NCCN Guidelines for Patients Brain Cancer: Gliomas
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1
[CANCER RESEARCH 49, 6137-6143. November 1, 1989] Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1 Susan Preston-Martin,2 Wendy Mack, and Brian E. Henderson Department of Preventive Medicine, University of Southern California School of Medicine, Los Angeles, California 90033 ABSTRACT views with proxy respondents, we were unable to include a large proportion of otherwise eligible cases because they were deceased or Detailed job histories and information about other suspected risk were too ill or impaired to participate in an interview. The Los Angeles factors were obtained during interviews with 272 men aged 25-69 with a County Cancer Surveillance Program identified the cases (26). All primary brain tumor first diagnosed during 1980-1984 and with 272 diagnoses had been microscopically confirmed. individually matched neighbor controls. Separate analyses were con A total of 478 patients were identified. The hospital and attending ducted for the 202 glioma pairs and the 70 meningioma pairs. Meningi- physician granted us permission to contact 396 (83%) patients. We oma, but not glioma, was related to having a serious head injury 20 or were unable to locate 22 patients, 38 chose not to participate, and 60 more years before diagnosis (odds ratio (OR) = 2.3; 95% confidence were aphasie or too ill to complete the interview. We interviewed 277 interval (CI) = 1.1-5.4), and a clear dose-response effect was observed patients (74% of the 374 patients contacted about the study or 58% of relating meningioma risk to number of serious head injuries (/' for trend the initial 478 patients). -

Brain Tumors
BRAIN TUMORS What kinds of brain tumors affect pets? Brain tumors occur relatively often in dogs and cats. The most common type of brain tumor is a meningioma, which originates from the layer surrounding the brain, called the meninges. Meningiomas are slow-growing benign tumors that are often present for months to years before clinical signs appear. Other common types in- clude glial cell tumors, which originate in the brain tissue, and choroid plexus tumors, which originate from the tissue in the brain that produces spinal fluid. Tumors in structures around the brain (like nasal tumors, skull tumors, and pituitary tumors) may also com- press the brain. Lymphoma is a type of cancer that can affect multiple parts of the brain and spine. What are the symptoms? Symptoms vary and depend on the size and location of the tumor. Common signs include changes in behavior, circling or pacing, staring into space, getting stuck in corners, and seizures. Other signs can include weakness, lack of alertness, difficulty eating or swallowing, and problems with the “vestibular system,” or system of bal- ance, such as lack of coordination, head tilt, leaning/circling/falling to one side, and abnormal eye movements. How are brain tumors diagnosed? An MRI scan produces an image of the brain that’s more detailed than a CT scan or x-ray and can identify a tumor. Often the appearance of the tumor on MRI suggests the type of tumor (i.e. meningioma vs lymphoma). However, a biopsy of the tumor is required to give a definitive diagnosis. In some cases, spinal fluid is collected to help diagnose lymphoma. -

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -

Neuro-Oncology
Neuro-Oncology Neuro-Oncology 17:iv1–iv62, 2015. doi:10.1093/neuonc/nov189 CBTRUS Statistical Report: Primary Brain and Central Nervous System Tumors Diagnosed in the United States in 2008-2012 Quinn T. Ostrom M.A., M.P.H.1,2*, Haley Gittleman M.S.1,2*, Jordonna Fulop R.N.1, Max Liu3, Rachel Blanda4, Courtney Kromer B.A.5, Yingli Wolinsky Ph.D., M.B.A.1,2, Carol Kruchko B.A.2, and Jill S. Barnholtz-Sloan Ph.D.1,2 1Case Comprehensive Cancer Center, Case Western Reserve University School of Medicine, Cleveland, OH USA 2Central Brain Tumor Registry of the United States, Hinsdale, IL USA 3Solon High School, Solon, OH USA 4Georgetown University, Washington D.C. USA 5Case Western Reserve University School of Medicine, Cleveland, OH USA *Contributed equally to this Report. Introduction for collection of central (state) cancer data as mandated in 1992 by Public Law 102-515, the Cancer Registries Amendment The objective of the CBTRUS Statistical Report: Primary Brain and Act.2 This mandate was expanded to include non-malignant Central Nervous System Tumors Diagnosed in the United States brain tumors diagnosed in 2004 and later with the 2002 in 2008-2012 is to provide a comprehensive summary of the passage of Public Law 107–260.3 CBTRUS researchers combine current descriptive epidemiology of primary brain and central the NPCR data with data from the SEER program4 of the NCI, nervous system (CNS) tumors in the United States (US) popula- which was established for national cancer surveillance in the tion. CBTRUS obtained the latest available data on all newly early 1970s. -

