Human Anatomy & Physiology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Cardiovascular System 9
Chapter Cardiovascular System 9 Learning Outcomes On completion of this chapter, you will be able to: 1. State the description and primary functions of the organs/structures of the car- diovascular system. 2. Explain the circulation of blood through the chambers of the heart. 3. Identify and locate the commonly used sites for taking a pulse. 4. Explain blood pressure. 5. Recognize terminology included in the ICD-10-CM. 6. Analyze, build, spell, and pronounce medical words. 7. Comprehend the drugs highlighted in this chapter. 8. Describe diagnostic and laboratory tests related to the cardiovascular system. 9. Identify and define selected abbreviations. 10. Apply your acquired knowledge of medical terms by successfully completing the Practical Application exercise. 255 Anatomy and Physiology The cardiovascular (CV) system, also called the circulatory system, circulates blood to all parts of the body by the action of the heart. This process provides the body’s cells with oxygen and nutritive ele- ments and removes waste materials and carbon dioxide. The heart, a muscular pump, is the central organ of the system. It beats approximately 100,000 times each day, pumping roughly 8,000 liters of blood, enough to fill about 8,500 quart-sized milk cartons. Arteries, veins, and capillaries comprise the network of vessels that transport blood (fluid consisting of blood cells and plasma) throughout the body. Blood flows through the heart, to the lungs, back to the heart, and on to the various body parts. Table 9.1 provides an at-a-glance look at the cardiovascular system. Figure 9.1 shows a schematic overview of the cardiovascular system. -

Gross Anatomical Studies on the Arterial Supply of the Intestinal Tract of the Goat
IOSR Journal of Agriculture and Veterinary Science (IOSR-JAVS) e-ISSN: 2319-2380, p-ISSN: 2319-2372. Volume 10, Issue 1 Ver. I (January. 2017), PP 46-53 www.iosrjournals.org Gross Anatomical Studies on the Arterial Supply of the Intestinal Tract of the Goat Reda Mohamed1, 2*, ZeinAdam2 and Mohamed Gad2 1Department of Basic Veterinary Sciences, School of Veterinary Medicine, Faculty of Medical Sciences, University of the West Indies, Trinidad and Tobago. 2Anatomy and Embryology Department, Faculty of Veterinary Medicine, Beni Suef University Egypt. Abstract: The main purpose of this study was to convey a more precise explanation of the arterial supply of the intestinal tract of the goat. Fifteen adult healthy goats were used. Immediately after slaughtering of the goat, the thoracic part of the aorta (just prior to its passage through the hiatus aorticus of the diaphragm) was injected with gum milk latex (colored red) with carmine. The results showed that the duodenum was supplied by the cranial pancreaticoduodenal and caudal duodenal arteries. The jejunum was supplied by the jejunal arteries. The ileum was supplied by the ileal; mesenteric ileal and antimesenteric ileal arteries. The cecum was supplied by the cecal artery. The ascending colon was supplied by the colic branches and right colic arteries. The transverse colon was supplied by the middle colic artery. The descending colon was supplied by the middle and left colic arteries. The sigmoid colon was supplied by the sigmoid arteries. The rectum was supplied by the cranial; middle and caudal rectal arteries. Keywords: Anatomy,Arteries, Goat, Intestine I. Introduction Goats characterized by their high fertility rate and are of great economic value; being a cheap meat, milk and some industrial substances. -

Threatening External Iliac Vein Injury During Total Hip Arthroplasty
경희의학 : 제 27 권 제 1 호 □ 증 례 □ J Kyung Hee Univ Med Cent : Vol. 27, No. 1, 2011 Threatening External Iliac Vein Injury during Total Hip Arthroplasty Kang Woo Lee, M.D., Jo Young Hyun, M.D., Jae Woo Yi, M.D., Ph.D. Department of Anesthesiology and Pain Medicine, School of Medicine, Kyung Hee University, Seoul, Korea INTRODUCTION nal iliac vein during total hip replacement, which resulted in hemorrhagic shock. Since its inception in the 1960’s, total hip arthro- plasty (THA) has grown in volume and complexity. CASE REPORT Total hip arthroplasty has revolutionized the treatment of end-stage hip arthritis and is felt to be among the A 63-year-old female patient (150 cm, 59 kg) was most cost effective of all medical interventions diagnosed as secondary osteoarthritis of left hip joint. available.(1) The complications associated with THA She was scheduled to undergo total hip replacement. have been increased as a result of increasing life The patient’s previous medical history entailed ten expectancy and widened indications for THA. But the years of hypertension, which was well-controlled with complications related to total hip arthroplasty are not oral anti-hypertensive drugs. Routine monitors such as common. Especially vascular injuries are very rare but electrocardiogram, pulse oxymeter, non-invasive blood can cause limb loss or become life threatening. A pressure were used. Induction of anesthesia was achieved thorough understanding of the possible complications with propofol 120 mg, rocuronium 50 mg intravenously. following total hip arthroplasty aids in optimizing Anesthesia was maintained with sevoflurane. After loss patient outcomes The occurrence of the complication of all four twitches from the train-of-four obtained by related to THA has not been emphasized enough in ulnar nerve stimulation, endotracheal intubation was anesthesia literature and has been overlooked in the performed. -

