Trigeminal Nerve
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Perioral Gustatory Sweating: Case Report
The Journal of Laryngology & Otology (2012), 126, 532–534. CLINICAL RECORD © JLO (1984) Limited, 2012 doi:10.1017/S0022215112000229 Perioral gustatory sweating: case report S C KÄYSER1, K J A O INGELS2, F J A VAN DEN HOOGEN2 1Department of Primary and Community Care, Radboud University Nijmegen Medical Centre, and 2Department of Otorhinolaryngology/Head and Neck Surgery, Radboud University Nijmegen Medical Centre, The Netherlands Abstract Objective: Presentation of a case of perioral Frey syndrome. Design: Case report. Subject: A 72-year-old woman with hyperhidrosis around the mouth and chin. Results: This patient suffered from bilateral perioral gustatory sweating following a mandibular osteotomy; such a case has not previously been described. Possible pathophysiological hypotheses are discussed in relation to the anatomy and innervation of the salivary glands. Conclusion: Perioral gustatory sweating is a rare complication of osteotomy. Key words: Gustatory sweating; Frey Syndrome; Perioral; Hyperhidrosis Introduction perioral excessive sweating and flushing which only Frey syndrome, also known as auriculotemporal syndrome, is a occurred during (and not preceding) eating. Her complaints well-known complication of parotid surgery. Approximately had begun following bilateral osteotomy of the mandible in 24 per cent of patients undergoing parotidectomy experience 1960, at the age of 25 years. The indication for this procedure gustatory sweating, although the reported incidence varies had been prognathism. Her recovery had been complicated greatly.1 Frey syndrome appears following a latency period by inadequate bone healing and loss of the right and left of one to 36 months (or longer) after surgery.2,3 inferior alveolar nerves (Figure 1). The aetiology of Frey syndrome is explained by ‘aberrant The diagnosis of hyperhidrosis was made using the nervous regeneration’. -

Numb Tongue, Numb Lip, Numb Chin: What to Do When?
NUMB TONGUE, NUMB LIP, NUMB CHIN: WHAT TO DO WHEN? Ramzey Tursun, DDS, FACS Marshall Green, DDS Andre Ledoux, DMD Arshad Kaleem, DMD, MD Assistant Professor, Associate Fellowship Director of Oral, Head & Neck Oncologic and Microvascular Reconstructive Surgery, DeWitt Daughtry Family Department of Surgery, Division of Oral Maxillofacial Surgery, Leonard M. Miller School of Medicine, University of Miami INTRODUCTION MECHANISM OF NERVE Microneurosurgery of the trigeminal nerve INJURIES has been in the spotlight over the last few years. The introduction of cone-beam When attempting to classify the various scanning, three-dimensional imaging, mechanisms of nerve injury in the magnetic resonance neurography, maxillofacial region, it becomes clear that endoscopic-assisted surgery, and use of the overwhelming majority are iatrogenic allogenic nerve grafts have improved the in nature. The nerves that are most often techniques that can be used for affected in dento-alveolar procedures are assessment and treatment of patients with the branches of the mandibular division of nerve injuries. Injury to the terminal cranial nerve V, i.e., the trigeminal nerve. branches of the trigeminal nerve is a well- The lingual nerve and inferior alveolar known risk associated with a wide range of nerve are most often affected, and third dental and surgical procedures. These molar surgery is the most common cause 1 injuries often heal spontaneously without of injury. medical or surgical intervention. However, they sometimes can cause a variety of None of these nerves provide motor symptoms, including lost or altered innervation. However, damage to these sensation, pain, or a combination of these, nerves can cause a significant loss of and may have an impact on speech, sensation and/or taste in affected patients. -