The Use of Rodent Tumors in Experimental Cancer Therapy Conclusions and Recommendations from an International Workshop1'2
[CANCER RESEARCH 45, 6541-6545, December 1985] Meeting Report The Use of Rodent Tumors in Experimental Cancer Therapy Conclusions and Recommendations from an International Workshop1'2 This workshop was convened to address the question of how of a specific tumor cannot be predicted with any certainty. Virus- best to use animal models of solid tumors in cancer therapy induced rodent tumors almost always express common virus- research. The discussion among the 58 participants focused on coded antigens and are usually strongly immunogenic, but hosts the following topics: appropriate solid tumor models; xenografts neonatally infected with virus may be immunologically tolerant to of human tumors; assay systems such as local tumor control, virus-coded antigens. Chemically induced rodent tumors tend to clonogenic assays following tumor excision, and tumor regrowth express individually distinct antigens. Depending partially upon delay; and applications of such models in chemotherapy, radio the carcinogen and the target organ, the degree of immunoge therapy, and combined modalities studies. nicity is variable, but a large proportion of chemically induced A major goal of the meeting was to produce a set of guiding tumors are immunogenic. Spontaneous rodent tumors are usu principles for experiments on animal tumors. This report is largely ally nonimmunogenic, although a minority may be weakly to a statement of those guiding principles, with suggestions and moderately immunogenic (1, 2). comments concerning investigations using animal models in Because no tumor can be expected to be nonimmunogenic if cancer therapy research.3 The authors believe that this discus it is placed in an allogeneic environment, tumors should as a sion of "tricks of the trade" will be useful to research workers general rule only be transplanted syngeneically. -

Radiotherapy: Seizing the Opportunity in Cancer Care
RADIOTHERAPY: seizing the opportunity in cancer care November 2018 Foreword The incidence of cancer is increasing, resulting in a rising demand for high‑quality cancer care. In 2018, there were close to 4.23 million new cases of cancer in Europe, and this number is predicted to rise by almost a quarter to 5.2 million by 2040.1 This growing demand poses a major challenge to healthcare systems and highlights the need to ensure all cancer patients have access to high-quality, efficient cancer care. One critical component of cancer care is too often forgotten in these discussions: radiotherapy. Radiotherapy is recommended as part of treatment for more than 50% of cancer patients.2 3 However, at least one in four people needing radiotherapy does not receive it.3 This report aims to demonstrate the significant role of radiotherapy in achieving high‑quality cancer care and highlights what needs to be done to close the current gap in utilisation of radiotherapy across Europe. We call on all stakeholders, with policymakers at the helm, to help position radiotherapy appropriately within cancer policies and models of care – for the benefit of cancer patients today and tomorrow. 2 1 Governments and policymakers: Make radiotherapy a central component of cancer care in policies, planning and budgets Our 5 2 Patient groups, media five-point Professional societies working and other stakeholders: Help with national and EU‑level improve general awareness and plan decision‑makers: Achieve understanding of radiotherapy recognition of all radiotherapy to -

Cerebellar Anaplastic Astrocytoma in Adult Patients: 15 Consecutive Cases from a Single Institution and Literature Review
medRxiv preprint doi: https://doi.org/10.1101/2020.09.09.20188938; this version posted September 14, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted medRxiv a license to display the preprint in perpetuity. All rights reserved. No reuse allowed without permission. Cerebellar anaplastic astrocytoma in adult patients: 15 consecutive cases from a single institution and literature review Artem Belyaev1, Dmitry Usachev1, Marina Ryzhova1, Gleb Gulida1, Vasilisa Skvortsova2,3, Igor Pronin1, Grigory Kobiakov1. 1 Burdenko Neurosurgery Center, 4th Tverskaya-Yamskaya, 16, Moscow, 125047, Russia 2 Wellcome Trust Centre for Neuroimaging, University College London, London, United Kingdom; 3 Max Planck University College London Centre for Computational Psychiatry and Ageing Research, London, United Kingdom; Abstract: Adult cerebellar anaplastic astrocytomas (cAA) are rare entities and their clinical and genetic appearances are still ill defined. Previously, malignant gliomas of the cerebellum were combined and reviewed together (cAA and cerebellar glioblastomas (cGB), that could have possibly affected overall results. We present characteristics of 15 adult patients with cAA and compared them to a series of 45 patients with a supratentorial AA (sAA). The mean age at cAA diagnosis was 39.3 years (range 19-72). A history of neurofibromatosis type I was noted in 1 patient (6.7%). An IDH-1 mutation was identified in 6/15 cases and a methylated MGMT promoter in 5/15 cases. Patients in study and control groups were matched in age, sex and IDH- 1 mutation status. Patients in a study group tended to have a more frequent multifocal presentation at diagnosis (13% vs. -

