Nausea and Vomiting
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

IRRITABLE BOWEL SYNDROME by Michael Sperling MD
IRRITABLE BOWEL SYNDROME By Michael Sperling MD Irritable bowel syndrome (IBS) involves vague symptoms of abdominal pain, diarrhea, constipation, gas and bloating for which there is no understandable cause. Incredibly, IBS affects up to 20% of the population but only three- quarters of those people actually seek medical attention. It is the second most common reason for work absenteeism. Irritable bowel symptoms may also be related to other complaints such as belching, heartburn, swallowing problems, fullness after eating, nausea, frequent urination, painful menstruation and pain during intercourse. Extremely severe cases can sometimes be related to a history of traumatic abuse. Some common associations or factors: Michael Sperling, MD 1. ‘Spastic colon’ is frequently found along with irritable bowel syndrome. Spastic colon consists of painful muscle contractions which can be relieved by bulk agents or anti- spasm drugs. 2. Post-infectious IBS occurs when irritable bowel follows a gastrointestinal infection, such as the stomach flu. These recurrent symptoms can last up to two years. 3. Stress and anxiety can worsen IBS symptoms so occasionally anti-anxiety agents may be helpful. 4. Food intolerances classically worsen symptoms of irritable bowel in some people. Common “offending foods” include lactose, legumes (beans) and cruciferous vegetables like brussel sprouts, cauliflower, broccoli and cabbage. 5. Hypersensitivity of the bowel wall: Normal colon activity is not usually noticed however in “visceral hypersensitivity”, the bowel wall reacts painfully to normal activity. This condition may be helped by the use of low dose antidepressants, which can block these painful stimuli. Careful and selective testing of patients with these symptoms and the development of a long-term doctor/patient relationship is the key to diagnosing and managing these symptoms. -

Stomach Flu (Viral Gastroenteritis)
Stomach Flu (Viral Gastroenteritis) The stomach flu (also called viral gastroenteritis) is caused by a virus (rotavirus, adenovirus, Norwalk virus to name a few) that affect the stomach and small intestines. It may come on suddenly or over the course of a few hours. The illness is usually brief, lasting 24-72 hours. Symptoms include: Nausea Vomiting Stomach cramps Diarrhea Mild fever Fatigue Body Chills/Sweats Loss of appetite Muscle aches To help take care of yourself: • The best thing to do is to let your stomach rest from solid foods. • Sip on clear liquids (Hi-C, apple, cranberry, and grape juices, Jell-O, Gatorade- type liquids and ginger-ale or ginger tea). There are special properties in ginger that help soothe the stomach. It is extremely important to keep up your hydration. Water is great for hydration but Gatorade-type products are better because they will restore your electrolytes (Sodium, Potassium and Chloride) which are essential for body functions. You may "stir" the bubbles out of the soda if the carbonation is harsh on your stomach. • Once you have not vomited for a few hours and your stomach is feeling better, you may start to eat solid foods. You may try crackers, plain noodles, eggs, broth, pretzels and yogurt. • The BRAT diet (Bananas, Rice, Applesauce & Toast) includes foods that are low in fiber and are easily digested. • Stay away from dairy products, citric (including orange and grapefruit juices), tomato-based & spicy foods. • SLOWLY increase your dietary intake to include fruits, vegetables and meat once symptoms are gone (usually over 2-3 days). -

Acute Abdomen
Acute abdomen: Shaking down the Acute abdominal pain can be difficult to diagnose, requiring astute assessment skills and knowledge of abdominal anatomy 2.3 ANCC to discover its cause. We show you how to quickly and accurately CONTACT HOURS uncover the clues so your patient can get the help he needs. By Amy Wisniewski, BSN, RN, CCM Lehigh Valley Home Care • Allentown, Pa. The author has disclosed that she has no significant relationships with or financial interest in any commercial companies that pertain to this educational activity. NIE0110_124_CEAbdomen.qxd:Deepak 26/11/09 9:38 AM Page 43 suspects Determining the cause of acute abdominal rapidly, indicating a life-threatening process, pain is often complex due to the many or- so fast and accurate assessment is essential. gans in the abdomen and the fact that pain In this article, I’ll describe how to assess a may be nonspecific. Acute abdomen is a patient with acute abdominal pain and inter- general diagnosis, typically referring to se- vene appropriately. vere abdominal pain that occurs suddenly over a short period (usually no longer than What a pain! 7 days) and often requires surgical interven- Acute abdominal pain is one of the top tion. Symptoms may be severe and progress three symptoms of patients presenting in www.NursingMadeIncrediblyEasy.com January/February 2010 Nursing made Incredibly Easy! 43 NIE0110_124_CEAbdomen.qxd:Deepak 26/11/09 9:38 AM Page 44 the ED. Reasons for acute abdominal pain Visceral pain can be divided into three Your patient’s fall into six broad categories: subtypes: age may give • inflammatory—may be a bacterial cause, • tension pain. -

