ITPE Sample.Fm
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Percutaneous Nephrostomy and Sclerotherapy with 96% Ethanol for the Treatment of Simple Renal Cysts: Pilot Study Mustafa Kadıhasanoğlu1, Mete Kilciler2, Özcan Atahan3
İstanbul Med J 2016; 17: 20-3 Original Article DOI: 10.5152/imj.2016.20981 Percutaneous Nephrostomy and Sclerotherapy with 96% Ethanol for the Treatment of Simple Renal Cysts: Pilot Study Mustafa Kadıhasanoğlu1, Mete Kilciler2, Özcan Atahan3 Introduction: The objectives of this study was to evaluate the safety and efficacy of aspiration with percutaneous nephrostomy tube and sclerotherapy with 96% ethanol for simple renal cyst. Methods: Between 2011-2014, 34 patients with symptomatic renal cysts were included in the study. Mean age was 52.3±4.6 years (range, 39-72 years). The Abstract patients had only flank pain. Procedure was performed with ultrasound guidance and under fluoroscopic control. After puncture with 18 G angiography needle, guide-wire was advanced to the collecting system. An 14Fr nephrostomy catheter was then advanced over the guide wire. After taking cystography 96% ethyl alcohol was injected into the cyst and drained amount 10%. We continued daily to inject same amount of alcohol postoperatively until the drainage was less than 50 mL. 6th months and yearly follow-up were performed with ultrasound.. Results: Percutaneous access was achieved in all patients. Cysts were unilateral, single and with a mean diameter 9.1±3.2 cm (range, 7-16 cm). Median drained volume was 212 mL (200-1600 mL) and median the injected ethanol volume was 54 mL (20- 160 mL). Radiological improvement at the end of the 6th month was amount 94.1% and 91.1% at the end of the 1st year while 83.3% of patients had symptomatic decline. There was no major complication after the procedure. -

Surgical Treatment of Snoring and Obstructive Sleep Apnea Syndrome
Medical Policy Surgical Treatment of Snoring and Obstructive Sleep Apnea Syndrome Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy: Medicare Description References Authorization Information Policy History Policy Number: 130 BCBSA Reference Number: 7.01.101 Related Policies None Policy Commercial Members: Managed Care (HMO and POS), PPO, and Indemnity Medicare HMO BlueSM and Medicare PPO BlueSM Members Uvulopalatopharyngoplasty (UPPP) may be MEDICALLY NECESSARY for the treatment of clinically significant obstructive sleep apnea syndrome (OSAS) in appropriately selected adult patients who have failed an adequate trial of continuous positive airway pressure (CPAP) or failed an adequate trial of an oral appliance (OA). Clinically significant OSA is defined as those patients who have: Apnea/hypopnea Index (AHI) or Respiratory Disturbance Index (RDI) 15 or more events per hour, or AHI or RDI 5 or more events and 14 or less events per hour with documented symptoms of excessive daytime sleepiness, impaired cognition, mood disorders or insomnia, or documented hypertension, ischemic heart disease, or history of stroke. Hyoid suspension, surgical modification of the tongue, and/or maxillofacial surgery, including mandibular- maxillary advancement (MMA), may be MEDICALLY NECESSARY in appropriately selected adult patients with clinically significant OSA and objective documentation of hypopharyngeal obstruction who have failed an adequate trial of continuous positive airway pressure (CPAP) or failed an adequate trial of an oral appliance (OA). Clinically significant OSA is defined as those patients who have: AHI or RDI 15 or more events per hour, or AHI or RDI 5 or more events and 14 or less events per hour with documented symptoms of excessive daytime sleepiness, impaired cognition, mood disorders or insomnia, or documented hypertension, ischemic heart disease, or history of stroke. -

Urology 1 Cystoscopes
