Postoperative Hypoparathyroidism in Thyroid Surgery
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Axis Scientific Human Circulatory System 1/2 Life Size A-105864
Axis Scientific Human Circulatory System 1/2 Life Size A-105864 05. Superior Vena Cava 13. Ascending Aorta 21. Hepatic Vein 28. Celiac Trunk II. Lung 09. Pulmonary Trunk 19. Common III. Spleen Hepatic Artery 10. Pulmonary 15. Pulmonary Artery 17. Splenic Artery (Semilunar) Valve 20. Portal Vein 03. Left Atrium 18. Splenic Vein 01. Right Atrium 16. Pulmonary Vein 26. Superior 24. Superior 02. Right Ventricle Mesenteric Vein Mesenteric Artery 11. Supraventricular Crest 07. Interatrial Septum 22. Renal Artery 27. Inferior 14. Aortic (Semilunar) Valve Mesenteric Vein 08. Tricuspid (Right 23. Renal Vein 12. Mitral (Left Atrioventricular) Valve VI. Large Intestine Atrioventricular) Valve 29. Testicular / 30. Common Iliac Artery Ovarian Artery 32. Internal Iliac Artery 25. Inferior 31. External Iliac Artery Mesenteric Artery 33. Median Sacral Artery 41. Posterior Auricular Artery 57. Deep Palmar Arch 40. Occipital Artery 43. Superficial Temporal Artery 58. Dorsal Venous Arch 36. External Carotid Artery 42. Maxillary Artery 56. Superficial Palmar Arch 35. Internal Carotid Artery 44. Internal Jugular Vein 39. Facial Artery 45. External Jugular Vein 38. Lingual Artery and Vein 63. Deep Femoral Artery 34. Common Carotid Artery 37. Superior Thyroid Artery 62. Femoral Artery 48. Thyrocervical Trunk 49. Inferior Thyroid Artery 47. Subclavian Artery 69. Great Saphenous Vein 46. Subclavian Vein I. Heart 51. Thoracoacromial II. Lung Artery 64. Popliteal Artery 50. Axillary Artery 03. Left Atrium 01. Right Atrium 04. Left Ventricle 02. Right Ventricle 65. Posterior Tibial Artery 52. Brachial Artery 66. Anterior Tibial Artery 53. Deep Brachial VII. Descending Artery Aorta 70. Small Saphenous Vein IV. Liver 59. -

Bilateral Variations in the Divisions of Common Carotid Artery – a Case Report
eISSN 1308-4038 International Journal of Anatomical Variations (2012) 5: 116–119 Case Report Bilateral variations in the divisions of common carotid artery – a case report Published online December 20th, 2012 © http://www.ijav.org Bheemshetty S. PATIL Abstract Shankarappa D. DESAI During routine dissection, we found bilateral variation in the division of common carotid artery in a 48-year-old male cadaver. The right carotid, originated from the brachiocephalic trunk Ishwar B. BAGOJI behind the right sternoclavicular joint. The left carotid, originated directly from the aortic arch. Gavishiddappa A. HADIMANI Division of common carotid artery occured at higher level; i.e., above the level of superior lamina of thyroid cartilage. On the right side 4.2 cm and on left side 3.5 cm above the superior lamina of thyroid cartilage and just behind the angle of mandible. The arteries did not have any branches; Department of Anatomy, Shri B. M. Patil Medical College, except on the right side the superior thyroidal artery arose from the 2.5 cm below the bifurcation. Blde University, Bijapur, Karnataka, INDIA. Knowledge of origin and bifurcation of common carotid artery is very important to the ENT surgeons, general surgeons, endocrinologist and vascular surgeons. Bheemshetty S. Patil © Int J Anat Var (IJAV). 2012; 5: 116–119. Lecturer Department of Anatomy Shri B. M. Patil Medical College Blde University Bijapur-586103 Karnataka, INDIA. +91 8352-262770/ext. 2211 [email protected] Received October 10th, 2011; accepted August 26th, 2012 Key words [common carotid artery] [thyroid cartilage] [angle of mandible] [bifurcation of common carotid artery] Introduction gives off no branches in the neck, whereas the external does The right common carotid artery arises from the [2]. -

