Full Disclosure Forms
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Systemic Restoration of UBA1 Ameliorates Disease in Spinal Muscular Atrophy
Systemic restoration of UBA1 ameliorates disease in spinal muscular atrophy Rachael A. Powis, … , Mimoun Azzouz, Thomas H. Gillingwater JCI Insight. 2016;1(11):e87908. https://doi.org/10.1172/jci.insight.87908. Research Article Neuroscience Therapeutics The autosomal recessive neuromuscular disease spinal muscular atrophy (SMA) is caused by loss of survival motor neuron (SMN) protein. Molecular pathways that are disrupted downstream of SMN therefore represent potentially attractive therapeutic targets for SMA. Here, we demonstrate that therapeutic targeting of ubiquitin pathways disrupted as a consequence of SMN depletion, by increasing levels of one key ubiquitination enzyme (ubiquitin-like modifier activating enzyme 1 [UBA1]), represents a viable approach for treating SMA. Loss of UBA1 was a conserved response across mouse and zebrafish models of SMA as well as in patient induced pluripotent stem cell–derive motor neurons. Restoration of UBA1 was sufficient to rescue motor axon pathology and restore motor performance in SMA zebrafish. Adeno- associated virus serotype 9–UBA1 (AAV9-UBA1) gene therapy delivered systemic increases in UBA1 protein levels that were well tolerated over a prolonged period in healthy control mice. Systemic restoration of UBA1 in SMA mice ameliorated weight loss, increased survival and motor performance, and improved neuromuscular and organ pathology. AAV9-UBA1 therapy was also sufficient to reverse the widespread molecular perturbations in ubiquitin homeostasis that occur during SMA. We conclude that UBA1 represents a safe and effective therapeutic target for the treatment of both neuromuscular and systemic aspects of SMA. Find the latest version: https://jci.me/87908/pdf RESEARCH ARTICLE Systemic restoration of UBA1 ameliorates disease in spinal muscular atrophy Rachael A. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

Mitochondrial Heat Shock Protein 60: Evaluation of Its Role As a Neuroprotectant in Familial ALS and Its Mutation As a Cause of Hereditary Spastic Paraplegia
Mitochondrial Heat Shock Protein 60: Evaluation of its role as a neuroprotectant in familial ALS and its mutation as a cause of hereditary spastic paraplegia By Laura A. Cooper Integrated Program in Neuroscience McGill University, Montreal June 2011 A thesis submitted to McGill University in partial fulfillment of the requirements of the degree of master’s in science © Laura A. Cooper, 2011 TABLE OF CONTENTS ABSTRACT…………………………………………………………………………….vi RÉSUMÉ……………………………………………………………………………….viii ACKNOWLEDGMENTS……………………………………………………………..xi LIST OF FIGURES……………………………………………………………………xiii ABBREVIATIONS………………………………………………………………….....xv INTRODUCTION……………………………………………………………………..xx CHAPTER 1 – Literature Review 1.1 Amyotrophic Lateral Sclerosis 1.1.1 Clinical Overview..................................................................................................1 1.1.2 Sporadic ALS…………………………………………………………………….2 1.1.3 Familial ALS……………………………………………………………………..4 1.1.4 Cu/Zn Superoxide Dismutase Mutation and fALS……………………………….4 1.1.5 Protein Aggregation in SOD1-Related fALS…………………………………….5 1.1.6 Mitochondrial Abnormalities in Mouse Models of SOD1-Related fALS………..7 1.1.7 Relationship Between Mutant SOD1 and Mitochondrial Abnormalities………..8 1.2 Heat Shock Proteins 1.2.1 Normal Function in the Central Nervous System and Relevance to ALS……….9 1.2.2 Heat Shock Proteins as a Therapeutic Target in ALS………………………….10 1.3 Mitochondrial Heat Shock Protein Hsp60 1.3.1 Structure and Function………………………………………………………....12 ii 1.3.2 Mitochondrial Hsp60 in Neuroprotection……………………………………. -
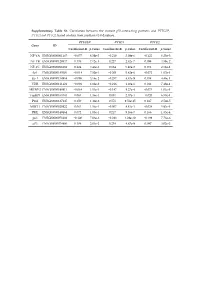
Supplementary Table S1. Correlation Between the Mutant P53-Interacting Partners and PTTG3P, PTTG1 and PTTG2, Based on Data from Starbase V3.0 Database
