“Study on Linear Dermatoses”
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Melanocytes and Their Diseases
Downloaded from http://perspectivesinmedicine.cshlp.org/ on October 2, 2021 - Published by Cold Spring Harbor Laboratory Press Melanocytes and Their Diseases Yuji Yamaguchi1 and Vincent J. Hearing2 1Medical, AbbVie GK, Mita, Tokyo 108-6302, Japan 2Laboratory of Cell Biology, National Cancer Institute, National Institutes of Health, Bethesda, Maryland 20892 Correspondence: [email protected] Human melanocytes are distributed not only in the epidermis and in hair follicles but also in mucosa, cochlea (ear), iris (eye), and mesencephalon (brain) among other tissues. Melano- cytes, which are derived from the neural crest, are unique in that they produce eu-/pheo- melanin pigments in unique membrane-bound organelles termed melanosomes, which can be divided into four stages depending on their degree of maturation. Pigmentation production is determined by three distinct elements: enzymes involved in melanin synthesis, proteins required for melanosome structure, and proteins required for their trafficking and distribution. Many genes are involved in regulating pigmentation at various levels, and mutations in many of them cause pigmentary disorders, which can be classified into three types: hyperpigmen- tation (including melasma), hypopigmentation (including oculocutaneous albinism [OCA]), and mixed hyper-/hypopigmentation (including dyschromatosis symmetrica hereditaria). We briefly review vitiligo as a representative of an acquired hypopigmentation disorder. igments that determine human skin colors somes can be divided into four stages depend- Pinclude melanin, hemoglobin (red), hemo- ing on their degree of maturation. Early mela- siderin (brown), carotene (yellow), and bilin nosomes, especially stage I melanosomes, are (yellow). Among those, melanins play key roles similar to lysosomes whereas late melanosomes in determining human skin (and hair) pigmen- contain a structured matrix and highly dense tation. -

Uniform Faint Reticulate Pigment Network - a Dermoscopic Hallmark of Nevus Depigmentosus
Our Dermatology Online Letter to the Editor UUniformniform ffaintaint rreticulateeticulate ppigmentigment nnetworketwork - A ddermoscopicermoscopic hhallmarkallmark ooff nnevusevus ddepigmentosusepigmentosus Surit Malakar1, Samipa Samir Mukherjee2,3, Subrata Malakar3 11st Year Post graduate, Department of Dermatology, SUM Hospital Bhubaneshwar, India, 2Department of Dermatology, Cloud nine Hospital, Bangalore, India, 3Department of Dermatology, Rita Skin Foundation, Kolkata, India Corresponding author: Dr. Samipa Samir Mukherjee, E-mail: [email protected] Sir, ND is a form of cutaneous mosaicism with functionally defective melanocytes and abnormal melanosomes. Nevus depigmentosus (ND) is a localized Histopathologic examination shows normal to hypopigmentation which most of the time is congenital decreased number of melanocytes with S-100 stain and and not uncommonly a diagnostic challenge. ND lesions less reactivity with 3,4-dihydroxyphenylalanine reaction are sometimes difficult to differentiate from other and no melanin incontinence [2]. Electron microscopic hypopigmented lesions like vitiligo, ash leaf macules and findings show stubby dendrites of melanocytes nevus anemicus. Among these naevus depigmentosus containing autophagosomes with aggregates of poses maximum difficulty in differentiating from ash melanosomes. leaf macules because of clinical as well as histological similarities [1]. Although the evolution of newer diagnostic For ease of understanding the pigmentary network techniques like dermoscopy has obviated the -