An Unusual Origin and Course of the Thyroidea Ima Artery, with Absence of Inferior Thyroid Artery Bilaterally
Surgical and Radiologic Anatomy (2019) 41:235–237 https://doi.org/10.1007/s00276-018-2122-1 ANATOMIC VARIATIONS An unusual origin and course of the thyroidea ima artery, with absence of inferior thyroid artery bilaterally Doris George Yohannan1 · Rajeev Rajan1 · Akhil Bhuvanendran Chandran1 · Renuka Krishnapillai1 Received: 31 May 2018 / Accepted: 21 October 2018 / Published online: 25 October 2018 © Springer-Verlag France SAS, part of Springer Nature 2018 Abstract We report an unusual origin and course of the thyroidea ima artery in a male cadaver. The ima artery originated from the right subclavian artery very close to origin of the right vertebral artery. The artery coursed anteriorly between the common carotid artery medially and internal jugular vein laterally. It then coursed obliquely, from below upwards, from lateral to medial superficial to common carotid artery, to reach the inferior pole of the right lobe of thyroid and branched repeatedly to supply the anteroinferior and posteroinferior aspects of both the thyroid lobes and isthmus. The superior thyroid arteries were normal. Both the inferior thyroid arteries were absent. The unusual feature of this thyroidea ima artery is its origin from the subclavian artery close to vertebral artery origin, the location being remarkably far-off from the usual near midline position, and the oblique and relatively superficial course. This report is a caveat to neck surgeons to consider such a superficially running vessel to be a thyroidea ima artery. Keywords Thyroid vascular anatomy · Thyroidea ima artery · Artery of Neubauer · Blood supply of thyroid · Variations Introduction (1.1%), transverse scapular (1.1%), or pericardiophrenic or thyrocervical trunk [8, 10]. -

13 Bhatia.P65
CORE Metadata, citation and similar papers at core.ac.uk Provided by Via Medica Journals Folia Morphol. Vol. 64, No. 3, pp. 217–224 Copyright © 2005 Via Medica O R I G I N A L A R T I C L E ISSN 0015–5659 www.fm.viamedica.pl Anatomical variations in the branches of the human aortic arch: a recent study of a South Australian population Kartik Bhatia, Mounir N. Ghabriel, Maciej Henneberg The Department of Anatomical Sciences, University of Adelaide, South Australia [Received 31 May 2005; Accepted 4 July 2005] Variations of the branches of the aortic arch are likely to occur as a result of the altered development of certain branchial arch arteries during the embryonic period of gestation. In the present investigation the pattern of branches of the aortic arch was studied in 81 cadavers from a recent South Australian popula- tion of European descent, who have migrated to (n = 38) or were born and lived in (n = 43) South Australia during the twentieth century. Two principal variations were noted in the present study. Firstly, in 6 cadavers, the left verte- bral artery originated directly from the arch of the aorta, between the left com- mon carotid and the left subclavian arteries. The 6 subjects were among the subgroup born in South Australia, giving an incidence of 13.95%, which is much higher than in previous reports. The overall incidence of 7.41%, when related to the whole group, is also higher than incidences reported in other populations. The presence of this variation suggests that in some individuals part of the aortic arch is formed from the left 7th inter-segmental artery. -