Supplementary Table S1. Correlation between the mutant p53-interacting partners and PTTG3P, PTTG1 and PTTG2, based on data from StarBase v3.0 database. PTTG3P PTTG1 PTTG2 Gene ID Coefficient-R p-value Coefficient-R p-value Coefficient-R p-value NF-YA ENSG00000001167 −0.077 8.59e-2 −0.210 2.09e-6 −0.122 6.23e-3 NF-YB ENSG00000120837 0.176 7.12e-5 0.227 2.82e-7 0.094 3.59e-2 NF-YC ENSG00000066136 0.124 5.45e-3 0.124 5.40e-3 0.051 2.51e-1 Sp1 ENSG00000185591 −0.014 7.50e-1 −0.201 5.82e-6 −0.072 1.07e-1 Ets-1 ENSG00000134954 −0.096 3.14e-2 −0.257 4.83e-9 0.034 4.46e-1 VDR ENSG00000111424 −0.091 4.10e-2 −0.216 1.03e-6 0.014 7.48e-1 SREBP-2 ENSG00000198911 −0.064 1.53e-1 −0.147 9.27e-4 −0.073 1.01e-1 TopBP1 ENSG00000163781 0.067 1.36e-1 0.051 2.57e-1 −0.020 6.57e-1 Pin1 ENSG00000127445 0.250 1.40e-8 0.571 9.56e-45 0.187 2.52e-5 MRE11 ENSG00000020922 0.063 1.56e-1 −0.007 8.81e-1 −0.024 5.93e-1 PML ENSG00000140464 0.072 1.05e-1 0.217 9.36e-7 0.166 1.85e-4 p63 ENSG00000073282 −0.120 7.04e-3 −0.283 1.08e-10 −0.198 7.71e-6 p73 ENSG00000078900 0.104 2.03e-2 0.258 4.67e-9 0.097 3.02e-2 Supplementary Table S2. -

The Ubiquitin Proteasome System in Neuromuscular Disorders: Moving Beyond Movement
International Journal of Molecular Sciences Review The Ubiquitin Proteasome System in Neuromuscular Disorders: Moving Beyond Movement 1, , 2, 3,4 Sara Bachiller * y , Isabel M. Alonso-Bellido y , Luis Miguel Real , Eva María Pérez-Villegas 5 , José Luis Venero 2 , Tomas Deierborg 1 , José Ángel Armengol 5 and Rocío Ruiz 2 1 Experimental Neuroinflammation Laboratory, Department of Experimental Medical Science, Lund University, Sölvegatan 19, 221 84 Lund, Sweden; [email protected] 2 Departamento de Bioquímica y Biología Molecular, Facultad de Farmacia, Universidad de Sevilla/Instituto de Biomedicina de Sevilla-Hospital Universitario Virgen del Rocío/CSIC/Universidad de Sevilla, 41012 Sevilla, Spain; [email protected] (I.M.A.-B.); [email protected] (J.L.V.); [email protected] (R.R.) 3 Unidad Clínica de Enfermedades Infecciosas, Hospital Universitario de Valme, 41014 Sevilla, Spain; [email protected] 4 Departamento de Especialidades Quirúrgicas, Bioquímica e Inmunología, Facultad de Medicina, 29071 Universidad de Málaga, Spain 5 Departamento de Fisiología, Anatomía y Biología Celular, Universidad Pablo de Olavide, 41013 Sevilla, Spain; [email protected] (E.M.P.-V.); [email protected] (J.Á.A.) * Correspondence: [email protected] These authors contributed equally to the work. y Received: 14 July 2020; Accepted: 31 August 2020; Published: 3 September 2020 Abstract: Neuromuscular disorders (NMDs) affect 1 in 3000 people worldwide. There are more than 150 different types of NMDs, where the common feature is the loss of muscle strength. These disorders are classified according to their neuroanatomical location, as motor neuron diseases, peripheral nerve diseases, neuromuscular junction diseases, and muscle diseases. Over the years, numerous studies have pointed to protein homeostasis as a crucial factor in the development of these fatal diseases. -

FARE2021WINNERS Sorted by Institute
FARE2021WINNERS Sorted By Institute Swati Shah Postdoctoral Fellow CC Radiology/Imaging/PET and Neuroimaging Characterization of CNS involvement in Ebola-Infected Macaques using Magnetic Resonance Imaging, 18F-FDG PET and Immunohistology The Ebola (EBOV) virus outbreak in Western Africa resulted in residual neurologic abnormalities in survivors. Many case studies detected EBOV in the CSF, suggesting that the neurologic sequelae in survivors is related to viral presence. In the periphery, EBOV infects endothelial cells and triggers a “cytokine stormâ€. However, it is unclear whether a similar process occurs in the brain, with secondary neuroinflammation, neuronal loss and blood-brain barrier (BBB) compromise, eventually leading to lasting neurological damage. We have used in vivo