Testicular Torsion
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Non-Certified Epididymitis DST.Pdf
Clinical Prevention Services Provincial STI Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 Tel : 604.707.5600 Fax: 604.707.5604 www.bccdc.ca BCCDC Non-certified Practice Decision Support Tool Epididymitis EPIDIDYMITIS Testicular torsion is a surgical emergency and requires immediate consultation. It can mimic epididymitis and must be considered in all people presenting with sudden onset, severe testicular pain. Males less than 20 years are more likely to be diagnosed with testicular torsion, but it can occur at any age. Viability of the testis can be compromised as soon as 6-12 hours after the onset of sudden and severe testicular pain. SCOPE RNs must consult with or refer all suspect cases of epididymitis to a physician (MD) or nurse practitioner (NP) for clinical evaluation and a client-specific order for empiric treatment. ETIOLOGY Epididymitis is inflammation of the epididymis, with bacterial and non-bacterial causes: Bacterial: Chlamydia trachomatis (CT) Neisseria gonorrhoeae (GC) coliforms (e.g., E.coli) Non-bacterial: urologic conditions trauma (e.g., surgery) autoimmune conditions, mumps and cancer (not as common) EPIDEMIOLOGY Risk Factors STI-related: condomless insertive anal sex recent CT/GC infection or UTI BCCDC Clinical Prevention Services Reproductive Health Decision Support Tool – Non-certified Practice 1 Epididymitis 2020 BCCDC Non-certified Practice Decision Support Tool Epididymitis Other considerations: recent urinary tract instrumentation or surgery obstructive anatomic abnormalities (e.g., benign prostatic -

The Impact of Testicular Torsion on Testicular Function
Review Article pISSN: 2287-4208 / eISSN: 2287-4690 World J Mens Health Published online Apr 10, 2019 https://doi.org/10.5534/wjmh.190037 The Impact of Testicular Torsion on Testicular Function Frederik M. Jacobsen1 , Trine M. Rudlang1 , Mikkel Fode1 , Peter B. Østergren1 , Jens Sønksen1 , Dana A. Ohl2 , Christian Fuglesang S. Jensen1 ; On behalf of the CopMich Collaborative 1Department of Urology, Herlev and Gentofte Hospital, University of Copenhagen, Herlev, Denmark, 2Department of Urology, University of Michigan, Ann Arbor, MI, USA Torsion of the spermatic cord is a urological emergency that must be treated with acute surgery. Possible long-term effects of torsion on testicular function are controversial. This review aims to address the impact of testicular torsion (TT) on the endo- crine- and exocrine-function of the testis, including possible negative effects of torsion on the function of the contralateral testis. Testis tissue survival after TT is dependent on the degree and duration of TT. TT has been demonstrated to cause long- term decrease in sperm motility and reduce overall sperm counts. Reduced semen quality might be caused by ischemic dam- age and reperfusion injury. In contrast, most studies find endocrine parameters to be unaffected after torsion, although few report minor alterations in levels of gonadotropins and testosterone. Contralateral damage after unilateral TT has been sug- gested by histological abnormalities in the contralateral testis after orchiectomy of the torsed testis. The evidence is, however, limited as most human studies are small case-series. Theories as to what causes contralateral damage mainly derive from animal studies making it difficult to interpret the results in a human context. -

