MRADL: Mobility Related Activity of Daily Living
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hospice Care Network Hospice Care Network Northwell Health at Home Northwell Health Post-Acute Services 1 “None of Us, Including Me, Ever Do Great Things
Hospice Care Network Hospice Care Network 2019 Annual Report MANAGEMENT TEAM ADMINISTRATIVE LEADERSHIP MEDICAL LEADERSHIP Executive Director – Maureen Hinkelman, RN, MA Medical Director – Lori Ann Attivissimo, MD, FACP, FAAHPM, HMDC Associate Executive Director of Clinical Operations – Orael Keenan, RN, MSN Hospice Physician – Edward Halbridge, MD ABOUT US Medical Director – Lori Ann Attivissimo, MD, FACP, FAAHPM, HMDC Hospice Physician – Joi Marszalek, DO Our Mission Assistant Vice President of Counseling & Pediatric Services – Mary Gravina, LCSW Hospice Physician – Eirene Milano, MD Our mission is to enable people to live in peace and with dignity in a caring environment during the final stages of life by Assistant Vice President of Hospice Operations – Marie Zanotelli Hospice Physician – Sonia Tercero Moreno, MD offering care and comfort both to them and to those with whom they share their lives. Assistant Vice President of Inpatient Hospice Services – Darrin London, ANP Hospice Physician - Dimitris Platis, MD Hospice Physician - Tarek Zetoune, MD We develop and provide individualized programs of care and supportive services during dying, death and bereavement that enhance quality of life by addressing physical, emotional, spiritual and social needs. Nurse Practitioner – Carmen Bassaragh, ANP-C PATIENT CARE AND BUSINESS LEADERSHIP Nurse Practitioner – Lori Finkel, ANP-BC, CHPN Director of Admissions – Linda Rossi, RN, CHPN Background Nurse Practitioner – Tara Lauria, ANP-C Director of Financial and Operations Management - Letizia Cinelli Hospice Care Network is a not for profit healthcare organization serving patients and families in Nassau, Suffolk and Queens Nurse Practitioner – Darrin London, ANP counties. Hospice Care Network has been helping patients since 1988 and is a proud member of Northwell Health. -

A Study of the Use of Clinician I Personnel to Perform Intravenous Therapy
Old Dominion University ODU Digital Commons OTS Master's Level Projects & Papers STEM Education & Professional Studies 1996 A Study of the Use of Clinician I Personnel to Perform Intravenous Therapy Laura L. Walker Old Dominion University Follow this and additional works at: https://digitalcommons.odu.edu/ots_masters_projects Part of the Education Commons Recommended Citation Walker, Laura L., "A Study of the Use of Clinician I Personnel to Perform Intravenous Therapy" (1996). OTS Master's Level Projects & Papers. 334. https://digitalcommons.odu.edu/ots_masters_projects/334 This Master's Project is brought to you for free and open access by the STEM Education & Professional Studies at ODU Digital Commons. It has been accepted for inclusion in OTS Master's Level Projects & Papers by an authorized administrator of ODU Digital Commons. For more information, please contact [email protected]. A STUDY OF THE USE CLINICIAN I PERSONNEL TO PERFORM INTRAVENOUS THERAPY A Research Paper Presented to the Graduate Faculty of the Department of Occupational and Technical Studies at Old Dominion University In Partial Fulfillment Of the Requirements for the Degree Master of Science in Education by Laura L. Walker August 1996 APPROVAL PAGE This research paper was prepared under the direction of Dr. John M. Ritz, Graduate Advisor. It was submitted to the Graduate Program Director of Occupational and Technical Studies as partial fulfillment of the requirements for the Degree of Master of Science in Education. "-""' Date: !s -I4- - 7b · Graduate Advisor and Graduate Program Director ACKNOWLEDGMENTS This study on the use of unlicensed assistive personnel in health care would have been difficult to prepare without the assistance of the staff members of the Progressive Care Unit of Children's Hospital of the King's Daughters, Norfolk, Virginia. -
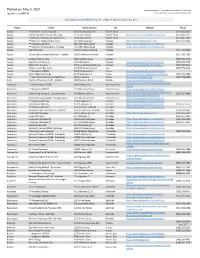
Posted on May 5, 2021 Sites with Asterisks (**) Are Able to Vaccinate 16-17 Year Olds
Posted on May 5, 2021 Sites with asterisks (**) are able to vaccinate 16-17 year olds. Updated at 4:00 PM All sites are able to vaccinate adults 18 and older. Visit www.vaccinefinder.org for a map of vaccine sites near you. Parish Facility Street Address City Website Phone Acadia ** Acadia St. Landry Hospital 810 S Broadway Street Church Point (337) 684-4262 Acadia Church Point Community Pharmacy 731 S Main Street Church Point http://www.communitypharmacyrx.com/ (337) 684-1911 Acadia Thrifty Way Pharmacy of Church Point 209 S Main Street Church Point (337) 684-5401 Acadia ** Dennis G. Walker Family Clinic 421 North Avenue F Crowley http://www.dgwfamilyclinic.com (337) 514-5065 Acadia ** Walgreens #10399 806 Odd Fellows Road Crowley https://www.walgreens.com/covid19vac Acadia ** Walmart Pharmacy #310 - Crowley 729 Odd Fellows Road Crowley https://www.walmart.com/covidvaccine Acadia Biers Pharmacy 410 N Parkerson Avenue Crowley (337) 783-3023 Acadia Carmichael's Cashway Pharmacy - Crowley 1002 N Parkerson Avenue Crowley (337) 783-7200 Acadia Crowley Primary Care 1325 Wright Avenue Crowley (337) 783-4043 Acadia Gremillion's Drugstore 401 N Parkerson Crowley https://www.gremillionsdrugstore.com/ (337) 783-5755 Acadia SWLA CHS - Crowley 526 Crowley Rayne Highway Crowley https://www.swlahealth.org/crowley-la (337) 783-5519 Acadia Miller's Family Pharmacy 119 S 5th Street, Suite B Iota (337) 779-2214 Acadia ** Walgreens #09862 1204 The Boulevard Rayne https://www.walgreens.com/covid19vac Acadia Rayne Medicine Shoppe 913 The Boulevard Rayne https://rayne.medicineshoppe.com/contact -

