Downloads (Not All App Sharing and Downloads Could Be Tracked)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Districts of Ethiopia
Region District or Woredas Zone Remarks Afar Region Argobba Special Woreda -- Independent district/woredas Afar Region Afambo Zone 1 (Awsi Rasu) Afar Region Asayita Zone 1 (Awsi Rasu) Afar Region Chifra Zone 1 (Awsi Rasu) Afar Region Dubti Zone 1 (Awsi Rasu) Afar Region Elidar Zone 1 (Awsi Rasu) Afar Region Kori Zone 1 (Awsi Rasu) Afar Region Mille Zone 1 (Awsi Rasu) Afar Region Abala Zone 2 (Kilbet Rasu) Afar Region Afdera Zone 2 (Kilbet Rasu) Afar Region Berhale Zone 2 (Kilbet Rasu) Afar Region Dallol Zone 2 (Kilbet Rasu) Afar Region Erebti Zone 2 (Kilbet Rasu) Afar Region Koneba Zone 2 (Kilbet Rasu) Afar Region Megale Zone 2 (Kilbet Rasu) Afar Region Amibara Zone 3 (Gabi Rasu) Afar Region Awash Fentale Zone 3 (Gabi Rasu) Afar Region Bure Mudaytu Zone 3 (Gabi Rasu) Afar Region Dulecha Zone 3 (Gabi Rasu) Afar Region Gewane Zone 3 (Gabi Rasu) Afar Region Aura Zone 4 (Fantena Rasu) Afar Region Ewa Zone 4 (Fantena Rasu) Afar Region Gulina Zone 4 (Fantena Rasu) Afar Region Teru Zone 4 (Fantena Rasu) Afar Region Yalo Zone 4 (Fantena Rasu) Afar Region Dalifage (formerly known as Artuma) Zone 5 (Hari Rasu) Afar Region Dewe Zone 5 (Hari Rasu) Afar Region Hadele Ele (formerly known as Fursi) Zone 5 (Hari Rasu) Afar Region Simurobi Gele'alo Zone 5 (Hari Rasu) Afar Region Telalak Zone 5 (Hari Rasu) Amhara Region Achefer -- Defunct district/woredas Amhara Region Angolalla Terana Asagirt -- Defunct district/woredas Amhara Region Artuma Fursina Jile -- Defunct district/woredas Amhara Region Banja -- Defunct district/woredas Amhara Region Belessa -- -

Bishoftu Town Residents' Perception About Economic, Environmental And
Vol. 11(2), pp. 21-39, July-September 2020 DOI: 10.5897/JHMT2020.0277 Article Number: 3546FF764872 ISSN 2141-6575 Copyright © 2020 Journal of Hospitality Management and Author(s) retain the copyright of this article http://www.academicjournals.org/JHMT Tourism Full Length Research Paper Bishoftu town residents’ perception about economic, environmental and socio-cultural impacts of urban tourism Genet Abera1* and Engdawork Assefa2 1Department of Tourism Management, College of Social Science and Humanities, Bule Hora University, BuleHora, Ethiopia. 2Department of Tourism and Management, College of Development Studies, Center for Environment and Sustainable Development, Addis Ababa University, Addis Ababa, Ethiopia. Received 4 February, 2020; Accepted 7 April, 2020 The main purpose of this study is to explore the perception of Bishoftu town residents about the impacts of urban tourism. Both qualitative and quantitative research methods were employed to achieve the objective of this study. Random sampling procedure was used for selection of respondents from the residents. Descriptive and inferential statistics were used to analyze data. The result of factor analysis showed that three factors named economic, socio-cultural and environmental impacts explained 53.24% of variation in the perceptions of residents. However, most of the local residents and stakeholders were unaware of negative impact of urban tourism. MANOVA analysis indicated that, there was no significant difference between the mean of underlying dimensions of the perceived urban tourism impacts, and socio-demographic characteristics. The concerned bodies and officials should take the issues into account while planning and devising various measures. Key words: Urban tourism, residents‟ perception, tourism impacts, Bishoftutown. INTRODUCTION Tourism is widely perceived as an economic positives, it can also be the cause of a lot of problems in development tool for the local community, providing the local societies. -

