Fractures of the Proximal Tibia (Shinbone)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Kansas Journal of Medicine, Volume 12 Issue 3
KANSAS JOURNAL of MEDICINE wheelbarrow to readjust his grip, he lost control of the wheelbarrow, whose weight pulled him causing him to slide approximately five feet off the trail, where he lost balance and landed on his right knee. The patient landed on a dirt surface. He did not recall hearing a popping sound, but immediately felt pain. There was no loss of consciousness Tibial Plateau Fracture Following Low and no other injuries were sustained. Energy Fall in the Rocky Mountains The patient was unable to bear weight following the fall. Joint sta- Alexandra V. Arvanitakis, B.S.1, Kerry C. Mian, B.S.1, bility was unable to be assessed due to pain. Fellow workers tried to Raymond Kreienkamp, Ph.D.2, Charles E. Rhoades, M.D.1 assist the patient to a vehicle, but the pain was too great to flex his 1University of Kansas Medical Center, Department of knee even 10 degrees while supported by crutches. A medical team Orthopedic Surgery, Kansas City, KS was sent to evaluate the patient in the field. At that time, the patient 2St. Louis University School of Medicine had developed a large right knee effusion. Joint laxity was unable Received Sept. 23, 2018; Accepted for publication Feb. 28, 2019; Published online Aug. 21, 2019 to be assessed due to joint swelling and discomfort. However, given the potential stress on the knee while holding a wheelbarrow and INTRODUCTION falling, a ligamentous injury was suspected. The knee was diffusely Tibial plateau fractures are debilitating injuries. They can occur tender. He was evacuated by stretcher to an emergency vehicle and in younger individuals who sustain a high energy trauma or, with transported, with leg braced, to an emergency department at a local increasing age, lesser degrees of trauma and underlying bone pathol- community hospital. -

Skier Tibia (Leg) Fractures
Skier Tibia (Leg) Fractures In years past, the prototypical ski fracture was sustained at the lower part of the outside of the leg in the region of the ankle. However, in the past 10 years, with the advent of the modern ski boots and improvements in binding, the most commonly seen lower leg skier fracture is the tibia (or shinbone) fracture. 10% of these fractures are associated with a collision. Thus, 90 % are associated with an isolated fall or noncontact type of injury, which is generally the result of binding malfunctions and inappropriate release. The most common mechanism leading to a tibia (leg) fracture is a forward fall. Risk factors for sustaining a skier tibia fracture include: beginners or novice skiers, less than 20 years of age, higher outdoor temperatures, and increased snow depth. Non-risk factors include ski lengths, icy conditions, and male versus female sex. The modern ski boot very closely resembles an extremely well padded short leg cast in the treatment of many orthopaedic lower extremity fractures. It of course goes to a much higher level than the former shorter boot top-level varieties. The binding release and designs have been based on the fracture strength of the adult tibia (shin) bone at the top of the modern ski boot. The treatment of most skier leg fractures includes a closed reduction and cast application for variable periods of time, with or without weight bearing allowed. However, severe misalignments of the bones can lead to later bony prominences that may be incompatible with snug, rigid, high fitting ski boots. -

Assessment, Management and Decision Making in the Treatment Of
Pediatric Ankle Fractures Anthony I. Riccio, MD Texas Scottish Rite Hospital for Children Update 07/2016 Pediatric Ankle Fractures The Ankle is the 2nd most Common Site of Physeal Injury in Children 10-25% of all Physeal Injuries Occur About the Ankle Pediatric Ankle Fractures Primary Concerns Are: • Anatomic Restoration of Articular Surface • Restoration of Symmetric Ankle Mortise • Preservation of Physeal Growth • Minimize Iatrogenic Physeal Injury • Avoid Fixation Across Physis in Younger Children Salter Harris Classification Prognosis and Treatment of Pediatric Ankle Fractures is Often Dictated by the Salter Harris Classification of Physeal Fractures Type I and II Fractures: Often Amenable to Closed Tx / Lower Risk of Physeal Arrest Type III and IV: More Likely to Require Operative Tx / Higher Risk of Physeal Arrest Herring JA, ed. Tachdjian’s Pediatric Orthopaedics, 5th Ed. 2014. Elsevier. Philadelphia, PA. ISOLATED DISTAL FIBULA FRACTURES Distal Fibula Fractures • The Physis is Weaker than the Lateral Ankle Ligaments – Children Often Fracture the Distal Fibula but…. – …ligamentous Injuries are Not Uncommon • Mechanism of Injury = Inversion of a Supinated Foot • SH I and II Fractures are Most Common – SH I Fractures: Average Age = 10 Years – SH II Fractures: Average Age = 12 Years Distal Fibula Fractures Lateral Ankle Tenderness SH I Distal Fibula Fracture vs. Lateral Ligamentous Injury (Sprain) Distal Fibula Fractures • Sankar et al (JPO 2008) – 37 Children – All with Open Physes, Lateral Ankle Tenderness + Normal Films – 18%: Periosteal -