The Allied Health Care Professional's Role in Assisting Medical Decision
LWW/TLD TLD200107 April 20, 2012 16:4 Top Lang Disorders Vol. 32, No. 2, pp. 119–136 Copyright c 2012 Wolters Kluwer Health | Lippincott Williams & Wilkins The Allied Health Care Professional’s Role in Assisting Medical Decision Making at the End of Life Heather Lambert As a patient approaches the end of life, he or she faces a number of very difficult medical decisions. Allied health care professionals, including speech–language pathologists (SLPs) and occupational therapists (OTs), can be instrumental in assisting their patients to make advance care plans, al- though their traditional job descriptions do not include this role. The allied health care professional is often in a trusted position, permitting insight into the values and beliefs of the patient and fa- cilitating the depth of communication necessary when making difficult decisions. Professionals who work with clients at the end of life need to be aware of the many issues surrounding end- of-life decision making and the preparation of advance directives for care. This article provides an overview of the complex issues the practicing clinician needs to keep in mind when assisting clients with advance care planning. This service requires that clinicians step outside their roles as rehabilitation experts, a move that is supported by professional associations. The concepts of medical decision making and informed consent are discussed in the context of decisions made in advance of illness at the end of life. The professional needs also to be aware of the legali- ties of advance decision making, as laws and statutes differ between states/provinces. There are overarching pieces of legislation that inform local legal and policy issues; the impact of these is briefly addressed. -

Walker-Hackensack-Akeley School District (0113-01)
Special Education Program Compliance Review Final Report June 29, 2018 Walker-Hackensack-Akeley School District (0113-01) Eric Pingrey, Superintendent Eva M Pohl, Director of Special Education Table of Contents Introduction and Authority .................................................................................................................. 3 Scope of Monitoring ........................................................................................................................ 3 Resulting Findings and Corrective Action ....................................................................................... 3 District Overview ............................................................................................................................. 4 Monitoring Findings by Area ............................................................................................................... 4 Area 1: Governance ........................................................................................................................ 4 Area 2: Facilities, Equipment and Materials .................................................................................... 8 Area 3: Child Find and Evaluation ................................................................................................. 10 Area 4: IEP and IFSP Process and Implementation ...................................................................... 14 Summary of Corrective Action Required .......................................................................................... -

Interpretative Statement: Delegation of Health Services in Iowa Schools Melissa Walker, School Nurse Consultant, Iowa Department of Education 2016-2017
Iowa Department of Education Interpretative Statement: Delegation of Health Services in Iowa Schools Melissa Walker, School Nurse Consultant, Iowa Department of Education 2016-2017 Interpretative Statement: Delegation of Health Services in Iowa Schools Purpose: Iowa students, as healthcare consumers, have the right to nursing care that meets the legal standards of health care regardless of the setting (National Council of State Boards of Nursing [NCSBN], 2005) (IAC 655 Chapter 6). School nurses are accountable for their practice of nursing in the educational setting and are also an integral member of the interdisciplinary education team to provide student’s access to quality instruction in the least restrictive, safe school environment. School nurses ensure that students receive health services for physical or mental health conditions that permit school attendance so they may equally access education as their peers and also assist parents or legal guardians to reasonably meet compulsory attendance regulations for their child pursuant to Iowa Code 299. All health services provided to students that constitute nursing or any activity representing nursing in the school setting is a regulatory responsibility of the state licensing board of Nursing (NCSBN, 2005). The purpose of this statement is to provide a resource for Iowa school nurses to maintain accountability in safe, effective nursing practice by working with and through others when using professional judgment in the delegation of nursing tasks for students who require health services to attend school (NCSBN, 2005). Background: Delegation is used in many professional arenas of employment, to include education and healthcare. Nursing delegation in schools is the process conducted by a nurse to transfer to a competent individual the authority to perform selected nursing tasks or activities in selected situations for a student (NCSBN, 2005). -

