A consensus meeting, involving experts in the treatment of these disorders, reviewed key areas and considered the strength of the evidence and clinical implications. The guidelines were drawn up after feedback from participants. The guidelines primarily cover the pharmacological management of withdrawal, short- and long-term substitution, maintenance of abstinence and prevention of complications, where appropriate, for substance abuse or harmful use or addiction as well management in pregnancy, comorbidity with psychiatric disorders and in younger and older people. Keywords Substance misuse, addiction, guidelines, pharmacotherapy, comorbidity Introduction guidelines (e.g. -

Randomized Controlled Trial of Dexamphetamine Maintenance for the Treatment of Methamphetamine
RESEARCH REPORT doi:10.1111/j.1360-0443.2009.02717.x Randomized controlled trial of dexamphetamine maintenance for the treatment of methamphetamine dependenceadd_2717 146..154 Marie Longo1, Wendy Wickes1, Matthew Smout1, Sonia Harrison1, Sharon Cahill1 & Jason M. White1,2 Pharmacotherapies Research Unit, Drug and Alcohol Services South Australia, Norwood, South Australia, Australia1 and Discipline of Pharmacology, University of Adelaide, Adelaide, South Australia, Australia2 ABSTRACT Aim To investigate the safety and efficacy of once-daily supervised oral administration of sustained-release dexam- phetamine in people dependent on methamphetamine. Design Randomized, double-blind, placebo-controlled trial. Participants Forty-nine methamphetamine-dependent drug users from Drug and Alcohol Services South Australia (DASSA) clinics. Intervention Participants were assigned randomly to receive up to 110 mg/day sustained- release dexamphetamine (n = 23) or placebo (n = 26) for a maximum of 12 weeks, with gradual reduction of the study medication over an additional 4 weeks. Medication was taken daily under pharmacist supervision. Measurements Primary outcome measures included treatment retention, measures of methamphetamine consump- tion (self-report and hair analysis), degree of methamphetamine dependence and severity of methamphetamine withdrawal. Hair samples were analysed for methamphetamine using liquid chromatography-mass spectrometry. Findings Treatment retention was significantly different between groups, with those who received dexamphetamine remaining in treatment for an average of 86.3 days compared with 48.6 days for those receiving placebo (P = 0.014). There were significant reductions in self-reported methamphetamine use between baseline and follow-up within each group (P < 0.0001), with a trend to a greater reduction among the dexamphetamine group (P = 0.086). -

Management of Acute Withdrawal and Detoxification for Adults Who Misuse Methamphetamine: a Review of the Clinical Evidence and Guidelines
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Management of Acute Withdrawal and Detoxification for Adults who Misuse Methamphetamine: A Review of the Clinical Evidence and Guidelines Service Line: Rapid Response Service Version: 1.0 Publication Date: February 08, 2019 Report Length: 28 Pages Authors: Michelle Clark, Robin Featherstone Cite As: Management of Acute Withdrawal and Detoxification for Adults who Misuse Methamphetamine: A Review of the Clinical Evidence and Guidelines. Ottawa: CADTH; 2019 Feb. (CADTH rapid response report: summary with critical appraisal). ISSN: 1922-8147 (online) Disclaimer: The information in this document is intended to help Canadian health care decision-makers, health care professionals, health systems leaders, and policy-makers make well-informed decisions and thereby improve the quality of health care services. While patients and others may access this document, the document is made available for informational purposes only and no representations or warranties are made with respect to its fitness for any particular purpose. The information in this document should not be used as a substitute for professional medical advice or as a substitute for the application of clinical judgment in respect of the care of a particular patient or other professional judgment in any decision-making process. The Canadian Agency for Drugs and Technologies in Health (CADTH) does not endorse any information, drugs, therapies, treatments, products, processes, or services. While care has been taken to ensure that the information prepared by CADTH in this document is accurate, complete, and up-to-date as at the applicable date the material was first published by CADTH, CADTH does not make any guarantees to that effect. -

