Management of Refractory ARDS
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Oxygen Saturation Index
RESEARCH LETTERS We observed that poor psychosocial care had high Department of Pediatrics, Dr SN Medical College, association with malnutrition, and that the interactions Jodhpur, Rajasthan, India. between SAM children and their parents were less optimal *[email protected] than for the controls. The restriction of movement leading REFERENCES to lesser interaction with the surroundings, curtailed 1. Operational Guidelines on Facility Based Management of independence, volition activity, and the ability to ask for or Children with Severe Acute Malnutrition, Ministry of obtain food could lead to malnutrition [4]. If mother is also Health and Family Welfare,Government of India,2011. illiterate, it further increases the chances of developing Available from: http://www.nihf.org/ nchrc –publictions/ severe acute malnutrition [5]. The limitations of this study operational guidelines. Accessed February 25,2014. were small sample size and a hospital-based setting that 2. Ruel MT, Arimond M. Measuring childcare practices: approaches, indicators, and implications for programs. Intl could not delineate the actual home environment. Food Policy Res Inst. 2003;6:1-81. We feel that it is imperative that the psychosocial care 3. Bradley RH, Munfrom DJ, Whiteside L, Caldwell BM, environment of the child suffering with severe acute Casey PH, Kirby R, et al. A reexamination of the malnutrition be thoroughly probed using a questionnaire association between HOME scores and income. Nurs Res. 1994;43:260-6. such as the one suggested in our study, and psychosocial 4. Engle PL, Bentley M, Pelto G. The role of care in nutrition care and rehabilitation should be brought into focus and programmes: current research and a research agenda. -

Flow Versus Pressure Triggering in Mechanically Ventilated Acute Respiratory Failure Patients Magdy M
198 Original article Flow versus pressure triggering in mechanically ventilated acute respiratory failure patients Magdy M. Khalila, Nevine M. Elfattaha, Mohsen M. El-Shafeyb, Nermine M. Riada, Raed A. Aidb, Alaa M. Ananyc Background The effects of fl ow triggering (FT) compared the PT group (P < 0.001). In patients with obstructive with pressure triggering (PT) on breathing effort have pulmonary disorders, combined pulmonary disorders, and been the focus of several studies, and discrepant results less severe disease (APACHE II <32.5), there was no have been reported; yet, it remains an area of confl ict that signifi cant difference between both PT and FT groups in warrants further studies. these parameters. Objective The aim of this work is to compare fl ow versus Conclusion FT may be considered to be better than PT in ventilating patients with acute respiratory failure. PT in ventilating acute respiratory failure patients with a restrictive pattern and those with higher severity scoring. In Patients and methods One hundred patients with acute obstructive and mixed ventilatory impairment, use of either respiratory failure of pulmonary origin were assigned of them does not make a difference. Egypt J Broncho 2015 randomly to two groups: 50 patients ventilated with PT 9:198–210 and 50 patients ventilated with FT. The primary end points © 2015 Egyptian Journal of Bronchology. were weaning duration, evaluation of patient/machine synchronization, total duration of ventilation and ICU stay as Egyptian Journal of Bronchology 2015 9:198–210 well time under sedation and occurrence of complications. Keywords: mechanical ventilation, respiratory failure, triggering Mortality was considered the secondary end point. -

High-Frequency Ventilator Device Trade Name
SUMMARY OF SAFETY AND EFFECTIVENESS DATA I. General Information Device Generic Name: High-Frequency Ventilator Device Trade Name: SensorMedics Model 3100B High- Frequency Oscillatory Ventilator Sponsor Name and Address: SensorMedics Corporation 22705 Savi Ranch Parkway Yorba Linda, CA 92887-4645 PMA Number: P890057/S14 Date of Panel Recommendation: July 16, 2001 Date of Notice of Approval: September 24, 2001 II. Indications for Use The SensorMedics 3100B is indicated for use in the ventilatory support and treatment of selected patients 35 kilograms and greater with acute respiratory failure. III. Contraindications This Model 3100B has no specific contraindications. IV. Device Description The Model 3100B consists of six subsystems, and is used with an external air/oxygen blender and an external humidifier. The six subsystems are: (1) pneumatic logic and control; (2) patient circuit; (3) oscillator subsystem; (4) airway pressure monitor; (5) electronic control and alarm subsystem; and (6) electrical power supply. During use with a patient in acute respiratory failure, the Model 3100B maintains a positive mean airway pressure, upon which pressure oscillations are superimposed at a rate between approximately 3 and 15 per second. The pressure oscillations achieve ventilation of the patient. Page 1 of 15 Pneumatic Logic and Control The pneumatic logic and control subsystem receives pressurized, blended gas from the external air/oxygen blender. The subsystem includes three controls: 1. A bias flow control sets the continuous rate at which the blended gas flows from the external blender, through the bias flow tube and the patient circuit, and past the tracheal tube connection port. The bias flow can be set as high as 60 L/min. -

