Tympanic Membrane Perforation a Hole in the Eardrum (Tympanic
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Perforated Eardrum
Vinod K. Anand, MD, FACS Nose and Sinus Clinic Perforated Eardrum A perforated eardrum is a hole or rupture m the eardrum, a thin membrane which separated the ear canal and the middle ear. The medical term for eardrum is tympanic membrane. The middle ear is connected to the nose by the eustachian tube. A perforated eardrum is often accompanied by decreased hearing and occasional discharge. Paih is usually not persistent. Causes of Eardrum Perforation The causes of perforated eardrum are usually from trauma or infection. A perforated eardrum can occur: if the ear is struck squarely with an open hand with a skull fracture after a sudden explosion if an object (such as a bobby pin, Q-tip, or stick) is pushed too far into the ear canal. as a result of hot slag (from welding) or acid entering the ear canal Middle ear infections may cause pain, hearing loss and spontaneous rupture (tear) of the eardrum resulting in a perforation. In this circumstance, there may be infected or bloody drainage from the ear. In medical terms, this is called otitis media with perforation. On rare occasions a small hole may remain in the eardrum after a previously placed P.E. tube (pressure equalizing) either falls out or is removed by the physician. Most eardrum perforations heal spontaneously within weeks after rupture, although some may take up to several months. During the healing process the ear must be protected from water and trauma. Those eardrum perforations which do not heal on their own may require surgery. Effects on Hearing from Perforated Eardrum Usually, the larger the perforation, the greater the loss of hearing. -

Otitis Media: Causes and Treatment
Otitis media: causes and treatment This leaflet is for patients with otitis media (infection of the middle ear). If you do not understand anything or have any other concerns, please speak to a member of staff. What is otitis media? It is inflammation and infection of the middle ear. This is the eardrum and the small space behind the eardrum. What causes otitis media? Inflammation and blockage of the Eustachian tube following chest infection, colds, flu and throat infection which can cause a build-up of mucus in the middle ear. What are the symptoms? • Earache. • Dulled hearing may develop for a few days. • Fever (high temperature). • Sometimes the eardrum perforates (bursts). This lets out infected mucus, and the ear becomes runny for a few days. As the pain is due to a tense eardrum, if the eardrum bursts, the pain often settles. A perforated eardrum usually heals quickly after the infection clears. It is important that during the next 6 weeks that the ear canal is kept dry during the healing process. Once the infection (and perforation) have cleared, your hearing should return to normal. What is the treatment for otitis media? Most bouts of ear infection will clear on their own within three days. The immune system can usually clear bacteria or viruses causing ear infections. • Painkillers such as Paracetamol or Ibuprofen will ease the pain and will also lower a raised temperature. It is important that you take painkillers as prescribed until the pain eases. • Antibiotics are prescribed if the infection is severe, or is getting worse after 2-3 days. -

Eardrum Regeneration: Membrane Repair
OUTLINE Watch an animation at: Infographic: go.nature.com/2smjfq8 Pages S6–S7 EARDRUM REGENERATION: MEMBRANE REPAIR Can tissue engineering provide a cheap and convenient alternative to surgery for eardrum repair? DIANA GRADINARU he eardrum, or tympanic membrane, forms the interface between the outside world and the delicate bony structures Tof the middle ear — the ossicles — that conduct sound vibrations to the inner ear. At just a fraction of a millimetre thick and held under tension, the membrane is perfectly adapted to transmit even the faintest of vibrations. But the qualities that make the eardrum such a good conductor of sound come at a price: fra- gility. Burst eardrums are a major cause of conductive hearing loss — when sounds can’t pass from the outer to the inner ear. Most burst eardrums are caused by infections or trauma. The vast majority heal on their own in about ten days, but for a small proportion of people the perforation fails to heal natu- rally. These chronic ruptures cause conductive hearing loss and group (S. Kanemaru et al. Otol. Neurotol. 32, 1218–1223; 2011). increase the risk of middle ear infections, which can have serious In a commentary in the same journal, Robert Jackler, a head complications. and neck surgeon at Stanford University, California, wrote that, Surgical intervention is the only option for people with ear- should the results be replicated, the procedure represents “poten- drums that won’t heal. Tympanoplasty involves collecting graft tially the greatest advance in otology since the invention of the material from the patient to use as a patch over the perforation. -

