Graded Resident Competencies in Anatomical Pathology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
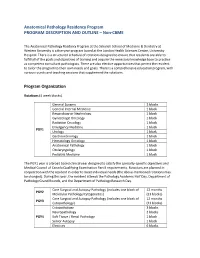
Anatomical Pathology Residency Program PROGRAM DESCRIPTION and OUTLINE – Non-CBME
Anatomical Pathology Residency Program PROGRAM DESCRIPTION AND OUTLINE – Non-CBME The Anatomical Pathology Residency Program at the Schulich School of Medicine & Dentistry at Western University is a five year program based at the London Health Sciences Centre, University Hospital. There is a structured schedule of rotations designed to ensure that residents are able to fulfill all of the goals and objectives of training and acquire the necessary knowledge base to practice as competent consultant pathologists. There are also elective opportunities that permit the resident to tailor the program to their own needs and goals. There is a comprehensive education program, with various rounds and teaching sessions that supplement the rotations. Program Organization Rotations (4 week blocks) General Surgery 2 blocks General Internal Medicine 1 block Respirology or Nephrology 1 block Gynecologic Oncology 1 block Radiation Oncology 1 block Emergency Medicine 1 block PGY1 Urology 1 block Gastroenterology 1 block Hematology Oncology 1 block Anatomical Pathology 1 block Otolaryngology 1 block Pediatric Medicine 1 block The PGY1 year is a broad based clinical year designed to satisfy the specialty-specific objectives and Medical Council of Canada Qualifying Examination Part II requirements. Rotations are planned in conjunction with the resident in order to meet individual needs (the above-mentioned rotations may be changed). During this year, the resident attends the Pathology Academic Half Day, Department of Pathology Grand Rounds, and the Department -

2019-General-Pathology-Faq.Pdf
FREQUENTLY ASKED QUESTIONS – 2019 Program: GENERAL PATHOLOGY Specialty/Field Questions: 1. a) What are some strengths about your specialty? What draws and keeps people in your specialty? • The opportunity to understand the nature of disease in an in-depth way that isn’t achieved in any other specialty. You get to practice scientific diagnostic medicine over a broad range of subjects and you have a fair degree of control over your schedule. You are very much a part of the team taking care of the patient (it just isn’t as obvious!), and this is becoming even more apparent in the era of precision medicine. • Although there is limited direct contact with patients, there is a great deal of contact with a variety of clinicians outside the laboratory as well as with physician, PhD, and technical staff colleagues within the laboratory. We get satisfaction from the interactions we have with others, and knowing that we are helping a clinician take the next step in diagnosing or treating a patient. The stereotypical image of the hermit- like pathologist who stays in their office and never talks to anyone is rapidly disappearing in today’s pathology practice. b) What are some common complaints about your specialty? • There is limited direct clinical contact – you’ll never have an office full of patients who regard you as their doctor and most pathologists have a hospital-based practice which can limit professional autonomy. • You often have to sit/stand at a microscope and/or computer a lot, so sometimes you need to get creative about staying active during the day. -

Anatomical Pathology
Timely and accurate pathology results are Pathology disciplines critical to the functioning of our entire medical system. 70% of all diagnoses are made using a pathology test. All chronic conditions require monitoring via pathology testing. Pathologists play a Pathology informs the clinical decisions of medical practitioners much wider role than just diagnosing cancer, and work across a range across the healthcare spectrum. of different specialities, in addition to anatomical pathology. These include: Given its critical role, the risks of not adequately supporting Pathologists are Indispensable to Quality Patient Care a strong national pathology system are: Chemical pathology, which deals with the entire range of disease, • Incorrect diagnoses; and encompasses detecting changes in a number of substances in • Delayed diagnoses; blood and body fluids (such as electrolytes, enzymes and proteins); • Patients receiving incorrect treatment; Forensic pathology, which seeks to investigate and define the cause • Tumours inadequately or inappropriately treated (e.g. of unexpected death; unnecessary surgery); and Genetics, which looks at chromosomes and DNA from cells to • Possible early patient death. diagnose genetic diseases; These issues may impact upon the physical, emotional and Haematology, which deals with diseases that affect the blood such as financial well-being of individual patients, their families and the anaemia, leukaemia, lymphoma, clotting or bleeding disorders as well community at large. as management of blood transfusions; Immunopathology, which deals with the diagnosis and management As the peak body representing the profession, the RCPA of conditions in which the immune system does not function properly; believes the underlying principles of a world class pathology service are: Microbiology, which deals with diseases caused by infectious agents • A commitment to patient safety and quality such as bacteria, viruses, fungi and parasites; and • A highly trained and sufficiently resourced workforce General pathology, which covers the profession as a whole. -

