Management of Penetrating Brain Injury : a Case Report
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3
ISSN: 2643-4474 Raval et al. Neurosurg Cases Rev 2020, 3:046 DOI: 10.23937/2643-4474/1710046 Volume 3 | Issue 2 Neurosurgery - Cases and Reviews Open Access CASE REPORT Case Report: A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3 1 Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Gujarat, India Check for updates 2Medical Officer, CHC Dolasa, Gujarat, India 3GAIMS-GK General Hospital, Gujarat, India *Corresponding author: Dr. Himanshu Raval, Resident, Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Elisbridge, Ahmedabad, Gujarat, 380006, India, Tel: 942-955-3329 Abstract Introduction Background: Head injury is common component of any Road traffic accident (RTA) is the most common road traffic accident injury. Injury involving only frontal sinus cause of cranio-facial injury and involvement of frontal is uncommon and unique as its management algorithm is bone fractures are rare and constitute 5-9% of only fa- changing over time with development of radiological modal- ities as well as endoscopic intervention. Frontal sinus inju- cial trauma. The degree of association has been report- ries may range from isolated anterior table fractures causing ed to be 95% with fractures of the anterior table or wall a simple aesthetic deformity to complex fractures involving of the frontal sinuses, 60% with the orbital rims, and the frontal recess, orbits, skull base, and intracranial con- 60% with complex injuries of the naso-orbital-ethmoid tents. Only anterior table injury of frontal sinus is rare in pen- region, 33% with other orbital wall fractures and 27% etrating head injury without underlying brain injury with his- tory of unconsciousness and questionable convulsion which with Le Fort level fractures. -

Skin Injuries – Can We Determine Timing and Mechanism?
Skin injuries – can we determine timing and mechanism? Jo Tully VFPMS Seminar 2016 What skin injuries do we need to consider? • Bruising • Commonest accidental and inflicted skin injury • Basic principles that can be applied when formulating opinion • Abrasions • Lacerations }we need to be able to tell the difference • Incisions • Stabs/chops • Bite marks – animal v human / inflicted v ‘accidental’ v self-inflicted Our role…. We are often/usually/always asked…………….. • “What type of injury is it?” • “When did this injury occur?” • “How did this injury occur?” • “Was this injury inflicted or accidental?” • IS THIS CHILD ABUSE? • To be able to answer these questions (if we can) we need knowledge of • Anatomy/physiology/healing - injury interpretation • Forces • Mechanisms in relation to development, plausibility • Current evidence Bruising – can we really tell which bruises are caused by abuse? Definitions – bruising • BLUNT FORCE TRAUMA • Bruise =bleeding beneath intact skin due to BFT • Contusion = bruise in deeper tissues • Haematoma - extravasated blood filling a cavity (or potential space). Usually associated with swelling • Petechiae =Pinpoint sized (0.1-2mm) hemorrhages into the skin due to acute rise in venous pressure • medical causes • direct forces • indirect forces Medical Direct Indirect causes mechanical mechanical forces forces Factors affecting development and appearance of a bruise • Properties of impacting object or surface • Force of impact • Duration of impact • Site - properties of body region impacted (blood supply, -

Wound Classification
Wound Classification Presented by Dr. Karen Zulkowski, D.N.S., RN Montana State University Welcome! Thank you for joining this webinar about how to assess and measure a wound. 2 A Little About Myself… • Associate professor at Montana State University • Executive editor of the Journal of the World Council of Enterstomal Therapists (JWCET) and WCET International Ostomy Guidelines (2014) • Editorial board member of Ostomy Wound Management and Advances in Skin and Wound Care • Legal consultant • Former NPUAP board member 3 Today We Will Talk About • How to assess a wound • How to measure a wound Please make a note of your questions. Your Quality Improvement (QI) Specialists will follow up with you after this webinar to address them. 4 Assessing and Measuring Wounds • You completed a skin assessment and found a wound. • Now you need to determine what type of wound you found. • If it is a pressure ulcer, you need to determine the stage. 5 Assessing and Measuring Wounds This is important because— • Each type of wound has a different etiology. • Treatment may be very different. However— • Not all wounds are clear cut. • The cause may be multifactoral. 6 Types of Wounds • Vascular (arterial, venous, and mixed) • Neuropathic (diabetic) • Moisture-associated dermatitis • Skin tear • Pressure ulcer 7 Mixed Etiologies Many wounds have mixed etiologies. • There may be both venous and arterial insufficiency. • There may be diabetes and pressure characteristics. 8 Moisture-Associated Skin Damage • Also called perineal dermatitis, diaper rash, incontinence-associated dermatitis (often confused with pressure ulcers) • An inflammation of the skin in the perineal area, on and between the buttocks, into the skin folds, and down the inner thighs • Scaling of the skin with papule and vesicle formation: – These may open, with “weeping” of the skin, which exacerbates skin damage. -

