Acsm Current Comment
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The 7 Step Shin Splints Treatment System
The Step SShhiinn SSpplliinnttss Treatment System By Brad Walker TM The 7 Step Shin Splints Treatment System Fix Your Shin Splints Once and For All and get back to Pain Free Running Quickly and Safely. Walker, Bradley E., 1971 7 Step Shin Splints Treatment System™ Copyright © 2012 The Stretching Institute™ All rights reserved. Except under conditions described in the copyright act, no part of this publication may in any form or by any means (electronic, mechanical, micro copying, photocopying, recording or otherwise) be reproduced, stored in a retrieval system or transmitted without prior written permission from the copyright owner. Inquires should be addressed to the publisher. Disclaimers The exercises presented in this publication are intended as an educational resource and are not intended as a substitute for proper medical advice. Please consult your physician, physical therapist or sports coach before performing any of the exercises described in this publication, particularly if you are pregnant, elderly or have any chronic or recurring muscle or joint pain. Discontinue any exercise that causes you pain or severe discomfort and consult a medical expert. Cover picture/s supplied by iStockphoto. The Stretching Institute has purchased the non-exclusive, non-transferable, non-sub licensable right to reproduce the cover picture/s an unlimited number of times in online and electronic publications, and web advertisements. Exercise graphics used with permission from the Physigraphe V2 Pro Clip Art CD-ROM available at ExRx.net. Copyright -

Shin Splints
A Patient’s Guide to Shin Splints Orthopedic and Sports Physical Therapy 245 North College Lafayette, LA 70506 Phone: 337.232.5301 Fax: 337.237.6504 Compliments of: Orthopedic and Sports Physical Therapy DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments orA treatments.Patient's The information Guide shouldto Shin NOT be Splints used in place of a visit with your health care provider, nor should you disregard the advice of your health care provider because of any information you read in this booklet. Orthopedic and Sports Physical Therapy Thank you for requesting your Orthopaedic and Sports Physical Therapy Patient Guide and giving us the opportunity to help you better understand your condition. Once you've had a chance to review the information provided, you may have additional questions. If that's the case, we would like to offer you a FREE consultation to discuss your condition more fully, answer all of your questions, and give you our best advice on how you can resolve your pain quickly and easily. To arrange your FREE consultation, please contact us at 337.232.5301 and begin feeling good again! Call today and begin feeling better tomorrow. The OSPT Team Orthopedic and Sports Physical Therapy 245 North College Lafayette, LA 70506 Phone: 337.232.5301 Fax: 337.237.6504 www.ospt.net All materials within these pages are the sole property of Medical Multimedia Group, LLC and are used herein by permission. -

Your Guide to Playing Safe Staying Active by Participating in Sports Is a Great Way to Be Healthy
Your Guide to Playing Safe Staying active by participating in sports is a great way to be healthy. All that running, jumping and stretching, though, carries the risk of injury. Play it safe with this quick guide to common problems. An adult sports medicine overview with contributions from sports medicine experts Sally Harris, MD, and Amol Saxena, DPM. TOP INJURIES BY SPORT Running Knee injuries, particularly irritation of the cartilage on the underside of the kneecap Shin splints Achilles tendinitis Plantar fasciitis (irritation in the tendons and ligaments that run from the heel to toes) Ankle sprains and calf strains General overuse injuries such as sprains, strains and stress fractures Swimming Overuse and repetitive motion injury to the shoulder or knee Cycling Achilles peritondinesis (inflammation of the tendon sheath) Patellofemoral pain syndrome (cartilage irritation on the underside of the kneecap) Lower back pain from hunched posture and poor bike fit Traumatic injury from high-speed falls Pelvic nerve pressure and pain—alleviated with padded bike shorts Nerve inflammation in the hands—alleviated with cushioned bike gloves and padded handle bars Baseball/Softball Shoulder problems (rotator cuff injuries and shoulder tendinitis) Pitchers—tendinitis of the shoulder, back, neck, elbow, forearm and wrist; tears to the ulnar collateral ligament in the elbow Catchers—risk of back and knee problems Ankle sprains and fractures Traumatic injuries due to ball hitting body Basketball Jammed fingers Knee or ankle injuries -