Appendicitis
Appendicitis Your child has abdominal pain, it might be appendicitis. Appendicitis is swelling or infection in the appendix. The appendix is a small organ attached to the large intestine. Appendicitis usually develops over 12-24 hours. It has symptoms such as abdominal pain, nausea, vomiting, fever, and loss of appetite. Most importantly, pain that continues, worsens and moves to the right lower side of the abdomen is common in appendicitis. Appendicitis is the most common childhood “emergency” that must be treated in a timely manner. However, it’s important to know that many conditions have symptoms similar to appendicitis but don’t require surgery. At Hasbro Children’s Hospital (HCH), we evaluate your child’s abdominal pain to determine if appendicitis is the cause. That way, we avoid unnecessary operations. What happens now? Your child will be well cared for. First your child will be seen in the HCH emergency department (ED) by a nurse and doctor trained in pediatric emergency medicine. If necessary, your child will have tests that include blood work and a urinalysis. Your child’s pain will be managed with intravenous (IV) pain medication. Your child will not be allowed to eat or drink and may receive fluids through an intravenous line. Members of the pediatric surgical team will examine your child to help determine whether your child has appendicitis or another condition. We will perform a painless ultrasound on your child and the ultrasound images will be read by pediatric radiology doctors with advanced training in imaging children. Usually, ultrasound is the only imaging required but sometimes an MRI may be needed as well. -

Nausea and Vomiting (Stomach “Bug” Or Gastroenteritis)
Nausea and Vomiting •(Stomach Nausea and vomiting “Bug” is most commonly or caused Gastroenteritis) by a viral infection and may be associated with diarrhea. • This illness is self-limited with the majority of people finding improvement within 24-hours and are back to normal by 72-hours after onset of the illness. • This illness can be treated at home and does not require a visit to a medical provider. Symptoms: • Nausea with or without vomiting • Muscle aches • Generalized or upper abdominal pain/cramping • Headache • Watery diarrhea (no blood) • Possible fever Self-care measures: • Stop eating solid foods • Rest • Suck on ice chips or sip small amounts of water on a frequent basis • If you vomit, wait about 20 minutes then resume fluid intake • Slowly increase the amount of fluid intake • Water, Pedialyte® or sports drinks are acceptable • Avoid caffeine, alcohol and carbonated beverages • Acetaminophen (Tylenol®) 650 mg every 6 hours as needed for fever, chills, headache or body aches • Use Imodium for diarrhea lasting more than 2 days Recovery: • You may try solid food when: 1) Nausea and vomiting have resolved 2) You are tolerating fluids 3) You feel hungry When you do eat: • Start with small amounts of simple foods (crackers, toast, Jello®, etc.) • Over the next 24-36 hours slowly build up to your normal diet • Add dairy, high-fat foods, raw vegetables, citrus and red meat last Limit spread to others: • Wash hands with soap and water frequently • Stay home (or in your residence hall) for at least the first 24-hours • If you live in a residence hall call 540-568-6949 to get information about obtaining some appropriate food or fluids When to seek medical attention: • If the vomiting persists more than 24-hours • If you develop bloody diarrhea • If you have obvious pain or tenderness isolated to the right lower abdomen UHC self-care guidelines are based on the most recent recommendations of national medical authorities.. -
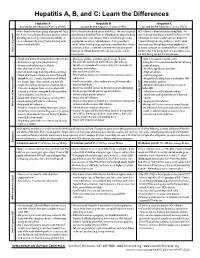
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -

Travelers' Diarrhea
Travelers’ Diarrhea What is it and who gets it? Travelers’ diarrhea (TD) is the most common illness affecting travelers. Each year between 20%-50% of international travelers, an estimated 10 million persons, develop diarrhea. The onset of TD usually occurs within the first week of travel but may occur at any time while traveling and even after returning home. The primary source of infection is ingestion of fecally contaminated food or water. You can get TD whenever you travel from countries with a high level of hygiene to countries that have a low level of hygiene. Poor sanitation, the presence of stool in the environment, and the absence of safe restaurant practices lead to widespread risk of diarrhea from eating a wide variety of foods in restaurants, and elsewhere. Your destination is the most important determinant of risk. Developing countries in Latin America, Africa, the Middle East, and Asia are considered high risk. Most countries in Southern Europe and a few Caribbean islands are deemed intermediate risk. Low risk areas include the United States, Canada, Northern Europe, Australia, New Zealand, and several of the Caribbean islands. Anyone can get TD, but persons at particular high-risk include young adults , immunosuppressed persons, persons with inflammatory-bowel disease or diabetes, and persons taking H-2 blockers or antacids. Attack rates are similar for men and women. TD is caused by bacteria, protozoa or viruses that are ingested by eating contaminated food or beverages. For short-term travelers in most areas, bacteria are the cause of the majority of diarrhea episodes. What are common symptoms of travelers’ diarrhea? Most TD cases begin abruptly. -