imaging and post-necropsy immunostaining to elucidate the CNS pathophysiology in Rhesus macaques infected with EBOV (Makona). Whole brain MRI with T1 relaxometry (pre- and post-contrast) and FDG-PET were performed to monitor the progression of disease in two cohorts of EBOV infected macaques from baseline to terminal endpoint (day 5-6). Post-necropsy, multiplex fluorescence immunohistochemical (MF-IHC) staining for various cellular markers in the thalamus and brainstem was performed. Serial blood and CSF samples were collected to assess disease progression. The linear mixed effect model was used for statistical analysis. Post-infection, we first detected EBOV in the serum (day 3) and CSF (day 4) with dramatic increases until euthanasia. The standard uptake values of FDG-PET relative to whole brain uptake (SUVr) in the midbrain, pons, and thalamus increased significantly over time (p<0.01) and positively correlated with blood viremia (p≤0.01). -

SPINAL MUSCULAR ATROPHY: PATHOLOGY, DIAGNOSIS, CLINICAL PRESENTATION, THERAPEUTIC STRATEGIES & TREATMENTS Content
SPINAL MUSCULAR ATROPHY: PATHOLOGY, DIAGNOSIS, CLINICAL PRESENTATION, THERAPEUTIC STRATEGIES & TREATMENTS Content 1. DISCLAIMER 2. INTRODUCTION 3. SPINAL MUSCULAR ATROPHY: PATHOLOGY, DIAGNOSIS, CLINICAL PRESENTATION, THERAPEUTIC STRATEGIES & TREATMENTS 4. BIBLIOGRAPHY 5. GLOSSARY OF MEDICAL TERMS 1 SPINAL MUSCULAR ATROPHY: PATHOLOGY, DIAGNOSIS, CLINICAL PRESENTATION, THERAPEUTIC STRATEGIES & TREATMENTS Disclaimer The information in this document is provided for information purposes only. It does not constitute advice on any medical, legal, or regulatory matters and should not be used in place of consultation with appropriate medical, legal, or regulatory personnel. Receipt or use of this document does not create a relationship between the recipient or user and SMA Europe, or any other third party. The information included in this document is presented as a synopsis, may not be exhaustive and is dated November 2020. As such, it may no longer be current. Guidance from regulatory authorities, study sponsors, and institutional review boards should be obtained before taking action based on the information provided in this document. This document was prepared by SMA Europe. SMA Europe cannot guarantee that it will meet requirements or be error-free. The users and recipients of this document take on any risk when using the information contained herein. SMA Europe is an umbrella organisation, founded in 2006, which includes spinal muscular atrophy (SMA) patient and research organisations from across Europe. SMA Europe campaigns to improve the quality of life of people who live with SMA, to bring effective therapies to patients in a timely and sustainable way, and to encourage optimal patient care. SMA Europe is a non-profit umbrella organisation that consists of 23 SMA patients and research organisations from 22 countries across Europe. -

Supplementary Material Contents
Supplementary Material Contents Immune modulating proteins identified from exosomal samples.....................................................................2 Figure S1: Overlap between exosomal and soluble proteomes.................................................................................... 4 Bacterial strains:..............................................................................................................................................4 Figure S2: Variability between subjects of effects of exosomes on BL21-lux growth.................................................... 5 Figure S3: Early effects of exosomes on growth of BL21 E. coli .................................................................................... 5 Figure S4: Exosomal Lysis............................................................................................................................................ 