ACUTE PAINFUL SCROTUM ALGORITHM- Suspicion for Testicular Torsion
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Urology / Gynecology Business Unit (UGBU) Strategy
Urology / Gynecology Business Unit (UGBU) Strategy Minoru Okabe Head of Uro/Gyn Business Unit Olympus Corporation March 30, 2016 Todayʼs Agenda 1.Business Overview 2.Recognition of Current Conditions 3.Market Trends 4.Business Strategies 5.Targets and Indicators 2 2016/3/30 No data copy / No data transfer permitted Todayʼs Agenda 1.Business Overview 2.Recognition of Current Conditions 3.Market Trends 4.Business Strategies 5.Targets and Indicators 3 2016/3/30 No data copy / No data transfer permitted Positioning of UG Business within Olympus 4 2016/3/30 No data copy / No data transfer permitted Distribution of Sales and Positioning FY2016 Net Sales (Forecast) Urology / Gynecology Business Unit (UGBU)* ET 72.0 Surgical Flexible and rigid endoscopes Benign prostatic hypertrophy and bladder Medical Business Devices* GI (ureteroscopes and cystoscopes) tumor resectoscopes and therapeutic FY2016 Net Sales electrodes (disposable) 337.4 205.6 (Forecast) ¥615.0 billion Urology field Flexible hysteroscopes * The figure for Surgical Devices net sales (¥205.6 billion) includes Stone treatment Gynecology field net sales of the Urology / Gynecology Business Unit (UGBU). devices (disposable) Resectoscopes Colposcopes 5 2016/3/30 No data copy / No data transfer permitted Applications and Characteristics of Major Products Field Urology Flexible Ureteroscope Stone Treatment Therapeutic Flexible Cystoscope Resectoscope URF-V2 Devices Electrodes (Disposable) CYF-VH OES Pro. (Disposable) Product Flexible ureteroscopes are used for Flexible cystoscopes are Resectoscopes are used to treat treating urinary stones. used to treat bladder benign prostatic hypertrophy and Feature Olympus flexible ureteroscopes have a tumors. bladder tumors. dominating edge realized by merging GI Olympus flexible Bipolar TURis electrodes endoscope technologies with the small cystoscopes have a (disposable) boast higher levels of diameter scope technologies of former dominating edge realized cutting safety and performance company Gyrus. -

Reference Sheet 1
MALE SEXUAL SYSTEM 8 7 8 OJ 7 .£l"00\.....• ;:; ::>0\~ <Il '"~IQ)I"->. ~cru::>s ~ 6 5 bladder penis prostate gland 4 scrotum seminal vesicle testicle urethra vas deferens FEMALE SEXUAL SYSTEM 2 1 8 " \ 5 ... - ... j 4 labia \ ""\ bladderFallopian"k. "'"f"";".'''¥'&.tube\'WIT / I cervixt r r' \ \ clitorisurethrauterus 7 \ ~~ ;~f4f~ ~:iJ 3 ovaryvagina / ~ 2 / \ \\"- 9 6 adapted from F.L.A.S.H. Reproductive System Reference Sheet 3: GLOSSARY Anus – The opening in the buttocks from which bowel movements come when a person goes to the bathroom. It is part of the digestive system; it gets rid of body wastes. Buttocks – The medical word for a person’s “bottom” or “rear end.” Cervix – The opening of the uterus into the vagina. Circumcision – An operation to remove the foreskin from the penis. Cowper’s Glands – Glands on either side of the urethra that make a discharge which lines the urethra when a man gets an erection, making it less acid-like to protect the sperm. Clitoris – The part of the female genitals that’s full of nerves and becomes erect. It has a glans and a shaft like the penis, but only its glans is on the out side of the body, and it’s much smaller. Discharge – Liquid. Urine and semen are kinds of discharge, but the word is usually used to describe either the normal wetness of the vagina or the abnormal wetness that may come from an infection in the penis or vagina. Duct – Tube, the fallopian tubes may be called oviducts, because they are the path for an ovum. -

