Lumbar Sympathetic Block 57 Sascha Qian, Vikram Sengupta, Ned Urbiztondo, and Nameer Haider
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Impact of Celiac Neurolysis on Survival in Patients with Pancreatic Cancer
ORIGINAL ARTICLE: Clinical Endoscopy Impact of celiac neurolysis on survival in patients with pancreatic cancer Larissa L. Fujii-Lau, MD,1 William R. Bamlet, MD,2 Jason S. Eldrige, MD,3 Suresh T. Chari, MD,1 Ferga C. Gleeson, MD,1 Barham K. Abu Dayyeh, MD,1 Jonathan E. Clain, MD,1 Randall K. Pearson, MD,1 Bret T. Petersen, MD,1 Elizabeth Rajan, MD,1 Mark D. Topazian, MD,1 Santhi S. Vege, MD,1 Kenneth K. Wang, MD,1 Maurits J. Wiersema, MD,4 Michael J. Levy, MD1 Rochester, Minnesota; Fort Wayne, Indiana, USA Background: Pancreatic cancer (PC) often produces pain that is difficult to control. Celiac neurolysis (CN) is performed with the goal of improving pain control and quality of life while reducing opioid-related side effects. Objective: We aimed to evaluate whether CN provides a survival advantage for PC patients. Design: Retrospective case-control study. Setting: Single tertiary-care referral center. Patients: Review of a prospectively maintained database identified patients with unresectable PC who underwent CN over a 12-year period. Each patient was matched to 2 control patients with unresectable PC. Intervention: CN, which included both celiac plexus neurolysis (CPN) and celiac ganglia neurolysis (CGN). Main Outcome Measurements: Median survival in Kaplan-Meier curves and hazard ratios. Results: A total of 417 patients underwent CN and were compared with 840 controls with PC. Baseline charac- teristics were similar except the CN group had greater weight loss and pain requiring opioids. A mean of 16.6 Æ 5.8 mL of alcohol was administered. For patients who underwent CN, the median survival from the time of presentation was shorter compared with controls (193 vs 246 days; hazard ratio 1.32; 95% confidence interval, 1.13-1.54). -

EUS-Guided Versus Percutaneous Celiac Neurolysis for the Management of Intractable Pain Due to Unresectable Pancreatic Cancer: a Randomized Clinical Trial
Journal of Clinical Medicine Article EUS-Guided Versus Percutaneous Celiac Neurolysis for the Management of Intractable Pain Due to Unresectable Pancreatic Cancer: A Randomized Clinical Trial 1, 2, , 3, 4 5 Won Jae Yoon y, Yul Oh y z, Changhoon Yoo y , Sunguk Jang , Seong-Sik Cho , 2,§ 2, , 6, , Jeong-Hun Suh , Seong-Soo Choi * k and Do Hyun Park * k 1 Department of Internal Medicine, College of Medicine, Ewha Womans University, Seoul 07804, Korea; [email protected] 2 Department of Anesthesiology and Pain Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul 05505, Korea; [email protected] (Y.O.); [email protected] (J.-H.S.) 3 Department of Oncology, Asan Medical Center, University of Ulsan College of Medicine, Seoul 05505, Korea; [email protected] 4 Department of Gastroenterology and Hepatology, Cleveland Clinic, Cleveland, OH 44195, USA; [email protected] 5 Department of Occupational and Environmental Medicine, College of Medicine, Dong-A University, Busan 49201, Korea; [email protected] 6 Division of Gastroenterology, Department of Internal Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul 05505, Korea * Correspondence: [email protected] (S.-S.C.); [email protected] (D.H.P.) Yoon, Oh, and Yoo contributed equally to this paper. y This author is now with the Namyangju Baek Hospital, Namyangju-si, Korea. z § This author is now with the Seoulnanum Pain Clinic, Jeju-si, Korea. Park and Choi contributed equally to this paper as corresponding authors. k Received: 26 April 2020; Accepted: 28 May 2020; Published: 1 June 2020 Abstract: Although endoscopic ultrasound-guided celiac neurolysis (EUS-CN) and percutaneous celiac neurolysis (PCN) are utilized to manage intractable pain in pancreatic cancer patients, no direct comparison has been made between the two methods. -