Redalyc.HEMATOCELE CRÓNICO CALCIFICADO. a PROPOSITO DE UN CASO
Archivos Españoles de Urología ISSN: 0004-0614 [email protected] Editorial Iniestares S.A. España Jiménez Yáñez, Rosa; Gallego Sánchez, Juan Antonio; Gónzalez Villanueva, Luis; Torralbo, Gloria; Ardoy Ibáñez, Francisco; Pérez, Miguel HEMATOCELE CRÓNICO CALCIFICADO. A PROPOSITO DE UN CASO. Archivos Españoles de Urología, vol. 60, núm. 3, 2007, pp. 303-306 Editorial Iniestares S.A. Madrid, España Disponible en: http://www.redalyc.org/articulo.oa?id=181013938015 Cómo citar el artículo Número completo Sistema de Información Científica Más información del artículo Red de Revistas Científicas de América Latina, el Caribe, España y Portugal Página de la revista en redalyc.org Proyecto académico sin fines de lucro, desarrollado bajo la iniciativa de acceso abierto 303 HEMATOCELE CRÓNICO CALCIFICADO. A PROPOSITO DE UN CASO. en la que se realizan varias biopsias de la albugínea en 8. KIHL, B.; BRATT, C.G.; KNUTSSON, U. y cols.: la zona distal del cuerpo cavernoso con una aguja de “Priapism: evaluation of treatment with special re- biopsia tipo Trucut. Una modificación quirúrgica a cielo ferent to saphenocavernous shunting in 26 patients”. abierto más agresiva de este tipo de derivación es la Scand. J. Urol. Nephrol., 14: 1, 1980. intervención que propone El-Ghorab. En ella se realiza *9. MONCADA, J.: “Potency disturbances following una comunicación caverno-esponjosa distal mediante saphenocavernous bypass in priapism (Grayhack una incisión transversal en la cara dorsal del glande a procedure)”. Urologie, 18: 199, 1979. 0.5-1cm del surco balanoprepucial. Se retira una por- 10. WILSON, S.K.; DELK, J.R.; MULCAHY, J.J. y ción de albugínea en la parte distal de cada cuerpo cols.: “Upsizing of inflatable penile implant cylin- cavernoso. -

Testicular Torsion N
n Testicular Torsion n The testicle’s ability to produce sperm may be impaired. Testicular torsion is the most serious cause of This does not necessarily mean your son will be infertile pain of the scrotum (the sac containing the testi- (unable to have children). Fertility may still be normal as cles) in boys. This causes interruption of the blood long as the other testicle is unharmed. supply, which can rapidly lead to permanent dam- age to the testicle. Immediate surgery is required. In severe cases, the testicle may die. If this occurs, sur- Boys who are having pain in the testicles always gery may be needed to remove it. need prompt medical attention. What puts your child at risk of testicular torsion? What is testicular torsion? Torsion is most common in boys ages 12 and older. It Testicular torsion occurs when the spermatic cord leading rarely occurs in boys under 10. to the testicles becomes twisted. It causes sudden pain and There are no known risk factors. However, if torsion swelling of the scrotum. Loss of blood supply to the affected occurs in one testicle, there is a risk that it may occur testicle can rapidly cause damage. in the other testicle. When your son has surgery for tes- Boys with pain and swelling of the scrotum need imme- ticular torsion, the surgeon will place a few stitches in diate medical attention. If your child has testicular torsion, the second testicle to prevent it from becoming rotated. he will probably need emergency surgery. In severe cases, surgery should be performed within 4 to 6 hours to prevent permanent damage to the testicle. -

American Urological Association Guideline on the Management of Priapism
0022-5347/03/1704-1318/0 Vol. 170, 1318–1324, October 2003 ® THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright © 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000087608.07371.ca AMERICAN UROLOGICAL ASSOCIATION GUIDELINE ON THE MANAGEMENT OF PRIAPISM DROGO K. MONTAGUE (CO-CHAIR),* JONATHAN JAROW (CO-CHAIR),† GREGORY A. BRODERICK,‡ ROGER R. DMOCHOWSKI,§ JEREMY P. W. HEATON, TOM F. LUE,¶ AJAY NEHRA,** IRA D. SHARLIP,†† AND MEMBERS OF THE ERECTILE DYSFUNCTION GUIDELINE UPDATE PANEL‡‡ INTRODUCTION priapism would eventually resolve on its own albeit with Priapism, a relatively uncommon disorder, is a medical possible permanent damage to the penis. The literature re- emergency. Although not all forms of priapism require im- viewed for this guideline straddles both empirical and mediate intervention, ischemic priapism is associated with pathophysiology-based eras, and some of the reported posi- progressive fibrosis of the cavernosal tissues and erectile tive responses to treatment may reflect the natural course of dysfunction.1, 2 Thus, all patients with priapism should be priapism rather than a true treatment success. In addition, evaluated immediately in order to intervene as early as pos- the literature is bereft of followup data on patients with sible in those patients with ischemic priapism. The goal of priapism. the management of all patients with priapism is to achieve This document derives from a comprehensive review of the detumescence and preserve erectile function. Unfortunately, medical literature related to the management of priapism. As some of the treatments aimed at correcting priapism have noted, deficiencies in this literature made it impossible to the potential complication of erectile dysfunction. -