Palatal Injection Does Not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth
Open Access Review Article DOI: 10.7759/cureus.2120 Palatal Injection does not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth Joe Iwanaga 1 , R. Shane Tubbs 2 1. Seattle Science Foundation 2. Neurosurgery, Seattle Science Foundation Corresponding author: Joe Iwanaga, [email protected] Abstract The superior alveolar nerves course lateral to the maxillary sinus and the greater palatine nerve travels through the hard palate. This difficult three-dimensional anatomy has led some dentists and oral surgeons to a critical misunderstanding in developing the anterior and middle superior alveolar (AMSA) nerve block and the palatal approach anterior superior alveolar (P-ASA) nerve block. In this review, the anatomy of the posterior, middle and anterior superior alveolar nerves, greater palatine nerve, and nasopalatine nerve are revisited in order to clarify the anatomy of these blocks so that the perpetuated anatomical misunderstanding is rectified. We conclude that the AMSA and P-ASA nerve blockades, as currently described, are not based on accurate anatomy. Categories: Anesthesiology, Medical Education, Other Keywords: anatomy, innervation, local anesthesia, maxillary nerve, nerve block, tooth Introduction And Background Anesthetic blockade of the posterior superior alveolar (PSA) branch of the maxillary nerve has played an important role in the endodontic treatment of irreversible acute pulpitis of the upper molar teeth except for the mesiobuccal root of the first molar tooth [1, 2]. This procedure requires precise anatomical knowledge of the pterygopalatine fossa and related structures in order to avoid unnecessary complications and to make the blockade most effective. The infraorbital nerve gives rise to middle superior alveolar (MSA) and anterior superior alveolar (ASA) branches. -

The Influence of Mandibular Skeletal Characteristics on Inferior Alveolar Nerve Block Anesthesia
pISSN 2383-9309❚eISSN 2383-9317 Original Article J Dent Anesth Pain Med 2015;15(3):113-119❚http://dx.doi.org/10.17245/jdapm.2015.15.3.113 The influence of mandibular skeletal characteristics on inferior alveolar nerve block anesthesia Tae Min You1, Kee-Deog Kim2, Jisun Huh2, Eun-Jung Woo2, Wonse Park2 1Department of Advanced General Dentistry, College of Dentistry, Dankook University, Cheonan, Korea 2Department of Advanced General Dentistry, College of Dentistry, Yonsei University, Seoul, Korea Background: The inferior alveolar nerve block (IANB) is the most common anesthetic techniques in dentistry; however, its success rate is low. The purpose of this study was to determine the correlation between IANB failure and mandibular skeletal characteristics Methods: In total, 693 cases of lower third molar extraction (n = 575 patients) were examined in this study. The ratio of the condylar and coronoid distances from the mandibular foramen (condyle-coronoid ratio [CC ratio]) was calculated, and the mandibular skeleton was then classified as normal, retrognathic, or prognathic. The correlation between IANB failure and sex, treatment side, and the CC ratio was assessed. Results: The IANB failure rates for normal, retrognathic, and prognathic mandibles were 7.3%, 14.5%, and 9.5%, respectively, and the failure rate was highest among those with a CC ratio < 0.8 (severe retrognathic mandible). The failure rate was significantly higher in the retrognathic group than in normal group (P = 0.019), and there was no statistically significant difference between the other two groups. Conclusions: IANB failure could be attributable, in part, to the skeletal characteristics of the mandible. -

Nerves of the Orbit Optic Nerve the Optic Nerve Enters the Orbit from the Middle Cranial Fossa by Passing Through the Optic Canal
human anatomy 2016 lecture fourteen Dr meethak ali ahmed neurosurgeon Nerves of the Orbit Optic Nerve The optic nerve enters the orbit from the middle cranial fossa by passing through the optic canal . It is accompanied by the ophthalmic artery, which lies on its lower lateral side. The nerve is surrounded by sheath of pia mater, arachnoid mater, and dura mater. It runs forward and laterally within the cone of the recti muscles and pierces the sclera at a point medial to the posterior pole of the eyeball. Here, the meninges fuse with the sclera so that the subarachnoid space with its contained cerebrospinal fluid extends forward from the middle cranial fossa, around the optic nerve, and through the optic canal, as far as the eyeball. A rise in pressure of the cerebrospinal fluid within the cranial cavity therefore is transmitted to theback of the eyeball. Lacrimal Nerve The lacrimal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward along the upper border of the lateral rectus muscle . It is joined by a branch of the zygomaticotemporal nerve, whi(parasympathetic secretomotor fibers). The lacrimal nerve ends by supplying the skin of the lateral part of the upper lid. Frontal Nerve The frontal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward on the upper surface of the levator palpebrae superioris beneath the roof of the orbit . -