Radiofrequency Ablation and Alcohol Neurolysis of the Splanchnic Nerves for a Patient with Abdominal Pain from Pancreatic Cancer
Open Access Case Report DOI: 10.7759/cureus.10758 Radiofrequency Ablation and Alcohol Neurolysis of the Splanchnic Nerves for a Patient With Abdominal Pain From Pancreatic Cancer Rana AL-Jumah 1 , Ivan Urits 2 , Omar Viswanath 3 , Alan D. Kaye 4 , Jamal Hasoon 2 1. Department of Anesthesia, Baylor College of Medicine, Houston, USA 2. Department of Anesthesia, Critical Care and Pain Medicine, Beth Israel Deaconess Medical Center – Harvard Medical School, Boston, USA 3. Pain Management, Valley Pain Consultants, Envision Physician Services, Phoenix, USA 4. Anesthesiology, Louisiana State University Health Sciences Center, Shreveport, USA Corresponding author: Jamal Hasoon, [email protected] Abstract Abdominal pain related to gastrointestinal malignancy can be notoriously difficult to manage and can lead to significant morbidity and suffering. The blockade of the celiac plexus has traditionally been performed for alleviating abdominal pain related to malignancy. Visceral structures that are innervated by these nerves include the pancreas, liver, gallbladder, mesentery, omentum, and the gastrointestinal tract from the stomach to the transverse colon. Alternatively, this pain can be treated by disrupting visceral nociceptive signals at the splanchnic nerves. In this report, we describe our experience of treating a 50-year-old male patient suffering from severe abdominal pain related to pancreatic cancer with multiple liver metastases. The patient failed medication management and had an international normalized ratio of 1.6, which was a concern for performing a celiac plexus block given the proximity of major vascular structures. The patient instead underwent radiofrequency ablation (RFA) as well as alcohol neurolysis of the bilateral splanchnic nerves and obtained significant relief from the procedure. -

Family Medicine Clinical Rotations 2012 Session Objectives
Slide 1 UVM ECHO -- Chronic Pain Facilitators: Faculty: • Mark Pasanen, MD • Patti Fisher, MD • Liz Cote • Amanda Kennedy, PharmD • Charles MacLean, MD • Sanchit Maruti, MD • Rich Pinckney, MD, MPH • Carlos Pino, MD • Jill Warrington, MD Slide 2 Introduction to ZOOM • Mute microphone when not speaking • If using phone for audio, please mute computer • If using phone,*6 is used to mute/unmute • Position webcam effectively (and please enable video) • Test both audio & video • Use “chat” function for: • Attendance—type name and organization of each participant upon entry to each teleECHO session • Technical issues • We need your input! • Use “raise hand” feature; the ECHO team will call on you • Please speak clearly Slide 3 No Relevant Disclosures Faculty: Planners: • Mark Pasanen, MD • Elizabeth Cote • Charles MacLean, MD • Joan Devine, BSN, RN • Carlos Pino, MD • Sarah Morgan, MD, Medical • Patricia Fisher, MD Director Planner • Richard Pinckney, MD • Mark Pasanen, MD • Amanda Kennedy, PharmD • Charles MacLean, MD • Sanchit Maruti, MD • Jill Warrington, MD, PhD Slide 4 CME Disclosures Northern Vermont Area Health Education Center (AHEC) is approved as a provider of Continuing Medical Education (CME) by the New Hampshire Medical Society, accredited by the ACCME. Northern Vermont AHEC designates this educational activity for a maximum of 1.5 Category 1 Credits toward the AMA Physician’s Recognition Award. Interest Disclosures: • As an organization accredited by the ACCME to sponsor continuing medical education activities, Northern VT AHEC is required to disclose any real or apparent conflicts of interest (COI) that any speakers may have related to the content of their presentations. Slide 5 • RECORDING OF SESSION TO BEGIN Slide 6 Interventional Pain Medicine Carlos A. -
Celiac Plexus Neurolysis
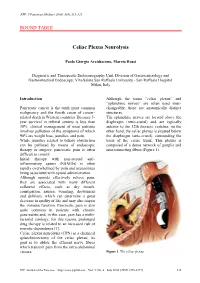
JOP. J Pancreas (Online) 2004; 5(4):315-321. ROUND TABLE Celiac Plexus Neurolysis Paolo Giorgio Arcidiacono, Marzia Rossi Diagnostic and Therapeutic Endosonography Unit, Division of Gastroenterology and Gastrointestinal Endoscopy, Vita-Salute San Raffaele University - San Raffaele Hospital. Milan, Italy Introduction Although the terms “celiac plexus” and “splanchnic nerves” are often used inter- Pancreatic cancer is the tenth most common changeably, these are anatomically distinct malignancy and the fourth cause of cancer- structures. related death in Western countries. Because 5- The splanchnic nerves are located above the year survival in referral centers is less than diaphragm (retro-crural) and are typically 30%, clinical management of most patients anterior to the 12th thoracic vertebra; on the involves palliation of the symptoms of which other hand, the celiac plexus is situated below 90% are weight loss, jaundice, and pain. the diaphragm (ante-crural), surrounding the While jaundice related to biliary obstruction basis of the celiac trunk. This plexus is can be palliated by means of endoscopic composed of a dense network of ganglia and therapy or surgery, pancreatic pain is often interconnecting fibres (Figure 1). difficult to control. Initial therapy with non-steroid anti- inflammatory agents (NSAIDs) is often rapidly overwhelmed by pain and necessitates being associated with opioid administration. Although opioids effectively relieve pain, they are associated with many different collateral effects, such as dry mouth, constipation, nausea, vomiting, drowsiness and delirium, which can determine a great decrease in quality of life and may also impair the immune function. Pancreatic pain is also quite common in patients with chronic pancreatitis and, in this case, pain has a multi- factorial etiology; for this reason, prolonged drug therapy is related to an increased risk of narcotic-dependence [1]. -