Risk Factors for Squamous Cell Carcinoma of the Penis— Population-Based Case-Control Study in Denmark
2683 Risk Factors for Squamous Cell Carcinoma of the Penis— Population-Based Case-Control Study in Denmark Birgitte Schu¨tt Madsen,1 Adriaan J.C. van den Brule,2 Helle Lone Jensen,3 Jan Wohlfahrt,1 and Morten Frisch1 1Department of Epidemiology Research, Statens Serum Institut, Artillerivej 5, Copenhagen, Denmark; 2Department of Pathology, VU Medical Center, Amsterdam and Laboratory for Pathology and Medical Microbiology, PAMM Laboratories, Michelangelolaan 2, 5623 EJ Eindhoven, the Netherlands;and 3Department of Pathology, Gentofte University Hospital, Niels Andersens Vej 65, Hellerup, Denmark Abstract Few etiologic studies of squamous cell carcinoma female sex partners, number of female sex partners (SCC) of the penis have been carried out in populations before age 20, age at first intercourse, penile-oral sex, a where childhood circumcision is rare. A total of 71 history of anogenital warts, and never having used patients with invasive (n = 53) or in situ (n = 18) penile condoms. Histories of phimosis and priapism at least 5 SCC, 86 prostate cancer controls, and 103 population years before diagnosis were also significant risk controls were interviewed in a population-based case- factors, whereas alcohol abstinence was associated control study in Denmark. For 37 penile SCC patients, with reduced risk. Our study confirms sexually tissue samples were PCR examined for human papil- transmitted HPV16 infection and phimosis as major lomavirus (HPV) DNA. Overall, 65% of PCR-examined risk factors for penile SCC and suggests that penile- penile SCCs were high-risk HPV-positive, most of oral sex may be an important means of viral transmis- which (22 of 24; 92%) were due to HPV16. -

Radionuclidescrotalimaging:Furtherexperiencewith 210 Newpatients Part2: Resultsanddiscussion
ADJUNC11VE MEDICAL KNOWLEDGE RadionuclideScrotalImaging:FurtherExperiencewith 210 NewPatients Part2: ResultsandDiscussion DavidC. P. Chen, Lawrence E. Holder,and Moshe Melloul TheUnionMemorialHospital,arkiTheJohnsHopkinsMedicallnstitutions,Baltimore,Maryland J Nuci Med 24: 841—853,1983 RESULTS Clinically these patients had less severe pain, less Acutescrotalpain.The finaldiagnosesof 109patients swelling, and more focal tenderness. The diagnosis is presenting with acute scrotal pain are shown in Table 1. confirmed by the scan findings. In the RNAs of a ma Those who had acute pain but whose complaints were jority of these patients (n 12), there was not enough directly related to trauma are listed separately in Table blood flow through spermatic cord or extra-cord vessels 5. Sixty-nine patients had acute scrotal inflammation to define them. Mild, increased perfusion was noted in that responded to antibiotic treatment. Despite imaging seven patients (four only in the cord vessels and three in diagnosis of inflammation, three patients were operated both cord and extra-cord vessels). Scrotal perfusion in on because the clinician strongly suspected torsion. The 17 patients showed a small area of increased focal ac pathologic results confirmed acute inflammation in the tivity that corresponded to the inflamed portion of the epididymis, with torsion absent. Forty-five patients had epididymis. In two patients the RNAs showed no in acute epididymitis. In 32 of these the RNA pattern creased scrotal perfusion. The scrotal image was ab consisted of increased perfusion through the vessels of normal in all 19 patients, demonstrating a focal area of the spermatic cord and to the lateral aspect of the hem tracer accumulation corresponding to the anatomical iscrotum, corresponding to the usual location of the ep location of the head (n 9), body (n 6), or tail (n ididymis. -