6 Figure S5: Effect of pH on exosomal action.................................................................................................................. 7 Figure S6: Effect of exosomes on growth of UPEC (pH = 6.5) suspended in exosome-depleted urine supernatant ....... 8 Effective exosomal concentration....................................................................................................................8 Figure S7: Sample constitution for luminometry experiments..................................................................................... 8 Figure S8: Determining effective concentration ......................................................................................................... -

Hnrnp C1/C2 May Regulate Exon 7 Splicing in the Spinal Muscular Atrophy Gene SMN1
Kobe J. Med. Sci., Vol. 54, No. 5, pp. E227-E236, 2008 HnRNP C1/C2 May Regulate Exon 7 Splicing in the Spinal Muscular Atrophy Gene SMN1 SANAE IRIMURA1, KEIKO KITAMURA1,2,3, NOZOMU KATO1,2,3, KAYOKO SAIKI2,3, ATSUKO TAKEUCHI3, GUNADI1, MASAFUMI MATSUO2, HISAHIDE NISHIO1,2 and MYEONG JIN LEE1,* 1Department of Genetic Epidemiology, 2Department of Pediatrics, Kobe University Graduate School of Medicine, Kobe, Japan; 3Kobe Pharmaceutical University, Kobe, Japan; Received 26 December 2008/ Accepted 28 December 2008 Key Words: Spinal muscular atrophy, Alternative pre-mRNA splicing, SMN genes, Exon 7, HnRNP C1/C2 Spinal muscular atrophy (SMA) is caused by loss of SMN1. A nearly identical gene, SMN2, fails to compensate for the loss of SMN1 because SMN2 produces mainly an exon 7-skipped product. The +6C in SMN1 exon 7 proceeds to include exon 7 into mRNA, while the +6U in SMN2 causes skipping of exon 7. Here, ∼45kD proteins bound to the SMN exon 7 RNA probe was found, and identified as hnRNP C1/C2. In gel-shift assay, hnRNP C1/C2 had a greater affinity for the RNA probe with +6C than for the RNA probe with +6U. In vitro splicing assay showed that anti-hnRNP C1/C2 antibody hampered splicing of SMN1 exon 7, but did not affect splicing of SMN2 exon 7. In conclusion, we showed the possibility that hnRNP C1/C2 enhanced SMN1 exon 7 splicing specifically. Spinal muscular atrophy (SMA) is a common autosomal recessive neuromuscular disorder that is characterized by degeneration of the anterior horn cells of the spinal cord, which leads to the axial and limb weakness associated with muscle atrophy. -
Newborn Screening for Spinal Muscular Atrophy (SMA): Phase I Update of the Evidence Review
Newborn Screening for Spinal Muscular Atrophy (SMA): Phase I Update of the Evidence Review Alex R. Kemper, MD, MPH, MS K.K. Lam, PhD Evidence Review Group Presented to the Advisory Committee on Heritable Disorders in Newborns and Children August 3, 2017 Evidence Review Group (ERG) ERG Members Role Institution Alex R. Kemper, MD, MPH, MS Chair Nationwide Children’s Hospital State NBS Public Health New England NBS Program, Anne M. Comeau, PhD Program University of Mass Medical School Department of Pediatrics, Clinical Care Expert Nancy S. Green, MD Columbia University Medical Center Scott Grosse, PhD Federal Advisor; NBS Expert CDC University of Rochester Medical Clinical Care Expert, Long-term Center, Department of Neurology Jennifer A. Kwon, MD Follow up and Pediatrics Public Health Impact Task NBS & Genetics, Jelili Ojodu, MPH Leader Association of Public Health Laboratories Decision Analysis Leader, Health Management & Policy/ SPH; Lisa Prosser, PhD NBS Health Economist Pediatrics/Univ of Michigan Med School State NBS Public Health Newborn Screening Laboratory Susan Tanksley, PhD Program TX Department of State Health Services K.K. Lam, PhD Project Leader Duke University 2 Overview: Spinal Muscular Atrophy (SMA) • Autosomal recessive disease affecting the motor neurons in the spinal cord and brainstem, resulting in progressive motor weakness and atrophy • Broad phenotype spectrum ranging in age of onset (birth to adulthood), severity, and clinical course • Estimated SMA incidence in the U.S.: • 1 in 6,000 to 1 in 11,000 (~9 - 16 in 100,000) -