Evidence-Informed Clinical Perspectives on Selecting Gait Trainer Features for Children with Cerebral Palsy
Analysis Evidence-informed clinical perspectives on selecting gait trainer features for children with cerebral palsy Ginny Paleg, Roslyn Livingstone Background/Aims: Children with cerebral palsy often use gait trainers to augment their mobility. These are supportive walking devices that take the weight of the body through a solid or fabric ‘seat’, stabilise the trunk, and support the pelvis. The purpose of this analysis article is to review the evidence and clinical considerations influencing the selection of gait trainer features for children with cerebral palsy and to describe gait trainer models. Methods: A scoping methodology was used to identify any relevant research and clinical literature supporting the selection of different gait trainer features. An internet search was undertaken to identify a wide range of gait trainers currently available. Factors influencing the selection of different gait trainer features including frame and wheel style and support options are discussed, combining information from manufacturers’ websites, expert opinion and evidence from the literature review. Results: Twenty-seven articles were included in this study. These included nine intervention studies, three articles describing gait trainer development, three expert opinion articles, a survey of therapist opinion and a study comparing physical properties of three different gait trainers. In addition information on device features relevant to gait trainers was drawn from 10 intervention studies of children using hand-held walkers. Twenty-four different gait trainers were identified as being commercially available in the UK, Canada and USA at time of searching. Conclusions: Evidence supporting selection of gait trainer styles and features for children with cerebral palsy is very limited. -

Template for Program Evaluations
Evaluation of the Special Education Programs Department of Special Education Hingham Public Schools Hingham, Massachusetts Conducted: March/April 2012 Submitted by: James A. Shillinglaw, CAS Walker Partnerships A Division of Walker Needham, Massachusetts 02492 Table of Contents: I. Introduction A. Purpose B. Reviewer II. Methodology III. Commendations IV. Factors Affecting the Implementation of Programming & Services V. Findings VI. Recommendations VII. Summary 2 I. Introduction The Director of Student Services, Dr. Jean Loud, requested that Walker Partnerships conduct an evaluation of the special education programs for the Hingham Public Schools. The overall focus of this review is to gain a greater understanding of the current status of special education programs and services within the district, identify the strengths of the existing programming, and determine what issues need to be addressed to enhance current programming. The administration wants to procure recommendations that will assist them with addressing future program needs, the inclusion of students with disabilities in general education classes and activities, and the instructional supports that may be required to ensure greater access to the general curriculum for students with special needs. A. Purpose The purpose of an independent evaluation of a specific program and service is to provide a school district with an objective report that identifies areas of strengths, needs, and recommendations. An independent evaluation allows for the district to be examined from the perspective that looks at what is working well in the district, but also speaks to areas that need to be strengthened. This evaluation is focused on the specific domain of programming and services that serves students with special needs. -

Occupational Therapy Learner Guide: Support the Fitting of Assistive Devices - Ii
Allied Health Professions’ Office of Queensland Occupational Therapy Learner Guide Support the fitting of assistive devices April 2017 Occupational Therapy Learner Guide – Support the fitting of assistive devices Published by the State of Queensland (Queensland Health), April 2017 This document is licensed under a Creative Commons Attribution 3.0 Australia licence. To view a copy of this licence, visit creativecommons.org/licenses/by/3.0/au © State of Queensland (Queensland Health) 2017. You are free to copy, communicate and adapt the work, as long as you attribute the State of Queensland (Queensland Health). For more information contact: Intellectual Property Officer, Department of Health, GPO Box 48, Brisbane QLD 4001, email [email protected], phone (07) 3328 9862. An electronic version of this document is available at https://www.health.qld.gov.au/ahwac/html/ahassist-modules/ Disclaimer: The content presented in this publication is distributed by the Queensland Government as an information source only. The State of Queensland makes no statements, representations or warranties about the accuracy, completeness or reliability of any information contained in this publication. The State of Queensland disclaims all responsibility and all liability (including without limitation for liability in negligence) for all expenses, losses, damages and costs you might incur as a result of the information being inaccurate or incomplete in any way, and for any reason reliance was placed on such information. Occupational Therapy Learner Guide: Support the fitting of assistive devices - ii - Acknowledgement The Allied Health Professions’ Office of Queensland wishes to acknowledge the Queensland Health Allied Health Clinicians who have contributed to the development of these learning support materials. -

