Early Accreta and Uterine Rupture in the Second Trimester
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Placental Abruption
Placental Abruption Definition: Placental separation, either partial or complete prior to the birth of the fetus Incidence 0.5 – 1% (4). Risk factors include hypertension, smoking, preterm premature rupture of membranes, cocaine abuse, uterine myomas, and previous abruption (5). Diagnosis: Symptoms (may present with any or all of these) o Vaginal bleeding (usually dark and non-clotting). o Abdominal pain and/or back pain varying from intermittent to severe. o Uterine contractions are usually present and may vary from low amplitude/high frequency to hypertonus. o Fetal distress or fetal death. Ultrasound o Adherent retroplacental clot OR may just appear to be a thick placenta o Resolving hematomas become hypoechoic within one week and sonolucent within 2 weeks May be a diagnosis of exclusion if vaginal bleeding and no other identified etiology Consider in differential with uterine irritability on toco and cat II-III tracing, as small proportion present without bleeding Classification: Grade I: Slight vaginal bleeding and some uterine irritability are usually present. Maternal blood pressure, and fibrinogen levels are unaffected. FHR remains normal. Grade II: Mild to moderate vaginal bleeding seen; tetanic contractions may be present. Blood pressure usually normal, but tachycardia may be present. May be postural hypotension. Decreased fibrinogen; with levels below 250 mg percent; may be evidence of fetal distress. Reviewed 01/16/2020 1 Updated 01/16/2020 Grade III: Bleeding is moderate to severe, but may be concealed. Uterus tetanic and painful. Maternal hypotension usually present. Fetal death has occurred. Fibrinogen levels are less then 150 mg percent with thrombocytopenia and coagulation abnormalities. -
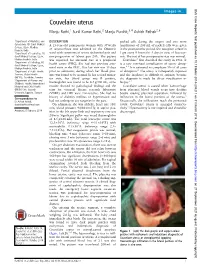
Couvelaire Uterus Manju Rathi,1 Sunil Kumar Rathi,2 Manju Purohit,3,4 Ashish Pathak2,5
BMJ Case Reports: first published as 10.1136/bcr-2014-204211 on 31 March 2014. Downloaded from Images in… Couvelaire uterus Manju Rathi,1 Sunil Kumar Rathi,2 Manju Purohit,3,4 Ashish Pathak2,5 1Department of Obstetrics and DESCRIPTION packed cells during the surgery and two more Gynecology, RD Gardi Medical A 23-year-old primiparous woman with 37 weeks transfusions of 200 mL of packed cells were given College, Ujjain, Madhya Pradesh, India of amenorrhoea was admitted to the Obstetric in the postoperative period. She was given cefazolin 2Department of Peadiatrics, RD ward with symptoms of severe abdominal pain and 1 gm every 8 hours for 5 days in view of leucocyt- Gardi Medical College, Ujjain, non-progression of labour past 20 h. The patient osis. The rest of her postoperative stay was normal. Madhya Pradesh, India 1 fi 3 was registered for antenatal care at a peripheral Couvelaire rst described the entity in 1911. It Department of Pathology, RD health centre (PHC). She had two previous ante- is a rare non-fatal complication of severe abrup- Gardi Medical College, Ujjain, 23 Madhya Pradesh, India natal visits at the PHC. Her last visit was 15 days tion. It is estimated to complicate 5% of all cases 2 4Department of Public Health prior to admission, during which her blood pres- of abruption. The entity is infrequently reported Sciences, Global Health sure was found to be normal. In her second trimes- and the incidence is difficult to estimate because (IHCAR), Stockholm, Sweden 5 ter visit, her blood group was B positive, the diagnosis is made by direct visualisation or Department of Women and 23 Children’s Health, International haemoglobin was found to be 8.5 g/100 mL, urine biopsy. -