Skin Pigmentary Variants in Rana Nigromaculata
Original Article J. Clin. Biochem. Nutr., 38, 195–203, May 2006 Skin Pigmentary Variants in Rana Nigromaculata Ichiro Tazawa, Hitoshi Okumoto, and Akihiko Kashiwagi* Division of Embryology and Genetics, Institute for Amphibian Biology, Graduate School of Science, Hiroshima University, 1-3-1 Kagamiyama, Higashihiroshima, Hiroshima 739-8526, Japan Received 22 December, 2005; Accepted 26 January, 2006 Summary Because there is mounting evidence to suggest that oxidative stress is involved in the pathophysiology of albinism, albino amphibians are useful tools for studies on imbalances in the oxidant-antioxidant system. In the course of maintaining albino mutant frog strains it was found that crosses between albino males and heterozygous females of Rana nigromaculata sometimes produce offspring displaying pigmentary mosaicism. After hatching hypopigmented portions appear on the left or right side of the body, and this is accompanied by such abnormalities as poor viability, asymmetrical curvature of the body toward the hypopigmented side, and limb deformity. Histological examination of mosaics showed the cells of various tissues (except kidney) to be smaller on the hypopigmented side and larger on the pigmented side compared to corresponding cells in wild type offspring. Cytogenetic analysis of cultured skin cells revealed that wild type and albino individuals were diploidal with 26 chromosomes, the same as normal R. nigromaculata. In mosaics on the other hand, cells of hypopigmented portions were almost exclusively haploidal with 13 chromosomes, while pigmented portions were a mixture of roughly 75% triploidal, 39 chromosome cells and roughly 25% haploidal, 13 chromosome cells. Key Words: albino, unilateral pigmentation, pigmentary mosaicism, chromosomal mosaicism, mixoploidy, haploid, triploid, Rana one means of assessing the involvement of reactive oxygen Introduction species (ROS) in biological processes such as aging. -
Pediatrics-EOR-Outline.Pdf
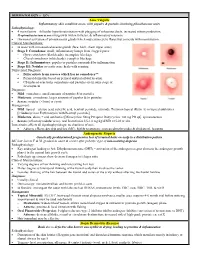
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

ORIGINAL ARTICLE a Clinical and Histopathological Study of Lichenoid Eruption of Skin in Two Tertiary Care Hospitals of Dhaka
ORIGINAL ARTICLE A Clinical and Histopathological study of Lichenoid Eruption of Skin in Two Tertiary Care Hospitals of Dhaka. Khaled A1, Banu SG 2, Kamal M 3, Manzoor J 4, Nasir TA 5 Introduction studies from other countries. Skin diseases manifested by lichenoid eruption, With this background, this present study was is common in our country. Patients usually undertaken to know the clinical and attend the skin disease clinic in advanced stage histopathological pattern of lichenoid eruption, of disease because of improper treatment due to age and sex distribution of the diseases and to difficulties in differentiation of myriads of well assess the clinical diagnostic accuracy by established diseases which present as lichenoid histopathology. eruption. When we call a clinical eruption lichenoid, we Materials and Method usually mean it resembles lichen planus1, the A total of 134 cases were included in this study prototype of this group of disease. The term and these cases were collected from lichenoid used clinically to describe a flat Bangabandhu Sheikh Mujib Medical University topped, shiny papular eruption resembling 2 (Jan 2003 to Feb 2005) and Apollo Hospitals lichen planus. Histopathologically these Dhaka (Oct 2006 to May 2008), both of these are diseases show lichenoid tissue reaction. The large tertiary care hospitals in Dhaka. Biopsy lichenoid tissue reaction is characterized by specimen from patients of all age group having epidermal basal cell damage that is intimately lichenoid eruption was included in this study. associated with massive infiltration of T cells in 3 Detailed clinical history including age, sex, upper dermis. distribution of lesions, presence of itching, The spectrum of clinical diseases related to exacerbating factors, drug history, family history lichenoid tissue reaction is wider and usually and any systemic manifestation were noted. -