Prep for Practical II
Images for Practical II BSC 2086L "Endocrine" A A B C A. Hypothalamus B. Pineal Gland (Body) C. Pituitary Gland "Endocrine" 1.Thyroid 2.Adrenal Gland 3.Pancreas "The Pancreas" "The Adrenal Glands" "The Ovary" "The Testes" Erythrocyte Neutrophil Eosinophil Basophil Lymphocyte Monocyte Platelet Figure 29-3 Photomicrograph of a human blood smear stained with Wright’s stain (765). Eosinophil Lymphocyte Monocyte Platelets Neutrophils Erythrocytes "Blood Typing" "Heart Coronal" 1.Right Atrium 3 4 2.Superior Vena Cava 5 2 3.Aortic Arch 6 4.Pulmonary Trunk 1 5.Left Atrium 12 9 6.Bicuspid Valve 10 7.Interventricular Septum 11 8.Apex of The Heart 9. Chordae tendineae 10.Papillary Muscle 7 11.Tricuspid Valve 12. Fossa Ovalis "Heart Coronal Section" Coronal Section of the Heart to show valves 1. Bicuspid 2. Pulmonary Semilunar 3. Tricuspid 4. Aortic Semilunar 5. Left Ventricle 6. Right Ventricle "Heart Coronal" 1.Pulmonary trunk 2.Right Atrium 3.Tricuspid Valve 4.Pulmonary Semilunar Valve 5.Myocardium 6.Interventricular Septum 7.Trabeculae Carneae 8.Papillary Muscle 9.Chordae Tendineae 10.Bicuspid Valve "Heart Anterior" 1. Brachiocephalic Artery 2. Left Common Carotid Artery 3. Ligamentum Arteriosum 4. Left Coronary Artery 5. Circumflex Artery 6. Great Cardiac Vein 7. Myocardium 8. Apex of The Heart 9. Pericardium (Visceral) 10. Right Coronary Artery 11. Auricle of Right Atrium 12. Pulmonary Trunk 13. Superior Vena Cava 14. Aortic Arch 15. Brachiocephalic vein "Heart Posterolateral" 1. Left Brachiocephalic vein 2. Right Brachiocephalic vein 3. Brachiocephalic Artery 4. Left Common Carotid Artery 5. Left Subclavian Artery 6. Aortic Arch 7. -

Molecular Signatures of Tissue-Specific
Developmental Cell Resource Molecular Signatures of Tissue-Specific Microvascular Endothelial Cell Heterogeneity in Organ Maintenance and Regeneration Daniel J. Nolan,1,6 Michael Ginsberg,1,6 Edo Israely,1 Brisa Palikuqi,1 Michael G. Poulos,1 Daylon James,1 Bi-Sen Ding,1 William Schachterle,1 Ying Liu,1 Zev Rosenwaks,2 Jason M. Butler,1 Jenny Xiang,4 Arash Rafii,1,7 Koji Shido,1 Sina Y. Rabbany,1,8 Olivier Elemento,3 and Shahin Rafii1,5,* 1Department of Genetic Medicine, Howard Hughes Medical Institute 2Ronald O. Perelman and Claudia Cohen Center for Reproductive Medicine 3HRH Prince Alwaleed Bin Talal Bin Abdulaziz Alsaud Institute for Computational Biomedicine 4Genomics Resource Core Facility Weill Cornell Medical College, New York, NY 10065, USA 5Ansary Stem Cell Institute, New York, NY 10065, USA 6Angiocrine Bioscience, New York, NY 10065, USA 7Weill Cornell Medical College-Qatar, Stem Cell and Microenvironment Laboratory, Education City, Qatar Foundation, Doha 24144, Qatar 8Bioengineering Program, Hofstra University, Hempstead, NY 11549, USA *Correspondence: srafi[email protected] http://dx.doi.org/10.1016/j.devcel.2013.06.017 SUMMARY been appreciated. Capillary ECs of the blood brain barrier (BBB) form a restrictive environment for passage between the Microvascular endothelial cells (ECs) within different brain tissue and the circulating blood. Many of the trafficking pro- tissues are endowed with distinct but as yet unrecog- cesses that are passive in other vascular beds are tightly nized structural, phenotypic, and functional attri- controlled in the brain (Rubin and Staddon, 1999). As opposed butes. We devised EC purification, cultivation, to the BBB, the capillary ECs of the kidney glomeruli are fenes- profiling, and transplantation models that establish trated for the filtration of the blood (Churg and Grishman, tissue-specific molecular libraries of ECs devoid of 1975). -

