Genomic Landscape and Mutational Spectrum of ADAMTS Family Genes in Mendelian Disorders Based on Gene Evidence Review for Variant Interpretation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Evolution of Biomolecular Structure Class II Trna-Synthetases and Trna
University of Illinois at Urbana-Champaign Luthey-Schulten Group Theoretical and Computational Biophysics Group Evolution of Biomolecular Structure Class II tRNA-Synthetases and tRNA MultiSeq Developers: Prof. Zan Luthey-Schulten Elijah Roberts Patrick O’Donoghue John Eargle Anurag Sethi Dan Wright Brijeet Dhaliwal September 25, 2006. A current version of this tutorial is available at http://www.scs.uiuc.edu/˜schulten/tutorials/evolution/ CONTENTS 2 Contents 1 Introduction 4 1.1 The MultiSeq Bioinformatic Analysis Environment . 4 1.2 Aminoacyl-tRNA Synthetases: Role in translation . 4 1.3 Getting Started . 7 1.3.1 Requirements . 7 1.3.2 Copying the tutorial files . 7 1.3.3 Configuring MultiSeq . 7 1.3.4 Configuring BLAST for MultiSeq . 10 1.4 The Aspartyl-tRNA Synthetase/tRNA Complex . 12 1.4.1 Loading the structure into MultiSeq . 12 1.4.2 Selecting and highlighting residues . 13 1.4.3 Domain organization of the synthetase . 14 1.4.4 Nearest neighbor contacts . 14 2 Evolutionary Analysis of AARS Structures 17 2.1 Loading Molecules . 17 2.2 Multiple Structure Alignments . 18 2.3 Structural Conservation Measure: Qres . 19 2.4 Structure Based Phylogenetic Analysis . 21 2.4.1 Limitations of sequence data . 21 2.4.2 Structural metrics look further back in time . 23 3 Complete Evolutionary Profile of AspRS 26 3.1 BLASTing Sequence Databases . 26 3.1.1 Importing the archaeal sequences . 26 3.1.2 Now the other domains of life . 27 3.2 Organizing Your Data . 28 3.3 Finding a Structural Domain in a Sequence . 29 3.4 Aligning to a Structural Profile using ClustalW . -

Polymorphisms of the BARX1 and ADAMTS17 Locus Genes in Individuals with Gastroesophageal Reflux Disease
J Neurogastroenterol Motil, Vol. 25 No. 3 July, 2019 pISSN: 2093-0879 eISSN: 2093-0887 https://doi.org/10.5056/jnm18183 JNM Journal of Neurogastroenterology and Motility Original Article Polymorphisms of the BARX1 and ADAMTS17 Locus Genes in Individuals With Gastroesophageal Reflux Disease Alexandra Argyrou,1 Evangelia Legaki,1 Christos Koutserimpas,2 Maria Gazouli,1* Ioannis Papaconstantinou,3 George Gkiokas,3 and George Karamanolis4 1Department of Basic Medical Sciences, Laboratory of Biology, School of Medicine, National and Kapodistrian University of Athens, Athens, Greece; 22nd Department of General Surgery, “Sismanoglio General Hospital of Athens, Athens, Greece; 32nd Department of Surgery, School of Medicine, National and Kapodistrian University of Athens, Athens, Greece; and 4Gastroenterology Unit, 2nd Department of Surgery, School of Medicine, National and Kapodistrian University of Athens, Athens, Greece Background/Aims Gastroesophageal reflux disease (GERD) represents a common condition having a substantial impact on the patients’ quality of life, as well as the health system. According to many studies, the BARX1 and ADAMTS17 genes have been suggested as genetic risk loci for the development of GERD and its complications. The purpose of this study is to investigate the potential association between GERD and BARX1 and ADAMTS17 polymorphisms. Methods The present is a prospective cohort study of 160 GERD patients and 180 healthy control subjects of Greek origin, examined for BARX1 and ADAMTS17 polymorphisms (rs11789015 and rs4965272) and a potential correlation to GERD. Results The rs11789015 AG and GG genotypes were found to be significantly associated with GERD (P = 0.032; OR, 1.65; 95% CI, 1.06- 2.57 and P = 0.033; OR, 3.00; 95% CI, 1.15-7.82, respectively), as well as the G allele (P = 0.007; OR, 1.60; 95% CI, 1.14- 2.24). -