High-Frequency Oscillatory Ventilation for Acute Respiratory Distress Syndrome in Adults a Randomized, Controlled Trial
High-Frequency Oscillatory Ventilation for Acute Respiratory Distress Syndrome in Adults A Randomized, Controlled Trial Stephen Derdak, Sangeeta Mehta, Thomas E. Stewart, Terry Smith, Mark Rogers, Timothy G. Buchman, Brian Carlin, Stuart Lowson, John Granton, and the Multicenter Oscillatory Ventilation for Acute Respiratory Distress Syndrome Trial (MOAT) Study Investigators Pulmonary/Critical Care Medicine, Wilford Hall Medical Center, San Antonio, Texas; Departments of Medicine, Anaesthesia, Critical Care Medicine, and Trauma, Mt. Sinai Hospital, Sunnybrook and Women’s College Health Sciences Center, and University Health Network, University of Toronto, Toronto, Ontario, Canada; Departments of Critical Care Medicine and Respiratory Care, Loma Linda University Medical Center, Loma Linda, California; Division of Surgery, Barnes Jewish Hospital, St. Louis, Missouri; Department of Pulmonary/Critical Care Medicine, Allegheny General Hospital, Pittsburgh, Pennsylvania; and Departments of Anesthesia and Critical Care Medicine, University of Virginia Medical Center, Charlottesville, Virginia Observational studies of high-frequency oscillatory ventilation in tients with the acute respiratory distress syndrome (ARDS) adults with the acute respiratory distress syndrome have demon- (1–3). To avoid ventilator-induced lung injury, current recom- strated improvements in oxygenation. We designed a multicenter, mendations focus on the avoidance of both alveolar overdis- randomized, controlled trial comparing the safety and effective- tension and cyclic -

Modes of Ventilation/New Anesthesia Machine Technology
What is new in ventilation - New modes of ventilation and new Anesthesia Machine Technology Mary Theroux, MD; Stephen Stayer, MD, FAAP General Review: -Differences between pressure control and volume ventilation. -Monitoring ventilation in pediatric patients. -Can an adult anesthesia machine bellows and circle system be used to ventilate infants and children, and if so, how should it be set up? -Is there an advantage to bringing an “ICU-type” ventilator into the OR for pediatric -- patients with non-compliant lungs? -Are the technical advances of two newly available anesthesia ventilators sufficient to provide adequate ventilation for all pediatric patients with non-compliant lungs? -What is High Frequency Oscillatory Ventilation? Do we need to know HFOV? -What new developments are there that soon may become available for pediatric ventilation in the operation room? Volume Control vs. Pressure Control: Pressure limited or pressure control ventilation (PCV) is frequently applied to infants and children. There are several advantages to this mode of ventilation. Limiting the peak inflating pressure delivered by the ventilator will limit the transalveolar pressure produced, thereby reducing ventilator-induced lung injury. (1) The decelerating flow used to produce PCV is thought to improve the distribution of gas flow. (2) When compared to volume control ventilation there is a more rapid improvement in lung compliance and oxygenation. (3) Lastly, setting anesthesia ventilators to deliver accurate small tidal volumes is difficult because of -