Chapter 34 • Drugs Used to Treat Nausea and Vomiting
• Chapter 34 • Drugs Used to Treat Nausea and Vomiting • Learning Objectives • Compare the purposes of using antiemetic products • State the therapeutic classes of antiemetics • Discuss scheduling of antiemetics for maximum benefit • Nausea and Vomiting • Nausea : the sensation of abdominal discomfort that is intermittently accompanied by a desire to vomit • Vomiting (emesis): the forceful expulsion of gastric contents up the esophagus and out of the mouth • Regurgitation : the rising of gastric or esophageal contents to the pharynx as a result of stomach pressure • Common Causes of Nausea and Vomiting • Postoperative nausea and vomiting • Motion sickness • Pregnancy Hyperemesis gravidarum: a condition in pregnancy in which starvation, dehydration, and acidosis are superimposed on the vomiting syndrome • Common Causes of Nausea and Vomiting (cont’d) • Psychogenic vomiting: self-induced or involuntary vomiting in response to threatening or distasteful situations • Chemotherapy-induced emesis (CIE) Anticipatory nausea and vomiting: triggered by sight and smell associated with treatment Acute CIE: stimulated directly by chemotherapy 1 to 6 hours after treatment Delayed emesis: occurs 24 to 120 hours after treatment; may be induced by metabolic by-products of chemotherapy • Drug Therapy for Selected Causes of Nausea and Vomiting • Postoperative nausea and vomiting (PONV) • Antiemetics include: Dopamine antagonists Anticholinergic agents Serotonin antagonists H2 antagonists (cimetidine, ranitidine) • Nursing Process for Nausea and Vomiting -

MANAGEMENT of ACUTE ABDOMINAL PAIN Patrick Mcgonagill, MD, FACS 4/7/21 DISCLOSURES
MANAGEMENT OF ACUTE ABDOMINAL PAIN Patrick McGonagill, MD, FACS 4/7/21 DISCLOSURES • I have no pertinent conflicts of interest to disclose OBJECTIVES • Define the pathophysiology of abdominal pain • Identify specific patterns of abdominal pain on history and physical examination that suggest common surgical problems • Explore indications for imaging and escalation of care ACKNOWLEDGEMENTS (1) HISTORICAL VIGNETTE (2) • “The general rule can be laid down that the majority of severe abdominal pains that ensue in patients who have been previously fairly well, and that last as long as six hours, are caused by conditions of surgical import.” ~Cope’s Early Diagnosis of the Acute Abdomen, 21st ed. BASIC PRINCIPLES OF THE DIAGNOSIS AND SURGICAL MANAGEMENT OF ABDOMINAL PAIN • Listen to your (and the patient’s) gut. A well honed “Spidey Sense” will get you far. • Management of intraabdominal surgical problems are time sensitive • Narcotics will not mask peritonitis • Urgent need for surgery often will depend on vitals and hemodynamics • If in doubt, reach out to your friendly neighborhood surgeon. Septic Pain Sepsis Death Shock PATHOPHYSIOLOGY OF ABDOMINAL PAIN VISCERAL PAIN • Severe distension or strong contraction of intraabdominal structure • Poorly localized • Typically occurs in the midline of the abdomen • Seems to follow an embryological pattern • Foregut – epigastrium • Midgut – periumbilical • Hindgut – suprapubic/pelvic/lower back PARIETAL/SOMATIC PAIN • Caused by direct stimulation/irritation of parietal peritoneum • Leads to localized -

