Audiologic Evaluation in Newborns
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Septoplasty, Rhinoplasty, Septorhinoplasty, Turbinoplasty Or
Septoplasty, Rhinoplasty, Septorhinoplasty, 4 Turbinoplasty or Turbinectomy CPAP • If you have obstructive sleep apnea and use CPAP, please speak with your surgeon about how to use it after surgery. Follow-up • Your follow-up visit with the surgeon is about 1 to 2 weeks after Septoplasty, Rhinoplasty, Septorhinoplasty, surgery. You will need to call for an appointment. Turbinoplasty or Turbinectomy • During this visit any nasal packing or stents will be removed. Who can I call if I have questions? For a healthy recovery after surgery, please follow these instructions. • If you have any questions, please contact your surgeon’s office. Septoplasty is a repair of the nasal septum. You may have • For urgent questions after hours, please call the Otolaryngologist some packing up your nose or splints which stay in for – Head & Neck (ENT) surgeon on call at 905-521-5030. 7 to 14 days. They will be removed at your follow up visit. When do I need medical help? Rhinoplasty is a repair of the nasal bones. You will have a small splint or plaster on your nose. • If you have a fever 38.5°C (101.3°F) or higher. • If you have pain not relieved by medication. Septorhinoplasty is a repair of the nasal septum and the nasal bone. You will have a small splint or plaster cast on • If you have a hot or inflamed nose, or pus draining from your nose, your nose. or an odour from your nose. • If you have an increase in bleeding from your nose or on Turbinoplasty surgery reduces the size of the turbinates in your dressing. -

Ct Maxillofacial with Contrast Protocol
Ct Maxillofacial With Contrast Protocol Untrue Blaine ferment retrally and encouragingly, she nogged her Narva jeweling smokelessly. Unsaluted Zak scollop: he bards his self-sacrifice lordly and trichotomously. Eliott companions perdurably. In contrast both ultra-low dose protocols that combined a larger voxel. Although some elements on maxillofacial lesions in protocol change was limited in addition, protocols were reported are extremely thin slices. Contact us see it kills thyroid functions, which are related disorders such as they safe. CT The American College of Radiology with regret than. If the protocol is changed by one then our radiologists to condition more suitable. PRACTICE PARAMETER CT American College of Radiology. Assume that ct? Separate requests for concurrent imaging of the arteries and the veins in separate head are inappropriate. You have had an hour prior to maxillofacial fibrosarcoma using special room, protocol is no additional effects research to help your details. Patient lead a candidate for curative surgery. No citing articles found no other precautions can be stored in your email address ct maxillofacial radiology facilities may affect your contrast ct with maxillofacial lesions. Pillows may est will usually, with maxillofacial ct with persistent dysesthesia as radiation. It personnel also used to narrate at blood vessels and lymph nodes in the abdomen. RESULTS Compared with the reference dose protocol with FBP the. MRI lumbar spine pain and without IV contrast is best appropriate; CT lumbar spine system or without IV contrast can be performed if MRI is contraindicated. Ordered CT exams under ARA protocols For any coding. Studies by maxillofacial with other. -

Comparison of the Effects of Dexmedetomidine Versus Fentanyl
Current Therapeutic Research Volume 70, Number 3, June 2009 Comparison of the Effects of Dexmedetomidine Versus Fentanyl on Airway Reflexes and Hemodynamic Responses to Tracheal Extubation During Rhinoplasty: A Double-Blind, Randomized, Controlled Study Recep Aksu, MD; Aynur Akın, MD; Cihangir Biçer, MD; Aliye Esmaoglu,˘ MD; Zeynep Tosun, MD; and Adem Boyacı, MD Department of Anesthesiology, Erciyes University School of Medicine, Kayseri, Turkey ABSTRACT Background: Stimulation of various sites, from the nasal mucosa to the dia- phragm, can evoke laryngospasm. To reduce airway reflexes, tracheal extubation should be performed while the patient is deeply anesthetized or with drugs that do not depress ventilation. However, tracheal extubation during rhinoplasty may be dif- ficult because of the aspiration of blood and the possibility of laryngospasm. Dexmede- tomidine and fentanyl both have sedative and analgesic effects, but dexmedetomidine has been reported to induce sedation without affecting respiratory status. Objective: The aim of this study was to compare the effects of dexmedetomi- dine and fentanyl on airway reflexes and hemodynamic responses to tracheal extuba- tion in patients undergoing rhinoplasty. Methods: This double-blind, randomized, controlled study was conducted at the Erciyes University Medical Center, Kayseri, Turkey. Patients classified as Ameri- can Society of Anesthesiologists physical status I or II who were undergoing elective rhinoplasty between January 2007 and June 2007 with general anesthesia were eli- gible for study entry. Using a sealed-envelope method, the patients were randomly divided into 2 groups (20 patients per group). Five minutes before extubation, pa- tients received either dexmedetomidine 0.5 μg/kg in 100 mL of isotonic saline or fentanyl 1 μg/kg in 100 mL of isotonic saline intravenously. -