Correlation of Parameters on Preoperative CT Images With
Injury, Int. J. Care Injured 48 (2017) 745–750 Contents lists available at ScienceDirect Injury journal homepage: www.elsevier.com/locate/injury Correlation of parameters on preoperative CT images with intra-articular soft-tissue injuries in acute tibial plateau fractures: A review of 132 patients receiving ARIF a,b,c b,c,d b,c,d b,c,d Hao-Che Tang , I-Jung Chen , Yu-Cheng Yeh , Chun-Jui Weng , b,c,d b,c,d b,c,d, Shih-Sheng Chang , Alvin Chao-Yu Chen , Yi-Sheng Chan * a Department of Orthopedic Surgery, Chang Gung Memorial Hospital, Keelung, Taiwan b College of Medicine, Chang Gung University, Taoyuan 333, Taiwan c Bone and Joint Research Center, Chang Gung Memorial Hospital, Linkou, Taiwan d Department of Orthopaedic Surgery, Division of Sports Medicine Section, Chang Gung Memorial Hospital, Linkou, Taiwan A R T I C L E I N F O A B S T R A C T Introduction: Tibial plateau fractures often occur in conjunction with soft-tissue injuries of knees. The Keywords: hypothesis of this study is that parameters of CT imaging can predict intra-articular soft-tissue injuries. Tibial plateau fracture Patients and methods: Patients who underwent arthroscopically assisted reduction and internal fixation CT (ARIF) for acute tibial plateau fractures performed by a single orthopedic surgeon between 2005 and 2015 Arthroscopy were included in this retrospective study. Patients with concomitant ipsilateral femoral fractures, who Meniscus tear ACL avulsion had received revision surgery or who had undergone index surgery more than 30 days from the event were excluded. -

Compartment Syndrome Secondary to Knee Lipohemarthrosis
Open Access Case Report DOI: 10.7759/cureus.16946 Compartment Syndrome Secondary to Knee Lipohemarthrosis Madeleine E. Kim 1 , Thor S. Stead 2 , Latha Ganti 3, 4, 5, 6 1. Emergency Medicine, Baylor School, Chattanooga, USA 2. Epidemiology and Public Health, Alpert Medical School of Brown University, Providence, USA 3. Emergency Medicine, Envision Physician Services, Plantation, USA 4. Emergency Medicine, University of Central Florida College of Medicine, Orlando, USA 5. Emergency Medicine, Ocala Regional Medical Center, Ocala, USA 6. Emergency Medicine, HCA Healthcare Graduate Medical Education Consortium Emergency Medicine Residency Program of Greater Orlando, Orlando, USA Corresponding author: Latha Ganti, [email protected] Abstract When treating patients presenting with knee trauma or intra-articular fracture, clinicians should maintain a high index of suspicion for lipohemarthrosis. Diagnosis of lipohemarthrosis can be accomplished via visualization of a fat-fluid level. Increased fluid and pressure build-up within the joint space may lead to compartment syndrome, which requires emergency compartment fasciotomy. In this paper, we discuss the importance of identifying lipohemarthrosis in patients presenting with intra-articular fracture, as well as the necessity of frequent patient re-evaluations in order to monitor the onset of compartment syndrome. Categories: Emergency Medicine, Orthopedics, Trauma Keywords: lipohemarthrosis, tibial fracture, compartment syndrome, fat-fluid level, fibular fracture, intra-articular fracture, compartment pressure Introduction Knee traumas account for over 500,000 visits to the emergency department (ED) per year in the United States [1-3]. When displaced, intra-articular fractures may result in bone marrow and blood spilling into the surrounding joint capsule [4]. This is defined as lipohemarthrosis. -