Urology 1 Cystoscopes 2 Urethrotomes 3 Resectoscopes 4 Uretero-Renoscopes 5 Nephroscopes 6 Lithotripsy (UreTron) 7 Laser Therapy 8 Small Caliber 9 Fluid Management 10 Accessories Richard Wolf Medical Instruments Corporation assumes no responsibility or liability for any errors or omissions in the content of this catalog. The information contained in this catalog is provided on an “as is” basis with no guarantees of completeness, accuracy, usefulness, or timeliness, and without warranties of any kind whatsoever, expressed or implied. 1777- 02.01-1118USA Cysto-Urethroscopes 8650 E-line design CYSTOSCOPES The E-line design guarantees optimum handling and safe, fatigue-free operation as well as a wide range of possible combinations. Basic Set for Cystoscopy Cysto-urethroscope sheath, 19.5 Fr. with obturator 8650.0341 Adapter with 1 instrument port 8650.264 Insert with Albarran deflector, 2 instrument ports 8650.204 Sterile universal sealing valve (pack of 5) 4712348 Viewing obturator 8650.724 Biopsy forceps Marburg 8650.614 Grasping forceps 8650.684 PANOVIEW telescope, 0° 8650.414 PANOVIEW telescope, 70° 8650.415 Otis urethrotome 8517.00 822.31 822.13 822.31 Flexible connector 822.13 Tray 8585030 1777- 02.01-1118USA 2 PANOVIEW Telescopes Overview CYSTOSCOPES Ø Viewing direction Color code Application mm 0° blue Standard 4 8650.414 12° orange Standard 4 8654.431 Standard 4 8654.422 30° red Long sheath 4 8668.433* 70° yellow Standard 4 8650.415 * Only 25° available. 1777- 02.01-1118USA 3 Cysto-Urethroscope 8650 for telescope 4 mm, 0°, 12°, 30°, 70° and adapters CYSTOSCOPES Sheaths and obturators Adapters Sheath incl. -
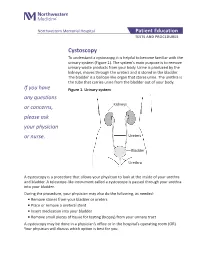
Cystoscopy to Understand a Cystoscopy, It Is Helpful to Become Familiar with the Urinary System (Figure 1)
Northwestern Memorial Hospital Patient Education TESTS AND PROCEDURES Cystoscopy To understand a cystoscopy, it is helpful to become familiar with the urinary system (Figure 1). The system’s main purpose is to remove urinary waste products from your body. Urine is produced by the kidneys, moves through the ureters and is stored in the bladder. The bladder is a balloon-like organ that stores urine. The urethra is the tube that carries urine from the bladder out of your body. If you have Figure 1. Urinary system any questions or concerns, Kidneys please ask your physician or nurse. Ureters Bladder Urethra A cystoscopy is a procedure that allows your physician to look at the inside of your urethra and bladder. A telescope-like instrument called a cystoscope is passed through your urethra into your bladder. During the procedure, your physician may also do the following, as needed: ■ Remove stones from your bladder or ureters ■ Place or remove a ureteral stent ■ Insert medication into your bladder ■ Remove small pieces of tissue for testing (biopsy) from your urinary tract A cystoscopy may be done in a physician’s office or in the hospital’s operating room (OR). Your physician will discuss which option is best for you. Preparation and procedure If the test is done in the OR, you will be asked to sign a written consent. The OR procedure and any special preparation will be explained to you. There may be some discomfort during the examination. Some patients may require sedation or anesthesia. Depending on the type of medication used for your procedure, you will be told if you need to stop eating and drinking before your procedure. -

ICD-10 Coding Clinic Corner: Accountability Act of 1996 (HIPAA) Is 413.65(A)(2): Diabetes and Osteomyelitis
Issue No. 6 Volume No. 2 September 2015 New and Revised Place of Service TABLE of CONTENTS Codes for OutpatientNote Hospital from Tony New and Revised Place of Joette P. Derricks, MPA, CMPE, CHC, CPC, CSSGB Service Codes for Outpatient Joh Vice President of Regulatory Affairs & Research Hospital ..................................... 1 MiraMed Global Services ERCP with Exchange of a Common Bile Duct Stent .......... 3 Any health insurer subject to the policy. Contractor editing shall Laparoscopic Procedure: An uniform electronic claim transaction treat POS 19 and POS 22 in the Education .................................. 