Scleritis‑Related Endophthalmitis in a University Hospital in Thailand
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
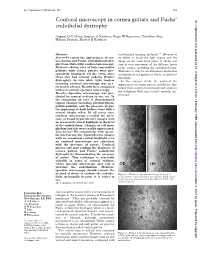
Confocal Microscopy in Cornea Guttata and Fuchs' Endothelial Dystrophy
Br J Ophthalmol 1999;83:185–189 185 Confocal microscopy in cornea guttata and Fuchs’ Br J Ophthalmol: first published as 10.1136/bjo.83.2.185 on 1 February 1999. Downloaded from endothelial dystrophy Auguste G-Y Chiou, Stephen C Kaufman, Roger W Beuerman, Toshihiko Ohta, Hisham Soliman, Herbert E Kaufman Abstract conventional imaging methods.3–13 Because of Aims—To report the appearances of cor- its ability to focus the light source and the nea guttata and Fuchs’ endothelial dystro- image on the same focal plane, it allows real phy from white light confocal microscopy. time in vivo assessment of the diVerent layers Methods—Seven eyes of four consecutive of the cornea, including the endothelial layer. patients with cornea guttata were pro- Therefore, it may be an alternative method in spectively examined. Of the seven eyes, evaluating cornea guttata or Fuchs’ endothelial three also had corneal oedema (Fuchs’ dystrophy. dystrophy). In vivo white light tandem In the current study, we analysed the scanning confocal microscopy was per- appearances of cornea guttata and Fuchs’ dys- formed in all eyes. Results were compared trophy from confocal microscopy and compare with non-contact specular microscopy. the technique with non-contact specular mi- Results—Specular microscopy was pre- croscopy. cluded by corneal oedema in one eye. In the remaining six eyes, it demonstrated typical changes including pleomorphism, polymegathism, and the presence of gut- tae appearing as dark bodies, some with a central bright reflex. In all seven eyes, confocal microscopy revealed the pres- ence of round hyporeflective images with an occasional central highlight at the level of the endothelium. -

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

Onchocerciasis
11 ONCHOCERCIASIS ADRIAN HOPKINS AND BOAKYE A. BOATIN 11.1 INTRODUCTION the infection is actually much reduced and elimination of transmission in some areas has been achieved. Differences Onchocerciasis (or river blindness) is a parasitic disease in the vectors in different regions of Africa, and differences in cause by the filarial worm, Onchocerca volvulus. Man is the the parasite between its savannah and forest forms led to only known animal reservoir. The vector is a small black fly different presentations of the disease in different areas. of the Simulium species. The black fly breeds in well- It is probable that the disease in the Americas was brought oxygenated water and is therefore mostly associated with across from Africa by infected people during the slave trade rivers where there is fast-flowing water, broken up by catar- and found different Simulium flies, but ones still able to acts or vegetation. All populations are exposed if they live transmit the disease (3). Around 500,000 people were at risk near the breeding sites and the clinical signs of the disease in the Americas in 13 different foci, although the disease has are related to the amount of exposure and the length of time recently been eliminated from some of these foci, and there is the population is exposed. In areas of high prevalence first an ambitious target of eliminating the transmission of the signs are in the skin, with chronic itching leading to infection disease in the Americas by 2012. and chronic skin changes. Blindness begins slowly with Host factors may also play a major role in the severe skin increasingly impaired vision often leading to total loss of form of the disease called Sowda, which is found mostly in vision in young adults, in their early thirties, when they northern Sudan and in Yemen. -