Gunshot Wounds
Gunshot Wounds Michael Sirkin, MD Chief, Orthopaedic Trauma Service Assistant Professor, New Jersey Medical School North Jersey Orthopaedic Institute Created March 2004; Reviewed March 2006, August 2010 Ballistics • Most bullets made of lead alloy – High specific gravity • Maximal mass • Less effect of air resistance • Bullet tips – Pointed – Round – Flat – Hollow Ballistics • Low velocity bullets – Made of low melting point lead alloys – If fired from high velocity they melt, 2° to friction • Deform • Change missile ballistics • High velocity bullets – Coated or jacketed with a harder metal – High temperature coating – Less deformity when fired Velocity • Energy = ½ mv2 • Energy increases by the square of the velocity and linearly with the mass • Velocity of missile is the most important factor determining amount of energy and subsequent tissue damage Kinetic Energy of High and Low Velocity Firearms Kinetic Energy of Shotgun Shells Wounding power • Low velocity, less severe – Less than 1000 ft/sec – Less than 230 grams • High velocity, very destructive – Greater than 2000 ft/sec – Weight less than 150 grams • Shotguns, very destructive at close range – About 1200 ft/sec – Weight up to 870 grams Factors that cause tissue damage • Crush and laceration • Secondary missiles • Cavitation • Shock wave Crush and Laceration • Principle mechanism in low velocity gunshot wounds • Material in path is crushed or lacerated • The kinetic energy is dissipated • Increased tissue damage with yaw or tumble – Increased profile – Increased rate of kinetic -
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. a Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD
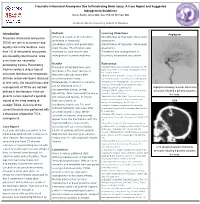
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. A Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD Southern Illinois University School of Medicine Methods Learning Objectives Introduction Angiogram Traumatic intracranial aneurysms A Pubmed search of the literature Identification of traumatic intracranial pertaining to traumatic aneurysms. (TICA) are rare in occurrence and pseudoaneurysms and penetrating Classification of traumatic intracranial equally rare in the literature. Less brain trauma. The literature was aneurysms. than 1% of intracranial aneurysms reviewed for case reports and Treatment and management of are caused by blunt trauma, while management recommendations. traumatic intracranial aneurysms. even fewer are caused by penetrating trauma. Penetrating Results References Traumatic intracranial aneurysm 1.Aarabi B. Management of traumatic aneurysms caused by trauma creates a unique type of high-velocity missile head wounds. Neurosurg Clin N Am. formation is the most commonly aneurysm that does not incorporate Oct 1995;6(4):775-797. described vascular injury after 2.Rao GP, Rao NS, Reddy PK. Technique of removal of an all three vessel wall layers. Because penetrating brain injury. impacted sharp object in a penetrating head injury using the of their rarity, the natural history and Histologically, traumatic aneurysms lever principle. Br J Neurosurg. Dec 1998;12(6):569-571. 3.Vascular complications of penetrating brain injury. J can be described as true management of TICAs are not well Trauma. Aug 2001;51(2 Suppl):S26-28. Angiogram showing traumatic intracranial (incorporating intima, media, defined in the literature. Here we 4.Crompton MR. The pathogenesis of cerebral aneurysms. aneurysm following a gunshot wound to adventitia), false (incorporating one or Brain. -