Effects of Q-Angle on Lower Extremity Biomechanics And
EFFECTS OF Q-ANGLE ON LOWER EXTREMITY BIOMECHANICS AND INJURIES IN FEMALE COLLEGIATE TRACK AND FIELD ATHLETES By MYRANDA HOPE HAM Candidate for Master of Science in Engineering, Biomedical Engineering, Mercer University, May 2020 A Thesis Submitted to the Graduate Faculty of Mercer University School of Engineering in Partial Fulfillment of the Requirements for the Degree MASTER OF SCIENCE IN ENGINEERING MACON, GA 2020 EFFECTS OF Q-ANGLE ON LOWER EXTREMITY BIOMECHANICS AND INJURIES IN FEMALE COLLEGIATE TRACK AND FIELD ATHLETES By MYRANDA HOPE HAM Approved: ______________________________________ Date __________________ Dr. Ha Vo, Advisor ______________________________________ Date __________________ Dr. Edward O’Brien, Committee Member ______________________________________ Date __________________ Dr. Richard Kunz, Committee Member ______________________________________ Date __________________ Dr. Laura Lackey, Dean ACKNOWLEDGEMENTS I would like to first thank Dr. Vo for all his help throughout this project. I would not have been able to complete this study without his guidance. Thank you to Dr. Kunz and Dr. O’Brien for serving as member of my committee. Thank you to Amos Mansfield for approving this study to be conducted with Mercer University student-athletes. Thank you to all the Mercer Women’s Track and Field coaches, including Josh Hayman, Leesa Morales, and Jerod Wims, for being flexible and allowing the athletes to participate in this study around their practice schedule. Thank you to every member of the Mercer Women’s Track and -

Achilles Tendon
Achilles Tendon The Achilles tendon, the largest and single strongest tendon in the body, connects the heel bone to the muscles in the back of your leg and thigh. The primary function of the Achilles tendon is to transmit the power of these muscles to the foot enabling walking and running. Why do Achilles tendon injuries occur? Achilles tendon injuries can occur especially when the tendon is subjected to strong forces such as in velocity sports: running, soccer, basketball, tennis, and baseball. Additionally, aging, and the Achilles tendons poor blood supply also increases your chance of injury. The area of the tendon with the poorest blood supply is the area (2 to 6 cm) just above its insertion into the heel bone. The blood flow to this area decreases as you get older. This means, older active individuals are more vulnerable to injury and need especially to take precautions such as wearing appropriate athletic gear, and doing proper stretching. People who over pronate , (flattening of the arch, turning out of the heels and splaying outward of the forefoot) can especially develop in unstable shoe gear foot pain as well as, Achilles tendinitis and Achilles tendonosis, two common overuse disorders that occur in the Achilles tendon, bunions, hammertoes , plantar fasciitis , shin splints and knee pain. Athletes and laborers who routinely put added stresses on their feet are vulnerable to Achilles tendon injuries. Weekend warriors, who are not in proper condition and infrequently, participate in athletic activities also are at greater risk for Achilles tendon injuries. Injury to the Achilles tendon can be sudden or gradual and the healing course can be lengthy. -