Celiac Plexus Nerve Neurolysis
Celiac Plexus Nerve Block/Neurolysis What is a celiac plexus block? Celiac plexus blocks are injections of pain medication that help relieve abdominal pain, commonly due to cancer or chronic pancreatitis. The celiac plexus is a bundle of nerves that surrounds the aorta, the main artery into your abdomen. Blocking these nerves from carrying pain information can help you stop feeling pain in your abdomen. How is a celiac plexus block done? First, you’ll be given an intravenous medication to relax you. Then, you’ll lie on your stomach on an x-ray table. The doctor will numb an area of skin on your back with a local anesthetic. Then, guided by an x-ray, he or she will: • Insert a thin needle into your back, next to your spine, and inject anesthetic • Insert a second needle on the other side of your spine • Inject dye to confirm that medication will go to the correct spot • Inject pain medication, such as epinephrine, clonidine or steroid; alcohol or phenol also may be injected to destroy the nerves Usually, the procedure takes less than 30 minutes, and you can go home the same day. How effective is a celiac plexus block? How long the pain relief lasts might be different for each person. For some, celiac plexus blocks can relieve pain for weeks. For others, the relief can last years. Many can return to their normal activities. Usually people need a series of injections to continue the pain relief. Sometimes it takes only two injections; sometimes it takes more than 10. -

Chemical Neurolysis and Radiofrequency Ablation of Lumbar
Novel Approaches in Regional Anesthesia & Pain Management Chapter 4 Chemical Neurolysis and Radiofrequency Ablation of Lumbar Sympathetic Ganglion in Peripheral Vascular Diseases of the Lower Limbs Kalpana Kulkarni*; Rajendra Kulkarni D Y Patil Medical College, Kolhapur MH INDIA *Correspondence to: Kalpana Kulkarni, D Y Patil Medical College, Kolhapur MH INDIA Phone: 9822065665; Email: [email protected] Abstract Peripheral vascular diseases (PVD) with impaired circulation is prevalent in 40-60% of Asian population. The resulting ischemic manifestations are cold lower extremities, claudication, discoloration, nonhealing ulcer/ gangrene of toes. Risk factors are atherosclerosis, hypertension, scleroderma, diabetes, dyslipidemia and thromboembolism or it may be associated with chronic regional pain syndrome (CRPS). Thromboangitis- obliterans (TAO) or Berger’s disease affects very young/ adult smokers. On Doppler ultrasonography, there is reduced/absent flow in peripheral arterial system usually in iliofemoral, popliteal, tibialis posterior and dorsalis Pedi’s artery in patients with ischemic lower limb. Major presenting symptoms are moderate to severe pain in the limbs, affection of sleep and significant work disability. Over last 5-6 decades, lumbar sympathetic ganglion block (LSGB) has become a technique of choice over complex surgical sympathectomy in managing ischemic limb ulcers. Chemical neurolysis of lumbar sympathetic ganglion using alcohol or phenol is a well-established method for prolonged effects especially in patients with limb ulcers. Currently radiofrequency (RF) ablation of lumbar sympathetic ganglion (LSG) is considered to be safe Novel Approaches in Regional Anesthesia & Pain Management and effective option but have concerns of high cost and availability. This review is supported by information’s obtained from current literature search in PubMed, Science Direct and Google for similar research work. -