Quality Assurance Program for Anatomical Pathologists Printed Copies Are Uncontrolled
Quality Assurance Assessment Program for Anatomical Pathologists This provincial best practice document is being developed in response to the Cochrane Report recommending a peer review program for pathology with results reported to the Health Authority Quality Committee, BC’s Agency for Pathology and Laboratory Medicine and the Diagnostic Accreditation Program, when appropriate. The program has been developed with input from the provincial Anatomic Pathology Working Group, along with review of current provincial practices and peer reviewed publications, specifically the Pan- Canadian Quality Assurance Recommendations for Interpretive Pathology. The program is designed to be proactive where quality activities are embedded directly into the clinical practice of anatomic pathologists via the Laboratory Information System (LIS), allowing standardized quality assurance data to be captured, reported, reviewed and discrepancies reported for follow up corrective action through standardized quality improvement processes. Objective: Develop a standardized approach to Quality Assurance (QA) in interpretive pathology for use by all anatomic pathologists. Capture pathologist QA activities, and provide meaningful statistics to individual pathologists, the Laboratory quality committee, health authority medical administration and the Agency to allow year over year comparisons by pathologist, facility, HA and comparisons across the province. To build a provincial anatomic pathology culture based on sustainable high quality diagnostic services to enable the enhancement of patient safety. To ensure the public have confidence in British Columbia’s anatomic pathology service regardless of geographic location or jurisdiction. Goal: For the activities related to all anatomic pathologists caseload be involved in a review, which is measurable and comparable to a standard baseline. Where appropriate, reviews will target surgical pathology, cytology and autopsy services, including all related ancillary testing. -

A Case of Neurofibromatosis 2 Presenting with a Mononeuritis Multiplex
Journal of Neurology, Neurosurgery, and Psychiatry 1992;55:391-393 391 SHORT REPORT J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.55.5.391 on 1 May 1992. Downloaded from A case of neurofibromatosis 2 presenting with a mononeuritis multiplex T J Kilpatrick, R J Hjorth, M F Gonzales Abstract forearm extensors. There was weakness of the A patient with neurofibromatosis 2 had an intrinsic muscles of the right hand and gener- asymmetrical peripheral neuropathy. A alised weakness of the left arm. The legs were nerve biopsy specimen revealed neuro- also wasted with symmetrical distal weakness. fibromatous changes, and the neuropathy The reflexes were depressed on the right but may have been a direct consequence of normal on the left, except for a depressed ankle neurofibromatosis. An apparent clinical jerk. The right plantar was flexor and the left response to immunosuppressive treat- unresponsive. There was a mild impairment of ment and plasma exchange is also repor- all sensory modalities in the hands and legs, ted. extending to the right knee and to the left anterior superior iliac spine. There were no palpable enlargements along the course of any The term neurofibromatosis defines two peripheral nerves. genetically and phenotypically distinct dis- The results of tests for urea, electrolytes and orders.' Neurofibromatosis 1, or von Reck- liver function, full blood examination and linghausen's disease, is an autosomal domi- random blood glucose and serum calcium, nant disorder with the genetic abnormality phosphate, vitamin B12, and folate concentra- localised to chromosome 17. Typical abnor- tions were all normal. There was no para- malities include cafe-au-lait spots, neuro- proteinaemia, antinuclear antibodies were not fibromas, and Lisch nodules in the iris. -

Specialty Training Requirements in Anatomical Pathology
Specialty Training Requirements in Anatomical Pathology 2013 EDITORIAL REVISION 2016 VERSION 2.1 These training requirements apply to those who begin training on or after July 1st, 2013. MINIMUM TRAINING REQUIREMENTS Five (5) years of accredited residency training. This period must include: Basic Clinical Training 1. Thirteen (13) blocks of basic clinical training relevant to Anatomical Pathology. This period must include: 1.1. Two (2) blocks in a surgical specialty 1.2. Two (2) blocks in Internal Medicine, including General Internal Medicine or other subspecialties 1.3. One (1) block in Pediatrics or a pediatric subspecialty 1.4. One (1) block in Obstetrics and Gynecology or a subspecialty thereof 1.5. One (1) block in an oncologic specialty 1.6. Six (6) blocks of further basic clinical training as approved by the program director Core Anatomical Pathology 2. Forty (40) blocks of approved residency training in Anatomical Pathology. These forty (40) blocks must include a minimum of: 2.1. Twenty-five (25) blocks or equivalent longitudinal experience in surgical pathology and adult autopsy pathology 2.2. One (1) block or equivalent longitudinal experience in molecular pathology and cytogenetics 2.3. Two (2) blocks or equivalent longitudinal experience in forensic pathology 2.4. Four (4) blocks or equivalent longitudinal experience in cytopathology, one (1) of which must be completed in final year 2.5. Two (2) blocks or equivalent longitudinal experience in pediatric pathology 2.6. Two (2) blocks or equivalent longitudinal experience in neuropathology © 2013 The Royal College of Physicians and Surgeons of Canada. All rights reserved. This document may be reproduced for educational purposes only, provided that the following phrase is included in all related materials: Copyright © 2013 The Royal College of Physicians and Surgeons of Canada. -