Guide to Prevention of Sports Injuries Guide to Prevention of Sports Injuries
Guide to Prevention of Sports Injuries Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefts for your physical and mental health. While exercise and sports-related activities often have a positive impact on our lives, they can also lead to serious injury. The last thing you want is to disrupt your exercise routine with an injury, requiring you to start all over again once you’re healed. Following are some tips to help you remain injury-free. Tips for Prevention of Causes of Sports Injuries Sports Injuries While sports injuries are highly prevalent among athletes, anyone who engages in physical activity can be injured. Warm Up. Common causes of sports injuries include: Always take time to warm up and stretch before a workout. • Not warming up or stretching properly before exercising A warm-up gets your body ready for exercise by gradually increasing your heart rate and loosening your muscles and • Using inadequate exercise equipment joints. Warm up by walking, cycling or jogging for 5 to 10 • Poor technique while exercising minutes. Once your body is warm, do some stretching to • Overtraining or pushing yourself too hard increase fexibility. • A traumatic accident Increase your range gradually. A key to preventing injuries is to gradually build the intensity, duration and frequency of your workouts. Avoid pushing When to Ice or Heat an Injury yourself too hard, too fast. Follow the 10 percent rule to increase activity in increments of 10 percent per week. Ice: Exercise consistently. • Apply ice for the frst 72 hours following injury to reduce infammation as long as swelling is Avoid the “weekend warrior” syndrome that compresses exercise into two days for the entire week. -

Ortho Symptoms Chart
3688 Veterans Memorial Dr. Hattiesburg, MS 39401 appointments, referrals & 2nd opinions: 601-554-7400 Online encyclopedia about orthopedics and spine care at: SouthernBoneandJoint.com UNDERSTANDING JOINT PAIN SYMPTOMS & WHEN YOU NEED TO SEE THE DOCTOR TRAUMA, FALL, FRACTURE: TRAUMA: Any time there is trauma (fall, impact, car accident) HAND: along with pain, a bone or joint could have fractured. NUMBNESS/WEAKNESS IN ARM / HAND: X-rays will be needed to check for broken bones. See an Numbness or weakness in the arm or hand can orthopedic specialist or an Emergency Room. be an emergency symptom related to a herniated disc in the neck. Left untreated, the symptom can become permanent. You should see a spine SHOULDER: specialist within 3 days. FROZEN SHOULDER can develop from NUMB FINGERS: Numbness in the tips of the overuse or inflammation. fingers can relate to Carpal Tunnel Syndrome. BURSITIS can make it difficult to raise the Watchful waiting with the use of a brace can be arm with twinges of pain. tried for a couple months. Numbness, if ignored TENDONITIS is inflammation of the over several months, can become permanent tendon which connects muscle to bone. and lifelong, along with weakness in grip. Self care for all three can include anti- Treatment can include a 30-minute surgery to inflammatories and R-I-C-E: Rest, Ice, relieve the tightness in the wrist. Compression & Elevation. Rest your shoulder for a day or so, using ice for 10 HIP PAIN not linked to dislocation due to trauma, fall or car minutes at a time. Compress the shoulder accident, is often linked to bursitis (inflammation of the joint) snugly with an elastic band (not tightly) or degeneration of the hip joint due to arthritis which damages and lie down with the shoulder elevated. -
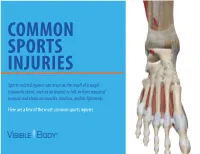
Sports-Related Injuries Can Occur As the Result of a Single Traumatic Event, Such As an Impact Or Fall, Or from Repeated Overuse
COMMON SPORTS INJURIES Sports-related injuries can occur as the result of a single traumatic event, such as an impact or fall, or from repeated overuse and strain on muscles, tendons, and/or ligaments. Here are a few of the most common sports injuries. BICEPS FEMORIS (LONG HEAD) PULLING YOUR LEG Strains and sprains make up the bulk of sports injuries. Strains happen when muscles or SEMITENDINOSUS tendons are overstretched or torn - if someone has a pulled muscle, that means they have a muscle strain. The most commonly strained muscles are the hamstrings. SEMIMEMBRANOSUS Strains are best prevented by proper stretching, strengthening, and proper warm-ups before athletic activity. 2 SPRAIN, SPRAIN GO AWAY ANTERIOR TALOFIBULAR LIGAMENT Sprains happen when ligaments (PARTIALLY TORN) are overstretched or torn. Sprained ankles often happen when a fall or awkward landing from a jump forces the ankle joint to move in an unusual way, stressing or possibly tearing the ligaments surrounding it. Walking, running, or jumping on an uneven surface can also cause a sprained ankle. Stretching, strengthening, and balance exercises (as well as supportive footwear) can help reduce the risk of ankle sprains. 3 YOU’RE FEMUR TEARING ME APART! Many other muscles, tendons, and ligaments frequently tear. ACL (anterior cruciate ligament tears tend to happen in sports that put stress on the knees through jumping, sudden stops, and rapid changes in direction. Keeping the strength of hamstring PATELLA and quadriceps muscles balanced and (KNEECAP) TIBIA practicing safe landing and pivoting techniques can help prevent ACL tears. Factoid! Around 55% of sports-related injuries involve the knees. -
EXERCISE RELATED SHIN PAIN – ‘No More Shin Splints!’
Dr JOHN P BEST B Med, Dip Sports Med (London), FACSP, FFSEM Sports Physician Conjoint Lecturer, University NSW Sports and Exercise Medicine EXERCISE RELATED SHIN PAIN – ‘no more shin splints!’ Shin and leg pain which occurs with exercise and other physical activity is very common. Shin pain comprises up to 12% of all sports injuries, affecting almost 30% of runners and a third of those in military training. The name for shin pain was previously ‘shin splints’. This is an unhelpful term and is not a diagnosis. When diagnosing shin pain, we need to establish whether it is from a localised problem or referred from another area. In the latter, it is relatively common to suffer shin or leg pain which is referred from the lower back (eg sciatica, pinched nerve). Also, there are some circulation disorders which may cause exercise-related shin or leg pain. This is known as claudication, and it is due to narrowing of the blood vessels to the leg, usually due to atherosclerosis (disease of the arteries). Often there is an overlap of different causes of shin pain. The pain may be muscular, from the bone, or from the lining of the bone. Occasionally, problems related to nerves or blood vessels being compressed may occur. The most common cause of shin pain with exercise is muscular . This is sometimes referred to as myofascial pain . It is common in those under 30 years of age and is associated with a recent increase in weight-bearing exercise (eg jogging). Another feature of myofascial pain is that it reduces when you have warmed up, but it usually recurs towards the end of physical activity. -