Regional Anesthesia in Head and Neck Surgery
TITLE: Regional Anesthesia in Head and Neck Surger SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 24, 2006 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY PHYSICIAN: Francis B. Quinn, MD SERIES EDITORS: Francis B. Quinn, Jr., MD and Matthew W. Ryan, MD "This material was prepared by resident physicians in partial fulfillment of educational requirements established for the Postgraduate Training Program of the UTMB Department of Otolaryngology/Head and Neck Surgery and was not intended for clinical use in its present form. It was prepared for the purpose of stimulating group discussion in a conference setting. No warranties, either express or implied, are made with respect to its accuracy, completeness, or timeliness. The material does not necessarily reflect the current or past opinions of members of the UTMB faculty and should not be used for purposes of diagnosis or treatment without consulting appropriate literature sources and informed professional opinion." Introduction Local anesthetic techniques were popularized early in the history of surgery with the advent of injectable nerve blocking agents. Until their discovery, patients were either held down or knocked unconscious to perform procedures. In the early days of general anesthesia, local anesthesia was preferred in all cases that it was applicable due to the significant risks associated with general anesthesia. Many procedures performed today under general anesthesia, such as tonsillectomy, rhinoplasty, and even bronchoscopy, were performed under local anesthesia to avoid the perils of general anesthetics. With the introduction of pulse oximetry, safer inhaled anesthetics, and combined intravenous and inhaled general anesthesia techniques, general anesthesia has become much safer, resulting in many surgeons being unfamiliar with regional nerve blocks to perform surgery. -

Cranial Nerve Palsy
Cranial Nerve Palsy What is a cranial nerve? Cranial nerves are nerves that lead directly from the brain to parts of our head, face, and trunk. There are 12 pairs of cranial nerves and some are involved in special senses (sight, smell, hearing, taste, feeling) while others control muscles and glands. Which cranial nerves pertain to the eyes? The second cranial nerve is called the optic nerve. It sends visual information from the eye to the brain. The third cranial nerve is called the oculomotor nerve. It is involved with eye movement, eyelid movement, and the function of the pupil and lens inside the eye. The fourth cranial nerve is called the trochlear nerve and the sixth cranial nerve is called the abducens nerve. They each innervate an eye muscle involved in eye movement. The fifth cranial nerve is called the trigeminal nerve. It provides facial touch sensation (including sensation on the eye). What is a cranial nerve palsy? A palsy is a lack of function of a nerve. A cranial nerve palsy may cause a complete or partial weakness or paralysis of the areas served by the affected nerve. In the case of a cranial nerve that has multiple functions (such as the oculomotor nerve), it is possible for a palsy to affect all of the various functions or only some of the functions of that nerve. What are some causes of a cranial nerve palsy? A cranial nerve palsy can occur due to a variety of causes. It can be congenital (present at birth), traumatic, or due to blood vessel disease (hypertension, diabetes, strokes, aneurysms, etc). -

Maxillary Nerve-Mediated Postseptoplasty Nasal Allodynia: a Case Report
E CASE REPORT Maxillary Nerve-Mediated Postseptoplasty Nasal Allodynia: A Case Report Shikha Sharma, MD, PhD,* Wilson Ly, MD, PharmD,* and Xiaobing Yu, MD*† Endoscopic nasal septoplasty is a commonly performed otolaryngology procedure, not known to cause persistent postsurgical pain or hypersensitivity. Here, we discuss a unique case of persis- tent nasal pain that developed after a primary endoscopic septoplasty, which then progressed to marked mechanical and thermal allodynia following a revision septoplasty. Pain symptoms were found to be mediated by the maxillary division of the trigeminal nerve and resolved after percuta- neous radiofrequency ablation (RFA) of bilateral maxillary nerves. To the best of our knowledge, this is the first report of maxillary nerve–mediated nasal allodynia after septoplasty. (A&A Practice. 2020;14:e01356.) GLOSSARY CT = computed tomography; FR = foramen rotundum; HIPAA = Health Insurance Portability and Accountability Act; ION = infraorbital nerve; LPP = lateral pterygoid plate; MRI = magnetic reso- nance imaging; RFA = radiofrequency ablation; SPG = sphenopalatine ganglion; US = ultrasound ndoscopic nasal septoplasty is a common otolaryn- septoplasty for chronic nasal obstruction with resection of gology procedure with rare incidence of postsurgical the cartilage inferiorly and posteriorly in 2010. Before this Ecomplications. Minor complications include epistaxis, surgery, the patient only occasionally experienced mild septal hematoma, septal perforation, cerebrospinal fluid leak, headaches. However, his postoperative course was compli- and persistent obstruction.1 Numbness or hypoesthesia of the cated by significant pain requiring high-dose opioids. After anterior palate, secondary to injury to the nasopalatine nerve, discharge, patient continued to have persistent deep, “ach- has been reported, but is usually rare and temporary, resolv- ing” nasal pain which radiated toward bilateral forehead ing over weeks to months.2 Acute postoperative pain is also and incisors. -