Scrotal and Genital Emergencies
Chapter 6 Scrotal and Genital Emergencies John Reynard and Hashim Hashim TORSION OF THE TESTIS AND TESTICULAR APPENDAGES During fetal development the testis descends into the inguinal canal and as it does so it pushes in front of it a covering of peri- toneum (Fig. 6.1). This covering of peritoneum, which actually forms a tube, is called the processus vaginalis. The testis lies behind this tube of peritoneum and by birth, or shortly after- ward, the lumen of the tube becomes obliterated. In the scrotum, the tube of peritoneum is called the tunica vaginalis. The testis essentially is pushed into the tunica vaginalis from behind. The tunica vaginalis, therefore, is actually two layers of peritoneum, which cover the testis everywhere apart from its most posterior surface (Fig. 6.2). The layer of peritoneum that is in direct contact with the testis is called the visceral layer of the tunica vaginalis, and the layer that surrounds this, and actually covers the inner surface of the scrotum, is called the parietal layer of the tunica vaginalis. In the neonate, the parietal layer of the tunica vaginalis may not have firmly fused with the other layers of the scrotum, and therefore it is possible for the tunica vaginalis and the contained testis to twist within the scrotum. This is called an extravaginal torsion, i.e., the twist occurs outside of the two layers of the tunica vaginalis. In boys and men, the parietal layer of the tunica vaginalis has fused with the other layers of the scrotum. Thus, an extravaginal torsion cannot occur. -
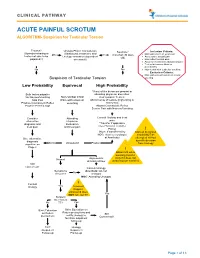
ACUTE PAINFUL SCROTUM ALGORITHM- Suspicion for Testicular Torsion
CLINICAL PATHWAY ACUTE PAINFUL SCROTUM ALGORITHM- Suspicion for Testicular Torsion Trauma? Urology Phone Consultation Neonate? Inclusion Criteria: (Open/penetrating or (Ultrasound, treatment, and Yes Yes (less than 30 days • Male patients 0-21 years old testes not able to be Urology evaluation dependent • Acute onset scrotal pain old) palpated?) on consult) • Intermittent scrotal pain • Acute or intermittent abdominal pain • Testicular trauma: blunt or penetrating No No • Non-verbal with testicular swelling Exclusion Criteria: • Male patients with painless scrotal Suspicion of Testicular Torsion swelling Low Probability Equivocal High Probability *If any of the below are present or Both testes palpable attending physician discretion: No Nausea/Vomiting Non-Verbal Child Can’t palpate Testicle Mild Pain Pain with nausea/ Abnormal lie of testicle (high-riding or Positive Cremasteric Reflex vomiting horizontal) Positive Prehn’s Sign Absent Cremasteric Reflex Severe Pain with Nausea/Vomiting Consider Attending Consult Urology and treat alternative Physician pain diagnosis and Evaluation *Transfer if applicable treat pain and treat pain (see EMTALA Transfer Policy) ! (Note: If transferred by Manual Detorsion NOC, must see urologist should NOT be See alternative at Anschutz) attempted without diagnosis specific direction Alt Dx Ultrasound Positive algorithm on from Urology Page 2 ! Obtain US while awaiting transfer (only if it does not Normal Asymmetric diminished flow delay/impede transfer) Still concerned? Consult Urology Symptoms Anschutz: -

Importance of the Testicular Torsion in the Male Infertility
Importance of the testicular torsion in the male infertility A. Rusz, Gy. Papp Military Hospital-State Health Centre (ÁEK) EAA Centre Budapest, Hungary Acute scrotum • Torsion of the testis • Torsion of the appendix testis • Acute epididymitis • Epididymo -orchitis • Other causes – Viral orchitis,varicocele,hernia,hematoma, systemic disease, idiopathic oedema, Testicular torsion • Torsion of spermatic cord • Strangulation of the blood supply • Oedema, ischemia, inflammation • Fibrosis, atrophy • Necrosis • Loss of exocrin and endocrin function Clinical findings • Sudden severe pain in testicle • Swelling of the testicle • Reddening of the scrotal skin • Lower abdominal pain,nausea,vomiting • Swollen,tender,retracted testicle • Horizontal testicular position • Color Doppler Sonography: absence of arterial flow Differential diagnosis • Acute epididymitis: age, pyuria • Acute orchitis: mumps, parotitis • Trauma: findings of injury • Cryptorchid testis is prone to torsion • Torsion frequently occurs during sleep Suspicion of torsion? Emergency! Immediate action is needed! Urgent decision about surgical intervention! Acute treatment • Manual detorsion (right „unscrewed”, left „screwed up”) and surgical fixation • Surgical detorsion and bilateral fixation • Orchiectomy and surgical fixation of opposite testicle • Testicular biopsy/cryopreservation (?) • Protective medical treatment (?) Protective medical treatments • Traditional empiric treatments – Antibiotics – Antiinflammatory drugs – Infusions,fluid therapy • Experimental – Opioids (morphine) -