Effects of Inverse Ratio Ventilation Combined with Lung Protective Ventilation on Pulmonary Function in Patients with Severe Burns for Surgery
Libyan Journal of Medicine ISSN: (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/zljm20 Effects of inverse ratio ventilation combined with lung protective ventilation on pulmonary function in patients with severe burns for surgery Yan-Chao Yang , Qiao Huai , Shu-Zhen Cui , Xiao-Wei Cao & Bu-Lang Gao To cite this article: Yan-Chao Yang , Qiao Huai , Shu-Zhen Cui , Xiao-Wei Cao & Bu-Lang Gao (2020) Effects of inverse ratio ventilation combined with lung protective ventilation on pulmonary function in patients with severe burns for surgery, Libyan Journal of Medicine, 15:1, 1767276, DOI: 10.1080/19932820.2020.1767276 To link to this article: https://doi.org/10.1080/19932820.2020.1767276 © 2020 The Author(s). Published by Informa UK Limited, trading as Taylor & Francis Group. Published online: 22 May 2020. Submit your article to this journal Article views: 367 View related articles View Crossmark data Full Terms & Conditions of access and use can be found at https://www.tandfonline.com/action/journalInformation?journalCode=zljm20 LIBYAN JOURNAL OF MEDICINE 2020, VOL. 15, 1767276 https://doi.org/10.1080/19932820.2020.1767276 ARTICLE Effects of inverse ratio ventilation combined with lung protective ventilation on pulmonary function in patients with severe burns for surgery Yan-Chao Yanga, Qiao Huaia, Shu-Zhen Cuia, Xiao-Wei Caob and Bu-Lang Gaoa aDepartment of Anesthesiology, Shijiazhuang First Hospital, Hebei Medical University, Shijiazhuang, Hebei Province, China; bRespiratory Department, Shijiazhuang First Hospital, Hebei Medical University, Shijiazhuang, Hebei Province, China ABSTRACT ARTICLE HISTORY Objective: To investigate the effects of inverse ratio ventilation combined with lung- Received 4 March 2020 protective ventilation on pulmonary function and inflammatory factors in severe burn Accepted 1 April 2020 Populations and Methods patients undergoing surgery. -

Predictors of Mortality in Acute Lung Injury During the Era
Acutelunginjury Predictors of mortality in acute lung injury during the Thorax: first published as 10.1136/thx.2007.093658 on 19 June 2008. Downloaded from era of lung protective ventilation E Seeley,1 D F McAuley,2 M Eisner,1 M Miletin,1,3 M A Matthay,1 R H Kallet4 1 Departments of Medicine and ABSTRACT ratio,9 respiratory system compliance (Crs)3 and Anesthesia, Cardiovascular Background: Lung protective ventilation has been widely oxygenation index (OI).7 To our knowledge, no Research Institute, University of large study of mortality predictors has been California, San Francisco, adopted for the management of acute lung injury (ALI) and California, USA; 2 Respiratory acute respiratory distress syndrome (ARDS). Consequently, conducted in North America since the implemen- Medicine Research Group, ventilator associated lung injury and mortality have tation of the lung protective ventilation. Thus we Queen’s University of Belfast, decreased. It is not known if this ventilation strategy conducted a retrospective study of these variables Belfast, Northern Ireland, UK; changes the prognostic value of previously identified to identify early predictors of mortality in ALI/ 3 Department of Medicine, William Osler Health Centre, demographic and pulmonary predictors of mortality, such as ARDS after adoption of lung protective ventila- Toronto, Canada; 4 Department respiratory compliance and the arterial oxygen tension to tion. We hypothesised that this ventilation strat- of Anesthesia, University of inspired oxygen fraction ratio (PaO2/FiO2). egy may attenuate the predictive value of California, San Francisco at San Methods: Demographic, clinical, laboratory and pulmon- previously identified pulmonary specific measures. Francisco General Hospital, San Francisco, California, USA ary variables were recorded in 149 patients with ALI/ ARDS. -
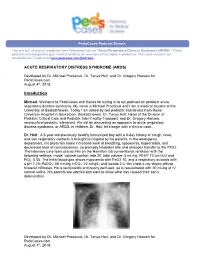
Acute Respiratory Distress Syndrome (ARDS).” These Podcasts Are Designed to Give Medical Students an Overview of Key Topics in Pediatrics
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on “Acute Respiratory Distress Syndrome (ARDS).” These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio versions are accessible on iTunes or at www.pedcases.com/podcasts. ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Developed by Dr. Michael Prodanuk, Dr. Tanya Holt, and Dr. Gregory Hansen for PedsCases.com. August 4th, 2018. Introduction Michael: Welcome to PedsCases and thanks for tuning in to our podcast on pediatric acute respiratory distress syndrome. My name is Michael Prodanuk and I am a medical student at the University of Saskatchewan. Today I am joined by two pediatric intensivists from Royal University Hospital in Saskatoon, Saskatchewan; Dr. Tanya Holt, Head of the Division of Pediatric Critical Care and Pediatric Inter-Facility Transport, and Dr. Gregory Hansen, neurocritical pediatric intensivist. We will be discussing an approach to acute respiratory distress syndrome, or ARDS, in children. Dr. Holt, let’s begin with a clinical case. Dr. Holt: A 6-year-old previously healthy immunized boy with a 6-day history of cough, fever, and sick respiratory contacts is brought to hospital by his parents. In the emergency department, his physician notes increased work of breathing, hypoxemia, hypercarbia, and decreased level of consciousness, so promptly intubates him and arranges transfer to the PICU. The intensive care team places him on the Hamilton G5 conventional ventilator with the following settings: mode: volume control; rate 20; tidal volume: 5 mL/kg; PEEP 10 cm H2O and FiO2: 0.55. The initial blood gas shows hypoxemia with PaO2 70, and a respiratory acidosis with a pH 7.20; PaCO2: 58 mmHg; HCO3: 22 mEq/L; and lactate 2.3. -