Staged Management of Tibial Plateau Fractures
A Review Paper Staged Management of Tibial Plateau Fractures Douglas R. Dirschl, MD, and Daniel Del Gaizo, MD also warrant staged management because of patient, soft tissue, ABSTRACT or biologic factors. A low-energy injury in a patient with com- Careful and thorough assessment of injury severity, promised physiology (uncontrolled diabetes, smoking, morbid with particular attention paid to identifying high-energy obesity, immunocompromised state, etc) may have a greater risk injuries, is critical to achieving optimal outcomes and of complications than a high-energy injury in a healthy patient.2 avoiding complications following tibial plateau fractures. Performing acute open reduction internal fixation will increase Staged management of tibial plateau fractures refers the risk of soft tissue complications (Figure 1).3 to the use of temporizing methods of care (often span- ning external fixation) in high-energy injuries, as well as delaying definitive fracture surgery until such a time History as the risk of soft tissue complications is decreased. A focused, yet complete, history and physical examination This article discusses the principles and techniques of is the first step in evaluating any patient with a fracture. It is staged management, including the use of less invasive crucial to recognize whether or not the patient was in a situ- methods for definitive stabilization. ation where a large amount of energy was imparted to the limb. Motor vehicle/motorcycle collisions, falls from heights ractures of the tibial plateau encompass a wide greater than 10 feet, or being struck by a vehicle while range of severity, from stable nondisplaced frac- walking are some of the more common high-energy mecha- tures with minimal soft tissue injury to highly nisms.2 An appropriate history also includes investigation comminuted unstable fractures with massive soft of patient factors (comorbid conditions) that could impact Ftissue injury that threaten limb viability.1 Careful and the treatment plan or affect the patient’s overall prognosis. -

ACR Appropriateness Criteria® Acute Trauma to the Knee
Revised 2019 American College of Radiology ACR Appropriateness Criteria® Acute Trauma to the Knee Variant 1: Adult or child 5 years of age or older. Fall or acute twisting trauma to the knee. No focal tenderness, no effusion, able to walk. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography knee May Be Appropriate ☢ Bone scan with SPECT or SPECT/CT knee Usually Not Appropriate ☢☢☢ CT knee with IV contrast Usually Not Appropriate ☢ CT knee without and with IV contrast Usually Not Appropriate ☢ CT knee without IV contrast Usually Not Appropriate ☢ MR arthrography knee Usually Not Appropriate O MRA knee without and with IV contrast Usually Not Appropriate O MRA knee without IV contrast Usually Not Appropriate O MRI knee without and with IV contrast Usually Not Appropriate O MRI knee without IV contrast Usually Not Appropriate O US knee Usually Not Appropriate O Variant 2: Adult or child 5 years of age or older. Fall or acute twisting trauma to the knee. One or more of the following: focal tenderness, effusion, inability to bear weight. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography knee Usually Appropriate ☢ Bone scan with SPECT or SPECT/CT knee Usually Not Appropriate ☢☢☢ CT knee with IV contrast Usually Not Appropriate ☢ CT knee without and with IV contrast Usually Not Appropriate ☢ CT knee without IV contrast Usually Not Appropriate ☢ MR arthrography knee Usually Not Appropriate O MRA knee without and with IV contrast Usually Not Appropriate O MRA knee without IV contrast Usually Not Appropriate O MRI knee without and with IV contrast Usually Not Appropriate O MRI knee without IV contrast Usually Not Appropriate O US knee Usually Not Appropriate O ACR Appropriateness Criteria® 1 Acute Trauma to the Knee Variant 3: Adult or skeletally mature child. -
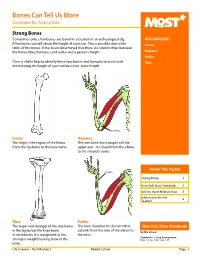
Bones Can Tell Us More Compiled By: Nancy Volk
Bones Can Tell Us More Compiled By: Nancy Volk Strong Bones Sometimes only a few bones are found in a location in an archeological dig. VOCABULARY A few bones can tell about the height of a person. This is possible due to the Femur ratios of the bones. It has been determined that there are relationships between the femur, tibia, humerus, and radius and a person’s height. Humerus Radius Here is a little help to identify these four bones and formulas to assist with Tibia determining the height of a person based on bone length. Humerus Femur: Humerus: The thigh is the region of the femur. The arm bone most people call the From the hip bone to the knee bone. upper arm. It is found from the elbow to the shoulder joints. Inside This Packet Radius Strong Bones 1 New York State Standards 1 Activity: Bone Relationships 2 Information for the Teacher 4 Tibia: Radius: The larger and stronger of the two bones The bone found in the forearm that New York State Standards in the leg below the knee bone. extends from the side of the elbow to Middle School In vertebrates It is recognized as the the wrist. Standard 4: Living Environment strongest weight bearing bone in the Idea 1: 1.2a, 1.2b, 1.2e, 1.2f body. Life Sciences - Post Module 3 Middle School Page 1 Activity: Bone Relationships MATERIALS NEEDED Skeleton Formulas: Tape Measure Bone relationship is represented by the following formulas: Directions and formulas P represents the person’s height. The last letter of each formula stands for the Calculator known length of the bone (femur, tibia, humerus, or radius) through measurement. -