The Architecture of the Protein Domain Universe
The architecture of the protein domain universe Nikolay V. Dokholyan Department of Biochemistry and Biophysics, The University of North Carolina at Chapel Hill, School of Medicine, Chapel Hill, NC 27599 ABSTRACT Understanding the design of the universe of protein structures may provide insights into protein evolution. We study the architecture of the protein domain universe, which has been found to poses peculiar scale-free properties (Dokholyan et al., Proc. Natl. Acad. Sci. USA 99: 14132-14136 (2002)). We examine the origin of these scale-free properties of the graph of protein domain structures (PDUG) and determine that that the PDUG is not modular, i.e. it does not consist of modules with uniform properties. Instead, we find the PDUG to be self-similar at all scales. We further characterize the PDUG architecture by studying the properties of the hub nodes that are responsible for the scale-free connectivity of the PDUG. We introduce a measure of the betweenness centrality of protein domains in the PDUG and find a power-law distribution of the betweenness centrality values. The scale-free distribution of hubs in the protein universe suggests that a set of specific statistical mechanics models, such as the self-organized criticality model, can potentially identify the principal driving forces of molecular evolution. We also find a gatekeeper protein domain, removal of which partitions the largest cluster into two large sub- clusters. We suggest that the loss of such gatekeeper protein domains in the course of evolution is responsible for the creation of new fold families. INTRODUCTION The principles of molecular evolution remain elusive despite fundamental breakthroughs on the theoretical front 1-5 and a growing amount of genomic and proteomic data, over 23,000 solved protein structures 6 and protein functional annotations 7-9. -
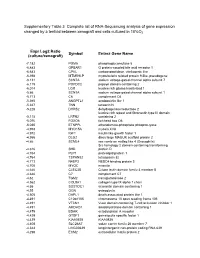

Supplementary Table 3 Complete List of RNA-Sequencing Analysis of Gene Expression Changed by ≥ Tenfold Between Xenograft and Cells Cultured in 10%O2
Supplementary Table 3 Complete list of RNA-Sequencing analysis of gene expression changed by ≥ tenfold between xenograft and cells cultured in 10%O2 Expr Log2 Ratio Symbol Entrez Gene Name (culture/xenograft) -7.182 PGM5 phosphoglucomutase 5 -6.883 GPBAR1 G protein-coupled bile acid receptor 1 -6.683 CPVL carboxypeptidase, vitellogenic like -6.398 MTMR9LP myotubularin related protein 9-like, pseudogene -6.131 SCN7A sodium voltage-gated channel alpha subunit 7 -6.115 POPDC2 popeye domain containing 2 -6.014 LGI1 leucine rich glioma inactivated 1 -5.86 SCN1A sodium voltage-gated channel alpha subunit 1 -5.713 C6 complement C6 -5.365 ANGPTL1 angiopoietin like 1 -5.327 TNN tenascin N -5.228 DHRS2 dehydrogenase/reductase 2 leucine rich repeat and fibronectin type III domain -5.115 LRFN2 containing 2 -5.076 FOXO6 forkhead box O6 -5.035 ETNPPL ethanolamine-phosphate phospho-lyase -4.993 MYO15A myosin XVA -4.972 IGF1 insulin like growth factor 1 -4.956 DLG2 discs large MAGUK scaffold protein 2 -4.86 SCML4 sex comb on midleg like 4 (Drosophila) Src homology 2 domain containing transforming -4.816 SHD protein D -4.764 PLP1 proteolipid protein 1 -4.764 TSPAN32 tetraspanin 32 -4.713 N4BP3 NEDD4 binding protein 3 -4.705 MYOC myocilin -4.646 CLEC3B C-type lectin domain family 3 member B -4.646 C7 complement C7 -4.62 TGM2 transglutaminase 2 -4.562 COL9A1 collagen type IX alpha 1 chain -4.55 SOSTDC1 sclerostin domain containing 1 -4.55 OGN osteoglycin -4.505 DAPL1 death associated protein like 1 -4.491 C10orf105 chromosome 10 open reading frame 105 -4.491 -