The Eardrum Moves When the Eyes Move
bioRxiv preprint doi: https://doi.org/10.1101/156570; this version posted June 29, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. The eardrum moves when the eyes move: A multisensory effect on the mechanics of hearing Short title: The eardrum moves when the eyes move K. G. Gruters*, D. L. K. Murphy*, D. W. Smith§, C. A. Shera‡, J. M. Groh*† *Department of Psychology and Neuroscience; Department of Neurobiology; Duke Institute for Brain Sciences, Duke University, Durham, NC 27708 §Program in Behavioral and Cognitive Neuroscience, Department of Psychology, University of Florida, Gainesville, FL 32611 ‡Caruso Department of Otolaryngology; Department of Physics and Astronomy, University of Southern California, Los Angeles, CA 90033 †To whom correspondence should be addressed Section: Biological Sciences: Neuroscience Acknowledgments: We are grateful to Tom Heil, Jessi Cruger, Karen Waterstradt, Christie Holmes, and Stephanie Schlebusch for technical assistance. We thank Marty Woldorff, Jeff Beck, Tobias Overath, Barbara Shinn-Cunningham, Valeria Caruso, Daniel Pages, Shawn Willett, Jeff Mohl for numerous helpful discussions and comments during the course of this project. bioRxiv preprint doi: https://doi.org/10.1101/156570; this version posted June 29, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. ABSTRACT Interactions between sensory pathways such as the visual and auditory systems are known to occur in the brain, but where they first occur is uncertain. Here we show a novel multimodal interaction evident at the eardrum. -

Determinants of Conductive Hearing Loss in Tympanic Membrane Perforation
Clinical and Experimental Otorhinolaryngology Vol. 8, No. 2: 92-96, June 2015 http://dx.doi.org/10.3342/ceo.2015.8.2.92 pISSN 1976-8710 eISSN 2005-0720 Original Article Determinants of Conductive Hearing Loss in Tympanic Membrane Perforation Hanaro Park·Seung No Hong·Hyo Sang Kim·Jae Joon Han·Juyong Chung·Myung-Whan Seo·Seung-Ha Oh Sun-O Chang·Jun Ho Lee Department of Otorhinolaryngology-Head and Neck Surgery, Seoul National University College of Medicine, Seoul, Korea Objectives. Tympanic membrane perforations are common, but there have been few studies of the factors determining the extent of the resulting conductive hearing loss. The aims of this study were to determine whether the size of tympan- ic membrane perforation, pneumatization of middle ear & mastoid cavity, and location of perforation were correlated with air-bone gap (ABG) of patients. Methods. Forty-two patients who underwent tympanoplasty type I or myringoplasty were included and preoperative audi- ometry were analyzed. Digital image processing was applied in computed tomography for the estimation of middle ear & mastoid pneumatization volume and tympanic membrane photograph for the evaluation of perforation size and location. Results. Preoperative mean ABG increased with perforation size (P=0.018), and correlated inversely with the middle ear & mastoid volume (P=0.005). However, perforations in anterior versus posterior locations showed no significant dif- ferences in mean ABG (P=0.924). Conclusion. The degree of conductive hearing loss resulting from a tympanic membrane perforation would be expected with the size of perforation and pneumatization of middle ear and mastoid. Keywords. Tympanic Membrane Perforation; Tympanoplasty INTRODUCTION ear, and corresponding models have been suggested [1-3]. -

Onward Referral of Adults with Hearing Difficulty Directly Referred to Audiology Services
Guidance for Audiologists: Onward Referral of Adults with Hearing Difficulty Directly Referred to Audiology Services Produced by: Service Quality Committee of the British Academy of Audiology Key Authors: Hanna Jeffery Suzanne Jennings Laura Turton Date of publication: November 2016 (minor amendment July 2017) Review date: November 2021 BAA – Service Quality Committee Acknowledgements The Service Quality Committee would like to thank all those who provided their opinions on the draft of this document sent out for consultation, including BAA members, The British Society of Audiology, The British Association of Audiological Physicians, ENT UK and The Royal College of General Practitioners. This document is a British Academy of Audiology document and has not been endorsed by any other organisation. Introduction This document is intended to guide Audiologists in service planning and in making referrals for a medical or other professional opinion. Along with “Guidelines for Primary Care: Direct Referral of Adults with Hearing Difficulty to Audiology Services (2016)1”, this document replaces the earlier guidelines (BAA 20092, TTSA 19893,4) and has been approved by the Board of the British Academy of Audiology. This document comprises a set of criteria which define the circumstances in which an Audiologist in the UK should refer an adult with hearing difficulties for a medical or other professional opinion. If any of these are found, then the patient should be referred to an Ear, Nose and Throat (ENT) department, to their GP or to an Audiologist with an extended scope of practice. The criteria have been written for all adults (age 18+), but local specifications regarding age range for direct referral should be adhered to. -