Uterine Rupture After Misoprostol Use for Termination of Pregnancy in Second Trimester with Previous Caesarean Section: a Case Report Marjan Ghaemi*
Case Report iMedPub Journals Critical Care Obstetrics and Gynecology 2018 http://www.imedpub.com/ Vol.4 No.3:14 ISSN 2471-9803 DOI: 10.21767/2471-9803.1000167 Uterine Rupture after Misoprostol Use for Termination of Pregnancy in Second Trimester with Previous Caesarean Section: A Case Report Marjan Ghaemi* Yas Hospital, Tehran University of Medical Sciences, Tehran, Iran *Corresponding author: Marjan Ghaemi, Yas Hospital, Tehran University of Medical Sciences, Tehran, Iran, Tel: 0098-912-1967735; E-mail: [email protected] Received date: September 25, 2018; Accepted date: October 16, 2018; Published date: October 22, 2018 Copyright: © 2018 Ghaemi M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Citation: Ghaemi M (2018) Uterine Rupture after Misoprostol Use for Termination of Pregnancy in Second Trimester with Previous Caesarean Section: A Case Report. Crit Care Obst Gyne Vol.4 No.3:14. cesarean section, hospitalized for severe oligohydramnios with unknown etiology and no history of fluid leakage. In her Abstract previous surgical history, she mentioned laparoscopic cholecystectomy 10 years ago. Considering her medical history Modalities for termination of pregnancy may result in some and normal kidney and bladder in fetal ultrasound, we did not adverse effects especially uterine rupture in women with have proved data for her severe oligohydramnios. Amnio- the previous cesarean section. Here we report uterine infusion was performed to prevent foetal cord compression and rupture in the 23rd week of pregnancy after Misoprostol uses for abortion induction in second pregnancy with the to assess foetal structures. -

Management of Prolonged Decelerations ▲
OBG_1106_Dildy.finalREV 10/24/06 10:05 AM Page 30 OBGMANAGEMENT Gary A. Dildy III, MD OBSTETRIC EMERGENCIES Clinical Professor, Department of Obstetrics and Gynecology, Management of Louisiana State University Health Sciences Center New Orleans prolonged decelerations Director of Site Analysis HCA Perinatal Quality Assurance Some are benign, some are pathologic but reversible, Nashville, Tenn and others are the most feared complications in obstetrics Staff Perinatologist Maternal-Fetal Medicine St. Mark’s Hospital prolonged deceleration may signal ed prolonged decelerations is based on bed- Salt Lake City, Utah danger—or reflect a perfectly nor- side clinical judgment, which inevitably will A mal fetal response to maternal sometimes be imperfect given the unpre- pelvic examination.® BecauseDowden of the Healthwide dictability Media of these decelerations.” range of possibilities, this fetal heart rate pattern justifies close attention. For exam- “Fetal bradycardia” and “prolonged ple,Copyright repetitive Forprolonged personal decelerations use may onlydeceleration” are distinct entities indicate cord compression from oligohy- In general parlance, we often use the terms dramnios. Even more troubling, a pro- “fetal bradycardia” and “prolonged decel- longed deceleration may occur for the first eration” loosely. In practice, we must dif- IN THIS ARTICLE time during the evolution of a profound ferentiate these entities because underlying catastrophe, such as amniotic fluid pathophysiologic mechanisms and clinical 3 FHR patterns: embolism or uterine rupture during vagi- management may differ substantially. What would nal birth after cesarean delivery (VBAC). The problem: Since the introduction In some circumstances, a prolonged decel- of electronic fetal monitoring (EFM) in you do? eration may be the terminus of a progres- the 1960s, numerous descriptions of FHR ❙ Complete heart sion of nonreassuring fetal heart rate patterns have been published, each slight- block (FHR) changes, and becomes the immedi- ly different from the others. -

Antepartum Haemorrhage
OBSTETRICS AND GYNAECOLOGY CLINICAL PRACTICE GUIDELINE Antepartum haemorrhage Scope (Staff): WNHS Obstetrics and Gynaecology Directorate staff Scope (Area): Obstetrics and Gynaecology Directorate clinical areas at KEMH, OPH and home visiting (e.g. Community Midwifery Program) This document should be read in conjunction with this Disclaimer Contents Initial management: MFAU APH QRG ................................................. 2 Subsequent management of APH: QRG ............................................. 5 Management of an APH ........................................................................ 7 Key points ............................................................................................................... 7 Background information .......................................................................................... 7 Causes of APH ....................................................................................................... 7 Defining the severity of an APH .............................................................................. 8 Initial assessment ................................................................................................... 8 Emergency management ........................................................................................ 9 Maternal well-being ................................................................................................. 9 History taking ....................................................................................................... -