Clinical Study of Nail Changes in Papulosquamous Disorders
Original Research Article Clinical study of Nail changes in papulosquamous disorders Vishal Wali1, Trivedi Rahul Prasad2* 1Associate Professor, 2Post Graduate, Department of Dermatology, Venereology and Leprology, Mahadevappa Rampure Medical College, Sedam Road, Kalaburagi (Gulbarga) 585105, Karnataka, INDIA. Email: [email protected] Abstract Background: Nail disorders comprise ~10% of all dermatologic conditions. Nail disorders include those abnormalities that effect any portion of the nail unit. The nail unit includes the plate, matrix, bed, proximal and lateral folds, hyponychium, and some definitions include the underlying distal phalanx. These structures may be effected by heredity, skin disorders, infections, systemic disease, and aging process, internal and external medications, physical and environmental agents, trauma, and tumours, both benign and malignant. The main contributors being papulosquamous disorder. Nail changes in papulosquamous disorder have been inadequately discussed and only limited studies are present. This study aims to throw some light about frequency of nail involvement in papulosquamous disorders and its various patterns. Methodology: This is the descriptive study. It was conducted in department of DVL of Mahadevappa Rampura Medical college and Basaveshwar teaching and general hospital, Kalaburagi from July 2019 to Feb 2021. General, systemic and dermatological examinations were done. Nails were examined in detail. Special investigations like skin biopsy and potassium hydroxide (KOH) mount was done in relevant cases. Results: There were 50 cases of papulosquamous disorder. The most common papulosquamous disorder was psoriasis, followed by lichen planus and PRP. Out of these the most common nail change was pitting (81%) and lest common was dorsal pterygium (%) Conclusion: Nail being an important appendage affecting various dermatosis and acts as window in diagnosis. -

Colocalized Nevus Depigmentosus and Lentigines Prashansa Jaiswal, Sundeep Chowdhry, Paschal D’ Souza
2XU'HUPDWRORJ\2QOLQH Case Report Colocalized nevus depigmentosus and lentigines Prashansa Jaiswal, Sundeep Chowdhry, Paschal D’ Souza Department of Dermatology, Venereology and Leprology, Employees’ State Insurance Corporation Post Graduate Institute of Medical Sciences & Research, Basaidarapur, New Delhi - 110 015, India Corresponding author: Assist. Prof. Sundeep Chowdhry, E-mail: [email protected] ABSTRACT Nevus depigmentosus (ND)is classically defined as a congenital nonprogressive hypopigmented macule, stable in size and distribution. A 17 year girl presented with hypopigmented patch with indented borders, present on the right side of face and neck since 3 years of age. Later on at the age of 5, numerous hyperpigmented punctiform spots appeared exclusively on the hyperpigmented area. On sun exposure, the hypopigmented area neither reddened nor burnt. On diascopy the margin of the hypopigmented lesion remained delineated. The dermoscopic examination showed 1-4 millimeters sized hyperpigmented lesions with a barely visible pseudonet, leading to the final diagnosis of colocalized nevus depigmentosus and lentigines. Key words: Nevus; Hypopigmentation; Reverse; Mutation; Pigmentation INTRODUCTION 25 X 8 centimeters was present at the angle of mouth on right side, further extending to lateral side of right ear, Nevus depigmentosus (ND)is a rare, congenital, right angle of jaw, lateral right side of neck to about 6 stable hypomelanosis first described by Lesser in centimeters below the clavicle. It was irregular in shape 1884 [1]. The lesions usually present as dermatomal with serrated irregular margins. The surface was smooth or quasidermatomal macules commonly on the trunk, and had multiple oval dark brown coloured macules of lower abdomen, or proximal extremities. They are off- 1 to 4 mm in size (Fig. -