Neuropathic Pain in Pancreatic Cancer: an Update of the Last Five Years
Review Neuropathic Pain in Pancreatic Cancer: An Update of the Last Five Years Raffaele Pezzilli Potenza County Medical Association, 85100 Potenza, Italy; [email protected] or [email protected]; Tel.: +39-09711564229 Abstract: Pain is the main symptom of pancreatic cancer (pancreatic ductal adenocarcinoma, PDAC). Pain in pancreatic cancer may be visceral, somatic or neuropathic in origin. Pain is produced by tissue damage, inflammation, ductal obstruction and infiltration. Visceral nociceptive signals caused by damage to the upper abdominal viscera are carried along sympathetic fibers, which travel to the celiac plexus nerves and ganglia, which are found at the T12-L2 vertebral levels, anterolateral to the aorta near the celiac trunk. From here, the signals are transmitted through the splanchnic nerves to the T5-T12 dorsal root ganglia and then on to the higher centers of the central nervous system. Somatic and neuropathic pain may arise from tumor extension into the surrounding peritoneum, retroperitoneum and bones and, in the latter case, into the nerves, such as the lumbosacral plexus. It should also be noted that other types of pain might arise because of therapeutic interventions, such as post-chemoradiation syndromes, which cause mucositis and enteritis. Management with non-steroidal anti-inflammatory agents and narcotics was the mainstay of therapy. In recent years, celiac plexus blocks and neurolysis, as well as intrathecal therapies have been used to control severe pain, at times resulting in a decreased need for drugs, avoiding their unwanted side effects. Pain may impair the patient’s quality of life, negatively affecting patient outcome and resulting in increased psychological stress. -

Epidural Alcohol Neurolysis–A Good Option for Cancer Pain Management in Developing Countries
Journal of Anesthesia & Critical Care: Open Access Research Article Open Access Epidural Alcohol Neurolysis–A Good Option for Cancer Pain Management in Developing Countries Volume 6 Issue 5 - 2016 Krishna Poddar,1 Sumanta Dasgupta,2 Rachit Background Gulati3 20 million new cancer cases are reported every year. Up to 73% 1Director, Kolkata Pain Clinic and In-charge Pain and Palliative of patients are in pain at the time of diagnosis. The goal of cancer Care, Central Hospital SE Railways, India 2Chief Specialist and Head of the department, Anaesthesiology treatment is generally pain reduction and functional recovery to and Critical Care Central Hospital SE Railways, India optimize the quality of life (QOL). Inadequate pain relief from systemic 3Post Graduate Trainee, Department of Physical Medicine and medications is common in patients with an advanced malignancy.1 Rehabilitation, India As many as 43% of patients with malignancies do not experience adequate pain relief from systemic medications, in those patients, Correspondence: Krishna Poddar, Director, Kolkata Pain Clinic and In-charge Pain and Palliative Care, Central Hospital the systemic opioid dose must be increased in order to control the SE Railways, India, Tel 9830048445, 2 pain. However, increase in the systemic opioid dose causes serious Email adverse effects. Nerve block or neurolysis as interventional approach can be an effective treatment option for patients experiencing dose Received: November 29, 2016 | Published: December 30, 2016 limiting adverse effects of opioids.3 The role of neurolytic blocks in the management of any type of cancer pain has not been firmly established by randomized, blinded clinical trials. Neurolytic Blocks had been extensively used in the early part of the 20th century for cancer pain management. -