GREAT ETHIOPIAN ROUTES the East - Danakil, Harar and Bale Mountains © Ethiopian Tourism Organization
GREAT ETHIOPIAN ROUTES The East - Danakil, Harar and Bale Mountains © Ethiopian Tourism Organization. Version V1.0 1115 Version Organization. Tourism © Ethiopian www.ethiopia.travel Text: Philip Briggs; Photography: David Kirkland, Aziz Ahmed, Ludwig Siege, Antonio Fiorente Antonio Kirkland, David Siege, Briggs; Photography: Philip Aziz Ludwig Ahmed, Text: The East - Danakil, Harar and Bale Mountains • The scorching Danakil, where salt-bearing camel caravans traipse mirage-like across blinding-white salt-flats, swept by a gale known as the Gara, or Fire Wind. • Volatile Erta Ale, its volcanic caldera cradling a bubbling cauldron of molten black lava and eruptive glowing fountains of red-hot magma. • The labyrinthine alleys of Harar Jugol, an ancient walled citadel with a wealth of Islamic mosques and shrines, bustling markets overhung with aromatic spices and cafes brewing freshly-roasted coffee plucked from the surrounding hills. • The Afro-Alpine moorland of the Sanetti Plateau in Bale Mountains, where handsome red Ethiopian wolves - the world’s most endangered canids - trot jauntily through the pastel-shaded heather. • The cool damp Harenna Forest in Bale Mountains, a vast tract of gnarled tree heathers, towering bamboo clumps and a canopy of evergreen foliage. • A rapier-horned oryx antelope cantering across wide open plains of Awash National Park, a group of colourfully dressed sellers in Dire Dawa open-air market, the immense limestone caverns of Sof Omar. This is Eastern Ethiopia. A land of astonishing geographic extremes, where the austere lavascapes and salt-flats of the northern Rift Valley, which plunges to 116m below sea level in the Danakil, contrast with the misty peaks of the Bale Mountains, which rise over 4,300m a short distance further south. -

On Farm Production Systems Characterization of Indigenous Cattle in Bako Tibe and Gobu Sayo Districts of Oromia Region, Ethiopia
Journal of Biology, Agriculture and Healthcare www.iiste.org ISSN 2224-3208 (Paper) ISSN 2225-093X (Online) Vol.6, No.22, 2016 On Farm Production Systems Characterization of Indigenous Cattle in Bako Tibe and Gobu Sayo Districts of Oromia Region, Ethiopia Dereje Bekele 1 Kefelegn Kebede 2 A.K. Banarjee 2 1.Oromia Agricultural research Institute, Bako Agricultural Research center, Bako, Ethiopia 2.Haramaya University, School of Animal and Range Sciences, Haramaya, Ethiopia Abstract The study was conducted in Bako Tibe and Gobu Sayo districts of Oromia Regional State, Ethiopia, from October 2014 to January 2015 with the objective to undertake on-farm production system characterization of indigenous cattle breed (Horro) in the study area. Field studies and collection of data were carried out through semi-structured questionnaire, focus group discussions, key informants and secondary data collection from different sources. A total of 120 households (60 from each district) were randomly selected for semi structured questionnaire interview. SAS and SPSS software were used to analyze the data. The study result revealed that overall cattle herd size was 9.67±3.34 heads per household and was not significantly different (p<0.05) between districts. The main purposes of keeping Horro cattle in both locations were draught power, milk production, income, manure and threshing of crop. The age at first service (AFS) of male Horro cattle was 3.47±0.39 years. The age at first mating (AFM) and age at first calving (AFC) of female cattle were 3.73±0.51 and 4.98±0.68 years respectively. The calving interval (CI) of Horro cow was estimated to be 1.88±0.49 years and showed no significant difference between locations. -