5 and code set standards under the same way. The definition of a Health Insurance Portability and “campus” is found in Title 42 CFR ICD-10 Coding Clinic Corner: Accountability Act of 1996 (HIPAA) is 413.65(a)(2): Diabetes and Osteomyelitis ..... 7 required to make changes to the Campus means the physical Place of Service (POS) code from the Stars of MiraMed ...................... 8 area immediately adjacent to POS code set maintained by the the provider’s main buildings, Are You a Good Auditor? ......... 9 Centers for Medicare and Medicaid other areas and structures that Services (CMS) effective January 1, Coding Case Scenario ............. 11 are not strictly contiguous to 2016. the main buildings but are The POS code set provides setting located within 250 yards of the If you have an article information necessary to main buildings, and any other appropriately pay Medicare and areas determined on an or idea to share for The Medicaid claims. Other payers may individual case basis, by the Code , please submit to: or may not use the POS codes in the CMS regional office, to be part Dr. -

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Italy and Ligurian Regional HTA Network Abstract Number: 169775
Abstract Number: 169775 Mini HTA: an effective tool for clinical governance, resource allocation and conflict management at local (Regional) level. Gaddo Flego MD, Francesco Cardinale MD, ASL Nr 4 "Chiavarese", Italy and Ligurian Regional HTA Network The Italian National Health System is centrally governed by the Ministry of Health and by Local Health Authorities (ASL) at Regional level. The Region of Liguria is divided into 5 ASL. Each ASL governs hospitals in the territory of competence. Liguria, for the government of technological innovation, approved with a formal act in 2011 (DGR 295) the creation of a Regional HTA Network in order to implement the process of Health Technology Assessment and to develop the concept of Evidence Based Medicine. The main point of the resolution is the introduction of a Mini HTA grid, that must be filled by proponents before the introduction of any technological innovation. Regional HTA Workflow Since 2011 the Ligurian Network Regional HTA Network has Organisation & Role Hospitals require innovative evaluated the following technologies through Mini devices: Director HTA grid compilation 1) Virtual Colonoscopy CAD Coordination group 2) Porcine Dermal Collagen Surgery Consists of all Professionals who Grid submission to Scientific 3) Sling for urinary incontinence may be involved in the Secretariat 4) Collagen Matrix for sutures evaluation, depending on the 5) Fixation device in surgery device to be evaluated: doctors 6) Sterilization devices with different specialisations, Analysis of quality of data 7) Implantable device for Glaucoma clinical engineers, chemists, produced in the grid, 8) Intravascular Catheter context and scientific health economists and 9) Optical Coherence Tomography literature by the Scientific 10) Pneumothorax drainage system representatives of the citizens. -

(Mitomycin) for Pyelocalyceal Solution with a Nephrostomy Tube
INSTRUCTION GUIDE for Instillation of JELMYTO® (mitomycin) for pyelocalyceal solution with a Nephrostomy Tube Important Information Please refer to the FDA-approved Prescribing Information and Instructions for Administration (IFA) for information about JELMYTO. JELMYTO is a cytotoxic drug. Follow applicable special handling and disposal procedures. This Instruction Guide contains supplemental information on how to instill JELMYTO via a nephrostomy tube. These instructions are derived from materials from the OLYMPUS Clinical Trial. It is important to note that in the OLYMPUS Clinical Trial, no investigators utilized a nephrostomy tube as the mode of administration. Important Information Regarding Nephrostomy Instillation Note: Follow practice/institutional protocol regarding placement for nephrostomy tube and time allowance for healing before proceeding with JELMYTO instillation. • Prior to administration, implement your clinic's practice for draining the patients' urine. • A Silicon or Silastic percutaneous nephrostomy tube with molded