Coeliac Plexus Neurolysis for Upper Abdominal Malignancies Using an Anterior Approach: Review of the Literature
Southern Afr Africanican Journal Journal of Anaesthesia of Anaesthesia and Analgesia and Analgesia 2015; 21(3):6-16 2015; 1(1):1–11 http://dx.doi.org/10.1080/22201181.2015.1056501 SouthSouth Afr Afr J J Anaesth Anaesth Analg Analg ISSNISSN 2220-1181 2220-1181 EISSNEISSN 2220-1173 2220-1173 Open Access Access article article distributed distributed under under the terms the of terms the of the © 2015© 2015 The The Author(s) Author(s) Creative Commons Commons License License [CC BY-NC-ND [CC BY-NC-ND 4.0] 4.0] http://creativecommons.org/licenses/by-nc-nd/4.0 RESEARCH Coeliac plexus neurolysis for upper abdominal malignancies using an anterior approach: review of the literature Anju Ghaia*, Hamesh Kumara and Sarthak Wadherab a Department of Anaesthesiology, Pain and Intensive Care, Pt BDS PGIMS Rohtak, Rohtak, Haryana, India bMBBS student *Corresponding author, email: [email protected] Background: Coeliac plexus neurolysis (CPN) helps to diminish pain arising from malignancy of upper abdominal viscera. Imag- ing modalities have increased the success rates by enhancing technical accuracy including fluoroscopy, computed tomography and ultrasound. Advancement in the imaging modalities used has helped in the accurate depiction of anatomy and position of the needle tip. Methods: In an anterior approach, the patient lies supine and the needle is inserted through the anterior abdominal wall into the retropancreatic space. The needle often traverses the stomach, liver or pancreas before reaching the coeliac plexus due to anatomical considerations. The literature has been reviewed regarding various imaging modalities using an anterior approach to coeliac plexus block with regard to success rate, improvement in pain scores, duration of pain relief and analgesic consumption. -

Celiac Plexus Neurolysis: an Effective Alternative for the Treatment Of
Educational Essay Celiac plexus neurolysis: an effective alternative for the treatment of persistent abdominal pain Ángela Bettiana Cura, Verónica Andrea Salto, Renzo Sebastián Mestas Nuñez, Favio Augusto Mestas Nuñez, Héctor Alberto Canosa. Resumen Abstract Introducción: La neurólisis del plexo celíaco (NPC) es Introduction: Celiac Plexus Neurolysis (CPN) is a percu- un procedimiento percutáneo que permite la inyec- taneous procedure performed to inject a local neurolytic ción de un agente neurolitíco local, proporcionando agent that provides a prolonged analgesia in patients una analgesia prolongada en pacientes con dolor with persistent or intractable upper abdominal pain. abdominal superior persistente o intratable. Hasta un 60 to 80% of patients suffering from oncologic eso- 80% de los pacientes con dolor oncológico de ori- phageal, gastric, pancreatic or biliary pain can benefit gen esofágico, gástrico, pancreático o biliar pueden from this technique and reduce the use of opiates and beneficiarse con este tratamiento, disminuyendo el their adverse effects. Objectives: To demonstrate the uso de opiáceos y sus efectos adversos. Objetivos: posterior intervertebral disc CT-guided access path for Demostrar el abordaje intervertebral discal posterior the performance of CPN and to describe its complica- guiado por TC para la realización de NPC y describir tions. Revision: The celiac plexus is a visceral plexus sus complicaciones. Revisión: El plexo celíaco es un located in the retroperitoneum. It provides sympathe- plexo visceral que se localiza en el retroperitoneo. tic, parasympathetic and sensory innervation to upper Proporciona inervación simpática, parasimpática y abdominal viscera. CT is a precise guide for the injection sensitiva a las vísceras del abdomen superior. La TC of a neurolytic agent (phenol or ethanol). -

Celiac and Splanchnic Plexus Neurolysis
Published online: 2021-03-26 Review Article How I Do It: Celiac and Splanchnic Plexus Neurolysis Abstract Aghiad Al-Kutoubi Celiac block to alleviate pain in the upper abdomen was first described by Kappis in 1914. Since Department of Diagnostic then the role of this procedure has been fairly established in the management of pain related to Radiology, IR Division, The pancreatic disease and also in pain related to liver, gall bladder and gastric diseases. This article American University of Beirut discusses the clinical indications and technical details of celiac and splanchnic neurolysis. Medical Center, Beirut, Lebanon Keywords: Block, celiac, neurolysis, splanchnic Introduction such as triamcinolone. This is generally used in benign disease. Celiac block to alleviate pain in the upper abdomen was first described by Kappis Celiac plexus neurolysis is the term used to in 1914. Since then, the role of this describe long-term treatment using alcohol procedure has been fairly established in the or phenol generally used in malignant management of pain related to pancreatic disease. disease and also in pain related to liver, gallbladder, and gastric diseases. Indications The need for this procedure is ideally Anatomy [Figures 1-3] discussed in a multidisciplinary forum. The The celiac plexus is the upper and largest main indication is chronic pain, which can no of the autonomic nerve plexi. It extends in longer be managed with medication mainly front of and along both sides of the aorta from upper abdominal organs. The most and around the celiac artery trunk in the common patients for this procedure are those retroperitoneal space.