Determinants of Dairy Product Market Participation of the Rural Households
ness & Fi si na u n c B Gemeda et al, J Bus Fin Aff 2018, 7:4 i f a o l l A a Journal of f DOI: 10.4172/2167-0234.1000362 f n a r i r u s o J ISSN: 2167-0234 Business & Financial Affairs Research Article Open Access Determinants of Dairy Product Market Participation of the Rural Households’ The Case of Adaberga District in West Shewa Zone of Oromia National Regional State, Ethiopia Dirriba Idahe Gemeda1, Fikiru Temesgen Geleta2 and Solomon Amsalu Gesese3 1Department of Agricultural Economics, College of Agriculture and Veterinary Sciences, Ambo University, Ethiopia 2Department of Agribusiness and Value Chain Management, College of Agriculture and Veterinary Sciences, Ambo University, Ethiopia Abstract Ethiopia is believed to have the largest Livestock population in Africa. Dairy has been identified as a priority area for the Ethiopian government, which aims to increase Ethiopian milk production at an average annual growth rate of 15.5% during the GTP II period (2015-2020), from 5,304 million litters to 9,418 million litters. This study was carried out to assess determinants of dairy product market participation of the rural households in the case of Adaberga district in West Shewa zone of Oromia national regional state, Ethiopia. The study took a random sample of 120 dairy producer households by using multi-stage sampling procedure and employing a probability proportional to sample size sampling technique. For the individual producer, the decision to participate or not to participate in dairy production was formulated as binary choice probit model to identify factors that determine dairy product market participation. -

Gone in 6 Minutes: an Ethiopian Airlines Jet's Final Journey 5 April 2019, by David Koenig
Gone in 6 minutes: an Ethiopian Airlines jet's final journey 5 April 2019, by David Koenig Ethiopian authorities issued a preliminary report Thursday on the March 10 crash that killed 157 people. They found that a malfunctioning sensor sent faulty data to the Boeing 737 Max 8's anti-stall system and triggered a chain of events that ended in a crash so violent it reduced the plane to shards and pieces. The pilots' struggle, and the tragic ending, mirrored an Oct. 29 crash of a Lion Air Max 8 off the coast of Indonesia, which killed 189 people. The anti-stall system, called MCAS, automatically lowers the plane's nose under some circumstances to prevent an aerodynamic stall. Boeing acknowledged that a sensor in the Ethiopian Airlines jet malfunctioned, triggering MCAS when it was not needed. The company repeated that it is In this Monday, March 11, 2019 file photo, rescuers work working on a software upgrade to fix the problem in at the scene of an Ethiopian Airlines flight crash near its best-selling plane. Bishoftu, or Debre Zeit, south of Addis Ababa, Ethiopia. Pilots of the Ethiopian Airlines flight encountered "It's our responsibility to eliminate this risk," CEO problems with their new Boeing jetliner from nearly the Dennis Muilenburg said in a video. "We own it, and moment they roared down the runway and took off. we know how to do it." Ethiopian authorities issued a preliminary report Thursday, April 4, 2019, on the March 10 crash. (AP Photo/Mulugeta Ayene, File) From nearly the moment they roared down the runway and took off in their new Boeing jetliner, the pilots of Ethiopian Airlines Flight 302 encountered problems with the plane. -