Frequently Asked Questions: Anatomic Pathology and Clinical
Frequently Asked Questions: Anatomic Pathology and Clinical Pathology (FAQs related to Pathology Program Requirements effective July 1, 2020) Review Committee for Pathology ACGME Question Answer Introduction Can residents leave in the middle of their Yes, as the American Board of Pathology allows residents to enter a pathology program to complete a fellowship and then fellowship program (except dermatopathology) after 24 months of residency, the return to finish their pathology residency? Review Committee allows this as well. The expectation is that once the fellowship is completed, residents return to the pathology residency program to complete their [Program Requirement: Int.C.1.] education. Programs do not need to notify the Review Committee or request exceptions for residents to pursue this pathway. In the Accreditation Data System (ADS) these residents should be listed as “In Program but Doing Research/Other Training ”while they are in a fellowship program, and reset to “Active Full time” status once the fellowship is completed and they have returned to the pathology residency program. If a resident wishes to focus only on No. All pathology programs are accredited as APCP-4, with anatomic pathology only anatomic pathology or clinical pathology, (AP-3) and clinical pathology only (CP-3) offered as tracks within the program, not as must the Sponsoring Institution apply for a separately accredited programs. There is no separate application process, as separate program or does the existing programs are free to offer these tracks to residents if they choose. The Educational program need any other approval from the Program section of the Program Requirements clearly denotes tracks so that programs Review Committee? can understand the expectations for residents in any of the tracks. -

Curriculum Vitae
Prepared: November 20, 2019 University of California, San Francisco CURRICULUM VITAE Name: Elham Khanafshar, MD, MS Position: Professor of Clinical Pathology, Step 2 Pathology School of Medicine Address: Box 1785 1600 Divisadero St.,MZ Bldg B, R207 University of California, San Francisco San Francisco, CA 94143 Voice: 415-353-7380 Email: [email protected] EDUCATION 1989 - 1997 Tehran University of Medical M.D. Sciences, Tehran, Iran 1997 - 1999 University of Southern California, M.S. Molecular & Experimental Los Angeles, CA Pathology 1999 - 2002 Cedars-Sinai Medical Center, Los Resident Anatomical & Clinical Angeles, CA Pathology 2002 - 2003 Cedars-Sinai Medical Center, Los Chief Resident Anatomical & Clinical Angeles, CA Pathology 2003 - 2004 University of California, San Fellow Surgical Pathology Diego, CA 2004 - 2005 University of Southern California, Fellow Cytopathology Los Angeles, CA 2007 - 2007 University of Toronto, Toronto, Visiting Endocrine Pathology ON Canada Pathologist 2010 - 2010 University of Wisconsin, Visiting Endocrine Pathology Minnesota, WI Pathologist LICENSES, CERTIFICATION 2001 Medical licensure, California 2003 Anatomical and Clinical Pathology Board Certification 2005 Cytopathology Board Certification 2005 Thin-Prep Certification 1 of 31 Prepared: November 20, 2019 2006 ImmunoCyt Certification 2016 UCSF Bilingual Clinician Certification 2019 American Heart Association Basic Life Support PRINCIPAL POSITIONS HELD 2002 - 2003 Cedars-Sinai Medical Center, Los Angeles, Chief Resident Anatomic and CA Clinical -

BASIC PATHOLOGY DEFINITIONS Pathology the Study of Disease
BASIC PATHOLOGY DEFINITIONS Pathology the study of disease. Pathology is a medical specialty studying disease processes, how they develop and what they are caused by and the application of this knowledge to the diagnosis of disease. Pathos= "disease" Logos= "a treatise/ a study" Anatomical pathology is a medical specialty that is concerned with the diagnosis of disease based on the macroscopic, microscopic, biochemical, immunologic and molecular examination of organs and tissues. Lesions are recognizable morphologic (anatomic) changes in tissues, either grossly or microscopically. Clinical pathology determines diagnosis of disease through the study of body fluids and body waste products. These include blood plasma, urine, cerebrospinal fluid, sputum', saliva, peritoneal fluid, thoracic fluid, and feces. Animal Biopsy Necropsy Necropsy a postmortem examination of a body after death or autopsy. At its core, it is the systematic dissection and examination of an animal carcass to search for abnormal anatomical changes (lesions) in the tissues. NECROPSY Necropsy, necroscopy (Gr.): examination of a body after death Necro= dead body Opsis= a sight, view AUTOPSY Autopsy (Gr.): to see with one's own eyes Auto=self, one's own Opsis= a sight, view OBDUCTION Obduction opening of the dead. It is mostly used for the FORENSIC pathology. DISSECTION Section mostly used for the, a slice of tissue in anatomy. Dissection is the dismembering of the body of a deceased animal or plant to study its anatomical structure. BIOPSY Biopsy an examination of tissue removed from a living body to discover the presence, cause, or extent of a disease. Biopsy (Gr.): view of the living" or "appearance of life. -

