Complete Surgical Resection of High-Grade Astroblastoma with Long Time Survival: Case Report and Review of the Literature
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1
[CANCER RESEARCH 49, 6137-6143. November 1, 1989] Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1 Susan Preston-Martin,2 Wendy Mack, and Brian E. Henderson Department of Preventive Medicine, University of Southern California School of Medicine, Los Angeles, California 90033 ABSTRACT views with proxy respondents, we were unable to include a large proportion of otherwise eligible cases because they were deceased or Detailed job histories and information about other suspected risk were too ill or impaired to participate in an interview. The Los Angeles factors were obtained during interviews with 272 men aged 25-69 with a County Cancer Surveillance Program identified the cases (26). All primary brain tumor first diagnosed during 1980-1984 and with 272 diagnoses had been microscopically confirmed. individually matched neighbor controls. Separate analyses were con A total of 478 patients were identified. The hospital and attending ducted for the 202 glioma pairs and the 70 meningioma pairs. Meningi- physician granted us permission to contact 396 (83%) patients. We oma, but not glioma, was related to having a serious head injury 20 or were unable to locate 22 patients, 38 chose not to participate, and 60 more years before diagnosis (odds ratio (OR) = 2.3; 95% confidence were aphasie or too ill to complete the interview. We interviewed 277 interval (CI) = 1.1-5.4), and a clear dose-response effect was observed patients (74% of the 374 patients contacted about the study or 58% of relating meningioma risk to number of serious head injuries (/' for trend the initial 478 patients). -

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
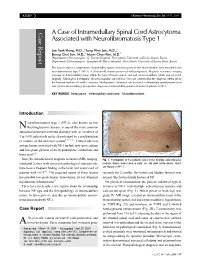
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Survival and Functional Outcome of Childhood Spinal Cord Low-Grade Gliomas
J Neurosurg Pediatrics 4:000–000,254–261, 2009 Survival and functional outcome of childhood spinal cord low-grade gliomas Clinical article KATRIN SCHEINEMANN, M.D.,1 UTE BARTELS, M.D.,2 ANNIE HUANG, M.D., PH.D.,2 CYNTHIA HAWKINS, M.D., PH.D.,3 ABHAYA V. KULKARNI, M.D., PH.D.,4 ERIC BOUFFET, M.D.,2 AND URI TABORI, M.D.2 1Division of Hematology/Oncology, McMaster Children’s Hospital, Hamilton; and Divisions of 2Hematology/ Oncology, 3Pathology, and 4Neurosurgery, The Hospital for Sick Children, Toronto, Ontario, Canada Object. Intramedullary spinal cord low-grade gliomas (LGGs) are rare CNS neoplasms in pediatric patients, and there is little information on therapy for and outcome of these tumors in this population. Furthermore, most patient series combine adult and pediatric patients or high- and low-grade tumors, resulting in controversial data regarding optimal treatment of these children. To clarify these issues, the authors performed a regional population-based study of spinal cord LGGs in pediatric patients. Methods.$OOSHGLDWULFSDWLHQWVZLWK/**VWUHDWHGGXULQJWKH05LPDJLQJHUD ² ZHUHLGHQWLÀHGLQ the comprehensive database of the Hospital for Sick Children in Toronto. Data on demographics, pathology, treat- ment details, and outcomes were collected. Results. Spinal cord LGGs in pediatric patients constituted 29 (4.6%) of 635 LGGs. Epidemiological and clini- cal data in this cohort were different than in patients with other spinal tumors and strikingly similar to data from pediatric patients with intracranial LGGs. The authors observed an age peak at 2 years and a male predominance in patients with these tumors. Histological testing revealed a Grade I astrocytoma in 86% of tumors. -