Concurrent Intraoperative Uterine Rupture and Placenta Accreta. Do
Concurrent intraoperative uterine rupture and placenta accreta Romanian Journal of Anaesthesia and Intensive Care 2018 Vol 25 No 1, 83-85 CASE REPORT DOI: http://dx.doi.org/10.21454/rjaic.7518.251.acc Concurrent intraoperative uterine rupture and placenta accreta. Do preoperative chronic hypertension, preterm premature rupture of membranes, chorioamnionitis, and placental abruption provide warning to this rare occurrence? M. Anthony Cometa, Scott M. Wasilko, Adam L. Wendling Department of Anesthesiology, Division of Obstetric Anesthesiology, University of Florida College of Medicine, Gainesville, FL, USA Abstract Uterine and placental pathology can be a major cause of morbidity and mortality in the parturient and infant. When presenting alone, placental abruption, uterine rupture, or placenta accreta can result in significant peripartum hemorrhage, requiring aggressive surgical and anesthetic management; however, the presence of multiple concurrent uterine and placental pathologies can result in significant morbidity and mortality. We present the anesthetic management of a parturient who underwent an urgent cesarean delivery for non- reassuring fetal tracing in the setting of chronic hypertension, preterm premature rupture of membranes, and chorioamnionitis who was subsequently found to have placental abruption, uterine rupture, and placenta accreta. Keywords: preterm premature rupture of membranes (PPROM), chorioamnionitis, placental abruption, uterine rupture, placenta accrete, cesarean-hysterectomy Received: 14 March 2018 / Accepted: 30 March 2018 Rom J Anaesth Intensive Care 2018; 25: 83-85 operative bleeding that requires aggressive fluid and blood product management and resuscitation [5]. At present, the literature does not reference the Introduction presentation and anesthetic management of these aforementioned conditions being concurrently present Various placental and uterine pathologies can result in one parturient. -

OBGYN-Study-Guide-1.Pdf
OBSTETRICS PREGNANCY Physiology of Pregnancy: • CO input increases 30-50% (max 20-24 weeks) (mostly due to increase in stroke volume) • SVR anD arterial bp Decreases (likely due to increase in progesterone) o decrease in systolic blood pressure of 5 to 10 mm Hg and in diastolic blood pressure of 10 to 15 mm Hg that nadirs at week 24. • Increase tiDal volume 30-40% and total lung capacity decrease by 5% due to diaphragm • IncreaseD reD blooD cell mass • GI: nausea – due to elevations in estrogen, progesterone, hCG (resolve by 14-16 weeks) • Stomach – prolonged gastric emptying times and decreased GE sphincter tone à reflux • Kidneys increase in size anD ureters dilate during pregnancy à increaseD pyelonephritis • GFR increases by 50% in early pregnancy anD is maintaineD, RAAS increases = increase alDosterone, but no increaseD soDium bc GFR is also increaseD • RBC volume increases by 20-30%, plasma volume increases by 50% à decreased crit (dilutional anemia) • Labor can cause WBC to rise over 20 million • Pregnancy = hypercoagulable state (increase in fibrinogen anD factors VII-X); clotting and bleeding times do not change • Pregnancy = hyperestrogenic state • hCG double 48 hours during early pregnancy and reach peak at 10-12 weeks, decline to reach stead stage after week 15 • placenta produces hCG which maintains corpus luteum in early pregnancy • corpus luteum produces progesterone which maintains enDometrium • increaseD prolactin during pregnancy • elevation in T3 and T4, slight Decrease in TSH early on, but overall euthyroiD state • linea nigra, perineum, anD face skin (melasma) changes • increase carpal tunnel (median nerve compression) • increased caloric need 300cal/day during pregnancy and 500 during breastfeeding • shoulD gain 20-30 lb • increaseD caloric requirements: protein, iron, folate, calcium, other vitamins anD minerals Testing: In a patient with irregular menstrual cycles or unknown date of last menstruation, the last Date of intercourse shoulD be useD as the marker for repeating a urine pregnancy test. -