Normative Values for Femoral Length, Tibial Length, Andthe Femorotibial
Article Normative Values for Femoral Length, Tibial Length, and the Femorotibial Ratio in Adults Using Standing Full-Length Radiography Stuart A Aitken MaineGeneral Medical Center, 35 Medical Center Parkway, Augusta, ME 04330, USA; [email protected] Abstract: Knowledge of the normal length and skeletal proportions of the lower limb is required as part of the evaluation of limb length discrepancy. When measuring limb length, modern standing full-length digital radiographs confer a level of clinical accuracy interchangeable with that of CT imaging. This study reports a set of normative values for lower limb length using the standing full-length radiographs of 753 patients (61% male). Lower limb length, femoral length, tibial length, and the femorotibial ratio were measured in 1077 limbs. The reliability of the measurement method was tested using the intra-class correlation (ICC) of agreement between three observers. The mean length of 1077 lower limbs was 89.0 cm (range 70.2 to 103.9 cm). Mean femoral length was 50.0 cm (39.3 to 58.4 cm) and tibial length was 39.0 cm (30.8 to 46.5 cm). The median side-to-side difference was 0.4 cm (0.2 to 0.7, max 1.8 cm) between 324 paired limbs. The mean ratio of femoral length to tibial length for the study population was 1.28:1 (range 1.16 to 1.39). A moderately strong inverse linear relationship (r = −0.35, p < 0.001, Pearson’s) was identified between tibial length and the Citation: Aitken, S.A. Normative corresponding femorotibial ratio. -

Tibial De-Rotational Osteotomies for Tibial Torsion
Tibial De-Rotational Osteotomies for Tibial Torsion Why does my child need tibial torsion surgery? What happens during the surgery? A lot of young children walk with their toes pointing in or First, the surgeon cracks the tibia and the smaller fibula bone out instead of straight ahead. The most common reason is next to it, usually just above the ankle. Surgically cracking a tibial torsion, a twist in the tibia bone of the lower leg. This bone is also known as an osteotomy. It is similar to breaking twist brings the knee and ankle out of alignment. The feet a bone, except that it is done on purpose. The surgeon respond by turning in (internal tibia torsion) or out (external weakens the tibia bone first by drilling holes through a small tibia torsion). Most of the time, tibial torsion gets better as a surgical opening. The next step is to rotate, or turn, the bone child exercises the leg muscles by walking and running. into correct alignment. The surgeon then places a pin in the bone just below the knee. The pin will be removed once the But when a child has spasticity, a condition in which muscle bone heals. In the meantime, your child will wear a cast that tone is very strong, tibial torsion can get worse instead starts at the pin and covers the leg and foot. The cast keeps of better as the child grows. Surgery helps children with the leg from moving while new bone grows. spasticity who can stand, but cannot walk or run normally because of tibial torsion. -