Diagnosing, Treating, and Managing Scleritis in 2020 an Expert Panel Recommendation Panel Members Melissa Toyos, Md Stephen D
DIAGNOSING, TREATING, AND MANAGING SCLERITIS IN 2020 AN EXPERT PANEL RECOMMENDATION PANEL MEMBERS MELISSA TOYOS, MD STEPHEN D. ANESI, MD, FACS n Partner and Director of Research n Massachusetts Eye Research & Surgery Institution n Toyos Clinic n Waltham, MA n Nashville, TN DAVID S. CHU, MD n Medical Director, Metropolitan Eye Research THOMAS A. ALBINI, MD & Surgery Institute n Professor of Clinical Ophthalmology n Associate Professor of Clinical Ophthalmology n University of Miami Health n Rutgers University n Bascom Palmer Eye Institute n Newark, NJ n Miami, FL ROBERT C. WANG, MD n Texas Retina Associates n Dallas, TX Corresponding Author: Melissa Toyos, MD; Toyos Clinic, Nashville, TN; [email protected]. This work was supported by an unrestricted medical writing grant from Mallinckrodt Pharmaceuticals and is based on a virtual roundtable discussion hosted by Evolve Medical Education LLC. Although uncommon, scleritis is a dangerous immune-me- DIAGNOSING SCLERITIS diated disease that can potentially threaten the structural Melissa Toyos, MD: What percentage of patients in integrity of the eye and may be indicative of potentially your practice have scleritis? life-threatening systemic vasculitis.1,2 Data on the genetic factors of scleritis is lacking, but it is thought that genes affect- Stephen D. Anesi, MD, FACS: Scleritis accounts for 10% ing systemic autoimmune diseases impact scleritis as well.2 to 15% of the patients I see in my practice. Differentiating between episcleritis and scleritis and posterior and anterior scleritis can be challenging for physicians. An David S. Chu, MD: I agree; 10% to 15% sounds right to accurate diagnosis is critical to properly treat the disease and me as well. -

Preseptal and Orbital Cellulitis
Journal of Microbiology and Infectious Diseases / 2014; 4 (3): 123-127 JMID doi: 10.5799/ahinjs.02.2014.03.0154 REVIEW ARTICLE Preseptal and orbital cellulitis Emine Akçay, Gamze Dereli Can, Nurullah Çağıl Yıldırım Beyazıt Univ. Medical Faculty Atatürk Training and Research Hospital Dept. of Ophthalmology, Ankara, Turkey ABSTRACT Preseptal cellulitis (PC) is defined as an inflammation of the eyelid and surrounding skin, whereas orbital cellulitis (OC) is an inflammation of the posterior septum of the eyelid affecting the orbit and its contents. Periorbital tissues may become infected as a result of trauma (including insect bites) or primary bacteremia. Orbital cellulitis generally occurs as a complication of sinusitis. The most commonly isolated organisms are Staphylococcus aureus, Streptococcus pneu- moniae, S. epidermidis, Haempphilus influenzae, Moraxella catarrhalis and S. pyogenes. The method for the diagnosis of OS and PS is computed tomography. Using effective antibiotics is a mainstay for the treatment of PC and OC. There is an agreement that surgical drainage should be performed in cases of complete ophthalmoplegia or significant visual impairment or large abscesses formation. This infections are also at a greater risk of acute visual loss, cavernous sinus thrombosis, meningitis, cerebritis, endo- phthalmitis, and brain abscess in children. Early diagnosis and appropriate treatment are crucial to control the infection. Diagnosis, treatment, management and complications of PC and OC are summarized in this manuscript. J Microbiol Infect Dis 2014; 4(3): 123-127 Key words: infection, cellulitis, orbita, preseptal, diagnosis, treatment Preseptal ve Orbital Sellülit ÖZET Preseptal selülit (PS) göz kapağı ve çevresindeki dokunun iltihabi reaksiyonu iken orbital selülit (OS) orbitayı ve onun içeriğini etkileyen septum arkası dokuların iltihabıdır. -