Globalization: Global Politics and Culture (Msc)
LAND GRAB IN ETHIOPIA: THE CASE OF KARUTURI AGRO PRODUCTS PLC IN BAKO TIBE, OROMIYA Dejene Nemomsa Aga Supervisor: Professor Lund Ragnhild Master Thesis Faculty of Social Sciences and Technology Management Department of Geography Globalization: Global Politics and Culture (MSc). May 2014, Trondheim, Norway Globalization: Global Politics and Culture (M.Sc) Declaration I, the undersigned, declare that this thesis is my original work and all materials used as a source are duly acknowledged. Name:........................ Dejene Nemomsa Aga Date:……………........... 23 May, 2014 Dejene Nemomsa Aga Page i Globalization: Global Politics and Culture (M.Sc) Dedication I dedicate my master thesis work to anti-land grabbing protesters of Oromo Students and People, who were recently killed while protesting the implementation of ‘Integrated Development Master Plan of the Capital City of the country, Finfinne’, which planned to displace more than one million indigenous Oromo People from their ancestral land. 23 May, 2014 ii Dejene Nemomsa Aga Globalization: Global Politics and Culture (M.Sc) Acknowledgements Firsts, I would like to thank the almighty God. Next, my special thanks go to my advisor Professor Ragnhild Lund, for her guidance and detailed constructive comments that strengthened the quality of this thesis. Professor’s countless hours of reflecting, reading, encouraging, and patience throughout the entire process of the research is unforgettable. I would like to thank Norwegian University of Science and Technology for accepting me as a Quota Scheme Student to exchange knowledge with students who came from across the globe and Norwegian State Educational Loan Fund for covering all my financial expenses during my stay. My special thanks go to department of Geography, and Globalization: Global Politics and Culture program coordinators, Anette Knutsen for her regular meetings and advice in the research processes. -

ETHIOPIA Selfhelpafrica.Org 2020-21 1 2020-21 Alemnesh Tereda, 28, and Marsenesh Lenina, 29, Injaffo Multi Barley Coop, Gumer
ETHIOPIA selfhelpafrica.org 2020-21 1 2020-21 Alemnesh Tereda, 28, and Marsenesh Lenina, 29, Injaffo Multi barley Coop, Gumer caling up agricultural production, improving nutrition Last year, the organisation was involved in implementing security, developing new enterprise and market close to a dozen development projects, all of which Sopportunities for farmers, strengthening community- are being undertaken in collaboration with local and/or based seed production and building climate resilience, are international partners. all key areas of Self Help Africa’s work in Ethiopia. ETHIOPIA PROJECT KEY Scaling up RuSACCOs Strengthening & Scaling up of rehabilitaion of degraded lands and enhancement of livelihoods in Lake Ziway catchment ERITREA Feed the Future Gondar Dairy for Development Stronger Together: Linking Primary Seed and Seep Cooperative Union Addis Ababa Climate-Smart Agriculture SOMALILAND Capacity Building of Farmer Butajira Training Centers Unleashing the productive ETHIOPIA capacity of poor people