A Role for SMARCB1 in Synovial Sarcomagenesis Reveals That SS18-SSX Induces Canonical BAF Destruction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
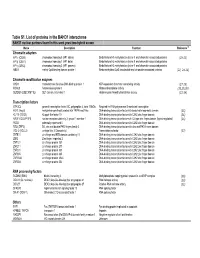
Table S1. List of Proteins in the BAHD1 Interactome
Table S1. List of proteins in the BAHD1 interactome BAHD1 nuclear partners found in this work yeast two-hybrid screen Name Description Function Reference (a) Chromatin adapters HP1α (CBX5) chromobox homolog 5 (HP1 alpha) Binds histone H3 methylated on lysine 9 and chromatin-associated proteins (20-23) HP1β (CBX1) chromobox homolog 1 (HP1 beta) Binds histone H3 methylated on lysine 9 and chromatin-associated proteins HP1γ (CBX3) chromobox homolog 3 (HP1 gamma) Binds histone H3 methylated on lysine 9 and chromatin-associated proteins MBD1 methyl-CpG binding domain protein 1 Binds methylated CpG dinucleotide and chromatin-associated proteins (22, 24-26) Chromatin modification enzymes CHD1 chromodomain helicase DNA binding protein 1 ATP-dependent chromatin remodeling activity (27-28) HDAC5 histone deacetylase 5 Histone deacetylase activity (23,29,30) SETDB1 (ESET;KMT1E) SET domain, bifurcated 1 Histone-lysine N-methyltransferase activity (31-34) Transcription factors GTF3C2 general transcription factor IIIC, polypeptide 2, beta 110kDa Required for RNA polymerase III-mediated transcription HEYL (Hey3) hairy/enhancer-of-split related with YRPW motif-like DNA-binding transcription factor with basic helix-loop-helix domain (35) KLF10 (TIEG1) Kruppel-like factor 10 DNA-binding transcription factor with C2H2 zinc finger domain (36) NR2F1 (COUP-TFI) nuclear receptor subfamily 2, group F, member 1 DNA-binding transcription factor with C4 type zinc finger domain (ligand-regulated) (36) PEG3 paternally expressed 3 DNA-binding transcription factor with -

Integrase Interactor 1 (INI-1) Deficient Renal Cell Carcinoma
Open Access Case Report DOI: 10.7759/cureus.13082 Integrase Interactor 1 (INI-1) Deficient Renal Cell Carcinoma Manpreet Singh 1 , Harkirat Singh 1 , Benjamin Hambro 1 , Jasleen Kaur 1 , Ravi Rao 2 1. Internal Medicine, St Agnes Medical Center, Fresno, USA 2. Hematology and Oncology, St Agnes Medical Center, Fresno, USA Corresponding author: Manpreet Singh, [email protected] Abstract Members of the SWItch/sucrose nonfermentable (SWI-SNF) family, including SWI/SNF related, matrix- associated, actin-dependent regulator of chromatin, subfamily A, member 4 (SMARCA4), SWI/SNF related, matrix‐associated, actin‐dependent regulator of chromatin, subfamily B member 1 (SMARCB1)/integrase interactor 1 (INI-1) are known tumor suppressor genes. Interactions between SMARCB1/INI-1 and key protein components in various cellular pathways are related to tumor progression and proliferation. SMARCB1/INI-1 protein was undetectable in rhabdoid tumor cells, whereas non-tumorous cells express the SMARCB1/INI-1 genes. Germline and sporadic mutations of several genes encoding for proteins in this complex are known to cause a spectrum of cancers, usually with sarcomatoid features which include a very aggressive renal medullary carcinoma. We report a case of a 29-year-old male who presented with SMARCA4 deficient renal tumor with a very aggressive clinical behavior which ultimately led to his death. Categories: Nephrology, Oncology Keywords: renal medullary carcinoma, ini-1, renal cell carcinoma, swi/snf, smarcb1, integrase interactor 1 Introduction Renal medullary carcinoma is a rare and very aggressive malignancy affecting young adults with rare cases in patients with sickle cell disease or trait [1]. The tumor arises predominantly in the renal medulla and exhibits a variety of growth patterns including reticular, solid, tubular, trabecular, cribriform, sarcomatoid, and micropapillary [1]. -