GASTROINTESTINAL COMPLAINT Nausea, Vomiting, Or Diarrhea (For Abdominal Pain – Refer to SO-501) I
DESCHUTES COUNTY ADULT JAIL SO-559 L. Shane Nelson, Sheriff Standing Order Facility Provider: October 17, 2018 STANDING ORDER GASTROINTESTINAL COMPLAINT Nausea, Vomiting, or Diarrhea (for Abdominal Pain – refer to SO-501) I. ASSESSMENT a. History i. Onset and duration ii. Frequency of vomiting, nausea, or diarrhea iii. Blood in stool or black stools? Blood in emesis or coffee-ground appearance? If yes, refer to SO-510 iv. Medications taken – do they help? v. Do they have abdominal pain? If yes, refer to SO-501 Abdominal Pain. vi. Do they have other symptoms – dysuria, urinary frequency, urinary urgency, urinary incontinence, vaginal/penile discharge, hematuria, fever, chills, flank pain, abdominal/pelvic pain in females or testicular pain in males, vaginal or penile lesions/sores? (if yes to any of the above – refer to Dysuria SO-522) vii. LMP in female inmates – if unknown, obtain HCG viii. History of substance abuse? Are they withdrawing? Refer to appropriate SO based on substance history and withdrawal concerns. ix. History of IBS or other known medical causes of chronic diarrhea, nausea, or vomiting? Have prescriptions been used for this in the past? x. History of abdominal surgeries? xi. Recent exposure to others with same symptoms? b. Exam i. Obtain Vital signs, including temperature ii. If complaints of dizziness or lightheadedness with standing, obtain orthostatic VS. iii. Is there jaundice present? iv. Are there signs of dehydration – tachycardia, tachypnea, lethargy, changes in mental status, dry mucous membranes, pale skin color, decreased skin turgor? v. Are you concerned for an Acute Gastroenteritis? Supersedes: March 20, 2018 Review Date: October 2020 Total Pages: 3 1 SO-559 October 17, 2018 Symptoms Exam Viruses cause 75-90% of acute gastroenteritis here in the US. -

Gastritis, Acute
Gastritis, Acute Craig G. Ruaux, BVSc, PhD, DACVIM (Small Animal) BASIC INFORMATION TREATMENT AND FOLLOW-UP Description Acute gastritis occurs when the stomach becomes inflamed. Treatment Options Inflammation of the stomach makes the stomach less able to As long as other diseases have been ruled out, the treatment of handle food and water. The stomach produces acid and digestive acute gastritis is usually uncomplicated. The disease is typically enzymes that begin the breakdown of proteins and fats; when the self-limited; that is, the clinical signs usually resolve quickly, and stomach is inflamed, these processes are disturbed. supportive treatment is all that is necessary. Causes The stomach usually needs a period of rest to allow the inflam- The most common cause of acute gastritis in dogs and cats is mation to settle down. Withholding solid food for a period of 24 dietary indiscretion (eating something that does not agree with hours allows the stomach to rest. Medications (given either by them or is foreign to the stomach). Some parasites of the gastro- injection or by mouth) are often prescribed for 2-3 days to stop intestinal tract and drug reactions can also cause acute gastritis. vomiting and control nausea. While off solid food, most animals Bacterial infections are extremely uncommon causes. Some drugs still tolerate liquids. It is important that adequate hydration be used to treat cancer can lead to acute gastritis and nausea; your maintained, and if your pet can not tolerate liquids your veteri- veterinarian will warn you of this if those drugs are being used. narian may recommend giving subcutaneous (injected under the skin) fluids. -

Management of Gastrointestinal Disorders in Rett Syndrome
Management of gastrointestinal disorders in Rett syndrome Jenny Downs & Helen Leonard Telethon Kids Institute, Perth, Western Australia What is meant by gastrointestinal disorders? The three most common gastro-intestinal problems affecting girls and women with Rett syndrome are: constipation, Gastro-Oesophageal Reflux Disease or Gastro-Esophageal Reflux Disease (GORD/GERD or reflux) and abdominal bloating. Constipation occurs where stools are dry, hard and difficult to pass. Constipation can cause considerable discomfort and pain. Reflux occurs when the muscle at the lower end of the oesophagus does not close properly after food has passed through to the stomach. As a result, stomach contents can pass back up the oesophagus which can be painful, and in extreme cases, damage to the oesophagus lining. Acid may also flow back into the oesophagus when the stomach doesn’t empty properly. This is known as delayed gastric emptying. Abdominal bloating describes the swelling of the abdomen, accompanied by feelings of tightness, fullness, discomfort and pain. Why do gastrointestinal disorders occur in Rett syndrome? As the digestive system operates alongside other systems in the body (the nervous, circulatory, muscular -skeletal, respiratory and endocrine systems), disruptions to any of these systems can affect the healthy operation of the digestive system. • Reduced intestinal motility, physical activity and some side effects from various medications may cause individuals with Rett syndrome to suffer constipation. • Reflux is likely to occur in individuals with restricted mobility and/or scoliosis. • The tendency to hyperventilate, breath hold and swallow air can cause abdominal bloating. Pain, anxiety and excitement may exacerbate these issues and increase discomfort.