Pressure Ulcer Staging Cards and Skin Inspection Opportunities.Indd
Pressure Ulcer Staging Pressure Ulcer Staging Suspected Deep Tissue Injury (sDTI): Purple or maroon localized area of discolored Suspected Deep Tissue Injury (sDTI): Purple or maroon localized area of discolored intact skin or blood-fi lled blister due to damage of underlying soft tissue from pressure intact skin or blood-fi lled blister due to damage of underlying soft tissue from pressure and/or shear. The area may be preceded by tissue that is painful, fi rm, mushy, boggy, and/or shear. The area may be preceded by tissue that is painful, fi rm, mushy, boggy, warmer or cooler as compared to adjacent tissue. warmer or cooler as compared to adjacent tissue. Stage 1: Intact skin with non- Stage 1: Intact skin with non- blanchable redness of a localized blanchable redness of a localized area usually over a bony prominence. area usually over a bony prominence. Darkly pigmented skin may not have Darkly pigmented skin may not have visible blanching; its color may differ visible blanching; its color may differ from surrounding area. from surrounding area. Stage 2: Partial thickness loss of Stage 2: Partial thickness loss of dermis presenting as a shallow open dermis presenting as a shallow open ulcer with a red pink wound bed, ulcer with a red pink wound bed, without slough. May also present as without slough. May also present as an intact or open/ruptured serum- an intact or open/ruptured serum- fi lled blister. fi lled blister. Stage 3: Full thickness tissue loss. Stage 3: Full thickness tissue loss. Subcutaneous fat may be visible but Subcutaneous fat may be visible but bone, tendon or muscle are not exposed. -

Penetrating Injury to the Head: Case Reviews K Regunath, S Awang*, S B Siti, M R Premananda, W M Tan, R H Haron**
CASE REPORT Penetrating Injury to the Head: Case Reviews K Regunath, S Awang*, S B Siti, M R Premananda, W M Tan, R H Haron** *Department of Neurosciences, Universiti Sains Malaysia, 16150 Kubang Kerian, Kelantan, **Department of Neurosurgery, Hospital Kuala Lumpur the right frontal lobe to a depth of approximately 2.5cm. SUMMARY (Figure 1: A & B) There was no obvious intracranial Penetrating injury to the head is considered a form of severe haemorrhage along the track of injury. The patient was taken traumatic brain injury. Although uncommon, most to the operating theatre and was put under general neurosurgical centres would have experienced treating anaesthesia. The nail was cut proximal to the entry wound patients with such an injury. Despite the presence of well and the piece of wood removed. The entry wound was found written guidelines for managing these cases, surgical to be contaminated with hair and debris. The nail was also treatment requires an individualized approach tailored to rusty. A bicoronal skin incision was fashioned centred on the the situation at hand. We describe a collection of three cases entry wound. A bifrontal craniotomy was fashioned and the of non-missile penetrating head injury which were managed bone flap removed sparing a small island of bone around the in two main Neurosurgical centres within Malaysia and the nail (Figure 1: C&D). Bilateral “U” shaped dural incisions unique management approaches for each of these cases. were made with the base to the midline. The nail was found to have penetrated with dura about 0.5cm from the edge of KEY WORDS: Penetrating head injury, nail related injury, atypical penetrating the sagittal sinus. -