Original Article Relationship Between Inferior Thyroid Artery and Recurrent Laryngeal Nerve
Bangladesh J Otorhinolaryngol 2016; 22(2): 60-65 Original Article Relationship between Inferior Thyroid Artery and Recurrent Laryngeal Nerve - A Study of 200 Cases Muhammad Ali Azad1, AKM Asaduzzaman2, Mohammad Delwar Hossain2, Faysal Bin Mohsin3, Abdullahis Safi3 Abstract Introduction: Thyroid surgery is a common modality of treatment for both benign and malignant thyroid disorders.Relationship between inferior thyroid artery (ITA) and recurrent laryngeal nerve (RLN) is crucial in preservation of recurrent laryngeal nerve. Thorough anatomical knowledge and meticulous surgery will ensure the integrity of recurrent laryngeal nerve. Objective: The purpose of this study is to observe the anatomical position of recurrent laryngeal nerve in relation to inferior thyroid artery which will eventually lead to identification of recurrent laryngeal nerve peroperatively. Methods: A cross sectional retrospective study was conducted during the time period of 1st January 2013 to 31st December 2015 in Combined Military Hospital, Dhaka among 200 patients who had undergone thyroidectomy. Results: In this series on the right side 71.8% cases RLN was dorsal to ITA, 21.7% cases it was ventral and in 6.5% cases RLN runs in between the branches of ITA. In case of left side 74.5% cases RLN was dorsal to ITA, 22.5% cases it was ventral and in 3% cases RLN runs in between the branches of ITA. Conclusion: Usually RLN runs dorsal to ITA. In left side it is deeper and in case of right side it is more superficial. RLN may pass through the branches of ITA, but it is not very common. Key words: Recurrent laryngeal nerve(RLN), Inferior thyroid artery (ITA). -

Anatomy and Physiology Model Guide Book
Anatomy & Physiology Model Guide Book Last Updated: August 8, 2013 ii Table of Contents Tissues ........................................................................................................................................................... 7 The Bone (Somso QS 61) ........................................................................................................................... 7 Section of Skin (Somso KS 3 & KS4) .......................................................................................................... 8 Model of the Lymphatic System in the Human Body ............................................................................. 11 Bone Structure ........................................................................................................................................ 12 Skeletal System ........................................................................................................................................... 13 The Skull .................................................................................................................................................. 13 Artificial Exploded Human Skull (Somso QS 9)........................................................................................ 14 Skull ......................................................................................................................................................... 15 Auditory Ossicles .................................................................................................................................... -

Direct Origin of the Artery of the Cervical Enlargement from the Left Subclavian Artery
Direct Origin of the Artery of the Cervical Enlargement from the Left Subclavian Artery Donald L. Miller Summary: An anatomic variation is described in which the trunk and internal mammary artery were catheterized and principal radiculomedullary artery to the cervical spinal cord, imaged in routine fashion. On the left, the internal mam the artery of the cervical enlargement, arises directly from the mary artery was examined and was unremarkable. left subclavian artery. This anomaly is important clinically The catheter was then introduced into a vessel believed because it may be necessary to catheterize this vessel selec to be the left inferior thyroid artery. On fluoroscopy, injec tively during spinal arteriography, and also because uninten tion of contrast material into this vessel showed that it had tional injection of this vessel can be associated with complica a superior and medial course, similar to the ascending tions. portion of the characteristic loop of the inferior thyroid artery. Index terms: Arteries, abnormalities and anomalies; Arteries, Digital subtraction arteriography (DSA) of this vessel anatomy; Arteries, spinal was performed with a gentle hand injection of contrast material. DSA images were monitored during the injection, The principal arterial supply to the anterior and it was immediately obvious that the anterior spinal spinal artery in the cervical spinal cord is from artery was opacified (Fig. 1). The catheter was pulled down anterior spinal branches of the vertebral arteries and out of the vessel approximately 1.5 seconds after the and from radiculomedullary branches of the ver beginning of the injection. The patient had no neurologic tebral artery and costocervical trunk (1-5). -