Bioinformatics Applications Through Visualization of Variations on Protein
1 Bioinformatics applications through visualization of variations on protein structures, comparative functional genomics, and comparative modeling for protein structure studies A dissertation presented by Alper Uzun to The Department of Biology In partial fulfillment of the requirements for the degree of Doctor of Philosophy in the field of Biology Northeastern University Boston, Massachusetts July 2009 2 ©2009 Alper Uzun ALL RIGHTS RESERVED 3 Bioinformatics applications through visualization of variations on protein structures, comparative functional genomics, and comparative modeling for protein structure studies by Alper Uzun ABSTRACT OF DISSERTATION Submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy in Biology in the Graduate School of Arts and Sciences of Northeastern University, July, 2009 4 Abstract The three-dimensional structure of a protein provides important information for understanding and answering many biological questions in molecular detail. The rapidly growing number of sequenced genes and related genomic information is intensively accumulating in the biological databases. It is significantly important to combine biological data and developing bioinformatics tools while information of protein sequences, structures and DNA sequences are exponentially growing. On the other hand, especially the number of known protein sequences is much larger than the number of experimentally solved protein structures. However the experimental methods cannot always be applied or protein structures -

Histone-Binding of DPF2 Mediates Its Repressive Role in Myeloid Differentiation
Histone-binding of DPF2 mediates its repressive role in myeloid differentiation Ferdinand M. Hubera,1, Sarah M. Greenblattb,1, Andrew M. Davenporta,1, Concepcion Martinezb,YeXub,LyP.Vuc, Stephen D. Nimerb,2, and André Hoelza,2 aDivision of Chemistry and Chemical Engineering, California Institute of Technology, Pasadena, CA 91125; bSylvester Comprehensive Cancer Center, University of Miami Miller School of Medicine, Miami, FL 33136; and cMolecular Pharmacology Program, Memorial Sloan Kettering Cancer Center, New York, NY 10065 Edited by Douglas C. Rees, Howard Hughes Medical Institute, California Institute of Technology, Pasadena, CA, and approved April 26, 2017 (received for review January 6, 2017) Double plant homeodomain finger 2 (DPF2) is a highly evolution- RUNX1 form a methylation-dependent repressive complex in arily conserved member of the d4 protein family that is ubiqui- AML, although it remains unclear whether the two proteins bind tously expressed in human tissues and was recently shown to each other directly or act concertedly as part of a larger complex. inhibit the myeloid differentiation of hematopoietic stem/progen- Here, we present the crystal structure of the human DPF2 itor and acute myelogenous leukemia cells. Here, we present the tandem PHD finger domain at a 1.6-Å resolution. We demon- crystal structure of the tandem plant homeodomain finger domain strate that the DPF2 tandem PHD finger domain binds acetylated of human DPF2 at 1.6-Å resolution. We show that DPF2 interacts H3 and H4 histone tails, identify the primary determinants of with the acetylated tails of both histones 3 and 4 via bipartite histone recognition, and confirm these interactions in vivo. -

Mediator of DNA Damage Checkpoint 1 (MDC1) Is a Novel Estrogen Receptor Co-Regulator in Invasive 6 Lobular Carcinoma of the Breast 7 8 Evelyn K
bioRxiv preprint doi: https://doi.org/10.1101/2020.12.16.423142; this version posted December 16, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC 4.0 International license. 1 Running Title: MDC1 co-regulates ER in ILC 2 3 Research article 4 5 Mediator of DNA damage checkpoint 1 (MDC1) is a novel estrogen receptor co-regulator in invasive 6 lobular carcinoma of the breast 7 8 Evelyn K. Bordeaux1+, Joseph L. Sottnik1+, Sanjana Mehrotra1, Sarah E. Ferrara2, Andrew E. Goodspeed2,3, James 9 C. Costello2,3, Matthew J. Sikora1 10 11 +EKB and JLS contributed equally to this project. 12 13 Affiliations 14 1Dept. of Pathology, University of Colorado Anschutz Medical Campus 15 2Biostatistics and Bioinformatics Shared Resource, University of Colorado Comprehensive Cancer Center 16 3Dept. of Pharmacology, University of Colorado Anschutz Medical Campus 17 18 Corresponding author 19 Matthew J. Sikora, PhD.; Mail Stop 8104, Research Complex 1 South, Room 5117, 12801 E. 17th Ave.; Aurora, 20 CO 80045. Tel: (303)724-4301; Fax: (303)724-3712; email: [email protected]. Twitter: 21 @mjsikora 22 23 Authors' contributions 24 MJS conceived of the project. MJS, EKB, and JLS designed and performed experiments. JLS developed models 25 for the project. EKB, JLS, SM, and AEG contributed to data analysis and interpretation. SEF, AEG, and JCC 26 developed and performed informatics analyses. MJS wrote the draft manuscript; all authors read and revised the 27 manuscript and have read and approved of this version of the manuscript. -