Risk-Adapted Therapy for Young Children with Embryonal Brain Tumors, High-Grade Glioma, Choroid Plexus Carcinoma Or Ependymoma (Sjyc07)
SJCRH SJYC07 CTG# - NCT00602667 Initial version, dated: 7/25/2007, Resubmitted to CPSRMC 9/24/2007 and 10/6/2007 (IRB Approved: 11/09/2007) Activation Date: 11/27/2007 Amendment 1.0 dated January 23, 2008, submitted to CPSRMC: January 23, 2008, IRB Approval: March 10, 2008 Amendment 2.0 dated April 16, 2008, submitted to CPSRMC: April 16, 2008, (IRB Approval: May 13, 2008) Revision 2.1 dated April 29, 2009 (IRB Approved: April 30, 2009 ) Amendment 3.0 dated June 22, 2009, submitted to CPSRMC: June 22, 2009 (IRB Approved: July 14, 2009) Activated: August 11, 2009 Amendment 4.0 dated March 01, 2010 (IRB Approved: April 20, 2010) Activated: May 3, 2010 Amendment 5.0 dated July 19, 2010 (IRB Approved: Sept 17, 2010) Activated: September 24, 2010 Amendment 6.0 dated August 27, 2012 (IRB approved: September 24, 2012) Activated: October 18, 2012 Amendment 7.0 dated February 22, 2013 (IRB approved: March 13, 2013) Activated: April 4, 2013 Amendment 8.0 dated March 20, 2014. Resubmitted to IRB May 20, 2014 (IRB approved: May 22, 2014) Activated: May 30, 2014 Amendment 9.0 dated August 26, 2014. (IRB approved: October 14, 2014) Activated: November 4, 2014 Un-numbered revision dated March 22, 2018. (IRB approved: March 27, 2018) Un-numbered revision dated October 22, 2018 (IRB approved: 10-24-2018) RISK-ADAPTED THERAPY FOR YOUNG CHILDREN WITH EMBRYONAL BRAIN TUMORS, HIGH-GRADE GLIOMA, CHOROID PLEXUS CARCINOMA OR EPENDYMOMA (SJYC07) Principal Investigator Amar Gajjar, M.D. Division of Neuro-Oncology Department of Oncology Section Coordinators David Ellison, M.D., Ph.D. -

Astrocytoma: a Hormone-Sensitive Tumor?
International Journal of Molecular Sciences Review Astrocytoma: A Hormone-Sensitive Tumor? Alex Hirtz 1, Fabien Rech 1,2,Hélène Dubois-Pot-Schneider 1 and Hélène Dumond 1,* 1 Université de Lorraine, CNRS, CRAN, F-54000 Nancy, France; [email protected] (A.H.); [email protected] (F.R.); [email protected] (H.D.-P.-S.) 2 Université de Lorraine, CHRU-Nancy, Service de Neurochirurgie, F-54000 Nancy, France * Correspondence: [email protected]; Tel.: +33-372746115 Received: 29 October 2020; Accepted: 27 November 2020; Published: 30 November 2020 Abstract: Astrocytomas and, in particular, their most severe form, glioblastoma, are the most aggressive primary brain tumors and those with the poorest vital prognosis. Standard treatment only slightly improves patient survival. Therefore, new therapies are needed. Very few risk factors have been clearly identified but many epidemiological studies have reported a higher incidence in men than women with a sex ratio of 1:4. Based on these observations, it has been proposed that the neurosteroids and especially the estrogens found in higher concentrations in women’s brains could, in part, explain this difference. Estrogens can bind to nuclear or membrane receptors and potentially stimulate many different interconnected signaling pathways. The study of these receptors is even more complex since many isoforms are produced from each estrogen receptor encoding gene through alternative promoter usage or splicing, with each of them potentially having a specific role in the cell. The purpose of this review is to discuss recent data supporting the involvement of steroids during gliomagenesis and to focus on the potential neuroprotective role as well as the mechanisms of action of estrogens in gliomas. -

The New WHO Classification of Brain Tumors and Molecular Profiling in the Diagnosis of Gliomas
The New WHO Classification of Brain Tumors and Molecular Profiling in the Diagnosis of Gliomas Aivi Nguyen, MD Neuropathology Fellow Division of Neuropathology Center for Personalized Diagnosis (CPD) Glial neoplasms – infiltrating gliomas Astrocytic tumors • Diffuse astrocytoma II • Anaplastic astrocytoma III • Glioblastoma • Giant cell glioblastoma IV • Gliosarcoma Oligodendroglial tumors • Oligodendroglioma II • Anaplastic oligodendroglioma III Oligoastrocytic tumors • Oligoastrocytoma II • Anaplastic oligoastrocytoma III Courtesy of Dr. Maria Martinez-Lage 2 2016 3 The 2016 WHO classification of tumours of the central nervous system Louis et al., Acta Neuropathologica 2016 4 Talk Outline Genetic, epigenetic and metabolic changes in gliomas • Mechanisms/tumor biology • Incorporation into daily practice and WHO classification Penn’s Center for Personalized Diagnostics • Tests performed • Results and observations to date Summary 5 The 2016 WHO classification of tumours of the central nervous system Louis et al., Acta Neuropathologica 2016 6 Mechanism of concurrent 1p and 19q chromosome loss in oligodendroglioma lost FUBP1 CIC Whole-arm translocation Griffin et al., Journal of Neuropathology and Experimental Neurology 2006 7 Oligodendroglioma: 1p19q co-deletion Since the 1990s Diagnostic Prognostic Predictive Li et al., Int J Clin Exp Pathol 2014 8 Mutations of Selected Genes in Glioma Subtypes GBM Astrocytoma Oligodendroglioma Oligoastrocytoma Killela et al., PNAS 2013 9 Escaping Senescence Telomerase reverse transcriptase gene -