Acute Keratoconus-Like Corneal Hydrops Secondary to Ocular
perim Ex en l & ta a l ic O p in l h Journal of Clinical & Experimental t C h f a o l m l a o Ke et al., J Clin Exp Ophthalmol 2017, 8:6 n l o r g u y o Ophthalmology J DOI: 10.4172/2155-9570.1000694 ISSN: 2155-9570 Case Report Open Access Acute Keratoconus-Like Corneal Hydrops Secondary to Ocular Massage Following Trabeculectomy Hongmin Ke, Chengguo Zuo and Mingkai Lin* State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, 54 Xianlie Nan Road, Guangzhou, China *Corresponding author: Mingkai Lin, State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, 54 Xianlie Nan Road, Guangzhou, China, 510060, E- mail: [email protected] Received date: November 13, 2017; Accepted date: November 21, 2017; Published date: November 23, 2017 Copyright: © 2017 Ke H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Purpose: To report a case of acute keratoconus-like corneal hydrops in a patient with long-term ocular massage following trabeculectomy. Methods: Case report and review of medical literature. Results: A rare complication of acute keratoconus-like corneal hydrops occurred in a patient following the use of ocular massage to maintain satisfactory aqueous humor filtration after trabeculectomy. The patient had a history of high myopia but denied previous ocular trauma, allergic disease and a family history of keratoconus. Slit-lamp examination demonstrated keratoconus-like corneal hydrops with formation of epithelial microcystic, and intrastromal cleft. -

CAUSES, COMPLICATIONS &TREATMENT of A“RED EYE”
CAUSES, COMPLICATIONS & TREATMENT of a “RED EYE” 8 Most cases of “red eye” seen in general practice are likely to be conjunctivitis or a superficial corneal injury, however, red eye can also indicate a serious eye condition such as acute angle glaucoma, iritis, keratitis or scleritis. Features such as significant pain, photophobia, reduced visual acuity and a unilateral presentation are “red flags” that a sight-threatening condition may be present. In the absence of specialised eye examination equipment, such as a slit lamp, General Practitioners must rely on identifying these key features to know which patients require referral to an Ophthalmologist for further assessment. Is it conjunctivitis or is it something more Iritis is also known as anterior uveitis; posterior uveitis is serious? inflammation of the choroid (choroiditis). Complications include glaucoma, cataract and macular oedema. The most likely cause of a red eye in patients who present to 4. Scleritis is inflammation of the sclera. This is a very rare general practice is conjunctivitis. However, red eye can also be presentation, usually associated with autoimmune a feature of a more serious eye condition, in which a delay in disease, e.g. rheumatoid arthritis. treatment due to a missed diagnosis can result in permanent 5. Penetrating eye injury or embedded foreign body; red visual loss. In addition, the inappropriate use of antibacterial eye is not always a feature topical eye preparations contributes to antimicrobial 6. Acid or alkali burn to the eye resistance. The patient history will usually identify a penetrating eye injury Most general practice clinics will not have access to specialised or chemical burn to the eye, but further assessment may be equipment for eye examination, e.g. -

Fusarium Keratitis and Corneal Collagen Cross
FUSARIUM KERATITIS AND SURGERY REFRACTIVE CORNEAL COLLAGEN CROSS-LINKING BY MINAS CORONEO, AO, BSC(MED), MBBS, MSC SYD, MD, MS, UNSW, FRACS, FRANZCO; RAJESH FOGLA, DNB, FRCS(EDIN), MMED(OPHTH); WILLIAM B. TRATTLER, MD; ASHIYANA NARIANI, MD, MPH; COMPLEX CASE MANAGEMENT COMPLEX GARGI KHARE VORA, MD; AND ALAN N. CARLSON, MD CASE PRESENTATION A 42-year-old white man is referred to the Duke University Eye Center Cornea Service for a central corneal ulcer with a hypopyon in his right eye. The patient sustained the ocular injury while mowing the lawn, with debris getting into the eye while he was wearing contact lenses. He was diagnosed with culture-positive Fusarium species by the referring ophthalmologist and was treat- ed with oral voriconazole 200 mg twice daily and frequent topical natamycin 5% and voriconazole 10 mg/mL. The patient under- went epithelium-off corneal collagen cross-linking (CXL) approxi- Figure 1. Initial evaluation of the eye with a Fusarium corneal mately 4 weeks after diagnosis of the ulcer and was treated with infiltrate and hypopyon. a loteprednol steroid taper after the procedure. His condition subsequently progressed, with increasing eye pain, a nonhealing epithelial defect, and a worsening corneal infiltrate. Upon evaluation, the patient has a large corneal infiltrate with necrotic stroma, which is approaching the limbus, and a hypopyon (Figure 1). His UCVA measures 20/70-1. B-scan ultrasound of the right eye shows no evidence of posterior segment involvement. Reculturing of the corneal infiltrate is negative for bacteria, fungus, and Acanthamoeba. Confocal microscopy reveals no evidence of hyphae or cysts. -