Case Report: Absence of Thyrocervical Trunk
May 2015, Volume 12, Number 2 Case Report: Absence of Thyrocervical Trunk Hassan Hassani Bafrani 1, Homayun Naderian 2, Mohammad Ali Atlasi 2, Abolfazl Azami-Tameh 2* 1. Gametogenesis Research Center, Kashan University of Medical Sciences, Kashan, Iran. 2. Anatomical Sciences Research Center, Kashan University of Medical Sciences, Kashan, Iran. Has been an Assistant Professor in the Department of Anatomy at Kashan University of Medical Sciences since 2011. His postdoctoral research was conducted in the field of neurodegeneration at Neuroanatomy Institute of RWTH Aachen Uni- versity in Germany. His special interest is the study glutamate receptors and transporters in neural survival. Article info: A B S T R A C T Received: 10 Dec. 2014 Accepted: 18 Mar. 2015 The thyrocervical trunk most commonly arises from the upper portion of the first segment of the subclavian artery, close to the medial edge of the scalenus anterior muscle and after short distance is divided to the inferior thyroid, transverse cervical, and suprascapular artery. This study reports important variations in branches of the thyrocervical trunk in Key Words: a singular female cadaver. On the right side, no thyrocervical trunk was found. The two branches which normally originate from the thyrocervical trunk had a different origin. The Subclavian artery, superficial cervical, suprascapular and internal thoracic arteries arose from the common Thyrocervical trunk, Variation trunk artery. An awareness of this rare variation is important because this area is used for complex, Neck posterior diagnostic and surgical procedures. triangle 1. Introduction In some cases, the superficial cervical artery is called the superficial branch of the transverse cervical artery einvestigation of the configuration of the because its course is superficial to the levator-rhomboid human thyrocervical trunk revealed, that muscle group. -

Study of Inferior Thyroid Artery and Its Relation to the Sympathetic Chain in Full Term Fetuses
DOI: 10.7860/IJARS/2016/20038:2168 Original Article Study of Inferior Thyroid Artery and its Relation to the Sympathetic Anatomy Section Chain in Full Term Fetuses KAFEEL HUSSAIN A, SWAYAM JOTHI S, RAJAMADHAVA R, NARAYANA RAO B.T ABSTRACT (cross sectional) study was conducted over a period Introduction: Familial dysautonomia and Sudden Infant of 3 years from 2013 to 2015. All the fetuses included in Death Syndrome (SIDS) are amongst the most frequently this study were over 36 weeks. Fetuses with neural tube encountered dysautonomias were sympathetic cardiac defects were excluded from this study. The fetuses were dysfunction is indicated by prolonged corrected QT embalmed by injecting 10% formalin into the serous interval. The therapy for long QT includes left cervical cavities of the abdomen, cranial cavities through the orbit sympathectomy and administration of beta adrenergic and into the muscles and limbs. receptor antagonists. Also, cervical and cervicothoracic Result: Of the 54 fetuses studied, the inferior thyroid sympathectomies are emerging as choices of treatment artery had a course behind the sympathetic chain on both for epilepsies, Raynauds syndrome and vascular disorders the sides in 24 (44%) and anterior to it on both sides in 10 of the upper extremities. There have been few studies (18.5 %) fetuses. The inferior thyroid artery was anterior in fetuses, inspite of the various structural anomalies to it on the right and posterior to it on the left in 5 (9.25%) encountered in the vicinity of the thyroid gland and this cases and anterior to it on the left and posterior to it on the warrants the need of a fetal study. -
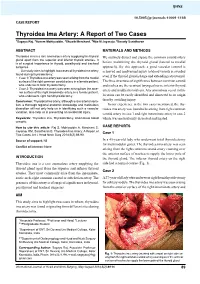
Thyroidea Ima Artery: a Report of Two Cases 1Sagaya Raj, 2Azeem Mohiyuddin, 3Shuaib Merchant, 4Rijo M Jayaraju, 5Beauty Sasidharan
IJHNS Thyroidea10.5005/jp-journals-10001-1188 Ima Artery: A report of Two Cases CASE REPORT Thyroidea Ima Artery: A Report of Two Cases 1Sagaya Raj, 2Azeem Mohiyuddin, 3Shuaib Merchant, 4Rijo M Jayaraju, 5Beauty Sasidharan ABSTRACT MATERIALS AND METHODS Thyroidea ima is a rare anomalous artery supplying the thyroid We routinely dissect and expose the common carotid artery gland apart from the superior and inferior thyroid arteries. It is of surgical importance in thyroid, parathyroid and tracheal before mobilizing the thyroid gland (lateral to medial surgeries. approach). By this approach, a good vascular control is Our study aims to highlight two cases of thyroidea ima artery achieved and inadvertent injury to blood vessels is avoided found during thyroidectomy: even if the thyroid gland is large and extending retrosternal. • Case 1: Thyroidea ima artery was seen arising from the medial surface of the right common carotid artery in a female patient, The three structures of significance between common carotid who underwent total thyroidectomy. and trachea are the recurrent laryngeal nerve, inferior thyroid • Case 2: Thyroidea ima artery was seen arising from the ante- artery and middle thyroid vein. Any anomalous vessel in this rior surface of the right innominate artery, in a female patient, who underwent right hemithyroidectomy. location can be easily identified and dissected to its origin thereby avoiding injury. Conclusion: Thyroidea ima artery, although a rare arterial varia- tion, a thorough regional anatomic knowledge and meticulous In our experience in the two cases mentioned, the thy- dissection will not only help us in identifying such a vascular roidea ima artery was found to be arising from right common variation, also help us in preventing an accidental injury. -