Clinical Management of Severe Acute Respiratory Infection (SARI) When COVID-19 Disease Is Suspected Interim Guidance 13 March 2020
Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected Interim guidance 13 March 2020 This is the second edition (version 1.2) of this document, which was originally adapted from Clinical management of severe acute respiratory infection when MERS-CoV infection is suspected (WHO, 2019). It is intended for clinicians involved in the care of adult, pregnant, and paediatric patients with or at risk for severe acute respiratory infection (SARI) when infection with the COVID-19 virus is suspected. Considerations for paediatric patients and pregnant women are highlighted throughout the text. It is not meant to replace clinical judgment or specialist consultation but rather to strengthen clinical management of these patients and to provide up-to-date guidance. Best practices for infection prevention and control (IPC), triage and optimized supportive care are included. This document is organized into the following sections: 1. Background 2. Screening and triage: early recognition of patients with SARI associated with COVID-19 3. Immediate implementation of appropriate IPC measures 4. Collection of specimens for laboratory diagnosis 5. Management of mild COVID-19: symptomatic treatment and monitoring 6. Management of severe COVID-19: oxygen therapy and monitoring 7. Management of severe COVID-19: treatment of co-infections 8. Management of critical COVID-19: acute respiratory distress syndrome (ARDS) 9. Management of critical illness and COVID-19: prevention of complications 10. Management of critical illness and COVID-19: septic shock 11. Adjunctive therapies for COVID-19: corticosteroids 12. Caring for pregnant women with COVID-19 13. Caring for infants and mothers with COVID-19: IPC and breastfeeding 14. -

Oxygenation Index, an Indicator of Optimal Distending Pressure During
Intensive Care Med (2002) 28:1151–1156 DOI 10.1007/s00134-002-1368-5 EXPERIMENTAL Huibert R. van Genderingen Oxygenation index, an indicator Johannus A. van Vught Jos R. C. Jansen of optimal distending pressure during Elisabeth L. I. M. Duval Dick G. Markhorst high-frequency oscillatory ventilation? Adrian Versprille D.G. Markhorst Received: 5 June 2001 tion) in series, followed by a similar Pediatric Intensive Care Unit, decrease of Paw (deflation). Accepted: 14 May 2002 Department of Pediatrics, Published online: 20 June 2002 Vrije Universiteit Medical Center, Measurements and results: At each © Springer-Verlag 2002 PO Box 7057, 1007 MB Amsterdam, Paw level, the OI and physiological The Netherlands shunt fraction were determined. The This study was supported by SensorMedics. A. Versprille OI reached a minimum of 6.2±1.4 at Pathophysiological Laboratory, Paw 30±4 cmH2O during inflation Department of Pulmonary Diseases, and a minimum of 2.4±0.3 at Paw Erasmus University Rotterdam, 13±2 cmH O during deflation. H.R. van Genderingen (✉) PO Box 1738, 3000 DR Rotterdam, 2 Department of Clinical The Netherlands Pawoptimal was 32±6 cmH2O on the Physics & Informatics, inflation limb and 14±2 cmH2O on Vrije Universiteit Medical Center, the deflation limb. The difference PO Box 7057,1007 MB Amsterdam, The Netherlands Abstract Objective: To test the hy- between the Paw at minimal OI and e-mail: [email protected] pothesis that, during high-frequency Pawoptimal was –1.9±4.2 cmH2O (NS) Tel.: +31-20-4444118 oscillatory ventilation (HFOV) of during inflation and –1.5±1.6 cmH2O Fax: +31-20-4444147 pigs with acute lung injury, the oxy- (p<0.05) during deflation. -