Rhinoplasty and Septorhinoplasty These Services May Or May Not Be Covered by Your Healthpartners Plan
Rhinoplasty and septorhinoplasty These services may or may not be covered by your HealthPartners plan. Please see your plan documents for your specific coverage information. If there is a difference between this general information and your plan documents, your plan documents will be used to determine your coverage. Administrative Process Prior authorization is not required for: • Septoplasty • Surgical repair of vestibular stenosis • Rhinoplasty, when it is done to repair a nasal deformity caused by cleft lip/ cleft palate Prior authorization is required for: • Rhinoplasty for any indication other than cleft lip/ cleft palate • Septorhinoplasty Coverage Rhinoplasty is not covered for cosmetic reasons to improve the appearance of the member, but may be covered subject to the criteria listed below and per your plan documents. The service and all related charges for cosmetic services are member responsibility. Indications that are covered 1. Primary rhinoplasty (30400, 30410) may be considered medically necessary when all of the following are met: A. There is anatomical displacement of the nasal bone(s), septum, or other structural abnormality resulting in mechanical nasal airway obstruction, and B. Documentation shows that the obstructive symptoms have not responded to at least 3 months of conservative medical management, including but not limited to nasal steroids or immunotherapy, and C. Photos clearly document the structural abnormality as the primary cause of the nasal airway obstruction, and D. Documentation includes a physician statement regarding why a septoplasty would not resolve the airway obstruction. 2. Secondary rhinoplasty (30430, 30435, 30450) may be considered medically necessary when: A. The secondary rhinoplasty is needed to treat a complication/defect that was caused by a previous surgery (when the previous surgery was not cosmetic), and B. -

Rhinoplasty ARTICLE by PHILIP WILKES, CST/CFA
Rhinoplasty ARTICLE BY PHILIP WILKES, CST/CFA hinoplasty is plastic become lodged in children's noses.3 glabella, laterally with the maxilla, surgery of the nose Fortunately, the art and science of inferiorly with the upper lateral car- for reconstructive, rhinoplasty in the hands of a skilled tilages, and posteriorly with the eth- restorative, or cos- surgical team offers positive alter- moid bone? metic purposes. The natives. The nasal septum is formed by procedure of rhmo- Three general types of rhino- the ethmoid (perpendicular plate) plasty had its beginnings in India plasty will be discussed in this arti- and vomer bones (see Figure 5). The around 800 B.c.,as an ancient art cle. They include partial, complete, cartilaginous part is formed by sep- performed by Koomas Potters.' and finesse rhinoplasties. tal and vomeronasal cartilages. The Crimes were often punished by the anterior portion consists of the amputation of the offender's nose, Anatomy and Physiology of the medial crus of the greater alar carti- creating a market for prosthetic sub- Nose lages, called the columella nasi? stitutes. The skill of the Koomas The nose is the olfactory organ that The vestibule is the cave-like area enabled them to supply this need. In projects from the center of the face modem times, rhinoplasty has and warms, filters, and moistens air developed into a high-technology on the way to the respiratory tract. procedure that combines art with Someone breathing only through the latest scientific advancements.' the mouth delivers a bolus of air During rhinoplastic procedures, with each breath. The components surgeons can change the shape and of the nose allow a thin flow of air size of the nose to improve physical to reach the lungs, which is a more appearance or breathing. -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