The Male Reproductive System
Management of Men’s Reproductive 3 Health Problems Men’s Reproductive Health Curriculum Management of Men’s Reproductive 3 Health Problems © 2003 EngenderHealth. All rights reserved. 440 Ninth Avenue New York, NY 10001 U.S.A. Telephone: 212-561-8000 Fax: 212-561-8067 e-mail: [email protected] www.engenderhealth.org This publication was made possible, in part, through support provided by the Office of Population, U.S. Agency for International Development (USAID), under the terms of cooperative agreement HRN-A-00-98-00042-00. The opinions expressed herein are those of the publisher and do not necessarily reflect the views of USAID. Cover design: Virginia Taddoni ISBN 1-885063-45-8 Printed in the United States of America. Printed on recycled paper. Library of Congress Cataloging-in-Publication Data Men’s reproductive health curriculum : management of men’s reproductive health problems. p. ; cm. Companion v. to: Introduction to men’s reproductive health services, and: Counseling and communicating with men. Includes bibliographical references. ISBN 1-885063-45-8 1. Andrology. 2. Human reproduction. 3. Generative organs, Male--Diseases--Treatment. I. EngenderHealth (Firm) II. Counseling and communicating with men. III. Title: Introduction to men’s reproductive health services. [DNLM: 1. Genital Diseases, Male. 2. Physical Examination--methods. 3. Reproductive Health Services. WJ 700 M5483 2003] QP253.M465 2003 616.6’5--dc22 2003063056 Contents Acknowledgments v Introduction vii 1 Disorders of the Male Reproductive System 1.1 The Male -

Varicocele.Pdf
Page 1 of 4 View this article online at: patient.info/health/varicocele-leaflet Varicocele A varicocele is like varicose veins of the small veins (blood vessels) next to one testicle (testis) or both testicles (testes). It usually causes no symptoms. It may cause discomfort in a small number of cases. Having a varicocele is thought to increase the chance of being infertile but most men with a varicocele are not infertile. Treatment is not usually needed, as most men do not have any symptoms or problems caused by the varicocele. If required, an operation can clear a varicocele. There is no agreement among experts as to whether treatment of a varicocele will cure infertility. If you are infertile and have a varicocele, it is best to discuss this with a specialist who will be up to date on current research and thinking in this area. What is a varicocele? A varicocele is a collection of enlarged (dilated) veins (blood vessels) in the scrotum. It occurs next to and above one testicle (testis) or both testes (testicles). The affected veins are those that travel in the spermatic cord. The spermatic cord is like a tube that goes from each testis up towards the lower tummy (abdomen). You can feel the spermatic cord above each testis in the upper part of the scrotum. The spermatic cord contains the tube that carries sperm from the testes to the penis (the vas deferens), blood vessels, lymphatic vessels and nerves. Normally, you cannot see or feel the veins in the spermatic cord that carry the blood from the testes. -

Reproductive System, Day 2 Grades 4-6, Lesson #12
Family Life and Sexual Health, Grades 4, 5 and 6, Lesson 12 F.L.A.S.H. Reproductive System, day 2 Grades 4-6, Lesson #12 Time Needed 40-50 minutes Student Learning Objectives To be able to... 1. Distinguish reproductive system facts from myths. 2. Distinguish among definitions of: ovulation, ejaculation, intercourse, fertilization, implantation, conception, circumcision, genitals, and semen. 3. Explain the process of the menstrual cycle and sperm production/ejaculation. Agenda 1. Explain lesson’s purpose. 2. Use transparencies or your own drawing skills to explain the processes of the male and female reproductive systems and to answer “Anonymous Question Box” questions. 3. Use Reproductive System Worksheets #3 and/or #4 to reinforce new terminology. 4. Use Reproductive System Worksheet #5 as a large group exercise to reinforce understanding of the reproductive process. 5. Use Reproductive System Worksheet #6 to further reinforce Activity #2, above. This lesson was most recently edited August, 2009. Public Health - Seattle & King County • Family Planning Program • © 1986 • revised 2009 • www.kingcounty.gov/health/flash 12 - 1 Family Life and Sexual Health, Grades 4, 5 and 6, Lesson 12 F.L.A.S.H. Materials Needed Classroom Materials: OPTIONAL: Reproductive System Transparency/Worksheets #1 – 2, as 4 transparencies (if you prefer not to draw) OPTIONAL: Overhead projector Student Materials: (for each student) Reproductive System Worksheets 3-6 (Which to use depends upon your class’ skill level. Each requires slightly higher level thinking.) Public Health - Seattle & King County • Family Planning Program • © 1986 • revised 2009 • www.kingcounty.gov/health/flash 12 - 2 Family Life and Sexual Health, Grades 4, 5 and 6, Lesson 12 F.L.A.S.H. -

