ORIGINAL ARTICLE Flow Cytometric Protein Expression Profiling As a Systematic Approach for Developing Disease-Specific Assays
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Screening and Identification of Key Biomarkers in Clear Cell Renal Cell Carcinoma Based on Bioinformatics Analysis
bioRxiv preprint doi: https://doi.org/10.1101/2020.12.21.423889; this version posted December 23, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Screening and identification of key biomarkers in clear cell renal cell carcinoma based on bioinformatics analysis Basavaraj Vastrad1, Chanabasayya Vastrad*2 , Iranna Kotturshetti 1. Department of Biochemistry, Basaveshwar College of Pharmacy, Gadag, Karnataka 582103, India. 2. Biostatistics and Bioinformatics, Chanabasava Nilaya, Bharthinagar, Dharwad 580001, Karanataka, India. 3. Department of Ayurveda, Rajiv Gandhi Education Society`s Ayurvedic Medical College, Ron, Karnataka 562209, India. * Chanabasayya Vastrad [email protected] Ph: +919480073398 Chanabasava Nilaya, Bharthinagar, Dharwad 580001 , Karanataka, India bioRxiv preprint doi: https://doi.org/10.1101/2020.12.21.423889; this version posted December 23, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract Clear cell renal cell carcinoma (ccRCC) is one of the most common types of malignancy of the urinary system. The pathogenesis and effective diagnosis of ccRCC have become popular topics for research in the previous decade. In the current study, an integrated bioinformatics analysis was performed to identify core genes associated in ccRCC. An expression dataset (GSE105261) was downloaded from the Gene Expression Omnibus database, and included 26 ccRCC and 9 normal kideny samples. Assessment of the microarray dataset led to the recognition of differentially expressed genes (DEGs), which was subsequently used for pathway and gene ontology (GO) enrichment analysis. -

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Anti-Human CD31 (EPR3094)-151Eu
PRD025-3151025D PRODUCT INFORMATION SHEET Anti-Human CD31/PECAM-1-151Eu Pathologist-Verified Clone for Imaging Mass Cytometry™ Catalog: 3151025D Clone: EPR3094 Package size and concentration: 25 µg, 0.5 mg/mL Isotype: Rabbit IgG Storage: Store at 4 °C. Do not freeze. Formulation: Antibody stabilizer with 0.05% sodium azide Reactivity: Human Application: IMC-Paraffin Technical Information Application: The metal-tagged antibody is designed and formulated for the application of Imaging Mass Cytometry (IMC™) using the Fluidigm Hyperion™ Imaging System on formalin-fixed, paraffin-embedded (FFPE) tissue sections. Quality control: Each lot of conjugated antibody is quality control- tested by Imaging Mass Cytometry on tissue sections. Recommended concentration: For optimal performance it is recommended that the antibody be titrated for the desired application. Suggested initial dilution range: IMC-Paraffin: 1:50 to 1:200 Description CD31, also known as platelet endothelial cell adhesion molecule-1 (PECAM-1) or endoCAM, is a type I transmembrane glycoprotein. It is expressed by endothelial cells on blood vessels, as well as by monocytes, granulocytes, platelets and a small subset of T cells. It plays a role in wound healing, angiogenesis and removal of aged neutrophils and in cellular migration in an inflammatory situation. Human spleen (FFPE) stained with 151Eu-anti-CD31 (EPR3094) at a dilution of 1:100 (green pseudocolor), 141Pr-anti-αSMA (1A4) (red pseudocolor), and iridium DNA intercalator (blue pseudocolor). Heat-mediated antigen retrieval was performed using Tris/EDTA buffer pH 9. Scale bar size = 100 µm. References Chang, Q. et al. "Staining of frozen and formalin-fixed, paraffin-embedded tissues with metal-labeled antibodies for imaging mass cytometry analysis." Current Protocols in Cytometry 82 (2017): 12.47.1–12.47.8. -