An Investigation of Various Inspiratory Times and Inflation Pressures
ISSN: 2378-3516 Gilmore et al. Int J Respir Pulm Med 2019, 6:107 DOI: 10.23937/2378-3516/1410107 Volume 6 | Issue 1 International Journal of Open Access Respiratory and Pulmonary Medicine OrIgInal researCh artICle An Investigation of Various Inspiratory Times and Inflation Pressures during Airway Pressure Release Ventilation Tim W Gilmore1*, Robert E Walter1,2, Patrick C Hardigan3, Clifton F Frilot II1 and Guy M Nehrenz3 1Louisiana State University Health Sciences Center, Shreveport, USA 2University Health Shreveport, USA Check for 3Nova Southeastern University, USA updates *Corresponding author: Tim W Gilmore, PhD, RRT-ACCS, RRT-NPS, AE-C, Louisiana State University Health Sciences Center, 1450 Claiborne Avenue, Shreveport, Louisiana, USA Abstract Keywords An Evaluation of Various Inspiratory Times and Inflation Airway pressure release ventilation (APRV), Ventilator set- Pressures During Airway Pressure Release Ventilation. tings, Inspiratory time, Inflation pressures Introduction: There are few recommendations how best to apply certain modes of mechanical ventilation, and the An Evaluation of Various Inspiratory Times and Infla- application of Airway Pressure Release Ventilation (APRV) tion Pressures During Airway Pressure Release Ventila- requires strategic implementation of specific inspiratory tion (I-time) and expiratory times (E-time) and particular mean airway pressures (MAWP), neither of which is standardized. Introduction We sought to identify whether an ideal I-time or MAWP could be identified to favor more positive clinical outcomes. Temporary positive pressure ventilation (PPV) is a Methods: A retrospective analysis of archived electronic common, potentially life-saving, modality, but it poses health record data to evaluate the clinical outcomes of significant risks [1-3]. It has been established that PPV is adult patients that had been placed on APRV for a target anti-physiologic and contributes to morbidity and mor- of at least 8 hours. -

A Study of Inflammatory Response and Lung Injury Induced by Variable Tidal Volumes in Mechanically Ventilated Children
http:// ijp.mums.ac.ir Original Article (Pages: 13193-13201) A Study of Inflammatory Response and Lung Injury Induced by Variable Tidal Volumes in Mechanically Ventilated Children *Ahlam M. Ismail1, Zeinab M. Mohey El- Deen 2, Ibtsam Faarouk M. El Karn 3, Mohamed M. Sayed4, Khaled A. Abdel Baseer 5,1 ¹Assistant professor of Pediatrics, Minia Faculty of Medicine, Minia University, Egypt. ²Professor of Pediatrics, Assiut Faculty of Medicine, Assiut University, Egypt. ³Professor of Clinical Pathology, Faculty of Medicine, Assiut University, Egypt. ⁴Lecturer of Pediatrics, Qena Faculty of Medicine, South Valley University, Egypt. ⁵Assistant professor of Pediatrics, Qena Faculty of Medicine, South Valley University, Egypt. Abstract Background We aimed to compare the effects of high tidal volume (Vt) versus low Vt mechanical ventilation (MV) on systemic interleukin-8 (IL-8), and tumor necrosis factor alpha (TNF- α) cytokines production and induction of lung injury in mechanically ventilated children. Materials and Methods: This prospective observational study was performed on 60 critically ill mechanically ventilated children from 2018 to 2019, at PICU of South Valley University and Minia University hospitals, Qena and Minia cities, Egypt. After application of the inclusion and exclusion criteria, we compared MV with high Vt of 9-11 ml (group I) versus low Vt of 5-7ml (group II) per kilogram of predicted body weight in critically ill children. Plasma levels of IL8 and TNF- α cytokines were estimated at the onset of MV and after 24 hours in both groups. Lung injury development was evidenced by change in oxygenation parameters. Results: Sixty patients on MV (30 with high Vt versus 30 with lower Vt) were enrolled in the study.