Anatomy of Maxillary and Mandibular Local Anesthesia
Anatomy of Mandibular and Maxillary Local Anesthesia Patricia L. Blanton, Ph.D., D.D.S. Professor Emeritus, Department of Anatomy, Baylor College of Dentistry – TAMUS and Private Practice in Periodontics Dallas, Texas Anatomy of Mandibular and Maxillary Local Anesthesia I. Introduction A. The anatomical basis of local anesthesia 1. Infiltration anesthesia 2. Block or trunk anesthesia II. Review of the Trigeminal Nerve (Cranial n. V) – the major sensory nerve of the head A. Ophthalmic Division 1. Course a. Superior orbital fissure – root of orbit – supraorbital foramen 2. Branches – sensory B. Maxillary Division 1. Course a. Foramen rotundum – pterygopalatine fossa – inferior orbital fissure – floor of orbit – infraorbital 2. Branches - sensory a. Zygomatic nerve b. Pterygopalatine nerves [nasal (nasopalatine), orbital, palatal (greater and lesser palatine), pharyngeal] c. Posterior superior alveolar nerves d. Infraorbital nerve (middle superior alveolar nerve, anterior superior nerve) C. Mandibular Division 1. Course a. Foramen ovale – infratemporal fossa – mandibular foramen, Canal -> mental foramen 2. Branches a. Sensory (1) Long buccal nerve (2) Lingual nerve (3) Inferior alveolar nerve -> mental nerve (4) Auriculotemporal nerve b. Motor (1) Pterygoid nerves (2) Temporal nerves (3) Masseteric nerves (4) Nerve to tensor tympani (5) Nerve to tensor veli palatine (6) Nerve to mylohyoid (7) Nerve to anterior belly of digastric c. Both motor and sensory (1) Mylohyoid nerve III. Usual Routes of innervation A. Maxilla 1. Teeth a. Molars – Posterior superior alveolar nerve b. Premolars – Middle superior alveolar nerve c. Incisors and cuspids – Anterior superior alveolar nerve 2. Gingiva a. Facial/buccal – Superior alveolar nerves b. Palatal – Anterior – Nasopalatine nerve; Posterior – Greater palatine nerves B. -

Simple Ways to Dissect Ciliary Ganglion for Orbital Anatomical Education
OkajimasDetection Folia Anat. of ciliary Jpn., ganglion94(3): 119–124, for orbit November, anatomy 2017119 Simple ways to dissect ciliary ganglion for orbital anatomical education By Ming ZHOU, Ryoji SUZUKI, Hideo AKASHI, Akimitsu ISHIZAWA, Yoshinori KANATSU, Kodai FUNAKOSHI, Hiroshi ABE Department of Anatomy, Akita University Graduate School of Medicine, Akita, 010-8543 Japan –Received for Publication, September 21, 2017– Key Words: ciliary ganglion, orbit, human anatomy, anatomical education Summary: In the case of anatomical dissection as part of medical education, it is difficult for medical students to find the ciliary ganglion (CG) since it is small and located deeply in the orbit between the optic nerve and the lateral rectus muscle and embedded in the orbital fat. Here, we would like to introduce simple ways to find the CG by 1): tracing the sensory and parasympathetic roots to find the CG from the superior direction above the orbit, 2): transecting and retracting the lateral rectus muscle to visualize the CG from the lateral direction of the orbit, and 3): taking out whole orbital structures first and dissecting to observe the CG. The advantages and disadvantages of these methods are discussed from the standpoint of decreased laboratory time and students as beginners at orbital anatomy. Introduction dissection course for the first time and with limited time. In addition, there are few clear pictures in anatomical The ciliary ganglion (CG) is one of the four para- textbooks showing the morphology of the CG. There are sympathetic ganglia in the head and neck region located some scientific articles concerning how to visualize the behind the eyeball between the optic nerve and the lateral CG, but they are mostly based on the clinical approaches rectus muscle in the apex of the orbit (Siessere et al., rather than based on the anatomical procedure for medical 2008). -