Are Maternal and Neonatal Outcomes Different in Placental Abruption
Placenta 85 (2019) 69–73 Contents lists available at ScienceDirect Placenta journal homepage: www.elsevier.com/locate/placenta Are maternal and neonatal outcomes different in placental abruption T between women with and without preeclampsia? Min Hana, Dan Liua, Shahn Zebb, Chunfang Lia, Mancy Tongc, Xuelan Lia,**, Qi Chend,e,* a Department of Obstetrics & Gynaecology, First affiliated hospital of Xi'an Jiaotong University, China b Xi'an Jiaotong University, Xi'an, China c Department of Obstetrics, Gynecology and Reproductive Sciences, Yale School of Medicine, New Haven, CT, USA d The Hospital of Obstetrics & Gynaecology, Fudan University China, China e Department of Obstetrics & Gynaecology, The University of Auckland, New Zealand ARTICLE INFO ABSTRACT Keywords: Introduction: Placental abruption is a serious pregnancy complication that causes maternal and neonatal mor- Placental abruption tality and morbidity. Whether maternal and neonatal outcomes differ between patients who concurrently pre- Preeclampsia sented with preeclampsia and those who did not, have not been fully investigated. Maternal fetal and neonatal outcomes Methods: A total number of 158 patients with placental abruption were included. Of them, 66 concurrently had preeclampsia. Maternal and neonatal characteristics including delivery weeks, time of onset and birthweight as well as the grade of placental abruption were collected and analysed. Results: The time at diagnosis of placental abruption in patients who concurrently presented preeclampsia was significantly earlier than that in patients who did not. The number of patients with grade III placental abruption was significantly higher in patients who concurrently presented with preeclampsia, compared to patients who did not. The odds ratio of an increase in grade III placental abruption in patients who concurrently presented preeclampsia was 5.27 (95%CL: 2.346, 12.41), compared to patients who did not. -

A Rare Case of Placenta Percreta Causing Uterine Rupture and Massive Haemoperitoneum in 2Nd Trimester: an Obvious Near Miss
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Parmar C et al. Int J Reprod Contracept Obstet Gynecol. 2021 Jun;10(6):2495-2497 www.ijrcog.org pISSN 2320-1770 | eISSN 2320-1789 DOI: https://dx.doi.org/10.18203/2320-1770.ijrcog20212201 Case Report A rare case of placenta percreta causing uterine rupture and massive haemoperitoneum in 2nd trimester: an obvious near miss Chirayu Parmar*, Mittal Parmar, Gayatri Desai Department of Gynecology, Kasturba Hospital, SEWA Rural, Jhagadi, Gujarat, India Received: 30 December 2020 Accepted: 05 May 2021 *Correspondence: Dr. Chirayu Parmar, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Placenta accreta spectrum is very rarely encountered with ruptured uterus and is commonly seen in third trimester of pregnancy. Hereby, a case of placenta percreta with uterine rupture in second trimester of pregnancy is presented. 40 year old women with previous 2 LSCS presented in emergency department with ninteen weeks pregnancy and massive haemoperitoneum. Emergency laprotomy revealed uterine rupture alnong with placenta percreta for which obstetric hysterectomy was done. Although, a rare occurrence, obstetricians should consider patients placenta accreta spectrum in -

Couvelaire Uterus ISSN: 2394-0026 (P) ISSN: 2394-0034 (O) Case Report
Couvelaire uterus ISSN: 2394-0026 (P) ISSN: 2394-0034 (O) Case Report Couvelaire uterus - A case report Mahendra G 1*, Ravindra S. Pukale 2, Vijayalakshmi S 3, Priya 4 1Assistant Professor, 2Associate professor, 3Professor and Head, 4Junior Resident Department of Obstetrics and Gynecology , Adichunchanagiri Institute of Medical S ciences, B.G. Nagara, India *Corresponding author email: [email protected] How to cite this article: Mahendra G , Ravindra S. Pukale, Vijayalakshmi S , Priya . Couvelaire uterus - A case report. IAIM, 2015; 2(3): 142 -145. Available online at www.iaimjournal.com Received on: 03-01-2015 Accepted on: 16-01-2015 Abstract “Couvelaire uterus” or “Utero-placental apoplexy” is a rare complication of severe forms of placental abruption. It occurs when vascular damage within the placenta causes hemorrhage that progresses to and infiltrates the wall of the uterus . We presented here rare case of 23 years old f emale with Couvelaire uterus. Key words Couvelaire uterus, Utero-placental apoplexy, Placental abruption. Introduction pregnancy induced hypertension ( PIH) in “Couvelaire uterus” or “Utero -placental previous pregnancy. Her personal and family apoplexy” is a rare complication of severe forms history was not significant. of placen tal abruption. It occurs when vascular damage within the placenta causes hemorrhage General examination • that progresses to and infiltrates the wall of the Pallor +++ uterus [1]. It is a syndrome that can only be • BP - 116/80 mm Hg in t he supine left diagnosed by direct visualization or biopsy (or lateral position both). For this reason, its occurrence is perhaps • Pulse rate - 108/min underreported and underestimated in the literature [2]. -