Clinical and Biological Characteristics of Medullary and Extramedullary Plasma Cell Dyscrasias
biology Article Clinical and Biological Characteristics of Medullary and Extramedullary Plasma Cell Dyscrasias Snjezana Janjetovic 1,2, Philipp Lohneis 3,4, Axel Nogai 5, Derya Balci 5,6, Leo Rasche 7, Doris Jähne 8, Carsten Bokemeyer 1, Georgia Schilling 1,9, Igor Wolfgang Blau 5,10 and Martin Schmidt-Hieber 2,5,11,* 1 Department of Oncology, Hematology and Bone Marrow Transplantation with Section Pneumology, University Clinic Hamburg-Eppendorf, 20251 Hamburg, Germany; [email protected] (S.J.); [email protected] (C.B.); [email protected] (G.S.) 2 Clinic of Hematology and Stem Cell Transplantation, HELIOS Clinic Berlin-Buch, 13125 Berlin, Germany 3 Institute of Pathology, Charité University Medicine Berlin, 10117 Berlin, Germany; [email protected] 4 Institute of Pathology, University of Cologne, 50923 Cologne, Germany 5 Clinic of Hematology, Oncology and Tumor Immunology, Campus Benjamin Franklin, Charité University Medicine Berlin, 12203 Berlin, Germany; [email protected] (A.N.); [email protected] (D.B.); [email protected] (I.W.B.) 6 St. Joseph Hospital Berlin-Tempelhof, 12101 Berlin, Germany 7 Department of Internal Medicine II, University Hospital Würzburg, 97080 Würzburg, Germany; [email protected] 8 Institute of Pathology, HELIOS Clinic Berlin-Zehlendorf, 14165 Berlin, Germany; [email protected] 9 Citation: Janjetovic, S.; Lohneis, P.; Department of Hematology, Oncology, Palliative Care and Rheumatology, Asklepios Hospital Altona, Asklepios Tumorzentrum, 22763 Hamburg, Germany Nogai, A.; Balci, D.; Rasche, L.; 10 Clinic of Hematology, Oncology and Tumor Immunology, Campus Virchow Klinikum, Charité University Jähne, D.; Bokemeyer, C.; Medicine Berlin, 10117 Berlin, Germany Schilling, G.; Blau, I.W.; 11 Clinic of Hematology and Oncology, Carl-Thiem-Klinikum, 03048 Cottbus, Germany Schmidt-Hieber, M. -

Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model
Downloaded from http://www.jimmunol.org/ by guest on September 25, 2021 T + is online at: average * The Journal of Immunology , 34 of which you can access for free at: 2016; 197:1477-1488; Prepublished online 1 July from submission to initial decision 4 weeks from acceptance to publication 2016; doi: 10.4049/jimmunol.1600589 http://www.jimmunol.org/content/197/4/1477 Molecular Profile of Tumor-Specific CD8 Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. Waugh, Sonia M. Leach, Brandon L. Moore, Tullia C. Bruno, Jonathan D. Buhrman and Jill E. Slansky J Immunol cites 95 articles Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2016/07/01/jimmunol.160058 9.DCSupplemental This article http://www.jimmunol.org/content/197/4/1477.full#ref-list-1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material References Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2016 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 25, 2021. The Journal of Immunology Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. -

Clinical Significance of Soluble CD31 in Patients with Systemic
Clinical Significance of Soluble CD31 in Patients with Systemic Sclerosis (SSc): Association with Limited Cutaneous SSc SHINICHI SATO, KAZUHIRO KOMURA, MINORU HASEGAWA, MANABU FUJIMOTO, and KAZUHIKO TAKEHARA ABSTRACT. Objective. To determine serum levels of soluble CD31 (sCD31) and its clinical associations in patients with systemic sclerosis (SSc). Methods. Serum sCD31 levels from 70 patients with SSc were examined by ELISA. For a longitu- dinal study, 64 sera from 17 SSc patients were analyzed (followup: 0.4–3.9 yrs). Results. Serum sCD31 levels were elevated in patients with SSc (n = 70) compared with healthy controls (n = 20) and patients with systemic lupus erythematosus (n = 15). Serum sCD31 levels were higher in patients with limited cutaneous SSc (lSSc; n = 37) than those with diffuse cutaneous SSc (n = 33). Patients with elevated sCD31 levels had pulmonary fibrosis and decreased percentage vital capacity (%VC) less frequently than those with normal sCD31 levels. sCD31 levels correlated posi- tively with %VC in patients with SSc. This association of elevated sCD31 levels with the lower frequency of pulmonary involvement and better %VC was still observed when analyzed among lSSc patients alone. The elevation of sCD31 was associated with shorter disease duration in patients with lSSc. In a longitudinal study, 75% of patients with SSc showed increased sCD31 levels only tran- siently in the early phase of the disease. Serum sCD31 levels remained normal during followup in all patients with normal sCD31 levels at the first visit. Conclusion. Elevated sCD31 levels were associated with lSSc with relatively early onset and lower frequency and severity of pulmonary fibrosis. -