The Future of Cancer Research: ACCELERATING SCIENTIFIC INNOVATION
The Future Of Cancer Research: ACCELERATING SCIENTIFIC INNOVATION President’s Cancer Panel Annual Report 2010-2011 U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Cancer Institute The President’s Cancer Panel LaSalle D. Leffall, Jr., M.D., F.A.C.S., Chair (through 12/31/11) Charles R. Drew Professor of Surgery Howard University College of Medicine Washington, DC 20059 Margaret L. Kripke, Ph.D. (through 12/31/11) Vivian L. Smith Chair and This report is submitted to the President of the United States Professor Emerita in fulfillment of the obligations of the President’s Cancer Panel The University of Texas to appraise the National Cancer Program as established in MD Anderson Cancer Center accordance with the National Cancer Act of 1971 (P.L. 92-218), Houston, TX 77030 the Health Research Extension Act of 1987 (P.L. 99-158), the National Institutes of Health Revitalization Act of 1993 (P.L. 103-43), and Title V, Part A, Public Health Service Act (42 U.S.C. 281 et seq.). Printed November 2012 For further information on the President’s Cancer Panel or additional copies of this report, please contact: Abby B. Sandler, Ph.D. Executive Secretary President’s Cancer Panel 9000 Rockville Pike Bld. 31/Rm B2B37 MSC 2590 Bethesda, MD 20892 301-451-9399 [email protected] http://pcp.cancer.gov The Future Of Cancer Research:: ACCELERATING SCIENTIFIC INNOVATION President’s Cancer Panel Annual Report 2010-2011 Suzanne H. Reuben Erin L. Milliken Lisa J. Paradis for The President’s Cancer Panel November 2012 U.S. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
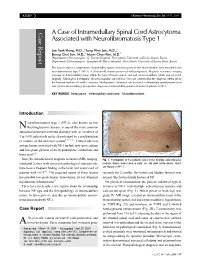
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Cancer Treatment and Survivorship Facts & Figures 2019-2021
Cancer Treatment & Survivorship Facts & Figures 2019-2021 Estimated Numbers of Cancer Survivors by State as of January 1, 2019 WA 386,540 NH MT VT 84,080 ME ND 95,540 59,970 38,430 34,360 OR MN 213,620 300,980 MA ID 434,230 77,860 SD WI NY 42,810 313,370 1,105,550 WY MI 33,310 RI 570,760 67,900 IA PA NE CT 243,410 NV 185,720 771,120 108,500 OH 132,950 NJ 543,190 UT IL IN 581,350 115,840 651,810 296,940 DE 55,460 CA CO WV 225,470 1,888,480 KS 117,070 VA MO MD 275,420 151,950 408,060 300,200 KY 254,780 DC 18,750 NC TN 470,120 AZ OK 326,530 NM 207,260 AR 392,530 111,620 SC 143,320 280,890 GA AL MS 446,900 135,260 244,320 TX 1,140,170 LA 232,100 AK 36,550 FL 1,482,090 US 16,920,370 HI 84,960 States estimates do not sum to US total due to rounding. Source: Surveillance Research Program, Division of Cancer Control and Population Sciences, National Cancer Institute. Contents Introduction 1 Long-term Survivorship 24 Who Are Cancer Survivors? 1 Quality of Life 24 How Many People Have a History of Cancer? 2 Financial Hardship among Cancer Survivors 26 Cancer Treatment and Common Side Effects 4 Regaining and Improving Health through Healthy Behaviors 26 Cancer Survival and Access to Care 5 Concerns of Caregivers and Families 28 Selected Cancers 6 The Future of Cancer Survivorship in Breast (Female) 6 the United States 28 Cancers in Children and Adolescents 9 The American Cancer Society 30 Colon and Rectum 10 How the American Cancer Society Saves Lives 30 Leukemia and Lymphoma 12 Research 34 Lung and Bronchus 15 Advocacy 34 Melanoma of the Skin 16 Prostate 16 Sources of Statistics 36 Testis 17 References 37 Thyroid 19 Acknowledgments 45 Urinary Bladder 19 Uterine Corpus 21 Navigating the Cancer Experience: Treatment and Supportive Care 22 Making Decisions about Cancer Care 22 Cancer Rehabilitation 22 Psychosocial Care 23 Palliative Care 23 Transitioning to Long-term Survivorship 23 This publication attempts to summarize current scientific information about Global Headquarters: American Cancer Society Inc. -

Sporadic (Nonhereditary) Colorectal Cancer: Introduction
Sporadic (Nonhereditary) Colorectal Cancer: Introduction Colorectal cancer affects about 5% of the population, with up to 150,000 new cases per year in the United States alone. Cancer of the large intestine accounts for 21% of all cancers in the US, ranking second only to lung cancer in mortality in both males and females. It is, however, one of the most potentially curable of gastrointestinal cancers. Colorectal cancer is detected through screening procedures or when the patient presents with symptoms. Screening is vital to prevention and should be a part of routine care for adults over the age of 50 who are at average risk. High-risk individuals (those with previous colon cancer , family history of colon cancer , inflammatory bowel disease, or history of colorectal polyps) require careful follow-up. There is great variability in the worldwide incidence and mortality rates. Industrialized nations appear to have the greatest risk while most developing nations have lower rates. Unfortunately, this incidence is on the increase. North America, Western Europe, Australia and New Zealand have high rates for colorectal neoplasms (Figure 2). Figure 1. Location of the colon in the body. Figure 2. Geographic distribution of sporadic colon cancer . Symptoms Colorectal cancer does not usually produce symptoms early in the disease process. Symptoms are dependent upon the site of the primary tumor. Cancers of the proximal colon tend to grow larger than those of the left colon and rectum before they produce symptoms. Abnormal vasculature and trauma from the fecal stream may result in bleeding as the tumor expands in the intestinal lumen.