Anatomy of the Ear ANATOMY & Glossary of Terms
Anatomy of the Ear ANATOMY & Glossary of Terms By Vestibular Disorders Association HEARING & ANATOMY BALANCE The human inner ear contains two divisions: the hearing (auditory) The human ear contains component—the cochlea, and a balance (vestibular) component—the two components: auditory peripheral vestibular system. Peripheral in this context refers to (cochlea) & balance a system that is outside of the central nervous system (brain and (vestibular). brainstem). The peripheral vestibular system sends information to the brain and brainstem. The vestibular system in each ear consists of a complex series of passageways and chambers within the bony skull. Within these ARTICLE passageways are tubes (semicircular canals), and sacs (a utricle and saccule), filled with a fluid called endolymph. Around the outside of the tubes and sacs is a different fluid called perilymph. Both of these fluids are of precise chemical compositions, and they are different. The mechanism that regulates the amount and composition of these fluids is 04 important to the proper functioning of the inner ear. Each of the semicircular canals is located in a different spatial plane. They are located at right angles to each other and to those in the ear on the opposite side of the head. At the base of each canal is a swelling DID THIS ARTICLE (ampulla) and within each ampulla is a sensory receptor (cupula). HELP YOU? MOVEMENT AND BALANCE SUPPORT VEDA @ VESTIBULAR.ORG With head movement in the plane or angle in which a canal is positioned, the endo-lymphatic fluid within that canal, because of inertia, lags behind. When this fluid lags behind, the sensory receptor within the canal is bent. -

NL0313A Hearing Loss – Introduction and Overview Printed with Permission from Better Hearing Institute
NL0313A Hearing Loss – Introduction and Overview Printed with Permission from Better Hearing Institute http://www.betterhearing.org The Better Hearing Institute (BHI) is a not-for-profit corporation that educates the public about the neglected problem of hearing loss and what can be done about it. Founded in 1973, we are working to: Erase the stigma and end the embarrassment that prevents millions of people from seeking help for hearing loss. Show the negative consequences of untreated hearing loss for millions of Americans. Promote treatment and demonstrate that this is a national problem that can be solved. 1. HOW WE HEAR Patricia E. Connelly, PhD, CCC-A, FAAA, New Jersey Medical School, NEWARK, NJ The Hearing System The anatomy of the hearing system can be divided into four components for our convenience in remembering the parts and associating these parts with their function. These divisions are the: 1. outer ear 2. middle ear 3. inner ear 4. central auditory pathways The Outer Ear (1) Several structures comprise the outer ear. The most readily seen is the pinna, also called the auricle. The pinna is made up of a frame of cartilage that is covered with skin. The pinna has obvious folds, elevations, depressions and a prominent bowl - all of which vary somewhat from person to person but a basic pattern in these features is fairly universal among all people. The pinna acts as a funnel to collect and direct sound down the ear canal. It also serves to enhance some sounds through its resonance characteristics. Finally, it helps us to appreciate front-back sound localization. -

Petubes Patient Handout.Pdf
Division of Pediatric Otolaryngology Information on Tympanostomy Tubes Tympanostomy tubes are small plastic or metal tubes that are placed into the tympanic membrane or ear drum. How long will the tube stay in place? Tubes usually fall out of the ear in 6 months- 2 years. If they remain in longer than 2 to 3 years they are sometimes removed. What is involved with Tympanostomy tube placement? This surgery is usually done under general anesthesia. The eardrum is examined using a microscope. A small hole is made in the ear drum called a myringotomy, fluid is removed, and the tube is placed. Tube in the eardrum What medical conditions are treated with tubes? Recurrent middle ear infections or frequent acute otitis media Otitis media with effusion or fluid in middle ear associated with hearing loss Eustachian tube dysfunction causing hearing loss or eardrum structure changes What is the Eustachian tube? This is the canal that links the middle ear with the throat. This tube allows air into the middle ear and drainage of fluid. This tube grows in width and length until children are about 5 years old. Reasons that the Eustachian tube may not work properly: Viral illness, exposure to allergens or tobacco smoke may lead to swelling of the eustachian tube resulting in fluid buildup in the middle ear. Children with cleft palate and craniofacial syndromes like Down’s syndrome may have poor eustachian tube function. How will Tympanostomy tube help my child? They allow air to re-enter middle ear space They reduce the number and severity of infections They improve hearing loss cause by middle ear fluid Why is adenoidectomy sometimes done with the Tympanostomy tubes? Adenoidectomy is the removal of the adenoid tissue behind the nose. -