Luer lock connector and locking loop must be placed prior to installation of JELMYTO. Latex should not be used, due to risk of rupture. Instillation Instructions A. Measure the Kidney Volume Before the First Instillation The Instillation Volume will be equal to the patient’s kidney volume. If the kidney volume is already known, proceed to Section B. If the kidney volume is NOT known, or needs to be reassessed, use the following steps: 1. Perform an antegrade pyelogram using diluted contrast (50%) so that the entire renal pelvis and calyces are observed and contrast starts to flow below the ureteropelvic junction (UPJ). 2. Record the volume of contrast injected at this point. 3. Allow the contrast to drain from the kidney. -

Synovial Fluidfluid 11
LWBK461-c11_p253-262.qxd 11/18/09 6:04 PM Page 253 Aptara Inc CHAPTER SynovialSynovial FluidFluid 11 Key Terms ANTINUCLEAR ANTIBODY ARTHROCENTESIS BULGE TEST CRYSTAL-INDUCED ARTHRITIS GROUND PEPPER HYALURONATE MUCIN OCHRONOTIC SHARDS RHEUMATOID ARTHRITIS (RA) RHEUMATOID FACTOR (RF) RICE BODIES ROPE’S TEST SEPTIC ARTHRITIS Learning Objectives SYNOVIAL SYSTEMIC LUPUS ERYTHEMATOSUS 1. Define synovial. VISCOSITY 2. Describe the formation and function of synovial fluid. 3. Explain the collection and handling of synovial fluid. 4. Describe the appearance of normal and abnormal synovial fluids. 5. Correlate the appearance of synovial fluid with possible cause. 6. Interpret laboratory tests on synovial fluid. 7. Suggest further testing for synovial fluid, based on preliminary results. 8. List the four classes or categories of joint disease. 9. Correlate synovial fluid analyses with their representative disease classification. 253 LWBK461-c11_p253-262.qxd 11/18/09 6:04 PM Page 254 Aptara Inc 254 Graff’s Textbook of Routine Urinalysis and Body Fluids oint fluid is called synovial fluid because of its resem- blance to egg white. It is a viscous, mucinous substance Jthat lubricates most joints. Analysis of synovial fluid is important in the diagnosis of joint disease. Aspiration of joint fluid is indicated for any patient with a joint effusion or inflamed joints. Aspiration of asymptomatic joints is beneficial for patients with gout and pseudogout as these fluids may still contain crystals.1 Evaluation of physical, chemical, and microscopic characteristics of synovial fluid comprise routine analysis. This chapter includes an overview of the composition and function of synovial fluid, and laboratory procedures and their interpretations. -
The Importance of Orofacial Myofunctional Therapy Before and After CO2 Laser Frenectomy in Achieving Optimal Orofacial Function
LASERfocus The Importance of Orofacial Myofunctional Therapy Before and After CO2 Laser Frenectomy in Achieving Optimal Orofacial Function by Karen M. Wuertz, DDS, ABCDSM, DABLS, FOM, and Brooke Pettus, RDH, BSDH, COMS Frenectomy Methods ing, speaking, and breathing patterns may be Frenotomies performed with a scalpel or scissors can be accompanied by caused by incorrect oral posture and oral re- significant bleeding, obscuring the surgical field making it difficult to ensure strictions. Therefore, in the authors’ opinion, if the restriction has been completely removed. Because of the increased risk the removal of oral restrictions is necessary to of early primary closure of the site, postoperative active wound care is es- attain optimal orofacial function, and must be sential to reduce the risk of potential scarring. To properly restore and main- combined with regular pre- and post-frenecto- tain optimum function, active wound care should be implemented as soon my orofacial myofunctional therapy (OMT).1,4 as possible. However, if sutures are placed, the active wound care may be OMT helps re-educate the tongue and orofa- delayed so as not to cause early tearing of tissue. Due to the contact nature of cial muscles during movement and at rest to conventional procedure, there is a certain potential for infection; in addition, create new neuromuscular patterns for proper higher levels of postoperative pain and discomfort have been reported.1,2 Elec- oral function, including chewing, swallowing, trocautery and a hot glass tip of dental diodes may leave a fairly substantial speaking, and breathing.5,6 Camacho et al.7 zone of thermal tissue change3 and may result in delayed healing. -