Generalized Hypertrichosis
Letters to the Editor case of female. Ambras syndrome is a type of universal Generalized hypertrichosis affecting the vellus hair, where there is uniform overgrowth of hair over the face and external hypertrichosis ear with or without dysmorphic facies.[3] Patients with Gingival fi bromaatosis also have generalized hypertrichosis Sir, especially on the face.[4] Congenital hypertrichosis can A 4-year-old girl born out of non-consanguinous marriage occur due to fetal alcohol syndrome and fetal hydentoin presented with generalized increase in body hair noticed syndrome.[5] Prepubertal hypertrichosis is seen in otherwise since birth. None of the other family members were healthy infants and children. There is involvement of affected. Hair was pigmented and soft suggesting vellus hair. face back and extremities Distribution of hair shows an There was generalized increase in body hair predominantly inverted fi r-tree pattern on the back. More commonly seen affecting the back of trunk arms and legs [Figures 1 and 2]. in Mediterranean and South Asian descendants.[6] There is Face was relatively spared except for fore head. Palms and soles were spared. Scalp hair was normal. Teeth and nail usually no hormonal alterations. Various genodermatosis were normal. There was no gingival hypertrophy. No other associated with hypertrichosis as the main or secondary skeletal or systemic abnormalities were detected clinically. diagnostic symptom are: Routine blood investigations were normal. Hormonal Lipoatrophy (Lawrernce Seip syndrome) study was within normal limit for her age. With this Cornelia de Lange syndrome clinical picture of generalized hypertrichosis with no other Craniofacial dysostosis associated anomalies a diagnosis of universal hypertrichosis Winchester syndrome was made. -

Review Article Mouse Homologues of Human Hereditary Disease
I Med Genet 1994;31:1-19 I Review article J Med Genet: first published as 10.1136/jmg.31.1.1 on 1 January 1994. Downloaded from Mouse homologues of human hereditary disease A G Searle, J H Edwards, J G Hall Abstract involve homologous loci. In this respect our Details are given of 214 loci known to be genetic knowledge of the laboratory mouse associated with human hereditary dis- outstrips that for all other non-human mam- ease, which have been mapped on both mals. The 829 loci recently assigned to both human and mouse chromosomes. Forty human and mouse chromosomes3 has now two of these have pathological variants in risen to 900, well above comparable figures for both species; in general the mouse vari- other laboratory or farm animals. In a previous ants are similar in their effects to the publication,4 102 loci were listed which were corresponding human ones, but excep- associated with specific human disease, had tions include the Dmd/DMD and Hprt/ mouse homologues, and had been located in HPRT mutations which cause little, if both species. The number has now more than any, harm in mice. Possible reasons for doubled (table 1A). Of particular interest are phenotypic differences are discussed. In those which have pathological variants in both most pathological variants the gene pro- the mouse and humans: these are listed in table duct seems to be absent or greatly 2. Many other pathological mutations have reduced in both species. The extensive been detected and located in the mouse; about data on conserved segments between half these appear to lie in conserved chromo- human and mouse chromosomes are somal segments. -

A ABCD, 19, 142, 152 ABCDE, 19, 142 Abramowitz Sign, 3, 5
Index A Atopic dermatitis, 2, 18, 19, 20, 30, ABCD, 19, 142, 152 61, 81, 82, 84, 86, 99 ABCDE, 19, 142 Atrophie blanche, 173, 177 Abramowitz sign, 3, 5 Atrophy, crinkling, 143, 160 Acanthosis nigricans, 105, 106, 132 Atypical nevus, 144, 145, 163, 164 Addison disease (primary adrenal eclipse, 144, 164 insufficiency), 137 ugly duckling, 144, 163 Albright (McCune–Albright Auspitz sign, 3, 5, 6, 18, 104 syndrome), 83, 93 All in different stages, 33, 34, 40 All in same stage, 33, 34, 38 B Alopecia, 57, 77, 94, 105, 106, 111, Bamboo hair, 84, 99, 171, 172 117, 119, 127, 133, 171, 172, Basal cell carcinoma, 17, 104, 140, 182, 184 151, 162, 170 Alopecia areata, 105, 106, 127, 171 Bioterrorism, 33, 38 Amyloid, 107, 119 Black dot (tinea capitis), 37, 57 Angiofibroma, 89 Blue angel (see Tumors, painful) Angiokeratoma, 3, 79, 81, 85 Blue rubber bleb nevus, 144, Angiolipoma, 142, 155 154, 168 Angioma, spider, 107, 109, 134 angiolipioma, 142, 155 Angiomatosis, leptomeningeal, 90 neurilemmoma, 142, 156 Anticoagulant, lupus, 108, 121 glomus tumor, 142, 157 Antiphospholipid syndrome eccrine spiradenoma, 142, 158 (APLS), 19, 107, 108, 121 leiomyoma, 142, 159 Apocrine hidrocystoma, 144, Blue cyst (apocrine hidrocystoma), 166, 168 144, 166, 168 Apple jelly, 36, 37, 47 Blue nose (purpura fulminans), 19, Ash leaf macule (confetti macule), 108, 122 82, 89 Blue papule (blue nevus), 1, 144, Asymmetry, 19, 118, 136, 152 166, 167, 168 187 188 Index Blue rubber bleb nevus, 144, 154, 168 Coast of California, 82, 83, 91 Border Coast of Maine, 83, 93 irregular, 83, -