Sequence Analysis of Familial Neurodevelopmental Disorders
SEQUENCE ANALYSIS OF FAMILIAL NEURODEVELOPMENTAL DISORDERS by Joseph Mark Tilghman A dissertation submitted to Johns Hopkins University in conformity with the requirements for the degree of Doctor of Philosophy Baltimore, Maryland December 2020 © 2020 Joseph Tilghman All Rights Reserved Abstract: In the practice of human genetics, there is a gulf between the study of Mendelian and complex inheritance. When diagnosis of families affected by presumed monogenic syndromes is undertaken by genomic sequencing, these families are typically considered to have been solved only when a single gene or variant showing apparently Mendelian inheritance is discovered. However, about half of such families remain unexplained through this approach. On the other hand, common regulatory variants conferring low risk of disease still predominate our understanding of individual disease risk in complex disorders, despite rapidly increasing access to rare variant genotypes through sequencing. This dissertation utilizes primarily exome sequencing across several developmental disorders (having different levels of genetic complexity) to investigate how to best use an individual’s combination of rare and common variants to explain genetic risk, phenotypic heterogeneity, and the molecular bases of disorders ranging from those presumed to be monogenic to those known to be highly complex. The study described in Chapter 2 addresses putatively monogenic syndromes, where we used exome sequencing of four probands having syndromic neurodevelopmental disorders from an Israeli-Arab founder population to diagnose recessive and dominant disorders, highlighting the need to consider diverse modes of inheritance and phenotypic heterogeneity. In the study described in Chapter 3, we address the case of a relatively tractable multifactorial disorder, Hirschsprung disease. -

Documentation and Localization of Force-Mediated Filamin a Domain
ARTICLE Received 29 May 2014 | Accepted 10 Jul 2014 | Published 14 Aug 2014 DOI: 10.1038/ncomms5656 Documentation and localization of force-mediated filamin A domain perturbations in moving cells Fumihiko Nakamura1, Mia Song1, John H. Hartwig1 & Thomas P. Stossel1 Endogenously and externally generated mechanical forces influence diverse cellular activities, a phenomenon defined as mechanotransduction. Deformation of protein domains by application of stress, previously documented to alter macromolecular interactions in vitro, could mediate these effects. We engineered a photon-emitting system responsive to unfolding of two repeat domains of the actin filament (F-actin) crosslinker protein filamin A (FLNA) that binds multiple partners involved in cell signalling reactions and validated the system using F-actin networks subjected to myosin-based contraction. Expressed in cultured cells, the sensor-containing FLNA construct reproducibly reported FLNA domain unfolding strikingly localized to dynamic, actively protruding, leading cell edges. The unfolding signal depends upon coherence of F-actin-FLNA networks and is enhanced by stimulating cell contractility. The results establish protein domain distortion as a bona fide mechanism for mechanotransduction in vivo. 1 Translational Medicine Division, Department of Medicine, Brigham and Women’s Hospital, Harvard Medical School, Boston, Massachusetts 02445, USA. Correspondence and requests for materials should be addressed to F.N. (email: [email protected]). NATURE COMMUNICATIONS | 5:4656 | DOI: 10.1038/ncomms5656 -

Lipid-Targeting Pleckstrin Homology Domain Turns Its Autoinhibitory Face Toward the TEC Kinases