Chlamydia Trachomatis Infection Mimicking Testicular Malignancy In
270 Sex Transm Inf 1999;75:270 Chlamydia trachomatis infection mimicking Sex Transm Infect: first published as 10.1136/sti.75.4.270 on 1 August 1999. Downloaded from Case report: testicular malignancy in a young man cobblestone A M Ward, J H Rogers, C S Estcourt A young man with a low risk history for sexually transmitted diseases presented with an appar- ently longstanding, previously asymptomatic scrotal mass, highly suggestive of testicular malignancy on palpation. Ultrasound sited the lesion in the epididymis. Although there was no evidence of urethritis, chlamydia polymerase chain reaction testing was positive. Tumour mark- ers were negative. Complete clinical and radiological response was achieved after a long course of doxycycline treatment, without surgical exploration of the scrotum, confirming the diagnosis of chlamydial epididymitis. (Sex Transm Inf 1999;75:270) Keywords: testicular malignancy; Chlamydia trachomatis; epididymitis A 36 year old Chinese man presented with a 2 Fifteen months later the patient was asymp- day history of a sore scrotal lump. He had no tomatic with normal examination and ultra- urethral discharge or dysuria, and no history of sonography, and negative urinary chlamydia sexually transmitted diseases. He denied any PCR. He declined semen analysis. extramarital sexual partners since his marriage 5 years ago, but acknowledged four or five female partners before that. The couple had one child and were using condoms for contra- Discussion ception. Longstanding, subacute epididymitis, present- Examination revealed left sided scrotal ing with a painless scrotal mass, and without swelling and a mildly tender mass, inseparable evidence of urethritis, is an unusual complica- from the lower pole of the left testis, with an tion of chlamydial infection.1 irregular surface and rock hard consistency. -

GERONTOLOGICAL NURSE PRACTITIONER Review and Resource M Anual
13 Male Reproductive System Disorders Vaunette Fay, PhD, RN, FNP-BC, GNP-BC GERIATRIC APPRoACH Normal Changes of Aging Male Reproductive System • Decreased testosterone level leads to increased estrogen-to-androgen ratio • Testicular atrophy • Decreased sperm motility; fertility reduced but extant • Increased incidence of gynecomastia Sexual function • Slowed arousal—increased time to achieve erection • Erection less firm, shorter lasting • Delayed ejaculation and decreased forcefulness at ejaculation • Longer interval to achieving subsequent erection Prostate • By fourth decade of life, stromal fibrous elements and glandular tissue hypertrophy, stimulated by dihydrotestosterone (DHT, the active androgen within the prostate); hyperplastic nodules enlarge in size, ultimately leading to urethral obstruction 398 GERONTOLOGICAL NURSE PRACTITIONER Review and Resource M anual Clinical Implications History • Many men are overly sensitive about complaints of the male genitourinary system; men are often not inclined to initiate discussion, seek help; important to take active role in screening with an approach that is open, trustworthy, and nonjudgmental • Sexual function remains important to many men, even at ages over 80 • Lack of an available partner, poor health, erectile dysfunction, medication adverse effects, and lack of desire are the main reasons men do not continue to have sex • Acute and chronic alcohol use can lead to impotence in men • Nocturia is reported in 66% of patients over 65 – Due to impaired ability to concentrate urine, reduced -