Corona Mortis: the Abnormal Obturator Vessels in Filipino Cadavers
ORIGINAL ARTICLE Corona Mortis: the Abnormal Obturator Vessels in Filipino Cadavers Imelda A. Luna Department of Anatomy, College of Medicine, University of the Philippines Manila ABSTRACT Objectives. This is a descriptive study to determine the origin of abnormal obturator arteries, the drainage of abnormal obturator veins, and if any anastomoses exist between these abnormal vessels in Filipino cadavers. Methods. A total of 54 cadaver halves, 50 dissected by UP medical students and 4 by UP Dentistry students were included in this survey. Results. Results showed the abnormal obturator arteries arising from the inferior epigastric arteries in 7 halves (12.96%) and the abnormal communicating veins draining into the inferior epigastric or external iliac veins in 16 (29.62%). There were also arterial anastomoses in 5 (9.25%) with the inferior epigastric artery, and venous anastomoses in 16 (29.62%) with the inferior epigastric or external iliac veins. Bilateral abnormalities were noted in a total 6 cadavers, 3 with both arterial and venous, and the remaining 3 with only venous anastomoses. Conclusion. It is important to be aware of the presence of these abnormalities that if found during surgery, must first be ligated to avoid intraoperative bleeding complications. Key Words: obturator vessels, abnormal, corona mortis INtroDUCTION The main artery to the pelvic region is the internal iliac artery (IIA) with two exceptions: the ovarian/testicular artery arises directly from the aorta and the superior rectal artery from the inferior mesenteric artery (IMA). The internal iliac or hypogastric artery is one of the most variable arterial systems of the human body, its parietal branches, particularly the obturator artery (OBA) accounts for most of its variability. -

Prenatal Diagnosis of a Variant of the Azygos Venous System
Lo Verso et al. SpringerPlus (2016) 5:1334 DOI 10.1186/s40064-016-2956-0 SHORT REPORT Open Access Prenatal diagnosis of a variant of the azygos venous system Clelia Lo Verso1*, Valentina Cigna2, Gianfranca Damiani2, Laura Lo Verso1, Rossella Conti3 and Vincenzo Duca3 Abstract Background: The azygos venous system consists of the azygos vein on the right side and the hemiazygos and accessory hemiazygos on the left side. The azygos vein runs through the abdominal cavity along the right side of the vertebral bodies, in a cranial direction, passes through the diaphragm and reaches the mediastinum, where it forms the arch of the azygos which flows into the superior vena cava. Along its course, the azygos vein communicates with the intercostal veins on the right, the hemiazygos vein that collects blood from the left lower intercostal veins, and accessory hemiazygos vein that drains into the left upper intercostal veins. The last two, at the level of the seventh thoracic vertebra, unite and end in the azygos vein. The accessory hemiazygos vein is normally included in the length between T4 and T8. The embryological origin of the accessory hemiazygos vein is the result of an expansion in the direction of the cranial hemiazygos vein, which comes from the left upper sovracardinale vein (Dudiak et al. in Semin Roentgenol 24(1):47–55, 1989; Radiographics 11(2):233–246, 1991; Webb et al. in Am J Roentgenol 139(1):157–161, 1982). Findings: This case report describes a rare variant of azygos vein system identified in prenatal diagnosis and con- firmed by postnatal ultrasonography. -