Enteroliths in a Kock Continent Ileostomy: Case Report and Review of the Literature
E200 Cases and Techniques Library (CTL) similar symptoms recurred 2 years later. A second ileoscopy showed a narrowed Enteroliths in a Kock continent ileostomy: efferent loop that was dilated by insertion case report and review of the literature of the colonoscope, with successful relief of her symptoms. Chemical analysis of one of the retrieved enteroliths revealed calcium oxalate crystals. Five cases have previously been noted in the literature Fig. 1 Schematic (●" Table 1). representation of a Kock continent The alkaline milieu of succus entericus in ileostomy. the ileum may induce the precipitation of a calcium oxalate concretion; in contrast, the acidic milieu found more proximally in the intestine enhances the solubility of calcium. The gradual precipitation of un- conjugated bile salts, calcium oxalate, and Valve calcium carbonate crystals around a nidus composed of fecal material or undigested Efferent loop fiber can lead to the formation of calcium oxalate calculi over time [5]. Endoscopy_UCTN_Code_CCL_1AD_2AJ Reservoir Competing interests: None Hadi Moattar1, Jakob Begun1,2, Timothy Florin1,2 1 Department of Gastroenterology, Mater Adult Hospital, South Brisbane, Australia The Kock continent ileostomy (KCI) was dure was done to treat ulcerative pan- 2 Mater Research, University of Queens- designed by Nik Kock, who used an intus- colitis complicated by colon cancer. She land, Translational Research Institute, suscepted ileostomy loop to create a nip- had a well-functioning KCI that she had Woolloongabba, Australia ple valve (●" Fig.1) that would not leak catheterized daily for 34 years before she and would allow ileal effluent to be evac- presented with intermittent abdominal uated with a catheter [1]. -

Septicaemia After Colonoscopy in Patients With
450 Gut, 1991,32,450-451 Septicaemia after colonoscopy in patients with cirrhosis Gut: first published as 10.1136/gut.32.4.450 on 1 April 1991. Downloaded from j R Thornton, M S Losowsky Abstract PATIENT 2 Two patients with ulcerative colitis and In 1987, a 34 year old man underwent routine chronic active hepatitis with cirrhosis, who colonoscopy because ofhis ulcerative colitis of 12 developed Gram negative septicaemia after years' duration. Twenty three years earlier a colonoscopy are described. These and two liver biopsy had shown that he had chronic similar reported cases indicate that giving active hepatitis and cirrhosis. Hepatitis B prophylactic antibiotics to patients with cir- markers were negative. In 1983 he developed rhosis undergoing colonoscopy should be con- ascites and had remained on spironolactone since sidered, particularly when the cirrhosis is then. advanced. At the time ofhis colonoscopy he claimed that he felt reasonably well and was continuing to work. However, he had a moderate amount of Prophylactic antibiotics have been advised for ascites. His medication was: prednisolone 5 mg patients undergoing colonoscopy who have daily, spironolactone 200 mg daily, and sul- valvular heart disease, cardiac prostheses, severe phasalazine 1 g twice daily. Preoperative blood immunodepression, or hepatic cirrhosis with tests were: bilirubin 53 ,umol/1, alanine amino- ascites.' The last of these recommendations is transferase 38 IU/, alkaline phosphatase 206 IU/ based on a single case report in which it was not 1, albumin 28 g/l, prothrombin time 16 seconds certain that colonoscopy was responsible for the (control 14 seconds). infection, as hepatic angiography was performed After bowel preparation with three litres of the day before peritonitis developed.' We were Golytely, colonoscopy to the caecum was per- unaware of this case but our recent experience formed.