Achilles Tendinitis in Running Athletes Andrew W
J Am Board Fam Pract: first published as 10.3122/jabfm.2.3.196 on 1 July 1989. Downloaded from Achilles Tendinitis In Running Athletes Andrew W. Nichols, M.D. Abstract: Achilles tendinitis is an injury that com normalities that predispose to Achilles tendinitis in monly affects athletes in the running and jumping clude gastrocnemius-soleus muscle weakness or in sports. It results from repetitive eccentric load-in flexibility and hindfoot malalignment with foot duced microtrauma that stresses the peritendinous hyperpronation. structures causing inflammation. Achilles tendinitis The initial treatment should be conservative with may be classified histologically as peritendinitis, ten relative rest, gastrocnemius-soleus rehabilitation. dinosis, or partial tendon rupture. cryotherapy, heel lifts, nonsteroidal anti-inflamma Training errors are frequently responsible for the tory drugs, and correction of biomechanical abnor onset of Achilles tendinitis. These include excessive malities. Surgery is recommended only for persons running mileage and training intensity, hill running, with chronic symptoms who wish to continue run running on hard or uneven surfaces, and wearing ning and have not benefited from conservative ther poorly designed running shoes. Biomechanical ab- apy. (J Am Bd Fam Pract 1989; 2:196-203.) In Homer's Iliad, the Greek chieftain Achilles was Anatomy mortally wounded by an arrow that pierced his The Achilles tendon (calcaneal tendon), which in heel, which was his only unprotected area, be serts on the calcaneus. is the common tendon of cause the remainder of his body had been made the gastrocnemius and soleus muscles. The gas invulnerable by an Immersion in the River Styx. 1 trocnemius muscle arises from two heads origi Today, the Achilles tendon is a common site of nating on the femoral condyles and lies superficial athletic injury because of the demanding training to the soleus. -