Are You Ready for ICD-10-PCS? Expert Tips, Tools, and Guidance to Make the Transition Simple
Are You Ready for ICD-10-PCS? Expert Tips, Tools, and Guidance to Make the Transition Simple By Amy Crenshaw Pritchett February 19, 2014 1 Agenda In this webinar: Expand your understanding of ICD-10-PCS with can’t miss ICD-10-PCS coding conventions & guidelines. Understand the basic differences between ICD-9-CM Volume 3 and ICD-10-PCS. Learn code structure, organization, & characters: Step 1 to coding section “0” ICD-10-PCS? Pinpoint the body system. To build your ICD-10-PCS code, you must identify the root operation. Study 7 options when assigning your PCS code’s 5th character. Master how to determine the device value for your PCS code’s character. Raise your awareness of unique ICD-10-PCS challenges pertaining to documentation and specificity: Prepare physicians now for more detailed transfusion notes under ICD- 10-PCS. Discover why writing “Right Carotid Endarterectomy” won’t be enough. Know where to find ICD-10-PCS tools, techniques, and best practices. 2 Understanding ICD-10-PCS ICD-10-PCS is a major departure from ICD-9-CM procedure coding, requiring you to know which root word applies. Effective October 1, 2014, this procedure coding system will be used to collect data, determine payment, and support the electronic health record for all inpatient procedures performed in the US. 3 Gear Up for ICD-10-PCS This procedure coding system is starkly different from ICD-9-CM procedure coding: Every ICD-10-PCS code has seven characters, each character defining one aspect of the procedure performed. For instance, not correctly identifying your physician’s approach – the fifth character – and not being able to distinguish between similar root operations can throw off your claims accuracy! 4 Converting to ICD-10-PCS Have your inpatient coders and clinical documentation specialists begun preparing for ICD-10-PCS yet? That’s why we’re here today … to ease your transition from ICD-9-CM procedure coding to ICD-10-PCS. -

Blood and Lymph Vascular Systems
BLOOD AND LYMPH VASCULAR SYSTEMS BLOOD TRANSFUSIONS Objectives Functions of vessels Layers in vascular walls Classification of vessels Components of vascular walls Control of blood flow in microvasculature Variation in microvasculature Blood barriers Lymphatic system Introduction Multicellular Organisms Need 3 Mechanisms --------------------------------------------------------------- 1. Distribute oxygen, nutrients, and hormones CARDIOVASCULAR SYSTEM 2. Collect waste 3. Transport waste to excretory organs CARDIOVASCULAR SYSTEM Cardiovascular System Component function Heart - Produce blood pressure (systole) Elastic arteries - Conduct blood and maintain pressure during diastole Muscular arteries - Distribute blood, maintain pressure Arterioles - Peripheral resistance and distribute blood Capillaries - Exchange nutrients and waste Venules - Collect blood from capillaries (Edema) Veins - Transmit blood to large veins Reservoir Larger veins - receive lymph and return blood to Heart, blood reservoir Cardiovascular System Heart produces blood pressure (systole) ARTERIOLES – PERIPHERAL RESISTANCE Vessels are structurally adapted to physical and metabolic requirements. Vessels are structurally adapted to physical and metabolic requirements. Cardiovascular System Elastic arteries- conduct blood and maintain pressure during diastole Cardiovascular System Muscular Arteries - distribute blood, maintain pressure Arterioles - peripheral resistance and distribute blood Capillaries - exchange nutrients and waste Venules - collect blood from capillaries -