Malignant CNS Solid Tumor Rules
Malignant CNS and Peripheral Nerves Equivalent Terms and Definitions C470-C479, C700, C701, C709, C710-C719, C720-C725, C728, C729, C751-C753 (Excludes lymphoma and leukemia M9590 – M9992 and Kaposi sarcoma M9140) Introduction Note 1: This section includes the following primary sites: Peripheral nerves C470-C479; cerebral meninges C700; spinal meninges C701; meninges NOS C709; brain C710-C719; spinal cord C720; cauda equina C721; olfactory nerve C722; optic nerve C723; acoustic nerve C724; cranial nerve NOS C725; overlapping lesion of brain and central nervous system C728; nervous system NOS C729; pituitary gland C751; craniopharyngeal duct C752; pineal gland C753. Note 2: Non-malignant intracranial and CNS tumors have a separate set of rules. Note 3: 2007 MPH Rules and 2018 Solid Tumor Rules are used based on date of diagnosis. • Tumors diagnosed 01/01/2007 through 12/31/2017: Use 2007 MPH Rules • Tumors diagnosed 01/01/2018 and later: Use 2018 Solid Tumor Rules • The original tumor diagnosed before 1/1/2018 and a subsequent tumor diagnosed 1/1/2018 or later in the same primary site: Use the 2018 Solid Tumor Rules. Note 4: There must be a histologic, cytologic, radiographic, or clinical diagnosis of a malignant neoplasm /3. Note 5: Tumors from a number of primary sites metastasize to the brain. Do not use these rules for tumors described as metastases; report metastatic tumors using the rules for that primary site. Note 6: Pilocytic astrocytoma/juvenile pilocytic astrocytoma is reportable in North America as a malignant neoplasm 9421/3. • See the Non-malignant CNS Rules when the primary site is optic nerve and the diagnosis is either optic glioma or pilocytic astrocytoma. -
Meningioma ACKNOWLEDGEMENTS
AMERICAN BRAIN TUMOR ASSOCIATION Meningioma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Meningioma Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit advocacy organization dedicated solely to brain tumor research. For nearly 45 years, the ABTA has been providing comprehensive resources that support the complex needs of brain tumor patients and caregivers, as well as the critical funding of research in the pursuit of breakthroughs in brain tumor diagnosis, treatment and care. To learn more about the ABTA, visit www.abta.org. We gratefully acknowledge Santosh Kesari, MD, PhD, FANA, FAAN chair of department of translational neuro- oncology and neurotherapeutics, and Marlon Saria, MSN, RN, AOCNS®, FAAN clinical nurse specialist, John Wayne Cancer Institute at Providence Saint John’s Health Center, Santa Monica, CA; and Albert Lai, MD, PhD, assistant clinical professor, Adult Brain Tumors, UCLA Neuro-Oncology Program, for their review of this edition of this publication. This publication is not intended as a substitute for professional medical advice and does not provide advice on treatments or conditions for individual patients. All health and treatment decisions must be made in consultation with your physician(s), utilizing your specific medical information. Inclusion in this publication is not a recommendation of any product, treatment, physician or hospital. COPYRIGHT © 2017 ABTA REPRODUCTION WITHOUT PRIOR WRITTEN PERMISSION IS PROHIBITED AMERICAN BRAIN TUMOR ASSOCIATION Meningioma INTRODUCTION Although meningiomas are considered a type of primary brain tumor, they do not grow from brain tissue itself, but instead arise from the meninges, three thin layers of tissue covering the brain and spinal cord. -