PREGNANCY in a RUDIMENTARY HORN of a UTERUS DIDELPHYS with Concealed Accidental Haemorrhage
PREGNANCY IN A RUDIMENTARY HORN OF A UTERUS DIDELPHYS With concealed accidental haemorrhage by VIMAL V. PARIKH*, M.D. (Born.) I Amongst all the malformations of own corresponding uterus - the right I ' ~ ( the female genital tract, perhaps the uterus and the cervix were well de ) rarest is a completely paired uterus veloped, but the left uterus was rudi I with each member of the pair having mentary and was attached to its cor its own cervix, opening into the cor responding vagina with an atretic responding member of the paired non-canalised cervix. There was a vaginae- that is uterus didelphys recto-vesical fold of peritoneum con (pseudo) with double vagina. (Very necting the rectum, with the bladder rarely still the uterus, the vagina and in between the two uteri. also the vulva ' are absolutely distinct There are 3 possible ways by which on the two sides - which is describ pregnancy can occur in a rudimentary ~d as true uterus didelphys). The horn- ( 1) through a small micro tubes, uterus and vagina are develop scopic cervical canal, (2) through a . ed from the two Mullerian ducts; the transperitoneal migration of the sper two ducts usually become fused, matozoa, or (3) through a trans except the uppermost parts which peritoneal migration of the fertilized form the two fallopian tubes. The ovum. varieties of malformation encounter The usual termination of a preg ed are very numerous and depend up nancy in a rudimentary horn is rup on the extent to which development ture, but few pregnancies are on re and fusion of the two halves, which cord which have continued to term I I should become blended, fail. -

Placental Abruption: Epidemiology, Risk Factors and Consequences
ACTA OVERVIEW Placental abruption: epidemiology, risk factors and consequences MINNA TIKKANEN Department of Obstetrics and Gynecology, University Central Hospital, Helsinki, Finland Key words Abstract Placental abruption, epidemiology, outcome, risk factor, consequence Placental abruption, classically defined as a premature separation of the placenta before delivery, is one of the leading causes of vaginal bleeding in the second half Correspondence of pregnancy. Approximately 0.4–1% of pregnancies are complicated by placental M. Tikkanen, Department of Obstetrics and abruption. The prevalence is lower in the Nordic countries (0.38–0.51%) compared Gynecology, University Central Hospital, 00029 with the USA (0.6–1.0%). Placental abruption is also one of the most important Helsinki, Finland. causes of maternal morbidity and perinatal mortality. Maternal risks include obstet- E-mail: minna.tikkanen@hus.fi ric hemorrhage, need for blood transfusions, emergency hysterectomy, disseminated Conflict of interest intravascular coagulopathy and renal failure. Maternal death is rare but seven times The author has stated explicitly that there are higher than the overall maternal mortality rate. Perinatal consequences include low no conflicts of interest in connection with this birthweight, preterm delivery, asphyxia, stillbirth and perinatal death. In developed article. countries, approximately 10% of all preterm births and 10–20% of all perinatal deaths are caused by placental abruption. In many countries, the rate of placen- Received: 27 August 2010 tal abruption has been increasing. Although several risk factors are known, the Accepted: 10 October 2010 etiopathogenesis of placental abruption is multifactorial and not well understood. DOI: 10.1111/j.1600-0412.2010.01030.x Abbreviations DIC, disseminated intravascular coagulopathy; IUGR, intrauterine growth restriction/retardation; PPROM, preterm premature rupture of the mem- branes ery, asphyxia, stillbirth and perinatal death (8).