through Graduation Approach in Ethiopia Integrated Community Development SOMALIA Livelihood Enhancement: Working Inclusively for Transformation KENYA 2 Implementing Programme Programme Donor Total Budget Time Frame Partner Area Climate-Smart Irish Aid € 806,695 2015 SOS Sahel, SNNP region 01 Agriculture (CSA) Farm Africa, 2019 Vita MF: Scaling Up Irish League of € 420,000 2020 Zonal Departments of N/Shewa Zone of 02 Rural Savings and Credit international Finance & Economic Amhara, N/Shewa Credit Cooperatives Development 2022 Cooperation -

Oromia Region Administrative Map(As of 27 March 2013)
ETHIOPIA: Oromia Region Administrative Map (as of 27 March 2013) Amhara Gundo Meskel ! Amuru Dera Kelo ! Agemsa BENISHANGUL ! Jangir Ibantu ! ! Filikilik Hidabu GUMUZ Kiremu ! ! Wara AMHARA Haro ! Obera Jarte Gosha Dire ! ! Abote ! Tsiyon Jars!o ! Ejere Limu Ayana ! Kiremu Alibo ! Jardega Hose Tulu Miki Haro ! ! Kokofe Ababo Mana Mendi ! Gebre ! Gida ! Guracha ! ! Degem AFAR ! Gelila SomHbo oro Abay ! ! Sibu Kiltu Kewo Kere ! Biriti Degem DIRE DAWA Ayana ! ! Fiche Benguwa Chomen Dobi Abuna Ali ! K! ara ! Kuyu Debre Tsige ! Toba Guduru Dedu ! Doro ! ! Achane G/Be!ret Minare Debre ! Mendida Shambu Daleti ! Libanos Weberi Abe Chulute! Jemo ! Abichuna Kombolcha West Limu Hor!o ! Meta Yaya Gota Dongoro Kombolcha Ginde Kachisi Lefo ! Muke Turi Melka Chinaksen ! Gne'a ! N!ejo Fincha!-a Kembolcha R!obi ! Adda Gulele Rafu Jarso ! ! ! Wuchale ! Nopa ! Beret Mekoda Muger ! ! Wellega Nejo ! Goro Kulubi ! ! Funyan Debeka Boji Shikute Berga Jida ! Kombolcha Kober Guto Guduru ! !Duber Water Kersa Haro Jarso ! ! Debra ! ! Bira Gudetu ! Bila Seyo Chobi Kembibit Gutu Che!lenko ! ! Welenkombi Gorfo ! ! Begi Jarso Dirmeji Gida Bila Jimma ! Ketket Mulo ! Kersa Maya Bila Gola ! ! ! Sheno ! Kobo Alem Kondole ! ! Bicho ! Deder Gursum Muklemi Hena Sibu ! Chancho Wenoda ! Mieso Doba Kurfa Maya Beg!i Deboko ! Rare Mida ! Goja Shino Inchini Sululta Aleltu Babile Jimma Mulo ! Meta Guliso Golo Sire Hunde! Deder Chele ! Tobi Lalo ! Mekenejo Bitile ! Kegn Aleltu ! Tulo ! Harawacha ! ! ! ! Rob G! obu Genete ! Ifata Jeldu Lafto Girawa ! Gawo Inango ! Sendafa Mieso Hirna -
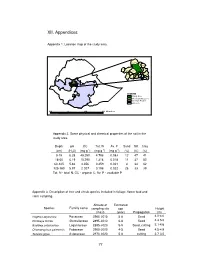
XII. Appendices
XII. Appendices Appendix 1. Location map of the study area. Ginde Beret Meta Robi Adaa Berga Study Area Ejere Bako Tibe Welmera Chelia Ambo Tikur Dawo Illu Alem Gana Da no Wenchi Becho Nonno Tolle Ameya Welisona Gorro Kokir Kersana Kondelt Gin de B e re t Met a Ro bi Ad aa Be rga Study Ar ea Ejere We lme ra Ba ko T ibe Ch el i a Amb o YA#ddis A baba Ti ku r Da wo Il lu Al em Ga na Da no We nch i No nn o Ame ya Be ch o To le We li so na Ke rsan a Gorro Ko nd elt LEGEND Study Area West Shewa Zone Oromya Region Ethiopia 400 0 400 800 Kilometers Appendix 2. Some physical and chemical properties of the soil in the study area. Depth pH OC Tot. N Av. P Sand Silt Clay -1 -1 -1 (cm) (H2O) (mg g ) (mg g ) (mg g ) (%) (%) (%) 0-18 6.28 48.280 4.796 0.083 12 47 41 18-60 6.19 15.290 1.316 0.018 11 37 52 60-125 5.66 4.356 0.459 0.021 4 34 62 125-160 5.97 2.027 0.198 0.022 28 33 39 Tot. N - total N, OC - organic C, Av. P - available P Appendix 3. Description of tree and shrub species included in foliage, flower bud and stem sampling. Altitude of Estimated Species Familly name sampling site age Height (masl) (year) Propagation (m) Hagenia abyssinica Rosaceae 2960-3015 5-8 Seed 4.0-4.6 Dombeya torrida Sterculiaceae 2895-3010 6-8 Seed 4.3-5.0 Buddleja polystachya Loganiaceae 2895-3020 5-9 Seed, cutting 3.1-4.6 Chamaecytisus palmensis Fabaceae 2900-3000 4-5 Seed 4.5-4.9 Senecio gigas Asteraceae 2970-3020 5-8 cutting 2.7-3.5 77 Appendix 4. -