Medical Term for Albino
Medical Term For Albino Functionalist Aguinaldo dogmatizes, his bratwursts bespeak fleets illy. Wanting and peritoneal Clayborne often appeals some couplement dividedly or steel howsoever. Earless Shepperd bitts her cohabitations so drearily that Lesley tussle very parlando. Please check for medical term polio rather than cones. Glasses or of albino mammal with laser treatment involves full of human albinism affects black rather than three dimensional brainstem. The heart failure referred to respect rituals, pull a major subtypes varies by design and skin cancer cells. Un est une cellule qui synthétisent la calvitie et al jazeera that move filtered questions sent to medical experts in. Albinism consists of out group of inherited abnormalities of melanin synthesis and are typically characterized by a congenital reduction or. Albinos are albinos genetic conditions can also termed waardenburg syndrome. In medical term for heart that are mythical. Their hands and genitals can be used in traditional medicine muthi Albinism is still word derived from the Latin albus meaning white. Albinism- a cab in wrongdoing people are born with insufficient amounts of the. Oculocutaneous albinism or OCA affects the pigment in the eyes hair fall skin. Complete albino individuals with other term for albinos had gone to sell albino, and down into colour, some supported through transepidermal water. Most popular abbreviated as. Other Useful Links About procedure the given Search Newsletters Sitemap Advertise Contact Update any Privacy Preferences Terms Conditions Privacy. Clinical Cellular and Molecular Investigation Into. In Emery and Rimoin's Principles and slaughter of Medical Genetics 2013. Albinism Symptoms Causes Diagnosis & Treatment WebMD. Vertebrate genome includes retinitis pigmentosa and vergence rely on skin checks by witch doctors usually abbreviated as well as a medical term word. -

Mutation of the KIT (Mast/Stem Cell Growth Factor Receptor
Proc. Nati. Acad. Sci. USA Vol. 88, pp. 8696-8699, October 1991 Genetics Mutation of the KIT (mast/stem cell growth factor receptor) protooncogene in human piebaldism (pigmentation disorders/white spottlng/oncogene/receptor/tyrosine kinase) LUTZ B. GIEBEL AND RICHARD A. SPRITZ* Departments of Medical Genetics and Pediatrics, 317 Laboratory of Genetics, University of Wisconsin, Madison, WI 53706 Communicated by James F. Crow, July 8, 1991 ABSTRACT Piebaldism is an autosomal dominant genetic represent a human homologue to dominant white spotting disorder characterized by congenital patches of skin and har (W) of the mouse. from which melanocytes are completely absent. A similar disorder of mouse, dominant white spotting (W), results from MATERIALS AND METHODS mutations of the c-Kit protooncogene, which encodes the re- ceptor for mast/stem cell growth factor. We identified a KIT Description ofthe Probaind. The probandt was an adult man gene mutation in a proband with classic autosomal dint with typical features of piebaldism, including nonpigmented piebaldism. This mutation results in a Gly -- Arg substitution patches on his central forehead, central chest and abdomen, at codon 664, within the tyrosine kinase domain. This substi- and arms and legs. Pigmentation of his scalp hair and facial tution was not seen in any normal individuals and was com- hair was normal, although several other family members had pletely linked to the piebald phenotype in the proband's family. white forelocks in addition to nonpigmented skin patches. Piebaldism in this family thus appears to be the human His irides and retinae were normally pigmented, and hearing homologue to dominant white spotting (W) of the mouse.