New Advances in Leukaemia Immunotherapy by the Use of Chimeric Artificial Antigen Receptors
Biagi et al. Italian Journal of Pediatrics 2011, 37:46 http://www.ijponline.net/content/37/1/46 ITALIAN JOURNAL OF PEDIATRICS REVIEW Open Access New advances in leukaemia immunotherapy by the use of Chimeric Artificial Antigen Receptors (CARs): state of the art and perspectives for the near future Ettore Biagi*, Virna Marin, Greta Maria Paola Giordano Attianese, Irene Pizzitola, Sarah Tettamanti, Elisabetta Cribioli and Andrea Biondi Abstract Leukaemia immunotherapy represents a fascinating and promising field of translational research, particularly as an integrative approach of bone marrow transplantation. Adoptive immunotherapy by the use of donor-derived expanded leukaemia-specific T cells has showed some kind of clinical response, but the major advance is nowadays represented by gene manipulation of donor immune cells, so that they acquire strict specificity towards the tumour target and potent lytic activity, followed by significant proliferation, increased survival and possibly anti- tumour memory state. This is achieved by gene insertion of Chimeric T-cell Antigen Receptors (CARs), which are artificial molecules containing antibody-derived fragments (to bind the specific target), joined with potent signalling T-Cell Receptor (TCR)-derived domains that activate the manipulated cells. This review will discuss the main application of this approach particularly focusing on the paediatric setting, raising advantages and disadvantages and discussing relevant perspectives of use in the nearest future. Keywords: Leukaemia immunotherapy, -

ROR1/CD19 Receptor Complex Promotes Growth of Mantle Cell Lymphoma Cells Independently of the B Cell Receptor–BTK Signaling Pathway † Qian Zhang,* Hong Y
Published September 18, 2019, doi:10.4049/jimmunol.1801327 Cutting Edge: ROR1/CD19 Receptor Complex Promotes Growth of Mantle Cell Lymphoma Cells Independently of the B Cell Receptor–BTK Signaling Pathway † Qian Zhang,* Hong Y. Wang,* Xiaobin Liu,* Selene Nunez-Cruz,* Mowafaqx Jillab, Olga Melnikov,† Kavindra Nath,‡ Jerry Glickson,‡ and Mariusz A. Wasik*,†, Inhibitors of Bruton tyrosine kinase (BTK), a kinase these mechanisms is of uttermost importance in design- downstream of BCR, display remarkable activity in a ing an appropriate therapeutic strategy to counteract the subset of mantle cell lymphoma (MCL) patients, but reprogramming. the drug resistance remains a considerable challenge. In ROR1 belongs to the receptor tyrosine kinase-like orphan this study, we demonstrate that aberrant expression of receptor (ROR) family and displays very restricted expression ROR1 (receptor tyrosine kinase-like orphan receptor 1), in normal tissues (11, 12). ROR1 is aberrantly expressed in seen in a large subset of MCL, results in BCR/BTK– various malignancies, including small lymphocytic lymphoma/ independent signaling and growth of MCL cells. ROR1 chronic lymphocytic leukemia (SLL/CLL) and MCL. ROR1 forms a functional complex with CD19 to persistently activates signaling molecules, such as RAC-1 and contractin activate the key cell signaling pathways PI3K–AKT and (13, 14), to promote cell proliferation, survival, and migration MEK–ERK in the BCR/BTK–independent manner. (13–15). CD19 is a B cell–specific receptor capable of stimu- lating the growth of malignant B cells (16). In normal This study demonstrates that ROR1/CD19 complex B lymphocytes, it is activated by SRC family kinases and effectively substitutes for BCR–BTK signaling to SYK, both downstream of BCR (17). -