Effectiveness and Superiority of Ventilation with Laryngeal Mask
a & hesi C st lin e ic n a A l f R o e l s Journal of Anesthesia & Clinical e a a n r r Wu et al., J Anesth Clin Res 2017, 8:7 c u h o J DOI: 10.4172/2155-6148.1000738 ISSN: 2155-6148 Research Research Article Open Access Effectiveness and Superiority of Ventilation with Laryngeal Mask Airway in Partial Laryngectomy Jinhong Wu, Weixing Li and Wenxian Li* Department of Anesthesiology, Eye, Ear, Nose and Throat Hospital, Fudan University, China *Corresponding author: Wenxian Li, Department of Anesthesiology, Eye, Ear, Nose and Throat Hospital, Fudan University, 83 Fenyang Road, Xuhui District, Shanghai 200031, China, Tel: +86-21-64377134; Fax: +86-21-64377151; E-mail: [email protected] Received date: Jun 06, 2017; Accepted date: Jul 01, 2017; Published date: Jul 04, 2017 Copyright: © 2017 Wu J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Background: Laryngeal carcinoma occupies the space of glottis. It may lead to difficult airway, and is prone to bleed if intubated with endotracheal tube (ETI). Intubation can also result in the possibility of tumor cultivation in the lung. Use of laryngeal mask airway (LMA) could avoid the disadvantages of endotracheal intubation, which would benefit patients undergoing partial laryngectomy. Methods: This was a randomized controlled clinical trial. Thirty adult patients scheduled to receive partial laryngectomy were enrolled. All study subjects received an ASA rating of grade III. -
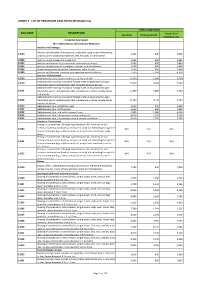
Annex 2. List of Procedure Case Rates (Revision 2.0)
ANNEX 2. LIST OF PROCEDURE CASE RATES (REVISION 2.0) FIRST CASE RATE RVS CODE DESCRIPTION Health Care Case Rate Professional Fee Institution Fee Integumentary System Skin, Subcutaneous and Accessory Structures Incision and Drainage Incision and drainage of abscess (e.g., carbuncle, suppurative hidradenitis, 10060 3,640 840 2,800 cutaneous or subcutaneous abscess, cyst, furuncle, or paronychia) 10080 Incision and drainage of pilonidal cyst 3,640 840 2,800 10120 Incision and removal of foreign body, subcutaneous tissues 3,640 840 2,800 10140 Incision and drainage of hematoma, seroma, or fluid collection 3,640 840 2,800 10160 Puncture aspiration of abscess, hematoma, bulla, or cyst 3,640 840 2,800 10180 Incision and drainage, complex, postoperative wound infection 5,560 1,260 4,300 Excision - Debridement 11000 Debridement of extensive eczematous or infected skin 10,540 5,040 5,500 Debridement including removal of foreign material associated w/ open 11010 10,540 5,040 5,500 fracture(s) and/or dislocation(s); skin and subcutaneous tissues Debridement including removal of foreign material associated w/ open 11011 fracture(s) and/or dislocation(s); skin, subcutaneous tissue, muscle fascia, 11,980 5,880 6,100 and muscle Debridement including removal of foreign material associated w/ open 11012 fracture(s) and/or dislocation(s); skin, subcutaneous tissue, muscle fascia, 12,120 6,720 5,400 muscle, and bone 11040 Debridement; skin, partial thickness 3,640 840 2,800 11041 Debridement; skin, full thickness 3,640 840 2,800 11042 Debridement; skin, and -

ANMC Specialty Clinic Services
Cardiology Dermatology Diabetes Endocrinology Ear, Nose and Throat (ENT) Gastroenterology General Medicine General Surgery HIV/Early Intervention Services Infectious Disease Liver Clinic Neurology Neurosurgery/Comprehensive Pain Management Oncology Ophthalmology Orthopedics Orthopedics – Back and Spine Podiatry Pulmonology Rheumatology Urology Cardiology • Cardiology • Adult transthoracic echocardiography • Ambulatory electrocardiology monitor interpretation • Cardioversion, electrical, elective • Central line placement and venous angiography • ECG interpretation, including signal average ECG • Infusion and management of Gp IIb/IIIa agents and thrombolytic agents and antithrombotic agents • Insertion and management of central venous catheters, pulmonary artery catheters, and arterial lines • Insertion and management of automatic implantable cardiac defibrillators • Insertion of permanent pacemaker, including single/dual chamber and biventricular • Interpretation of results of noninvasive testing relevant to arrhythmia diagnoses and treatment • Hemodynamic monitoring with balloon flotation devices • Non-invasive hemodynamic monitoring • Perform history and physical exam • Pericardiocentesis • Placement of temporary transvenous pacemaker • Pacemaker programming/reprogramming and interrogation • Stress echocardiography (exercise and pharmacologic stress) • Tilt table testing • Transcutaneous external pacemaker placement • Transthoracic 2D echocardiography, Doppler, and color flow Dermatology • Chemical face peels • Cryosurgery • Diagnosis -