Lipid-targeting pleckstrin homology domain turns its autoinhibitory face toward the TEC kinases Neha Amatyaa, Thomas E. Walesb, Annie Kwonc, Wayland Yeungc, Raji E. Josepha, D. Bruce Fultona, Natarajan Kannanc, John R. Engenb, and Amy H. Andreottia,1 aRoy J. Carver Department of Biochemistry, Biophysics and Molecular Biology, Iowa State University, Ames, IA 50011; bDepartment of Chemistry and Chemical Biology, Northeastern University, Boston, MA 02115; and cInstitute of Bioinformatics and Department of Biochemistry and Molecular Biology, University of Georgia, Athens, GA 30602 Edited by Natalie G. Ahn, University of Colorado Boulder, Boulder, CO, and approved September 17, 2019 (received for review May 3, 2019) The pleckstrin homology (PH) domain is well known for its phos- activation loop phosphorylation site are also controlled by noncatalytic pholipid targeting function. The PH-TEC homology (PHTH) domain domains (17). In addition to the N-terminal PHTH domain, the within the TEC family of tyrosine kinases is also a crucial component TEC kinases contain a proline-rich region (PRR) and Src ho- of the autoinhibitory apparatus. The autoinhibitory surface on the mology 3 (SH3) and Src homology 2 (SH2) domains that impinge PHTH domain has been previously defined, and biochemical investi- on the kinase domain to alter the conformational ensemble and gations have shown that PHTH-mediated inhibition is mutually thus the activation status of the enzyme. A crystal structure of the exclusive with phosphatidylinositol binding. Here we use hydrogen/ BTK SH3-SH2-kinase fragment has been solved (10) showing that deuterium exchange mass spectrometry, nuclear magnetic resonance the SH3 and SH2 domains of BTK assemble onto the distal side of (NMR), and evolutionary sequence comparisons to map where and the kinase domain (the surface opposite the activation loop), how the PHTH domain affects the Bruton’s tyrosine kinase (BTK) stabilizing the autoinhibited form of the kinase in a manner similar domain. -

Systematic Data-Querying of Large Pediatric Biorepository Identifies Novel Ehlers-Danlos Syndrome Variant Akshatha Desai1, John J
Desai et al. BMC Musculoskeletal Disorders (2016) 17:80 DOI 10.1186/s12891-016-0936-8 RESEARCH ARTICLE Open Access Systematic data-querying of large pediatric biorepository identifies novel Ehlers-Danlos Syndrome variant Akshatha Desai1, John J. Connolly1, Michael March1, Cuiping Hou1, Rosetta Chiavacci1, Cecilia Kim1, Gholson Lyon1, Dexter Hadley1 and Hakon Hakonarson1,2* Abstract Background: Ehlers Danlos Syndrome is a rare form of inherited connective tissue disorder, which primarily affects skin, joints, muscle, and blood cells. The current study aimed at finding the mutation that causing EDS type VII C also known as “Dermatosparaxis” in this family. Methods: Through systematic data querying of the electronic medical records (EMRs) of over 80,000 individuals, we recently identified an EDS family that indicate an autosomal dominant inheritance. The family was consented for genomic analysis of their de-identified data. After a negative screen for known mutations, we performed whole genome sequencing on the male proband, his affected father, and unaffected mother. We filtered the list of non- synonymous variants that are common between the affected individuals. Results: The analysis of non-synonymous variants lead to identifying a novel mutation in the ADAMTSL2 (p. Gly421Ser) gene in the affected individuals. Sanger sequencing confirmed the mutation. Conclusion: Our work is significant not only because it sheds new light on the pathophysiology of EDS for the affected family and the field at large, but also because it demonstrates the utility of unbiased large-scale clinical recruitment in deciphering the genetic etiology of rare mendelian diseases. With unbiased large-scale clinical recruitment we strive to sequence as many rare mendelian diseases as possible, and this work in EDS serves as a successful proof of concept to that effect. -