Pathology and Laboratory Medicine Service
PG-18-9 – SPACE PLANNING CRITERIA October 1, 2021 240 – Pathology and Laboratory Medicine Service CHAPTER 240: PATHOLOGY AND LABORATORY MEDICINE SERVICE 1 PURPOSE AND SCOPE .................................................................................................. 240-2 2 DEFINITIONS ................................................................................................................ 240-2 3 OPERATING RATIONALE AND BASIS OF CRITERIA .......................................................... 240-5 4 INPUT DATA STATEMENTS (IDS) ................................................................................... 240-7 5 SPACE PLANNING CRITERIA - MEDICAL CENTER LABORATORY ....................................... 240-8 6 SPACE PLANNING CRITERIA - OUTPATIENT CLINIC LABORATORY ................................. 240-27 7 PLANNING AND DESIGN CONSIDERATIONS ................................................................. 240-27 8 FUNCTIONAL RELATIONSHIPS..................................................................................... 240-30 9 FUNCTIONAL DIAGRAM ............................................................................................. 240-31 1 of 31 PG-18-9 – SPACE PLANNING CRITERIA October 1, 2021 240 – Pathology and Laboratory Medicine Service 1 PURPOSE AND SCOPE This document outlines the space planning criteria for Chapter 240: Pathology and Laboratory Medicine Service (PMLS). It applies to all medical facilities at the Department of Veterans Affairs (VA). Department of Veterans Affairs (VA) Medical Center -

Anatomical Pathology - Trainee Handbook
Anatomical Pathology - Trainee Handbook @ TRAINEE HANDBOOK 2021 Anatomical Pathology It is essential to read this Handbook in conjunction with the Trainee Handbook – Administrative Requirements which is relevant to all trainees. This has information about the College’s structure and policies, together with details of requirements for registration, training and examination applications. © January 2021 Royal College of Pathologists of Australasia TABLE OF CONTENTS GLOSSARY ..................................................................................................................................... i Section 1 ......................................................................................................................................... 1 Introduction ..................................................................................................................................... 1 Personal characteristics needed ..................................................................................................... 1 General aims of the training program .............................................................................................. 1 Training requirements ..................................................................................................................... 2 Supervision ..................................................................................................................................... 3 Assessment ................................................................................................................................... -
Objectives of Training in the Specialty of Anatomical Pathology
Objectives of Training in the Specialty of Anatomical Pathology 2010 VERSION 1.0 This document applies to those who begin training on or after July 1st, 2010. (Please see also the “Policies and Procedures.”) DEFINITION Anatomical Pathology is that branch of laboratory medicine concerned with the study of the morphologic aspects of disease. It includes the subdomains of cytopathology, gynecological pathology, dermatopathology, gastrointestinal pathology, cardiovascular pathology, respiratory pathology, musculoskeletal pathology, renal pathology, genito-urinary pathology, endocrine pathology, ophthalmic pathology, head and neck pathology, neuropathology, pediatric pathology, forensic pathology, and certain laboratory methods such as immunohistochemistry, immunofluorescence, in-situ hybridization, flow cytometry, molecular pathology, electron microscopy. GOALS Upon completion of training, a resident is expected to be a competent specialist in Anatomical Pathology capable of assuming a consultant’s role in the specialty. The resident must acquire a working knowledge of the theoretical basis of the specialty, including its foundations in the basic medical sciences and research. Residents must demonstrate the requisite knowledge, skills, and attitudes for effective patient-centered care and service to a diverse population. In all aspects of specialist practice, the graduate must be able to address issues of gender, sexual orientation, age, culture, ethnicity and ethics in a professional manner. ANATOMICAL PATHOLOGY COMPETENCIES At the completion of training, the resident will have acquired the following competencies and will function effectively as a: © 2010 The Royal College of Physicians and Surgeons of Canada. All rights reserved. This document may be reproduced for educational purposes only provided that the following phrase is included in all related materials: Copyright © 2010 The Royal College of Physicians and Surgeons of Canada.