The Care of a Patient with Fournier's Gangrene
CASE REPORT The care of a patient with Fournier’s gangrene Esma Özşaker, Asst. Prof.,1 Meryem Yavuz, Prof.,1 Yasemin Altınbaş, MSc.,1 Burçak Şahin Köze, MSc.,1 Birgül Nurülke, MSc.2 1Department of Surgical Nursing, Ege University Faculty of Nursing, Izmir; 2Department of Urology, Ege University Faculty of Medicine Hospital, Izmir ABSTRACT Fournier’s gangrene is a rare, necrotizing fasciitis of the genitals and perineum caused by a mixture of aerobic and anaerobic microor- ganisms. This infection leads to complications including multiple organ failure and death. Due to the aggressive nature of this condition, early diagnosis is crucial. Treatment involves extensive soft tissue debridement and broad-spectrum antibiotics. Despite appropriate therapy, mortality is high. This case report aimed to present nursing approaches towards an elderly male patient referred to the urology service with a diagnosis of Fournier’s gangrene. Key words: Case report; Fournier’s gangrene; nursing diagnosis; patient care. INTRODUCTION Rarely observed in the peritoneum, genital and perianal re- perineal and genital regions, it is observed in a majority of gions, necrotizing fasciitis is named as Fournier’s gangrene.[1-5] cases with general symptoms, such as fever related infection It is an important disease, following an extremely insidious and weakness, and without symptoms in the perineal region, beginning and causing necrosis of the scrotum and penis by negatively influencing the prognosis by causing a delay in diag- advancing rapidly within one-two days.[1] The rate of mortal- nosis and treatment.[2,3] Consequently, anamnesis and physical ity in the literature is between 4 and 75%[6] and it has been examination are extremely important. -

What Everyone Should Know to Stop Bleeding After an Injury
What Everyone Should Know to Stop Bleeding After an Injury THE HARTFORD CONSENSUS The Joint Committee to Increase Survival from Active Shooter and Intentional Mass Casualty Events was convened by the American College of Surgeons in response to the growing number and severity of these events. The committee met in Hartford Connecticut and has produced a number of documents with rec- ommendations. The documents represent the consensus opinion of a multi-dis- ciplinary committee involving medical groups, the military, the National Security Council, Homeland Security, the FBI, law enforcement, fire rescue, and EMS. These recommendations have become known as the Hartford Consensus. The overarching principle of the Hartford Consensus is that no one should die from uncontrolled bleeding. The Hartford Consensus recommends that all citizens learn to stop bleeding. Further information about the Hartford Consensus and bleeding control can be found on the website: Bleedingcontrol.org 2 SAVE A LIFE: What Everyone Should Know to Stop Bleeding After an Injury Authors: Peter T. Pons, MD, FACEP Lenworth Jacobs, MD, MPH, FACS Acknowledgements: The authors acknowledge the contributions of Michael Cohen and James “Brooks” Hart, CMI to the design of this manual. Some images adapted from Adam Wehrle, EMT-P and NAEMT. © 2017 American College of Surgeons CONTENTS SECTION 1 3 ■ Introduction ■ Primary Principles of Trauma Care Response ■ The ABCs of Bleeding SECTION 2 5 ■ Ensure Your Own Safety SECTION 3 6 ■ A – Alert – call 9-1-1 SECTION 4 7 ■ B – Bleeding – find the bleeding injury SECTION 5 9 ■ C – Compress – apply pressure to stop the bleeding by: ■ Covering the wound with a clean cloth and applying pressure by pushing directly on it with both hands, OR ■Using a tourniquet, OR ■ Packing (stuff) the wound with gauze or a clean cloth and then applying pressure with both hands SECTION 6 13 ■ Summary 2 SECTION 1: INTRODUCTION Welcome to the Stop the Bleed: Bleeding Control for the Injured information booklet. -

Arthroscopic Versus Open Debridement of Penetrating Knee Joint Injuries
ARTHROSCOPIC VERSUS OPEN DEBRIDEMENT OF PENETRATING KNEE JOINT INJURIES John R. Raskind, M.D.* Richard A. Marder, M.D. ABSTRACT included in this study. The group treated with arthroscopic Arthroscopic debridement of penetrating knee joint debridement consisted of seven motor vehicle "dash- injuries has become a common treatment method. A board" injuries, five motorcycle/moped/bicycle injuries and comparative study was undertaken to compare this two low velocity gun shot wounds. The mean wound size method with open joint debridement. Fourteen penetrat- in this group was 3.8 centimeters (cms) (range one to ing knee joint injuries (fourteen patients) were treated by twelve cms) and the mean patient age was 26.6 (range arthroscopic examination and debridement and were com- nine to fifty-twelve years). The open debridement group pared to sixteen penetrating knee joint injuries (fifteen consisted of eight motor vehicle "dashboard" injuries, five patients) treated by open debridement. There were no motorcycle/moped injuries, one low velocity gunshot resultant infections or operative complications in either wound, one weed-trimmer laceration, and one power-saw group. Of note, the arthroscopic debridement group had a laceration. The mean wound size in this group was 4.6 cms shorter postoperative hospital stay [mean of 1.6 days (range one to twelve cms) and the mean patient age was compared to a mean of 2.6 days in the open debridement 26.9 years (range fifteen to forty-three years). group (p < 0.02)], a significant incidence of additional Diagnosis was based upon examination of the wound, intra-articular injuries detected (p < 0.01), less postoper- AP, lateral, and notch radiographic views of the knee, and ative pain, and a superior cosmetic result. -