A Clinical Case of Fournier's Gangrene: Imaging Ultrasound
J Ultrasound (2014) 17:303–306 DOI 10.1007/s40477-014-0106-5 CASE REPORT A clinical case of Fournier’s gangrene: imaging ultrasound Marco Di Serafino • Chiara Gullotto • Chiara Gregorini • Claudia Nocentini Received: 24 February 2014 / Accepted: 17 March 2014 / Published online: 1 July 2014 Ó Societa` Italiana di Ultrasonologia in Medicina e Biologia (SIUMB) 2014 Abstract Fournier’s gangrene is a rapidly progressing Introduction necrotizing fasciitis involving the perineal, perianal, or genital regions and constitutes a true surgical emergency Fournier’s gangrene is an acute, rapidly progressive, and with a potentially high mortality rate. Although the diagnosis potentially fatal, infective necrotizing fasciitis affecting the of Fournier’s gangrene is often made clinically, emergency external genitalia, perineal or perianal regions, which ultrasonography and computed tomography lead to an early commonly affects men, but can also occur in women and diagnosis with accurate assessment of disease extent. The children [1]. Although originally thought to be an idio- Authors report their experience in ultrasound diagnosis of pathic process, Fournier’s gangrene has been shown to one case of Fournier’s gangrene of testis illustrating the main have a predilection for patients with state diabetes mellitus sonographic signs and imaging diagnostic protocol. as well as long-term alcohol misuse. However, it can also affect patients with non-obvious immune compromise. Keywords Fournier’s gangrene Á Sonography Comorbid systemic disorders are being identified more and more in patients with Fournier’s gangrene. Diabetes mel- Riassunto La gangrena di Fournier e` una fascite necro- litus is reported to be present in 20–70 % of patients with tizzante a rapida progressione che coinvolge il perineo, le Fournier’s Gangrene [2] and chronic alcoholism in regioni perianale e genitali e costituisce una vera emer- 25–50 % patients [3]. -

Urologic Disorders
Urologic Disorders Abdulaziz Althunayan Consultant Urologist Assistant professor of Surgery Urologic Disorders Urinary tract infections Urolithiasis Benign Prostatic Hyperplasia and voiding dysfunction Urinary tract infections Urethritis Acute Pyelonephritis Epididymitis/orchitis Chronic Pyelonephritis Prostatitis Renal Abscess cystitis URETHRITIS S&S – urethral discharge – burning on urination – Asymptomatic Gonococcal vs. Nongonococcal DX: – incubation period(3-10 days vs. 1-5 wks) – Urethral swab – Serum: Chlamydia-specific ribosomal RNA URETHRITIS Epididymitis Acute : pain, swelling, of the epididymis <6wk chronic :long-standing pain in the epididymis and testicle, usu. no swelling. DX – Epididymitis vs. Torsion – U/S – Testicular scan – Younger : N. gonorrhoeae or C. trachomatis – Older : E. coli Epididymitis Prostatitis Syndrome that presents with inflammation± infection of the prostate gland including: – Dysuria, frequency – dysfunctional voiding – Perineal pain – Painful ejaculation Prostatitis Prostatitis Acute Bacterial Prostatitis : – Rare – Acute pain – Storage and voiding urinary symptoms – Fever, chills, malaise, N/V – Perineal and suprapubic pain – Tender swollen hot prostate. – Rx : Abx and urinary drainage cystitis S&S: – dysuria, frequency, urgency, voiding of small urine volumes, – Suprapubic /lower abdominal pain – ± Hematuria – DX: dip-stick urinalysis Urine culture Pyelonephritis Inflammation of the kidney and renal pelvis S&S : – Chills – Fever – Costovertebral angle tenderness (flank Pain) – GI:abdo pain, N/V, and -

Non-Certified Epididymitis DST.Pdf
Clinical Prevention Services Provincial STI Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 Tel : 604.707.5600 Fax: 604.707.5604 www.bccdc.ca BCCDC Non-certified Practice Decision Support Tool Epididymitis EPIDIDYMITIS Testicular torsion is a surgical emergency and requires immediate consultation. It can mimic epididymitis and must be considered in all people presenting with sudden onset, severe testicular pain. Males less than 20 years are more likely to be diagnosed with testicular torsion, but it can occur at any age. Viability of the testis can be compromised as soon as 6-12 hours after the onset of sudden and severe testicular pain. SCOPE RNs must consult with or refer all suspect cases of epididymitis to a physician (MD) or nurse practitioner (NP) for clinical evaluation and a client-specific order for empiric treatment. ETIOLOGY Epididymitis is inflammation of the epididymis, with bacterial and non-bacterial causes: Bacterial: Chlamydia trachomatis (CT) Neisseria gonorrhoeae (GC) coliforms (e.g., E.coli) Non-bacterial: urologic conditions trauma (e.g., surgery) autoimmune conditions, mumps and cancer (not as common) EPIDEMIOLOGY Risk Factors STI-related: condomless insertive anal sex recent CT/GC infection or UTI BCCDC Clinical Prevention Services Reproductive Health Decision Support Tool – Non-certified Practice 1 Epididymitis 2020 BCCDC Non-certified Practice Decision Support Tool Epididymitis Other considerations: recent urinary tract instrumentation or surgery obstructive anatomic abnormalities (e.g., benign prostatic -