Supplementary Table 1: Adhesion Genes Data Set
Supplementary Table 1: Adhesion genes data set PROBE Entrez Gene ID Celera Gene ID Gene_Symbol Gene_Name 160832 1 hCG201364.3 A1BG alpha-1-B glycoprotein 223658 1 hCG201364.3 A1BG alpha-1-B glycoprotein 212988 102 hCG40040.3 ADAM10 ADAM metallopeptidase domain 10 133411 4185 hCG28232.2 ADAM11 ADAM metallopeptidase domain 11 110695 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 195222 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 165344 8751 hCG20021.3 ADAM15 ADAM metallopeptidase domain 15 (metargidin) 189065 6868 null ADAM17 ADAM metallopeptidase domain 17 (tumor necrosis factor, alpha, converting enzyme) 108119 8728 hCG15398.4 ADAM19 ADAM metallopeptidase domain 19 (meltrin beta) 117763 8748 hCG20675.3 ADAM20 ADAM metallopeptidase domain 20 126448 8747 hCG1785634.2 ADAM21 ADAM metallopeptidase domain 21 208981 8747 hCG1785634.2|hCG2042897 ADAM21 ADAM metallopeptidase domain 21 180903 53616 hCG17212.4 ADAM22 ADAM metallopeptidase domain 22 177272 8745 hCG1811623.1 ADAM23 ADAM metallopeptidase domain 23 102384 10863 hCG1818505.1 ADAM28 ADAM metallopeptidase domain 28 119968 11086 hCG1786734.2 ADAM29 ADAM metallopeptidase domain 29 205542 11085 hCG1997196.1 ADAM30 ADAM metallopeptidase domain 30 148417 80332 hCG39255.4 ADAM33 ADAM metallopeptidase domain 33 140492 8756 hCG1789002.2 ADAM7 ADAM metallopeptidase domain 7 122603 101 hCG1816947.1 ADAM8 ADAM metallopeptidase domain 8 183965 8754 hCG1996391 ADAM9 ADAM metallopeptidase domain 9 (meltrin gamma) 129974 27299 hCG15447.3 ADAMDEC1 ADAM-like, -

A Genome-Wide Association Study Identifies Four Novel Susceptibility Loci Underlying Inguinal Hernia
UCSF UC San Francisco Previously Published Works Title A genome-wide association study identifies four novel susceptibility loci underlying inguinal hernia. Permalink https://escholarship.org/uc/item/7g06z1k5 Journal Nature communications, 6(1) ISSN 2041-1723 Authors Jorgenson, Eric Makki, Nadja Shen, Ling et al. Publication Date 2015-12-21 DOI 10.1038/ncomms10130 Peer reviewed eScholarship.org Powered by the California Digital Library University of California ARTICLE Received 24 Aug 2015 | Accepted 6 Nov 2015 | Published 21 Dec 2015 DOI: 10.1038/ncomms10130 OPEN A genome-wide association study identifies four novel susceptibility loci underlying inguinal hernia Eric Jorgenson1,*, Nadja Makki2,3,*, Ling Shen1, David C. Chen4, Chao Tian5, Walter L. Eckalbar2,3, David Hinds5, Nadav Ahituv2,3 & Andrew Avins1 Inguinal hernia repair is one of the most commonly performed operations in the world, yet little is known about the genetic mechanisms that predispose individuals to develop inguinal hernias. We perform a genome-wide association analysis of surgically confirmed inguinal hernias in 72,805 subjects (5,295 cases and 67,510 controls) and confirm top associations in an independent cohort of 92,444 subjects with self-reported hernia repair surgeries (9,701 cases and 82,743 controls). We identify four novel inguinal hernia susceptibility loci in the regions of EFEMP1, WT1, EBF2 and ADAMTS6. Moreover, we observe expression of all four genes in mouse connective tissue and network analyses show an important role for two of these genes (EFEMP1 and WT1) in connective tissue maintenance/homoeostasis. Our findings provide insight into the aetiology of hernia development and highlight genetic pathways for studies of hernia development and its treatment. -