The Acute Scrotum – the Two Most Difficult US Problems
The acute scrotum – the two most difficult US problems Simon Freeman Derriford Hospital, Plymouth. UK [email protected] The Acute Scrotum 1. Ischaemia 1. Spermatic cord torsion 2. Torsion of a testicular or epididymal appendage 3. Testicular Infarction (Other vascular causes) 2. Trauma 3. Infection 1. Acute epididymitis, epididymo-orchitis, orchitis 2. Abscess 3. Fournier’s gangrene 4. Inflammation 1. Henoch-Schonlein purpura 5. Incarcerated/strangulated inguinoscrotal hernia 6. Other 1. Testicular tumour (rupture, haemorrhage, infarction) 2. Varicocoele 3. Hydrocoele/Spermatocoele rupture, infection Scrotal Trauma Suspected torsion of the spermatic cord Bottom Line: Does the Patient Need Surgery Now? Scrotal Trauma • Rare (<1% of trauma related injuries) • Testes protected by: – Mobility in scrotum – Cremasteric reflex – Strength of tunica albuginea Normal Anatomy • Tunica albuginea – Very high tensile strength (50kg) • Tunica vasculosa – Lies immediately below albuginea – When disrupted results in ischaemia and disruption of the blood-testis barrier (possible effect on fertility) Mechanism of Injury • Blunt injury (85%) – Crush against pubic bone (Rt>Lt) – Sporting activity >50% – RTA 9-17% • Penetrating injury (15%) – Sharp objects and missiles – Bites (human and animal) Blunt Scrotal Trauma • Spectrum of injuries – Testicular rupture – Testicular fracture – Testicular dislocation – Spermatic cord torsion – Haematoma • Intratesticular • Extratesticular – Haematocoele Clinical Examination • Clinical examination can be very difficult -

Erectile Dysfunction and Prostate Diseases Are the Predominant Google Search Terms Amongst Men’S Health Topics
IJIR: Your Sexual Medicine Journal https://doi.org/10.1038/s41443-021-00448-1 ARTICLE Erectile dysfunction and prostate diseases are the predominant Google search terms amongst men’s health topics 1 2 2,3 Karim Hanna ● Mark Arthur ● Charles Welliver Received: 26 December 2020 / Revised: 26 April 2021 / Accepted: 6 May 2021 © The Author(s), under exclusive licence to Springer Nature Limited 2021 Abstract Patients are becoming increasingly active consumers of health information on the internet with urologic concerns being no exception. Our objective was to explore online search trends for topics related to men’s health and identify information- seeking patterns related to news and media coverage of these topics. We used Google Trends (http://google.com/trends)to explore search trends for various search terms related to men’s health in the United States over a 5-year period. Search queries provided graphs depicting search volume as a function of time, geographical data, and related topics and queries. Isolated spikes in search volume were further explored to identify a related event. Erectile dysfunction was the most- searched topic over the last 5 years in the United States. Prostate cancer and benign prostatic hyperplasia were the second 1234567890();,: 1234567890();,: and third most-searched topics, respectively. Other popular topics involved symptoms or pathologies of the testicles and penis. Most topics had relatively stable search volumes, with the exceptions of premature ejaculation and Peyronie’s disease. Several observed spikes in search volume were attributable to singular events, mostly in the form of online article publications or social media posts. We believe it may be helpful for providers to stay informed of cultural events relating to medical conditions to anticipate patient concerns.