Guide to Walking Aids: Canes, Crutches, and Walkers
GUIDE TO WALKING AIDS: CANES, CRUTCHES, AND WALKERS The U.S. Census Bureau estimates that over 12% of Americans aged 15 years and older have difficulty walking and that almost 5% use crutches or a cane or walker to assist them with walking (Brault, 2012). Further, among American seniors, over 16% use a cane and over 11% use walkers (Reidel, 2015). There are many assistive technology (AT) aids on the market today to assist you with walking. The most common are canes, crutches, walkers, and rollators. This guide provides you with an overview and examples of these aids. Canes Standard Walking Cane A standard walking cane consists of a wooden or metal shaft with a handle at one end that you can grip with one hand, and a tip at the other end that touches the ground. The handle can be straight, flat, curved, or offset. The grip on the handle can be smooth or have finger holds. A cane with an offset handle has a shaft that curves at one end, resembling the top of a question mark. Some standard walking canes have height-adjustable shafts and are also foldable—usually into four interlocking sections—for storage and transport when not in use. The tip may be made of the same material as the shaft, or it may be made of metal or rubber. For some standard canes, a special tip may be added for additional traction or stability. For example, three- and four-pronged tips provide slightly more stability and allow the cane to stand upright when not in use. -
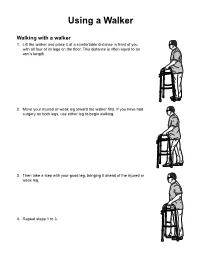
Using a Walker
Using a Walker Walking with a walker 1. Lift the walker and place it at a comfortable distance in front of you with all four of its legs on the floor. This distance is often equal to an arm’s length. 2. Move your injured or weak leg toward the walker first. If you have had surgery on both legs, use either leg to begin walking. 3. Then take a step with your good leg, bringing it ahead of the injured or weak leg. 4. Repeat steps 1 to 3. 2 healthinfotranslations.org Safety tips • Do not step too close to the walker because you may lose your balance. There should be space between you and the walker at all times. • Hold your head up and look straight ahead. Do not watch your feet. It is more tiring and you may run into something. • Walk slowly. Sitting with a walker 1. Slowly back up to the chair, bed or toilet until you feel it against the back of your legs. 2. Let go of the walker with one hand and reach back for the bed, chair arms or toilet seat, while sliding your injured or weak leg forward. healthinfotranslations.org 3 3. Slowly lower yourself to the seat by leaning forward and keeping your injured or weak leg straight out in front of you. Go slowly so that you do not land heavy in the chair. 4. If you have had surgery on both legs, place both hands on the chair arms, bed or commode seat. Lower yourself to the seat and slowly walk both legs forward. -

Sally Mallory, PT, ATP, CPST 214-763-9173 [email protected]
2020-04-27 Gait Analysis and Equipment Selection 1 Sally Mallory, PT, ATP, CPST 214-763-9173 [email protected] 2 1 2 2020-04-27 Thank you to our contributors • All of the children and their families, caregivers and therapists • Missy Ball, PT • Sally Mallory, PT, ATP, CPST • Jo McConnell, PT • Bente Storm, PT • Helle Rasmussen, PhD, PT • Lynda Reagan, PT • Megan Salley, MOTR/L • Elaine Westlake, PT, DPT, MA • Julie Kobak, MA, CCC-SLP This webinar is being recorded 3 4 2 4 2020-04-27 5 5 Our family of products 3 6 2020-04-27 Course Outline Importance of independent mobility Gait analysis with instrumentation & case study Factors impacting functional mobility Analysis of gait cycle Phases of gait Shank & thigh kinematics Ambulation equipment types Considerations for equipment selection BWSTT treadmill training vs ground training 7 7 During Ambulation • The whole body is active • Bones, joints and muscles, nerves, senses, heart and lungs work together and movements are coordinated. • To be able to walk, head and trunk control together with balance and active use of arms and legs are needed. 8 4 8 2020-04-27 Importance of Independent Mobility Increases level of engagement in educational and recreational activities Promotes problem solving skills Enhances quality of interactive behavior with other children, adults Increases exploration of environment Promotes cognitive, perceptual and visual spatial skills by learning to navigate around obstacles, avoid stairs or other drop offs Promotes healthy functioning of physiological systems (heart,