Test Your CPT Coding Knowledge for Penetrating Trauma
CODING AND PRACTICE MANAGEMENT CORNER Test your CPT coding knowledge for penetrating trauma by Jayme Lieberman, MD, FACS; Christopher Senkowski, MD, FACS; Charles Mabry, MD, FACS; and Jan Nagle, MS revious Bulletin articles thigh level. The emergency of all wounds, the tourniquet have provided Current medical service providers had is let down and hemostasis is PProcedural Terminology applied a tourniquet in the field, obtained. A 100 sq cm negative (CPT)* coding guidance for reducing the bleeding from the pressure dressing is placed on trauma cases, including: “Coding stump of the leg. The surgeon the amputated leg stump. At the for damage-control surgery”† and arrives at the ED and performs end of the operation, the patient “Effectively using E/M codes for the primary and secondary is maintained on a ventilator trauma care.”‡ This article presents Advanced Trauma Life Support® with ongoing resuscitation and is several clinical scenarios involving (ATLS®) surveys, an abdominal transferred to the intensive care penetrating trauma and challenges and retroperitoneal focused unit (ICU). (See Table 2, page 47.) 46 | the reader’s coding knowledge assessment with sonography for for each example provided. trauma (FAST) exam, and exams Postoperative work in the ICU of the patient’s leg. The surgeon Later the same day in ICU, the orders administration of blood, surgeon examines the patient Trauma Scenario 1 antibiotics, and fluids based on and orders a blood transfusion, the examination, vital signs, and adjusts intravenous (IV) fluids Initial work in ED available labs. It is determined that to stabilize electrolytes/ A 25-year-old male involved in the partially severed leg, which coagulopathy, titrates the an accident related to a tractor’s was mangled by the tractor, is ventilator settings, and orders power take-off mechanism arrives unsalvageable. -

Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations from the Prehospital Trauma Life Support Executive Committee
REVIEW ARTICLE Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations From the Prehospital Trauma Life Support Executive Committee Lance E. Stuke, MD, MPH, Peter T. Pons, MD, Jeffrey S. Guy, MD, MSc, MMHC, Will P. Chapleau, RN, EMT-P, Frank K. Butler, MD, Capt MC USN (Ret), and Norman E. McSwain, MD pine immobilization in trauma patients suspected of hav- In the case of penetrating injuries, delays in transport Sing a spinal injury has been a cornerstone of prehospital prolong the time before patients receive the prompt surgical treatment for decades. Current practices are based on the care needed to arrest hemorrhage. Even with experienced belief that a patient with an injured spinal column can prehospital providers, spine immobilization is time consum- deteriorate neurologically without immobilization. Most ing. The time required for experienced emergency medical treatment protocols do not differentiate between blunt and technicians to properly immobilize a cervical spine has been penetrating mechanisms of injury. Current Emergency Med- reported to be 5.64 minutes (Ϯ1.49 minutes).6 This scene ical Service (EMS) protocols for spinal immobilization of delay can be catastrophic for a patient with penetrating penetrating trauma are based on historic practices rather than trauma requiring urgent surgical intervention for airway com- scientific merits. Although blunt spinal column injuries will promise or hemorrhage. Studies have demonstrated that cervical collars increase occasionally produce unstable vertebral