PERIPHERAL VASCULATURE Average Vessel Diameter
PERIPHERAL VASCULATURE Average Vessel Diameter A Trio of Technologies. Peripheral Embolization Solutions A Single Solution. Fathom™ Steerable Guidewires Total Hypotube Tip Proximal/ UPN Length (cm) Length (cm) Length (cm) Distal O.D. Hepatic, Gastro-Intestinal and Splenic Vasculature 24 8-10 mm Common Iliac Artery 39 2-4 mm Internal Pudendal Artery M00150 900 0 140 10 10 cm .016 in 25 6-8 mm External Iliac Artery 40 2-4 mm Middle Rectal M00150 901 0 140 20 20 cm .016 in 26 4-6 mm Internal Iliac Artery 41 2-4 mm Obturator Artery M00150 910 0 180 10 10 cm .016 in 27 5-8 mm Renal Vein 42 2-4 mm Inferior Vesical Artery 28 43 M00150 911 0 180 20 20 cm .016 in 15-25 mm Vena Cava 2-4 mm Superficial Epigastric Artery 29 44 M00150 811 0 200 10 10 cm pre-shaped .014 in 6-8 mm Superior Mesenteric Artery 5-8 mm Femoral Artery 30 3-5 mm Inferior Mesenteric Artery 45 2-4 mm External Pudendal Artery M00150 810 0 200 10 10 cm .014 in 31 1-3 mm Intestinal Arteries M00150 814 0 300 10 10 cm .014 in 32 Male 2-4 mm Superior Rectal Artery A M00150 815 0 300 10 10 cm .014 in 33 1-3 mm Testicular Arteries 1-3 mm Middle Sacral Artery B 1-3 mm Testicular Veins 34 2-4 mm Inferior Epigastric Artery Direxion™ Torqueable Microcatheters 35 2-4 mm Iliolumbar Artery Female 36 2-4 mm Lateral Sacral Artery C 1-3 mm Ovarian Arteries Usable 37 D UPN Tip Shape RO Markers 3-5 mm Superior Gluteal Artery 1-3 mm Ovarian Veins Length (cm) 38 2-4 mm Inferior Gluteal Artery E 2-4 mm Uterine Artery M001195200 105 Straight 1 M001195210 130 Straight 1 M001195220 155 Straight 1 Pelvic -
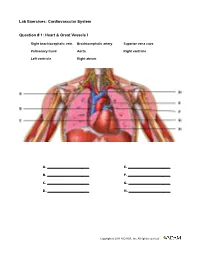
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I Right brachiocephalic vein Brachiocephalic artery Superior vena cava Pulmonary trunk Aorta Right ventricle Left ventricle Right atrium A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 2: Heart & Great Vessels II Left common carotid artery Brachiocephalic trunk Left subclavian artery Left brachiocephalic vein Left pulmonary artery Inferior vena cava Right pulmonary artery Right pulmonary vein A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 3: Heart & Great Vessels (Post) Left pulmonary artery Left subclavian artery Right brachiocephalic vein Left common carotid artery Right pulmonary artery Right pulmonary vein Left pulmonary vein Inferior vena cava A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 4: Arteries of Head & Neck Occipital artery Superficial temporal artery External carotid artery Internal carotid artery Facial artery Vertebral artery Common carotid artery A. E. B. F. C. G. D. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 5: Arteries of Trunk I Axillary artery Brachiocephailic trunk Right common carotid artery Left common carotid artery Left subclavian artery Axillary artery Arch of aorta Thoracic aorta A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 6: Arteries of Trunk II Femoral artery Left common iliac artery Superior mesenteric artery Celiac trunk Inferior mesenteric artery Right renal artery Right testicular artery Left renal artery A. -

Split Azygos Vein: a Case Report
Open Access Case Report DOI: 10.7759/cureus.13362 Split Azygos Vein: A Case Report Stefan Lachkar 1 , Joe Iwanaga 2 , Emma Newton 2 , Aaron S. Dumont 2 , R. Shane Tubbs 2 1. Anatomy, Seattle Chirdren's, Seattle, USA 2. Neurosurgery, Tulane University School of Medicine, New Orleans, USA Corresponding author: Joe Iwanaga, [email protected] Abstract The azygos venous system, which comprises the azygos, hemiazygos, and accessory hemiazygos veins, assists in blood drainage into the superior vena cava (SVC) from the thoracic cage and portions of the posterior mediastinum. Routine dissection of a fresh-frozen cadaveric specimen revealed a split azygos vein. The azygos vein branched off the inferior vena cava (IVC) at the level of the second lumbar vertebra as a single trunk and then split into two tributaries after forming a venous plexus. The right side of this system drained into the SVC and, inferiorly, the collective system drained into the IVC. Variant forms in the venous system, especially the vena cavae, are prone to dilation and tortuosity, leading to an increased likelihood of injury. Knowledge of the anatomical variations of the azygos vein is important for surgeons who use an anterior approach to the spine for diverse procedures. Categories: Anatomy Keywords: inferior vena cava, embryology, azygos vein, variation, anatomy, cadaver Introduction The inferior vena cava (IVC) is the largest vein in the human body. Its principal function is to return venous blood from the abdomen and lower extremities to the right atrium of the heart [1]. Developmental patterning of the IVC consists of three paired embryonic veins: subcardinal, supracardinal, and postcardinal.