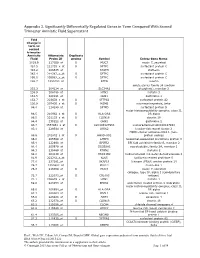
Appendix 2. Significantly Differentially Regulated Genes in Term Compared with Second Trimester Amniotic Fluid Supernatant
Appendix 2. Significantly Differentially Regulated Genes in Term Compared With Second Trimester Amniotic Fluid Supernatant Fold Change in term vs second trimester Amniotic Affymetrix Duplicate Fluid Probe ID probes Symbol Entrez Gene Name 1019.9 217059_at D MUC7 mucin 7, secreted 424.5 211735_x_at D SFTPC surfactant protein C 416.2 206835_at STATH statherin 363.4 214387_x_at D SFTPC surfactant protein C 295.5 205982_x_at D SFTPC surfactant protein C 288.7 1553454_at RPTN repetin solute carrier family 34 (sodium 251.3 204124_at SLC34A2 phosphate), member 2 238.9 206786_at HTN3 histatin 3 161.5 220191_at GKN1 gastrokine 1 152.7 223678_s_at D SFTPA2 surfactant protein A2 130.9 207430_s_at D MSMB microseminoprotein, beta- 99.0 214199_at SFTPD surfactant protein D major histocompatibility complex, class II, 96.5 210982_s_at D HLA-DRA DR alpha 96.5 221133_s_at D CLDN18 claudin 18 94.4 238222_at GKN2 gastrokine 2 93.7 1557961_s_at D LOC100127983 uncharacterized LOC100127983 93.1 229584_at LRRK2 leucine-rich repeat kinase 2 HOXD cluster antisense RNA 1 (non- 88.6 242042_s_at D HOXD-AS1 protein coding) 86.0 205569_at LAMP3 lysosomal-associated membrane protein 3 85.4 232698_at BPIFB2 BPI fold containing family B, member 2 84.4 205979_at SCGB2A1 secretoglobin, family 2A, member 1 84.3 230469_at RTKN2 rhotekin 2 82.2 204130_at HSD11B2 hydroxysteroid (11-beta) dehydrogenase 2 81.9 222242_s_at KLK5 kallikrein-related peptidase 5 77.0 237281_at AKAP14 A kinase (PRKA) anchor protein 14 76.7 1553602_at MUCL1 mucin-like 1 76.3 216359_at D MUC7 mucin 7, -

Proteolytic Activation Defines Distinct Lymphangiogenic Mechanisms for VEGFC and VEGFD
Proteolytic activation defines distinct lymphangiogenic mechanisms for VEGFC and VEGFD Hung M. Bui, … , Kari Alitalo, Mark L. Kahn J Clin Invest. 2016;126(6):2167-2180. https://doi.org/10.1172/JCI83967. Research Article Vascular biology Lymphangiogenesis is supported by 2 homologous VEGFR3 ligands, VEGFC and VEGFD. VEGFC is required for lymphatic development, while VEGFD is not. VEGFC and VEGFD are proteolytically cleaved after cell secretion in vitro, and recent studies have implicated the protease a disintegrin and metalloproteinase with thrombospondin motifs 3 (ADAMTS3) and the secreted factor collagen and calcium binding EGF domains 1 (CCBE1) in this process. It is not well understood how ligand proteolysis is controlled at the molecular level or how this process regulates lymphangiogenesis, because these complex molecular interactions have been difficult to follow ex vivo and test in vivo. Here, we have developed and used biochemical and cellular tools to demonstrate that an ADAMTS3-CCBE1 complex can form independently of VEGFR3 and is required to convert VEGFC, but not VEGFD, into an active ligand. Consistent with these ex vivo findings, mouse genetic studies revealed that ADAMTS3 is required for lymphatic development in a manner that is identical to the requirement of VEGFC and CCBE1 for lymphatic development. Moreover, CCBE1 was required for in vivo lymphangiogenesis stimulated by VEGFC but not VEGFD. Together, these studies reveal that lymphangiogenesis is regulated by two distinct proteolytic mechanisms of ligand activation: one in which VEGFC activation by ADAMTS3 and CCBE1 spatially and temporally patterns developing lymphatics, and one in which VEGFD activation by a distinct […] Find the latest version: https://jci.me/83967/pdf The Journal of Clinical Investigation RESEARCH ARTICLE Proteolytic activation defines distinct lymphangiogenic mechanisms for VEGFC and VEGFD Hung M.