High-Grade Glioma/Glioblastoma Multiforme: Is There a Role for Photodynamic Therapy?
S-31 Supplement High-Grade Glioma/Glioblastoma Multiforme: Is There a Role for Photodynamic Therapy? Presented by Harry T. Whelan, MD, Medical College of Wisconsin, Milwaukee, Wisconsin Abstract backward glance at the origins of PDT for brain tumors, In the United States, the 5-year survival rate for patients of all ages describes the clinical challenges to its use in the skull, with all types of brain tumors is approximately 20%, with the scale skewed toward even poorer survival in patients with gliomas. Al- and outlines the objectives of his phase I study for PDT though surgery and radiotherapy are primary treatment options, in children with brain cancer, the second most common surgery is rarely curative and radiotherapy has had little impact childhood cancer after leukemia. on overall survival. Predominantly studied in adults with advanced Gliomas are among the most challenging of brain high-grade gliomas, photodynamic therapy (PDT) represents tumor subtypes. The location of a benign tumor in the a paradigmatic shift in the treatment of brain tumors. With no eloquent areas of the brain could potentially render it clear standard of care for brain tumors, PDT may emerge as a po- tential alternative, although challenges regarding its clinical use inoperable, the presence of a blood–brain barrier limits remain and studies confirming its promise are necessary. JNCCN( the ability of systemically administered medications to 2012;10[Suppl 2]:S31–S34) reach the target site, and the intricate neuronal net- work makes targeted therapy challenging. Patients with high-grade gliomas (HGGs) in particular have a generally poor prognosis, and surgery is rarely curative. -

Impact of Adjuvant Radiotherapy in Patients with Central Neurocytoma: a Multicentric International Analysis
cancers Article Impact of Adjuvant Radiotherapy in Patients with Central Neurocytoma: A Multicentric International Analysis Laith Samhouri 1,†, Mohamed A. M. Meheissen 2,3,† , Ahmad K. H. Ibrahimi 4, Abdelatif Al-Mousa 4, Momen Zeineddin 5, Yasser Elkerm 3,6, Zeyad M. A. Hassanein 2,3 , Abdelsalam Attia Ismail 2,3, Hazem Elmansy 3,6, Motasem M. Al-Hanaqta 7 , Omar A. AL-Azzam 8, Amr Abdelaziz Elsaid 2,3 , Christopher Kittel 1, Oliver Micke 9, Walter Stummer 10, Khaled Elsayad 1,*,‡ and Hans Theodor Eich 1,‡ 1 Department of Radiation Oncology, University Hospital Münster, Münster 48149, Germany; [email protected] (L.S.); [email protected] (C.K.); [email protected] (H.T.E.) 2 Alexandria Clinical Oncology Department, Alexandria University, Alexandria 21500, Egypt; [email protected] (M.A.M.M.); [email protected] (Z.M.A.H.); [email protected] (A.A.I.); [email protected] (A.A.E.) 3 Specialized Universal Network of Oncology (SUN), Alexandria 21500, Egypt; [email protected] (Y.E.); [email protected] (H.E.) 4 Department of Radiotherapy and Radiation Oncology, King Hussein Cancer Center, Amman 11942, Jordan; [email protected] (A.K.H.I.); [email protected] (A.A.-M.) 5 Department of Pediatrics, King Hussein Cancer Center, Amman 11942, Jordan; [email protected] 6 Cancer Management and Research Department, Medical Research Institute, Alexandria University, Alexandria 21500, Egypt 7 Military Oncology Center, Royal Medical Services, Amman 11942, Jordan; [email protected] 8 Princess Iman Research Center, King Hussein Medical Center, Royal Medical Services, Amman 11942, Jordan; Citation: Samhouri, L.; Meheissen, [email protected] 9 M.A.M.; Ibrahimi, A.K.H.; Al-Mousa, Department of Radiotherapy and Radiation Oncology, Franziskus Hospital Bielefeld, A.; Zeineddin, M.; Elkerm, Y.; 33699 Bielefeld, Germany; [email protected] 10 Department of Neurosurgery, University Hospital Münster, 48149 Münster, Germany; Hassanein, Z.M.A.; Ismail, A.A.; [email protected] Elmansy, H.; Al-Hanaqta, M.M.; et al.