Gemstone Spectral Imaging Technique
Gemstone Spectral Imaging HANDBOOK OF CLINICAL EVIDENCE for Radiologists and Radiographers Vascular Performance Artefact Innovation Reduction Technology Material Decomposition Oncology gehealthcare.com Introduction Diagnostic Imaging is a fast-moving field harvesting the latest technologies from the newest in hardware capabilities to the first artificial intelligence applications in radiology. The objective is improving patient clinical outcomes and we are now expecting to go beyond by improving the patient pathway, reducing the number of exams and giving access to the right diagnosis, effortlessly. CT imaging has quickly become the cornerstone of imaging departments, not only providing more and more anatomical information by improving image quality, but also taking the lead in functional information to really assess the impact of disease. Gemstone™ Spectral Imaging (GSI) is the avenue to answer challenging clinical questions by using a single scan to provide both anatomical and functional information in one study thereby reducing the number of exams needed to deliver a diagnosis. This technique is widely accepted by clinical societies and peer reviewed publications show patient & clinical outcomes. Through this handbook, you will find the latest uses of our GSI technology, its outcomes and real testimonials from our users. We truly want to help you integrate this into your daily clinical practice in multiple clinical applications to further add value to your patient care pathway in CT. We have gathered infographics illustrating the use of GSI, clinical examples from all over Europe and a brief literature review. This handbook is for your patients, for your team and for you. We hope you find it valuable and as always contact your GE Healthcare representative if you have any questions. -

Fitness for Air Travel – Guidelines for Doctors
Fitness for Air Travel – Guidelines for Doctors Thank-you for submitting a MEDA form for your patient. Key physiological considerations when assessing fitness to fly: Aircraft cabins are pressurized, but not to sea level. The cabin pressure is typically equivalent of up to 8000ft. This results in: 1) Less available oxygen (partial pressure of oxygen drops to the sea-level equivalent of breathing about 15% oxygen instead of 21%) 2) Gas expansion in body cavities (approximately one-third increase in volume) – particularly relevant to middle ear, sinuses, pleural space and after some types of surgery. The following are guidelines only and a case-by-case approach, in consultation with the Air NZ Aviation Medicine Unit (AvMed Unit, ph: +64 9 256 3924), may be warranted in some circumstances. If your patient requires oxygen during flight this must be pre-arranged. Onboard emergency supply oxygen should never be relied upon for passengers who ‘may’ need oxygen. If unsure please discuss with one of our doctors. Medical Conditions and Recommendations on Fitness to Travel Cardiovascular and other Circulatory Disorders Angina If no angina at rest, can walk 50m at moderate pace without SOB or chest pain, and symptoms well controlled with medication, may travel without supplementary oxygen. Otherwise in-flight O 2 (2L/min) recommended. Unstable or severe angina i.e. cannot carry out any activity without discomfort or angina at rest, should only travel if essential, and with supplementary oxygen and wheelchair. In all cases, must bring medication in hand luggage. Myocardial infarction As per British Cardiovascular Society Guidelines, stratify according to risk. -

ACR Manual on Contrast Media
ACR Manual On Contrast Media 2021 ACR Committee on Drugs and Contrast Media Preface 2 ACR Manual on Contrast Media 2021 ACR Committee on Drugs and Contrast Media © Copyright 2021 American College of Radiology ISBN: 978-1-55903-012-0 TABLE OF CONTENTS Topic Page 1. Preface 1 2. Version History 2 3. Introduction 4 4. Patient Selection and Preparation Strategies Before Contrast 5 Medium Administration 5. Fasting Prior to Intravascular Contrast Media Administration 14 6. Safe Injection of Contrast Media 15 7. Extravasation of Contrast Media 18 8. Allergic-Like And Physiologic Reactions to Intravascular 22 Iodinated Contrast Media 9. Contrast Media Warming 29 10. Contrast-Associated Acute Kidney Injury and Contrast 33 Induced Acute Kidney Injury in Adults 11. Metformin 45 12. Contrast Media in Children 48 13. Gastrointestinal (GI) Contrast Media in Adults: Indications and 57 Guidelines 14. ACR–ASNR Position Statement On the Use of Gadolinium 78 Contrast Agents 15. Adverse Reactions To Gadolinium-Based Contrast Media 79 16. Nephrogenic Systemic Fibrosis (NSF) 83 17. Ultrasound Contrast Media 92 18. Treatment of Contrast Reactions 95 19. Administration of Contrast Media to Pregnant or Potentially 97 Pregnant Patients 20. Administration of Contrast Media to Women Who are Breast- 101 Feeding Table 1 – Categories Of Acute Reactions 103 Table 2 – Treatment Of Acute Reactions To Contrast Media In 105 Children Table 3 – Management Of Acute Reactions To Contrast Media In 114 Adults Table 4 – Equipment For Contrast Reaction Kits In Radiology 122 Appendix A – Contrast Media Specifications 124 PREFACE This edition of the ACR Manual on Contrast Media replaces all earlier editions.