Perforated Eardrum and Myringoplasty
Perforated eardrum and myringoplasty Disclaimer: The details in this section are for general information only. Always check with your own surgeon. What is a perforated eardrum? A perforated eardrum means there is a hole in the eardrum, which may have been caused by infection or injury. Quire often a hole in the eardrum may heal itself. Sometimes it does not cause any problems. However, it may cause recurrent infections with a discharge from the ear. If you have an infection you should avoid getting water in the ear. If the hole is large then you may experience some hearing loss. A hole in the eardrum can be identified by an ENT specialist using an instrument called an ‘auriscope’. Surgery to repair the perforation An operation to repair the perforation is called a ‘myringoplasty’. The benefits of closing a perforation include prevention of water entering the middle ear, which Source: Ear Nose & Throat Reference No: 6135-1 Issue date: 16/9/19 Review date: 16/9/22 Page 1 of 3 could cause ear infection. Repairing the hole means that you should get fewer ear infections. It may result in improved hearing, but repairing the eardrum alone seldom leads to great improvement in hearing. If the hole in the eardrum has only just occurred, no treatment may be required. You should discuss with your surgeon whether to wait and see, or have surgery now. You may change your mind about the operation at any time and signing a consent form does not mean that you have to have the operation. If you would like to have a second opinion about the treatment, you can ask your specialist. -
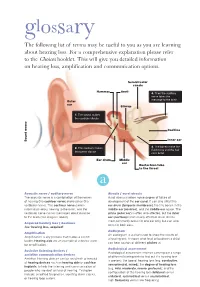
Glossary the Following List of Terms May Be Useful to You As You Are Learning About Hearing Loss
glossary The following list of terms may be useful to you as you are learning about hearing loss. For a comprehensive explanation please refer to the Choices booklet. This will give you detailed information on hearing loss, amplification and communication options. Semicircular canals Hammer Anvil 4. Then the auditory nerve takes the message to the brain. Outer ear Stirrup 1. The sound makes the eardrum vibrate Cochlea Inner ear Sound waves . The bones make the 2. The eardrum makes 3 fluid move and the hair the bones vibrate cells bend. Ear drum Middle ear Eustachian tube to the throat a Acoustic nerve / auditory nerve Atresia / aural atresia The acoustic nerve is a combination of the nerves Aural atresia involves some degree of failure of of hearing (the cochlear nerve) and balance (the development of the ear canal. It can also affect the vestibular nerve). The cochlear nerve carries ear drum (tympanic membrane), the tiny bones in the information about hearing to the brain, and the middle ear (ossicles), and the middle ear space. The vestibular nerve carries messages about balance pinna (outer ear) is often also affected, but the inner to the brain (see diagram above). ear (cochlea) is not usually affected. Aural atresia most commonly occurs in one ear only, but can also Acquired hearing loss / deafness occur in both ears. See ‘hearing loss, acquired’. Audiogram Amplification An audiogram is a chart used to show the results of Amplification is any process that makes a sound a hearing test. It shows what level of loudness a child louder. Hearing aids are an example of a device used can hear sounds of different pitches at. -

Audiometric Findings with Voluntary Tensor Tympani Contraction Brandon Wickens1 , Duncan Floyd2 and Manohar Bance3*
Wickens et al. Journal of Otolaryngology - Head and Neck Surgery (2017) 46:2 DOI 10.1186/s40463-016-0182-y ORIGINALRESEARCHARTICLE Open Access Audiometric findings with voluntary tensor tympani contraction Brandon Wickens1 , Duncan Floyd2 and Manohar Bance3* Abstract Background: Tensor tympani contraction may have a "signature" audiogram. This study demonstrates audiometric findings during voluntary tensor tympani contraction. Methods: Five volunteers possessing the ability to voluntarily contract their tensor tympani muscles were identified and enrolled. Tensor tympani contraction was confirmed with characteristic tympanometry findings. Study subjects underwent conventional audiometry. Air conduction and bone conduction threshold testing was performed with and without voluntary tensor tympani contraction. Main outcome measure: Changes in air conduction and bone conduction thresholds during voluntary tensor tympani contraction. Results: Audiometric results demonstrate a low frequency mixed hearing loss resulting from tensor tympani contraction. Specifically, at 250 Hz, air conduction thresholds increased by 22 dB and bone conduction thresholds increased by 10 dB. Conclusions: Previous research has demonstrated a low frequency conductive hearing loss in the setting of tensor tympanic contraction. This is the first study to demonstrate a low frequency mixed hearing loss associated with tensor tympani contraction. This finding may aid in the diagnosis of disorders resulting from abnormal tensor tympani function. Tensor tympani contraction