Supplementary Table 1: Adhesion Genes Data Set
Supplementary Table 1: Adhesion genes data set PROBE Entrez Gene ID Celera Gene ID Gene_Symbol Gene_Name 160832 1 hCG201364.3 A1BG alpha-1-B glycoprotein 223658 1 hCG201364.3 A1BG alpha-1-B glycoprotein 212988 102 hCG40040.3 ADAM10 ADAM metallopeptidase domain 10 133411 4185 hCG28232.2 ADAM11 ADAM metallopeptidase domain 11 110695 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 195222 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 165344 8751 hCG20021.3 ADAM15 ADAM metallopeptidase domain 15 (metargidin) 189065 6868 null ADAM17 ADAM metallopeptidase domain 17 (tumor necrosis factor, alpha, converting enzyme) 108119 8728 hCG15398.4 ADAM19 ADAM metallopeptidase domain 19 (meltrin beta) 117763 8748 hCG20675.3 ADAM20 ADAM metallopeptidase domain 20 126448 8747 hCG1785634.2 ADAM21 ADAM metallopeptidase domain 21 208981 8747 hCG1785634.2|hCG2042897 ADAM21 ADAM metallopeptidase domain 21 180903 53616 hCG17212.4 ADAM22 ADAM metallopeptidase domain 22 177272 8745 hCG1811623.1 ADAM23 ADAM metallopeptidase domain 23 102384 10863 hCG1818505.1 ADAM28 ADAM metallopeptidase domain 28 119968 11086 hCG1786734.2 ADAM29 ADAM metallopeptidase domain 29 205542 11085 hCG1997196.1 ADAM30 ADAM metallopeptidase domain 30 148417 80332 hCG39255.4 ADAM33 ADAM metallopeptidase domain 33 140492 8756 hCG1789002.2 ADAM7 ADAM metallopeptidase domain 7 122603 101 hCG1816947.1 ADAM8 ADAM metallopeptidase domain 8 183965 8754 hCG1996391 ADAM9 ADAM metallopeptidase domain 9 (meltrin gamma) 129974 27299 hCG15447.3 ADAMDEC1 ADAM-like, -

B Cell Checkpoints in Autoimmune Rheumatic Diseases
REVIEWS B cell checkpoints in autoimmune rheumatic diseases Samuel J. S. Rubin1,2,3, Michelle S. Bloom1,2,3 and William H. Robinson1,2,3* Abstract | B cells have important functions in the pathogenesis of autoimmune diseases, including autoimmune rheumatic diseases. In addition to producing autoantibodies, B cells contribute to autoimmunity by serving as professional antigen- presenting cells (APCs), producing cytokines, and through additional mechanisms. B cell activation and effector functions are regulated by immune checkpoints, including both activating and inhibitory checkpoint receptors that contribute to the regulation of B cell tolerance, activation, antigen presentation, T cell help, class switching, antibody production and cytokine production. The various activating checkpoint receptors include B cell activating receptors that engage with cognate receptors on T cells or other cells, as well as Toll-like receptors that can provide dual stimulation to B cells via co- engagement with the B cell receptor. Furthermore, various inhibitory checkpoint receptors, including B cell inhibitory receptors, have important functions in regulating B cell development, activation and effector functions. Therapeutically targeting B cell checkpoints represents a promising strategy for the treatment of a variety of autoimmune rheumatic diseases. Antibody- dependent B cells are multifunctional lymphocytes that contribute that serve as precursors to and thereby give rise to acti- cell- mediated cytotoxicity to the pathogenesis of autoimmune diseases -
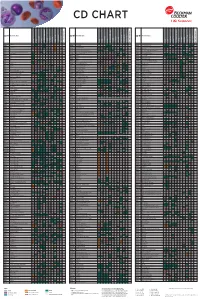
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Clinical Significance of Soluble CD31 in Patients with Systemic Sclerosis
Clinical Significance of Soluble CD31 in Patients with Systemic Sclerosis (SSc): Association with Limited Cutaneous SSc SHINICHI SATO, KAZUHIRO KOMURA, MINORU HASEGAWA, MANABU FUJIMOTO, and KAZUHIKO TAKEHARA ABSTRACT. Objective. To determine serum levels of soluble CD31 (sCD31) and its clinical associations in patients with systemic sclerosis (SSc). Methods. Serum sCD31 levels from 70 patients with SSc were examined by ELISA. For a longitu- dinal study, 64 sera from 17 SSc patients were analyzed (followup: 0.4–3.9 yrs). Results. Serum sCD31 levels were elevated in patients with SSc (n = 70) compared with healthy controls (n = 20) and patients with systemic lupus erythematosus (n = 15). Serum sCD31 levels were higher in patients with limited cutaneous SSc (lSSc; n = 37) than those with diffuse cutaneous SSc (n = 33). Patients with elevated sCD31 levels had pulmonary fibrosis and decreased percentage vital capacity (%VC) less frequently than those with normal sCD31 levels. sCD31 levels correlated posi- tively with %VC in patients with SSc. This association of elevated sCD31 levels with the lower frequency of pulmonary involvement and better %VC was still observed when analyzed among lSSc patients alone. The elevation of sCD31 was associated with shorter disease duration in patients with lSSc. In a longitudinal study, 75% of patients with SSc showed increased sCD31 levels only tran- siently in the early phase of the disease. Serum sCD31 levels remained normal during followup in all patients with normal sCD31 levels at the first visit. Conclusion. Elevated sCD31 levels were associated with lSSc with relatively early onset and lower frequency and severity of pulmonary fibrosis.