Orbital Malignant Peripheral Nerve Sheath Tumours
Br J Ophthalmol: first published as 10.1136/bjo.73.9.731 on 1 September 1989. Downloaded from British Journal of Ophthalmology, 1989, 73, 731-738 Orbital malignant peripheral nerve sheath tumours CHRISTOPHER J LYONS,' ALAN A McNAB,l ALEC GARNER,2 AND JOHN E WRIGHT' From the I Orbital clinic, Moorfields Eye Hospital, City Road, London EC] V 2PD, and the 2Department of Pathology, Institute ofOphthalmology, London EC] V 9A T SUMMARY We describe three patients with malignant peripheral nerve tumours in the orbit and review the existing literature on these rare lesions. Malignant peripheral nerve sheath tumours are Sensation was diminished over the distribution of the unusual in any part of the body and very rare in the second division of the right trigeminal nerve. The left orbit, where only 13 cases have previously been globe was normal. Plain anteroposterior skull x-rays described. These tumours can spread rapidly along showed a normal appearance, but undertilted the involved nerve to the middle cranial fossa. They occipitomental tomographic views revealed enlarge- are radioresistant, and total surgical excision offers ment of the right infraorbital canal (Fig. 1). copyright. the only hope of cure. Our experience with three An inferior orbital margin incision revealed patients may help clinicians to recognise these lesions tumour protruding from the infraorbital foramen and and excise them at an early stage. extending beneath the soft tissues of the cheek. The tumour had a firm consistency and a pale grey cut Case reports surface. The orbital periosteum on the floor of the orbit was elevated and a mass over 18 mm in diameter PATIENT 1 was found within an expanded infraorbital canal Four years prior to presentation a man which extended posteriorly into the superior orbital 55-year-old http://bjo.bmj.com/ noted a small lump at the medial end of his right fissure. -
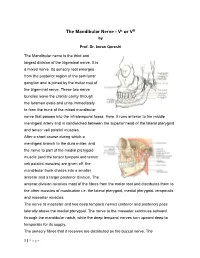
The Mandibular Nerve - Vc Or VIII by Prof
The Mandibular Nerve - Vc or VIII by Prof. Dr. Imran Qureshi The Mandibular nerve is the third and largest division of the trigeminal nerve. It is a mixed nerve. Its sensory root emerges from the posterior region of the semilunar ganglion and is joined by the motor root of the trigeminal nerve. These two nerve bundles leave the cranial cavity through the foramen ovale and unite immediately to form the trunk of the mixed mandibular nerve that passes into the infratemporal fossa. Here, it runs anterior to the middle meningeal artery and is sandwiched between the superior head of the lateral pterygoid and tensor veli palatini muscles. After a short course during which a meningeal branch to the dura mater, and the nerve to part of the medial pterygoid muscle (and the tensor tympani and tensor veli palatini muscles) are given off, the mandibular trunk divides into a smaller anterior and a larger posterior division. The anterior division receives most of the fibres from the motor root and distributes them to the other muscles of mastication i.e. the lateral pterygoid, medial pterygoid, temporalis and masseter muscles. The nerve to masseter and two deep temporal nerves (anterior and posterior) pass laterally above the medial pterygoid. The nerve to the masseter continues outward through the mandibular notch, while the deep temporal nerves turn upward deep to temporalis for its supply. The sensory fibres that it receives are distributed as the buccal nerve. The 1 | P a g e buccal nerve passes between the medial and lateral pterygoids and passes downward and forward to emerge from under cover of the masseter with the buccal artery.