Genome-Wide CRISPR Screening Identifies BRD9 As a Druggable Component Of
bioRxiv preprint doi: https://doi.org/10.1101/2021.02.04.429732; this version posted February 4, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. 1 Genome-Wide CRISPR Screening Identifies BRD9 as a Druggable Component of 2 Interferon-Stimulated Gene Expression and Antiviral Activity 3 Jacob Börolda,b,†, Davide Elettoa,†,#, Idoia Busnadiegoa, Nina K. Maira,b, Eva Moritza, 4 Samira Schiefera,b, Nora Schmidta,$, Philipp P. Petricc,d, W. Wei-Lynn Wonge, Martin 5 Schwemmlec & Benjamin G. Halea,* 6 7 aInstitute of Medical Virology, University of Zurich, Zurich, Switzerland. 8 bLife Science Zurich Graduate School, ETH and University of Zurich, Zurich, 9 Switzerland. 10 cInstitute of Virology, Freiburg University Medical Center, Faculty of Medicine, University 11 of Freiburg, Freiburg, Germany. 12 dSpemann Graduate School of Biology and Medicine, University of Freiburg, Freiburg, 13 Germany. 14 eInstitute of Experimental Immunology, University of Zurich, Zurich, Switzerland. 15 *Correspondence: Benjamin G. Hale, [email protected] 16 †Equal first authors listed in alphabetical order. 17 #Present address: Department of Biosystems Science and Engineering, ETH Zurich, 18 Basel, Switzerland. 19 $Present address: Helmholtz Institute for RNA-based Infection Research, Helmholtz- 20 Center for Infection Research, Wurzburg, Germany. 1 bioRxiv preprint doi: https://doi.org/10.1101/2021.02.04.429732; this version posted February 4, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. -

Watsonjn2018.Pdf (1.780Mb)
UNIVERSITY OF CENTRAL OKLAHOMA Edmond, Oklahoma Department of Biology Investigating Differential Gene Expression in vivo of Cardiac Birth Defects in an Avian Model of Maternal Phenylketonuria A THESIS SUBMITTED TO THE GRADUATE FACULTY In partial fulfillment of the requirements For the degree of MASTER OF SCIENCE IN BIOLOGY By Jamie N. Watson Edmond, OK June 5, 2018 J. Watson/Dr. Nikki Seagraves ii J. Watson/Dr. Nikki Seagraves Acknowledgements It is difficult to articulate the amount of gratitude I have for the support and encouragement I have received throughout my master’s thesis. Many people have added value and support to my life during this time. I am thankful for the education, experience, and friendships I have gained at the University of Central Oklahoma. First, I would like to thank Dr. Nikki Seagraves for her mentorship and friendship. I lucked out when I met her. I have enjoyed working on this project and I am very thankful for her support. I would like thank Thomas Crane for his support and patience throughout my master’s degree. I would like to thank Dr. Shannon Conley for her continued mentorship and support. I would like to thank Liz Bullen and Dr. Eric Howard for their training and help on this project. I would like to thank Kristy Meyer for her friendship and help throughout graduate school. I would like to thank my committee members Dr. Robert Brennan and Dr. Lilian Chooback for their advisement on this project. Also, I would like to thank the biology faculty and staff. I would like to thank the Seagraves lab members: Jailene Canales, Kayley Pate, Mckayla Muse, Grace Thetford, Kody Harvey, Jordan Guffey, and Kayle Patatanian for their hard work and support. -
Modeling Renal Cell Carcinoma in Mice: Bap1 and Pbrm1 Inactivation Drive Tumor Grade
Published OnlineFirst May 4, 2017; DOI: 10.1158/2159-8290.CD-17-0292 RESEARCH ARTICLE Modeling Renal Cell Carcinoma in Mice: Bap1 and Pbrm1 Inactivation Drive Tumor Grade Yi-Feng Gu1,2, Shannon Cohn1,2, Alana Christie2, Tiffani McKenzie2,3, Nicholas Wolff1,2, Quyen N. Do4, Ananth J. Madhuranthakam4, Ivan Pedrosa2,4, Tao Wang2,5, Anwesha Dey6, Meinrad Busslinger7, Xian-Jin Xie2,8, Robert E. Hammer9, Renée M. McKay1,2, Payal Kapur2,3, and James Brugarolas1,2 Downloaded from cancerdiscovery.aacrjournals.org on September 26, 2021. © 2017 American Association for Cancer Research. 17-CD-17-0292_p900-917.indd 900 7/20/17 10:05 AM Published OnlineFirst May 4, 2017; DOI: 10.1158/2159-8290.CD-17-0292 ABSTRACT Clear cell renal cell carcinoma (ccRCC) is characterized by BAP1 and PBRM1 muta- tions, which are associated with tumors of different grade and prognosis. However, whether BAP1 and PBRM1 loss causes ccRCC and determines tumor grade is unclear. We conditionally targeted Bap1 and Pbrm1 (with Vhl ) in the mouse using several Cre drivers. Sglt2 and Villin proximal convoluted tubule drivers failed to cause tumorigenesis, challenging the conventional notion of ccRCC origins. In contrast, targeting with PAX8, a transcription factor frequently overexpressed in ccRCC, led to ccRCC of different grades. Bap1 -defi cient tumors were of high grade and showed greater mTORC1 activation than Pbrm1 -defi cient tumors, which exhibited longer latency. Disrupting one allele of the mTORC1 negative regulator, Tsc1 , in Pbrm1 -defi cient kidneys triggered higher grade ccRCC. This study establishes Bap1 and Pbrm1 as lineage-specifi c drivers of ccRCC and histologic grade, implicates mTORC1 as a tumor grade rheostat, and suggests that ccRCCs arise from Bowman capsule cells. -