Male Infertility Low Testosterone
Male Infertility low testosterone. One of the first academic medical centers in the Both are fellowship-trained, male reproductive urologists prepared to deal nation to create a sperm bank continues to lead with the most complex infertility cases and the way in male infertility research and in complex to perform complex microsurgeries, such as vasectomy reversals and testicular-sperm clinical care. extraction. Partnering with URMC’s female infertility experts, the male infertility clinic An andrology lab and sperm bank were bank, today URMC’s Urology department is part of a designated in-vitro fertilization created more than 30 years ago at the now boasts two fellowship-trained male center of excellence in New York state. University of Rochester Medical Center infertility specialists—Jeanne H. O’Brien, (URMC). Grace M. Centola, Ph.D., M.D. and J. Scott Gabrielsen, M.D., Ph.D. Complex Care H.C.L.D., former associate professor of A nationally recognized male-infertility URMC’s male infertility clinicians see a Obstetrics and Gynecology at URMC, expert, O’Brien has received numerous growing number of patients with male- was instrumental in creating the bank, in awards and recognitions for both her factor infertility, such as decreased collaboration with Robert Davis, M.D., clinical and basic science research work. sperm counts, motility or morphology. and Abraham Cockett, M.D., from the Gabrielsen focuses on male reproductive The first steps in the care process are a Department of Urology. health, including male infertility, erectile baseline semen analysis, coupled with Building on the groundbreaking sperm dysfunction, male sexual dysfunction and an understanding of a patient’s health 4 UR Medicine | Department of Urology | urology.urmc.edu history. -
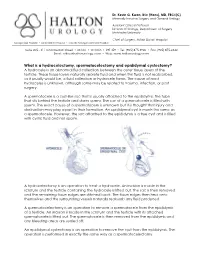
What Is a Hydrocelectomy, Spermatocelectomy and Epididymal Cystectomy? a Hydrocele Is an Abnormal Fluid Collection Between the Outer Tissue Layers of the Testicle
Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Chief of Surgery, Milton District Hospital Georgetown Hospital • Milton District Hospital • Oakville Trafalgar Memorial Hospital Suite 205 - 311 Commercial Street • Milton • Ontario • L9T 3Z9 • Tel: (905) 875-3920 • Fax: (905) 875-4340 Email: [email protected] • Web: www.haltonurology.com What is a hydrocelectomy, spermatocelectomy and epididymal cystectomy? A hydrocele is an abnormal fluid collection between the outer tissue layers of the testicle. These tissue layers naturally secrete fluid and when this fluid is not reabsorbed, as it usually would be, a fluid collection or hydrocele forms. The cause of most hydroceles is unknown, although some may be related to trauma, infection, or past surgery. A spermatocele is a cyst-like sac that is usually attached to the epididymis, the tube that sits behind the testicle and stores sperm. The sac of a spermatocele is filled with sperm. The exact cause of a spermatocele is unknown but it is thought that injury and obstruction may play a part in their formation. An epididymal cyst is much the same as a spermatocele. However, the sac attached to the epididymis is a true cyst and is filled with cystic fluid and not sperm. A hydrocelectomy is an operation to treat a hydrocele. An incision is made in the scrotum and the testicle containing the hydrocele is lifted out. The sac is then removed and the remaining tissue edges are stitched back. The tissue edges then heal onto themselves and the surrounding vessels naturally reabsorb any fluid produced.