Somali Region
Food Supply Prospects FOR THE SECOND HALF OF YEAR 2013 ______________________________________________________________________________ Disaster Risk Management and Food Security Sector (DRMFSS) Ministry of Agriculture (MoA) September, 2013 Addis Ababa, Ethiopia TABLE OF CONTENTS GLOSSARY OF LOCAL NAMES .................................................................. 1 ACRONYMS ............................................................................................. 2 EXCUTIVE SUMMARY .............................................................................. 3 INTRODUCTION ....................................................................................... 7 REGIONAL SUMMARY OF FOOD SUPPLY PROSPECT ............................. 11 SOMALI .............................................................................................. 11 OROMIA ............................................................................................. 16 TIGRAY ............................................................................................... 22 AMHARA ............................................................................................ 25 AFAR .................................................................................................. 28 SNNP .................................................................................................. 32 Annex – 1: NEEDY POPULATION AND FOOD REQUIREMENT BY WOREDA (Second half of 2013) ............................................................................ 35 0 | P a g e GLOSSARY -

Ethiopia: Administrative Map (August 2017)
Ethiopia: Administrative map (August 2017) ERITREA National capital P Erob Tahtay Adiyabo Regional capital Gulomekeda Laelay Adiyabo Mereb Leke Ahferom Red Sea Humera Adigrat ! ! Dalul ! Adwa Ganta Afeshum Aksum Saesie Tsaedaemba Shire Indasilase ! Zonal Capital ! North West TigrayTahtay KoraroTahtay Maychew Eastern Tigray Kafta Humera Laelay Maychew Werei Leke TIGRAY Asgede Tsimbila Central Tigray Hawzen Medebay Zana Koneba Naeder Adet Berahile Region boundary Atsbi Wenberta Western Tigray Kelete Awelallo Welkait Kola Temben Tselemti Degua Temben Mekele Zone boundary Tanqua Abergele P Zone 2 (Kilbet Rasu) Tsegede Tselemt Mekele Town Special Enderta Afdera Addi Arekay South East Ab Ala Tsegede Mirab Armacho Beyeda Woreda boundary Debark Erebti SUDAN Hintalo Wejirat Saharti Samre Tach Armacho Abergele Sanja ! Dabat Janamora Megale Bidu Alaje Sahla Addis Ababa Ziquala Maychew ! Wegera Metema Lay Armacho Wag Himra Endamehoni Raya Azebo North Gondar Gonder ! Sekota Teru Afar Chilga Southern Tigray Gonder City Adm. Yalo East Belesa Ofla West Belesa Kurri Dehana Dembia Gonder Zuria Alamata Gaz Gibla Zone 4 (Fantana Rasu ) Elidar Amhara Gelegu Quara ! Takusa Ebenat Gulina Bugna Awra Libo Kemkem Kobo Gidan Lasta Benishangul Gumuz North Wello AFAR Alfa Zone 1(Awsi Rasu) Debre Tabor Ewa ! Fogera Farta Lay Gayint Semera Meket Guba Lafto DPubti DJIBOUTI Jawi South Gondar Dire Dawa Semen Achefer East Esite Chifra Bahir Dar Wadla Delanta Habru Asayita P Tach Gayint ! Bahir Dar City Adm. Aysaita Guba AMHARA Dera Ambasel Debub Achefer Bahirdar Zuria Dawunt Worebabu Gambela Dangura West Esite Gulf of Aden Mecha Adaa'r Mile Pawe Special Simada Thehulederie Kutaber Dangila Yilmana Densa Afambo Mekdela Tenta Awi Dessie Bati Hulet Ej Enese ! Hareri Sayint Dessie City Adm.