Rotator Cuff Tendinitis Shoulder Joint Replacement Mallet Finger Low
We would like to thank you for choosing Campbell Clinic to care for you or your family member during this time. We believe that one of the best ways to ensure quality care and minimize reoccurrences is through educating our patients on their injuries or diseases. Based on the information obtained from today's visit and the course of treatment your physician has discussed with you, the following educational materials are recommended for additional information: Shoulder, Arm, & Elbow Hand & Wrist Spine & Neck Fractures Tears & Injuries Fractures Diseases & Syndromes Fractures & Other Injuries Diseases & Syndromes Adult Forearm Biceps Tear Distal Radius Carpal Tunnel Syndrome Cervical Fracture Chordoma Children Forearm Rotator Cuff Tear Finger Compartment Syndrome Thoracic & Lumbar Spine Lumbar Spine Stenosis Clavicle Shoulder Joint Tear Hand Arthritis of Hand Osteoporosis & Spinal Fx Congenital Scoliosis Distal Humerus Burners & Stingers Scaphoid Fx of Wrist Dupuytren's Comtracture Spondylolysis Congenital Torticollis Shoulder Blade Elbow Dislocation Thumb Arthritis of Wrist Spondylolisthesis Kyphosis of the Spine Adult Elbow Erb's Palsy Sprains, Strains & Other Injuries Kienböck's Disease Lumbar Disk Herniation Scoliosis Children Elbow Shoulder Dislocation Sprained Thumb Ganglion Cyst of the Wrist Neck Sprain Scoliosis in Children Diseases & Syndromes Surgical Treatments Wrist Sprains Arthritis of Thumb Herniated Disk Pack Pain in Children Compartment Syndrome Total Shoulder Replacement Fingertip Injuries Boutonnière Deformity Treatment -

Recruit Medicine Chapter 9 Management and Treatment Of
Management and Treatment of Training-Related Injuries in Initial Entry Training Chapter 9 MANAGEMENT AND TREATMENT OF TRAINING-RELATED INJURIES IN INITIAL ENTRY TRAINING † ‡ KEITH G. HAURET, MPT, MSPH*; BRUCE H. JONES, MD, MPH ; AND JOSEPH J. KNAPIK, ScD INTRODUCTION TYPES OF TRAINING-RELATED INJURIES Acute Injuries Overuse Injuries BASIC PRINCIPLES OF CARE FOR TRAINING-RELATED INJURIES Rest Ice Compression Elevation Nonsteroidal Anti-inflammatory Drugs SUMMARY * Lieutenant Colonel, Medical Specialist Corps, US Army (Retired); Epidemiologist, Injury Prevention Program, Directorate of Epidemiology and Disease Surveillance, US Army Center for Health Promotion and Preventive Medicine, Aberdeen Proving Ground, Maryland 21010 † Colonel, Medical Corps, US Army (Retired); Program Manager, Injury Prevention Program, Directorate of Epidemiology and Disease Surveillance, US Army Center for Health Promotion and Preventive Medicine, Aberdeen Proving Ground, Maryland 21010 ‡ Major, Medical Service Corps, US Army (Retired); Research Physiologist, Injury Prevention Program, Directorate of Epidemiology and Disease Surveil- lance, US Army Center for Health Promotion and Preventive Medicine, Aberdeen Proving Ground, Maryland 21010 147 Recruit Medicine INTRODUCTION Recruits entering the US Army begin their military of knowledge about specific injury risk factors. Health- training at one of the Army’s initial entry training care providers should recognize injuries at the earliest (IET) posts. For most recruits, the process begins with possible point, treat them immediately, and provide basic combat training (BCT), in which fundamental optimal methods of rehabilitation. Thus, the goals of soldier skills, military customs and courtesies, and injury management and treatment are to (a) minimize Army values are introduced. Physical fitness is also damage once the injury has occurred, (b) return the re- an important element of BCT.