Immune Defense at the Ocular Surface
Eye (2003) 17, 949–956 & 2003 Nature Publishing Group All rights reserved 0950-222X/03 $25.00 www.nature.com/eye Immune defense at EK Akpek and JD Gottsch CAMBRIDGE OPHTHALMOLOGICAL SYMPOSIUM the ocular surface Abstract vertebrates. Improved visual acuity would have increased the fitness of these animals and would The ocular surface is constantly exposed to a have outweighed the disadvantage of having wide array of microorganisms. The ability of local immune cells and blood vessels at a the outer ocular system to recognize pathogens distance where a time delay in addressing a as foreign and eliminate them is critical to central corneal infection could lead to blindness. retain corneal transparency, hence The first vertebrates were jawless fish that preservation of sight. Therefore, a were believed to have evolved some 470 million combination of mechanical, anatomical, and years ago.1 These creatures had frontal eyes and immunological defense mechanisms has inhabited the shorelines of ancient oceans. With evolved to protect the outer eye. These host better vision, these creatures were likely more defense mechanisms are classified as either a active and predatory. This advantage along with native, nonspecific defense or a specifically the later development of jaws enabled bony fish acquired immunological defense requiring to flourish and establish other habitats. One previous exposure to an antigen and the such habitat was shallow waters where lunged development of specific immunity. Sight- fish made the transition to land several hundred threatening immunopathology with thousand years later.2 To become established in autologous cell damage also can take place this terrestrial environment, the new vertebrates after these reactions. -

Treatment of Interface Keratitis with Oral Corticosteroids
Treatment of interface keratitis with oral corticosteroids Scott M. MacRae, MD, Larry F. Rich, MD, Damien C. Macaluso, MD ABSTRACT Purpose: To describe the results of treating interface keratitis using a combination of intensive topical and oral corticosteroids. Setting: Casey Eye Institute, Portland, Oregon, USA. Methods: Thirteen eyes treated for grade 2 to 3 interface keratitis using an oral cortico- steroid (prednisone 60 to 80 mg) as well as an hourly topical corticosteroid were retrospectively reviewed. The best corrected visual acuity (BCVA) was used as an objective guide of whether to treat with intense topical and oral corticosteroids, flap irrigation, or both. Predisposing factors such as intraoperative epithelial defects or a history of severe allergies or atopy were also looked for. Results: All 13 eyes responded favorably to the combination of intensive topical and oral corticosteroids and had a BCVA of 20/20 after the keratitis resolved. In 6 eyes (46%), the patients had a history of severe seasonal allergies. One day postoperatively, 3 eyes (23%) had an epithelial defect and 2 eyes (15%), lint particles or debris embedded in the interface. With oral corticosteroid use, 3 patients (23%) noted mild stomach irritation and 2 (15%) noted nervousness. All 5 side effects resolved without sequelae. No patient developed a serious side effect. Conclusion: A short, intense course of an oral corticosteroid was an effective treatment in patients with grade 2 or higher interface keratitis when combined with a topical corti- costeroid administered hourly. The BCVA is a helpful objective measure of the severity of interface keratitis and can be used to guide the clinician in the therapeutic strategy. -

Frequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, Karachi
Biostatistics and Biometrics Open Access Journal ISSN: 2573-2633 Research Article Biostat Biometrics Open Acc J Faisal’s Issue - January 2018 Copyright © All rights are reserved by Muhammad Faisal Fahim DOI: 10.19080/BBOAJ.2018.04.555639 Frequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, Karachi Shaheerah Gul1, Adil Salim Jafri1, Muhammad Faisal Fahim2* 1Department of Ophthalmology, Al-Ibrahim Eye Hospital, Pakistan 2Department of Research & Development, Al-Ibrahim Eye Hospital, Pakistan Submission: November 27, 2017; Published: January 19, 2018 *Corresponding author: Muhammad Faisal Fahim, M.Sc (Statistics), Statistician, Research & Development Department, Al-Ibrahim Eye Hospital, Isra postgraduate Institute of Ophthalmology, Karachi, Pakistan, Tel: ; Email: Abstract Objective: To determine frequency and risk factors of symptomatic dry eye disease at tertiary care eye hospital, Karachi. Material & Methods: This was a descriptive cross sectional study carried out at Al-Ibrahim Eye Hospital, Isra postgraduate Institute of Oph- thalmology, Karachi from March to October 2016. Non-Probability purposive sampling technique was used for data collection. Inclusion criteria give consent. Symptoms of dry eye were assessed using Tear breakup test (TBUT) test. SPSS version 20.0 was used to analyze data. were patients aged ≥ 21 years and on the basis of dry eye symptoms. Exclusion criteria were other systemic eye disease and those who did not Results: A total of 100 patients 65 female and 35 male were diagnosed with dry eye syndrome. The age group of 21-30 years having the high- est frequency of 34 patients, whereas after the 50 years of age the frequency of patients decreases to 21. -

Reactive Uveitis, Retinal Vasculitis and Scleritis As Ocular End-Stage of Acanthamoeba Keratitis: a Histological Study
Uveitis and vasculitis of Acanthamoeba keratitis ·Brief Report· Reactive uveitis, retinal vasculitis and scleritis as ocular end-stage of Acanthamoeba keratitis: a histological study Lei Shi1,2, Tobias Hager1, Fabian Norbert Fries1, Loay Daas1, Leonard Holbach3, Carmen Hofmann- Rummelt3, Elena Zemova1, Berthold Seitz1, Nóra Szentmáry1,4 1Department of Ophthalmology, Saarland University Medical wearers. Its annual incidence was 17.53 to 21.14 per one Center, Homburg/Saar 66424, Germany million contact lens wearers in the UK[1]. In Germany, with 2Department of Ophthalmology, The First Affiliated Hospital about 80 million inhabitants, about 150 new cases have been of USTC, Division of Life Sciences and Medicine, University reported in a 10-year-period[2]. Studies showed that 68%-92.3% of Science and Technology of China, Hefei 230001, Anhui of AK patients are contact lens wearers[1,3-4]. Expression of Province, P.R. China mannosilated glycoproteins on corneal epithelial cell surface is 3Department of Ophthalmology, Friedrich-Alexander upregulated in contact lens wearers[3]. This plays an important University Erlangen-Nürnberg, Erlangen 91052, Germany role in AK pathogenesis. The Acanthamoeba trophozoite binds 4Department of Ophthalmology, Semmelweis University, to these proteins though its mannose-binding site in order to Budapest 1093, Hungary release the so-called mannose-induced protease 133 (MIP-133) Correspondence to: Lei Shi. Department of Ophthalmology, and Acanthamoeba plasminogen activator (aPA). MIP-133 and Saarland University Medical Center, Homburg/Saar, Kirrberger aPA give rise to lysis of epithelial, stromal cells and stromal Str. 100. 66424, Germany. [email protected] matrix, leading to corneal erosions and ulceration[4]. Presence Received: 2019-05-01 Accepted: 2019-08-21 of bacteria or fungi also supports Acanthamoeba growth, often resulting in co-infection[5].