NCB® Proximal Tibia System Surgical Technique
NCB® Proximal Tibia System Surgical Technique NCB® Proximal Tibia System– Surgical Technique 3 Surgical Technique Table of Contents NCB Locking Plate Introduction 4 System for Proximal Tibia Plate Design 5 Screw Selection 5 Cable Fixation Options 6 MIS Radiolucent Targeting Device 7 System Features 7 Indications/Contraindications 8 Fracture Classification 8 Sample Cases 9 Preoperative Planning and Patient Positioning 11 Open Technique 12 Incision 12 Fracture Reduction 12 Optional: Bone Spacers 12 Insertion of NCB PT Plate 13 Insertion of NCB Screws 13 MIS Technique* 18 Plate Hole Numbering System 18 Incision and Fracture Reduction 18 Targeting Device Assembly 19 Insertion and Preliminary Fixation of NCB PT Plate 19 Insertion of NCB Screws in the Proximal Area 21 Insertion of NCB Screws in the Shaft 22 Implant Removal 24 Ordering Information 25 Implants 25 Graphic Case 28 Standard Instruments 29 MIS Instruments 30 Cannulated Option (Screws and Instruments) 32 * MIS Minimally Invasive Solutions™ Technique by Zimmer Planning Aid 33 4 NCB® Proximal Tibia System – Surgical Technique Introduction The NCB PT (Non-Contact Bridging for the Proximal Tibia) is an optimal plate solution for the treatment of complex fractures of the proximal tibia. The system allows for polyaxial screw placement (30°) with subsequent screw locking. Before locking, the screws can act as lag screws and be used for fracture reduction; a benefit which is not offered with standard locking systems. Implants are available with 2 or 3 proximal holes, left and right. Plate length In the locked mode, NCB PT Plate late varies from 5 to 9 shaft acts as an internal fixator without holes for the 2-proximal hole contact between the plate and the plate and between 3 and 13 shaft holes for the 3-proxi- bone surface reducing the risk of mal hole plate. -

Chapter 10 the Knee Joint
The Knee Joint • Knee joint – largest joint in body Chapter 10 – very complex The Knee Joint – primarily a hinge joint Manual of Structural Kinesiology Modified for Prentice WE: Arnheim’s principles of athletic training , ed 12, New R.T. Floyd, EdD, ATC, CSCS York, 2006, McGraw-Hill; from Saladin, KS: Anatomy &physiology: the unity of forms and function , ed 2, New York, 2001, McGraw- Hill. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-1 © 2007 McGraw-Hill Higher Education. All rights reserved. 10-2 Bones Bones • Enlarged femoral condyles articulate on • Fibula - lateral enlarged tibial condyles – serves as the attachment for • Medial & lateral tibial condyles (medial & knee joint lateral tibial plateaus) - receptacles for structures femoral condyles – does not articulate • Tibia – medial with femur or patella – bears most of weight – not part of knee joint Modified from Anthony CP, Kolthoff NJ: Textbook of anatomy and physiology , ed 9, St. Louis, 1975, Mosby. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-3 © 2007 McGraw-Hill Higher Education. All rights reserved. 10-4 Bones Bones • Patella • Key bony landmarks – sesamoid (floating) bone – Superior & inferior patellar poles – imbedded in quadriceps – Tibial tuberosity & patellar tendon – Gerdy’s tubercle – serves similar to a pulley – Medial & lateral femoral in improving angle of condyles pull, resulting in greater – Upper anterior medial tibial mechanical advantage in surface – Head of fibula knee extension Modified from Anthony CP, Kolthoff NJ: Textbook of anatomy and physiology , ed 9, St. Louis, 1975, Mosby. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-5 © 2007 McGraw-Hill Higher Education. All rights reserved.