Genome-Wide Identification of Mrnas Associated with the Protein SMN Whose Depletion Decreases Their Axonal Localization
Downloaded from rnajournal.cshlp.org on October 2, 2021 - Published by Cold Spring Harbor Laboratory Press Genome-wide identification of mRNAs associated with the protein SMN whose depletion decreases their axonal localization FLORENCE RAGE,1,2,3 NAWAL BOULISFANE,1,2,3 KHALIL RIHAN,1,2,3 HENRY NEEL,1,2,3,4 THIERRY GOSTAN,1,2,3 EDOUARD BERTRAND,1,2,3 RÉMY BORDONNÉ,1,2,3 and JOHANN SORET1,2,3,5 1Institut de Génétique Moléculaire de Montpellier UMR 5535, 34293 Montpellier Cedex 5, France 2Université Montpellier 2, 34095 Montpellier Cedex 5, France 3Université Montpellier 1, 34967 Montpellier Cedex 2, France ABSTRACT Spinal muscular atrophy is a neuromuscular disease resulting from mutations in the SMN1 gene, which encodes the survival motor neuron (SMN) protein. SMN is part of a large complex that is essential for the biogenesis of spliceosomal small nuclear RNPs. SMN also colocalizes with mRNAs in granules that are actively transported in neuronal processes, supporting the hypothesis that SMN is involved in axonal trafficking of mRNPs. Here, we have performed a genome-wide analysis of RNAs present in complexes containing the SMN protein and identified more than 200 mRNAs associated with SMN in differentiated NSC-34 motor neuron-like cells. Remarkably, ∼30% are described to localize in axons of different neuron types. In situ hybridization and immuno-fluorescence experiments performed on several candidates indicate that these mRNAs colocalize with the SMN protein in neurites and axons of differentiated NSC-34 cells. Moreover, they localize in cell processes in an SMN-dependent manner. Thus, low SMN levels might result in localization deficiencies of mRNAs required for axonogenesis. -

Role of Dcps in Mammalian RNA Regulation and Human Diseases
ROLE OF DCPS IN MAMMALIAN RNA REGULATION AND HUMAN DISEASES By MI ZHOU A dissertation submitted to the Graduate School-New Brunswick and The Graduate School of Biomedical Sciences Rutgers, The State University of New Jersey In partial fulfillment of the requirements For the degree of Doctor of Philosophy Graduate Program in Cell and Development Biology Written under the direction of Dr. Megerditch Kiledjian And approved by _________________________________ _________________________________ _________________________________ _________________________________ New Brunswick, New Jersey October, 2015 ABSTRACT OF THE DISSERTATION Role of DcpS in Mammalian RNA Regulation and Human Diseases By MI ZHOU Dissertation Director Dr. Megerditch Kiledjian In eukaryotic cells, mRNA degradation plays an important role in the control of gene expression and is therefore highly regulated. The scavenger decapping enzyme DcpS is a multifunctional protein that plays a critical role in mRNA degradation. We first sought to identify DcpS target genes in mammalian cells using a cell permeable DcpS inhibitor compound, RG3039, which was initially developed for therapeutic treatment of Spinal Muscular Atrophy (SMA). Microarray analysis following DcpS decapping inhibition by RG3039 revealed the steady state levels of 222 RNAs were altered. Of a subset selected for validation by qRT-PCR, two non-coding transcripts dependent on DcpS decapping activity, were identified and referred to as DcpS Responsive Noncoding Transcript (DRNT) 1 and 2 respectively. Only the increase in DRNT1 transcript was accompanied with an increase of its RNA stability and this increase was dependent on both DcpS and Xrn1. Our data indicate that DcpS is a transcript-restricted modulator of RNA stability in mammalian cells and the RG3039 ii quinazoline compound is pleotropic, influence gene expression in both an apparent DcpS dependent and independent manner.