Conventional and Variant Origin of the Transverse Cervical Artery in a Select Kenyan Population
https://dx.doi.org/10.4314/aja.v9i1.11 ORIGINAL COMMUNICATION Anatomy Journal of Africa. 2020. Vol 9 (1): 1727 - 1731 CONVENTIONAL AND VARIANT ORIGIN OF THE TRANSVERSE CERVICAL ARTERY IN A SELECT KENYAN POPULATION Jeremiah Munguti, Fiona Nyaanga, Vincent Kipkorir, Shane Bhupendra, Onyango Marita, Gagandeep Kaur, Thomas Amuti Correspondence to Thomas Amuti, Department of Human Anatomy University of Nairobi Kenya. Email: [email protected] ABSTRACT Data from previous studies have highlighted on the use of transverse cervical artery (TCA) flaps as posterior neck musculocutaneous flaps in reconstructive surgeries. General preference of flap selection relies heavily on the neurovascular supply of the flap in question and even though known, the transverse cervical artery has been shown to vary among populations, therefore affecting its use as a potential flap. Additionally, variant points of origin of the trans-cervical artery have been shown to predispose to brachial plexus compression. Our data on the same, however, remains partly elucidated and therefore a study aimed at describing the conventional and variant origin of the TCA in a Kenyan population would aid in deciding on its use as musculocutaneous flaps and determining the possible prevalence of brachial plexus compression because of its variant origin. The origin of the transverse cervical artery was studied bilaterally in 26 adult Kenyan cadavers in the Department of Human Anatomy, University of Nairobi. As regards their origin, the different types were photographed and grouped into five: Types I to V relative to its origin. The data collected was then analysed using SPSS version 21 and findings presented as percentages. The findings were presented in a bar graph and pie chart. -

Four Collateral Circulation Pathways Were Observed After Common Carotid Artery Occlusion
Four collateral circulation pathways were observed after common carotid artery occlusion Jianan Wang General Hospital of the PLA Rocket Force Chengrong Zheng General Hospital of the PLA Rocket Force Bei Hou General Hospital of the PLA Rocket Force Aihua Huang General Hospital of the PLA Rocket Force Xiongwei Zhang ( [email protected] ) General Hospital of the PLA Rocket Force https://orcid.org/0000-0001-9610-4987 Bin Du General Hospital of the PLA Rocket Force Research article Keywords: common carotid artery occlusion, collateral circulation, internal carotid artery steal Posted Date: September 18th, 2019 DOI: https://doi.org/10.21203/rs.2.10494/v2 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Version of Record: A version of this preprint was published on August 20th, 2019. See the published version at https://doi.org/10.1186/s12883-019-1425-0. Page 1/13 Abstract Background: Common carotid artery (CCA) occlusion (CCAO) is a rare condition. Owing to collateral circulation, ipsilateral internal carotid artery (ICA) and external carotid artery (ECA) are often patent. Methods: This study included 16 patients with unilateral CCAO and patent ipsilateral ICA and ECA. The pathways which supplied ICA were investigated by digital subtraction angiography (DSA), transcranial Doppler (TCD), magnetic resonance angiography (MRA) and computed tomography angiography (CTA). Results: In all 16 patients, TCD found antegrade blood ow in ipsilateral ICA in all 16 patients, which was supplied