Prescription Medications: Misuse, Abuse, Dependence, and Addiction
Substance Abuse Treatment May 2006 Volume 5 Issue 2 ADVISORYNews for the Treatment Field Prescription Medications: Misuse, Abuse, Dependence, and Addiction How serious are prescription Older adults are particularly vulnerable to misuse and medication use problems? abuse of prescription medications. Persons ages 65 and older make up only 13 percent of the population but Development and increased availability of prescription account for one-third of all medications prescribed,3 drugs have significantly improved treatment of pain, and many of these prescriptions are for psychoactive mental disorders, anxiety, and other conditions. Millions medications with high abuse and addiction liability.4 of Americans use prescription medications safely and Data from the National Survey on Drug Use and Health responsibly. However, increased availability and vari- indicate that nonmedical use of prescription medications ety of medications with psychoactive effects (see Table was the second most common form of substance abuse 1) have contributed to prescription misuse, abuse, among adults older than 55.5 dependence, and addiction. In 2004,1 the number of Americans reporting abuse2 of prescription medications Use of prescription medications in ways other than was higher than the combined total of those reporting prescribed can have a variety of adverse health conse- abuse of cocaine, hallucinogens, inhalants, and heroin. quences, including overdose, toxic reactions, and serious More than 14.5 million persons reported having used drug interactions leading to life-threatening conditions, prescription medications nonmedically within the past such as respiratory depression, hypertension or hypoten- year. Of this 14.5 million, more than 2 million were sion, seizures, cardiovascular collapse, and death.6 between ages 12 and 17. -

An Overview of Outpatient and Inpatient Detoxification
An Overview of Outpatient and Inpatient Detoxification Motoi Hayashida, M.D., Sc.D. lcohol detoxification can be defined as a period facility, where they reside for the duration of of medical treatment, usually including counsel- treatment, which may range from 5 to 14 days. A ing, during which a person is helped to overcome The process of detoxification in either setting initially physical and psychological dependence on alcohol (Chang involves the assessment and treatment of acute with- and Kosten 1997). The immediate objectives of alcohol drawal symptoms, which may range from mild (e.g., detoxification are to help the patient achieve a substance- tremor and insomnia) to severe (e.g., autonomic free state, relieve the immediate symptoms of withdrawal, hyperactivity, seizures, and delirium) (Swift 1997). and treat any comorbid medical or psychiatric conditions. Medications often are provided to help reduce a patient’s These objectives help prepare the patient for entry into withdrawal symptoms. Benzodiazepines (e.g., diazepam long-term treatment or rehabilitation, the ultimate goal of detoxification (Swift 1997). The objectives of long- and chlordiazepoxide) are the most commonly used term treatment or rehabilitation include the long-term drugs for this purpose, and their efficacy is well estab- maintenance of the alcohol-free state and the incor- lished (Swift 1997). Benzodiazepines not only reduce poration of psychological, family, and social interven- alcohol withdrawal symptoms but also prevent alcohol tions to help ensure its persistence (Swift 1997). withdrawal seizures, which occur in an estimated 1 to Alcohol detoxification can be completed safely and 4 percent of withdrawal patients (Schuckit 1995). -

Heterogeneity of Stimulant Dependence: a National Drug Abuse Treatment Clinical Trials Network Study
The American Journal on Addictions, 18: 206–218, 2009 Copyright C American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1080/10550490902787031 Heterogeneity of Stimulant Dependence: A National Drug Abuse Treatment Clinical Trials Network Study Li-Tzy Wu, ScD,1 Dan G. Blazer, MD, PhD,1 Ashwin A. Patkar, MD,1 Maxine L. Stitzer, PhD,2 Paul G. Wakim, PhD,3 Robert K. Brooner, PhD2 1Duke University School of Medicine, Department of Psychiatry and Behavioral Sciences, Duke Clinical Research Institute, Durham, North Carolina 2Johns Hopkins University School of Medicine, Department of Psychiatry and Behavioral Sciences, Baltimore, Maryland 3National Institute on Drug Abuse, Bethesda, Maryland We investigated the presence of DSM-IV subtyping for of disorders has noteworthy advantages because it facilitates dependence on cocaine and amphetamines (with versus with- research, improves communications among clinicians and out physical dependence) among outpatient stimulant users researchers, and serves as a necessary tool for collecting enrolled in a multisite study of the Clinical Trials Network 1 (CTN). Three mutually exclusive groups were identified: and communicating public health statistics. The categorical primary cocaine users (n = 287), primary amphetamine users classification, however, also constitutes a primary limitation (n = 99), and dual users (cocaine and amphetamines; n = because it works best when all members of a given diagnosis 29). Distinct subtypes were examined with latent class and are homogeneous and when there are clear boundaries between logistic regression procedures. Cocaine users were distinct distinct diagnoses.1 from amphetamine users in age and race/ethnicity. There were four distinct classes of primary cocaine users: non- DSM-IV acknowledges this limitation and further suggests dependence (15%), compulsive use (14%), tolerance and the presence of heterogeneity among individuals who share compulsive use (15%), and physiological dependence (toler- a diagnosis. -