The Impact of Chromosomal Translocation Locus and Fusion Oncogene Coding Sequence in Synovial Sarcomagenesis
Oncogene (2016) 35, 5021–5032 © 2016 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-9232/16 www.nature.com/onc ORIGINAL ARTICLE The impact of chromosomal translocation locus and fusion oncogene coding sequence in synovial sarcomagenesis KB Jones1,2,3, JJ Barrott1,2,3, M Xie4, M Haldar5, H Jin1,2,3, J-F Zhu1,2,3, MJ Monument1,3, TL Mosbruger3,6, EM Langer5, RL Randall1,3, RK Wilson4,7,8,9, BR Cairns2,3,10, L Ding4,7,8,9 and MR Capecchi5 Synovial sarcomas are aggressive soft-tissue malignancies that express chromosomal translocation-generated fusion genes, SS18-SSX1 or SS18-SSX2 in most cases. Here, we report a mouse sarcoma model expressing SS18-SSX1, complementing our prior model expressing SS18-SSX2. Exome sequencing identified no recurrent secondary mutations in tumors of either genotype. Most of the few mutations identified in single tumors were present in genes that were minimally or not expressed in any of the tumors. Chromosome 6, either entirely or around the fusion gene expression locus, demonstrated a copy number gain in a majority of tumors of both genotypes. Thus, by fusion oncogene coding sequence alone, SS18-SSX1 and SS18-SSX2 can each drive comparable synovial sarcomagenesis, independent from other genetic drivers. SS18-SSX1 and SS18-SSX2 tumor transcriptomes demonstrated very few consistent differences overall. In direct tumorigenesis comparisons, SS18-SSX2 was slightly more sarcomagenic than SS18-SSX1, but equivalent in its generation of biphasic histologic features. Meta-analysis of human synovial sarcoma patient series identified two tumor–gentoype–phenotype correlations that were not modeled by the mice, namely a scarcity of male hosts and biphasic histologic features among SS18-SSX2 tumors. -

Increased ACTL6A Occupancy Within Mswi/SNF Chromatin Remodelers
bioRxiv preprint doi: https://doi.org/10.1101/2021.03.22.435873; this version posted March 22, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Increased ACTL6A Occupancy Within mSWI/SNF Chromatin Remodelers Drives Human Squamous Cell Carcinoma Chiung-Ying Chang1,2,7, Zohar Shipony3,7, Ann Kuo1,2, Kyle M. Loh4,5, William J. Greenleaf3,6, Gerald R. Crabtree1,2,5* 1Howard Hughes Medical Institute, Stanford University School of Medicine, Stanford, California 94305, USA. 2Department of Pathology, Stanford University School of Medicine, Stanford, California 94305, USA. 3Department of Genetics, Stanford University School of Medicine, Stanford, California 94305, USA. 4Institute for Stem Cell Biology and Regenerative Medicine, Stanford University School of Medicine, Stanford, California 94305, USA. 5Department of Developmental Biology, Stanford University School of Medicine, Stanford, California 94305, USA. 6Department of Applied Physics, Stanford University, Stanford, California 94305, USA. 7These authors contributed equally. *Corresponding author: Gerald R. Crabtree, [email protected] Summary Mammalian SWI/SNF (BAF) chromatin remodelers play dosage-sensitive roles in many human malignancies and neurologic disorders. The gene encoding the BAF subunit, ACTL6A, is amplified at an early stage in the development of squamous cell carcinomas (SCCs), but its oncogenic role remains unclear. Here we demonstrate that ACTL6A overexpression leads to its stoichiometric assembly into BAF complexes and drives its interaction and engagement with specific regulatory regions in the genome. In normal epithelial cells, ACTL6A was sub-stoichiometric to other BAF subunits. However, increased ACTL6A levels by ectopic expression or in SCC cells led to near-saturation of ACTL6A within BAF complexes. -