Director's Report 2/00
Director's Report 2/00 National Institute on Drug Abuse Director's Report to the National Advisory Council on Drug Abuse February, 2000 Index Research Findings Basic Research Behavioral Research Treatment Research and Development Research on AIDS and Other Medical Consequences of Drug Abuse Epidemiology, Etiology and Prevention Research Services Research Intramural Research Program Activities Review Activities Congressional Affairs International Activities Meetings and Conferences Media and Education Activities Planned Meetings Publications Staff Highlights Grantee Honors [Office of Director] [First Report Section] https://archives.drugabuse.gov/DirReports/DirRep200/DirectorRepIndex.html[11/17/16, 9:37:32 PM] Director's Report 2/00 Archive Home | Accessibility | Privacy | FOIA (NIH) | Current NIDA Home Page The National Institute on Drug Abuse (NIDA) is part of the National Institutes of Health (NIH) , a component of the U.S. Department of Health and Human Services. Questions? _ See our Contact Information. https://archives.drugabuse.gov/DirReports/DirRep200/DirectorRepIndex.html[11/17/16, 9:37:32 PM] Director's Report 2/00 - Basic Research National Institute on Drug Abuse Director's Report to the National Advisory Council on Drug Abuse February, 2000 Research Findings Basic Research A Brain Protein Is Involved in Switching On Cocaine Addiction Chronic exposure to cocaine causes the delta-FosB transcription factor to be expressed persistently in the nucleus accumbens. Thus, researchers hypothesized that delta-FosB may mediate some of the long-lived increases in sensitivity to the stimulant and rewarding effects of cocaine. Dr. Eric Nestler of Yale University and his colleagues tested whether delta-FosB expression actually increased the responsiveness to cocaine by generating genetically altered mice that produced large quantities of delta-FosB in the nucleus accumbens. -
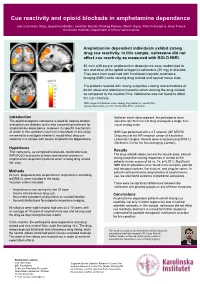
Cue Reactivity and Opioid Blockade in Amphetamine Dependence
Cue reactivity and opioid blockade in amphetamine dependence Joar Guterstam, Nitya Jayaram-Lindström, Jonathan Berrebi, Predrag Petrovic, Martin Ingvar, Peter Fransson & Johan Franck Karolinska Institutet, Department of clinical neuroscience Amphetamine dependent individuals exhibit strong drug cue reactivity. In this sample, naltrexone did not affect cue reactivity as measured with BOLD fMRI. 40 men with severe amphetamine dependence were randomized to one oral dose of the opioid antagonist naltrexone (50 mg) or placebo. They were then examined with functional magnetic resonance imaging (fMRI) while viewing drug related and neutral movie clips. The patients reacted with strong subjective craving and activations of limbic areas and attentional networks when viewing the drug related, as compared to the neutral, films. Naltrexone was not found to affect the cue reactivity. fMRI image of activations when viewing drug related vs. neutral films (whole-brain results, p<0.05, Family-Wise Error corrected). Introduction Between each video segment, the participants were The opioid antagonist naltrexone is used for treating alcohol asked to rate their level of drug craving on a single item and opioid use disorder, but is also a promising treatment for visual analog scale. amphetamine dependence. However, its specific mechanism of action in this condition is not well understood. In this study, fMRI was performed with a 3 T scanner (GE MR750 we aimed to investigate whether it would affect drug cue Discovery) at the MR research center of Karolinska reactivity in a sample with severe amphetamine dependence. University Hospital. Results were analyzed using SPM 12 (Wellcome Center for Neuroimaging, London). Hypothesis That naltrexone, as compared to placebo, would attenuate Results fMRI BOLD activations of brain motivational systems in The drug-related videos, but not the neutral ones, elicited amphetamine dependent patients when viewing drug related strong subjective craving responses in almost all the film clips.