Loss of Integrase Interactor 1 (INI1) Expression in a Subset of Differentiated Thyroid Cancer
diagnostics Article Loss of Integrase Interactor 1 (INI1) Expression in a Subset of Differentiated Thyroid Cancer Kung-Chen Ho 1, Jie-Jen Lee 1, Chi-Hsin Lin 2,3, Ching-Hsiang Leung 4 and Shih-Ping Cheng 1,5,* 1 Department of Surgery, MacKay Memorial Hospital and Mackay Medical College, Taipei 104215, Taiwan; [email protected] (K.-C.H.); [email protected] (J.-J.L.) 2 Department of Medical Research, MacKay Memorial Hospital, Taipei 104215, Taiwan; [email protected] 3 Department of Bioscience Technology, Chung Yuan Christian University, Taoyuan City 320314, Taiwan 4 Division of Endocrinology and Metabolism, Department of Internal Medicine, MacKay Memorial Hospital and Mackay Medical College, Taipei 104215, Taiwan; [email protected] 5 Department of Pharmacology, School of Medicine, College of Medicine, Taipei Medical University, Taipei 110301, Taiwan * Correspondence: [email protected]; Tel.: +886-2-2543-3535 Received: 19 April 2020; Accepted: 2 May 2020; Published: 5 May 2020 Abstract: Alterations in the switching defective/sucrose non-fermenting (SWI/SNF) chromatin-remodeling complex are enriched in advanced thyroid cancer. Integrase interactor 1 (INI1), encoded by the SMARCB1 gene on the long arm of chromosome 22, is one of the core subunits of the SWI/SNF complex. INI1 immunohistochemistry is frequently used for the diagnosis of malignant rhabdoid neoplasms. In the present study, we found normal and benign thyroid tissues generally had diffusely intense nuclear immunostaining. Loss of INI1 immunohistochemical expression was observed in 8% of papillary thyroid cancer and 30% of follicular thyroid cancer. Furthermore, loss of INI1 expression was associated with extrathyroidal extension (p < 0.001) and lymph node metastasis (p = 0.038). -

1 Canonical BAF Complex in Regulatory T Cells 2 3 Chin
bioRxiv preprint doi: https://doi.org/10.1101/2020.02.26.964981; this version posted February 27, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. 1 A genome-wide CRISPR screen reveals a role for the BRD9-containing non- 2 canonical BAF complex in regulatory T cells 3 4 Chin-San Loo1,3,#, Jovylyn Gatchalian2,#, Yuqiong Liang1, Mathias Leblanc1, Mingjun 5 Xie1, Josephine Ho2, Bhargav Venkatraghavan1, Diana C. Hargreaves2*, and Ye 6 Zheng1* 7 8 1. NOMIS Center for Immunobiology and Microbial Pathogenesis, Salk Institute for 9 Biological Studies 10 2. Molecular and Cellular Biology Laboratory, Salk Institute for Biological Studies 11 3. Division of Biological Sciences, University of California, San Diego 12 # Co-first authors 13 * Co-corresponding authors 14 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.02.26.964981; this version posted February 27, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. 15 Summary 16 Regulatory T cells (Tregs) play a pivotal role in suppressing auto-reactive T cells 17 and maintaining immune homeostasis. Treg development and function are 18 dependent on the transcription factor Foxp3. Here we performed a genome-wide 19 CRISPR/Cas9 knockout screen to identify the regulators of Foxp3 in mouse 20 primary Tregs. The results showed that Foxp3 regulators are highly enriched in 21 genes encoding SWI/SNF and SAGA complex subunits. Among the three 22 SWI/SNF-related complexes, the non-canonical or ncBAF (also called GBAF or 23 BRD9-containing BAF) complex promoted the expression of Foxp3, whereas the 24 PBAF complex repressed its expression.