Molecular and Clinical Characterization of 5Mc Regulators in Glioma: Results of A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

6064.Full.Pdf
Activation-Induced Cytidine Deaminase-Dependent DNA Breaks in Class Switch Recombination Occur during G1 Phase of the Cell Cycle and Depend upon This information is current as Mismatch Repair of September 27, 2021. Carol E. Schrader, Jeroen E. J. Guikema, Erin K. Linehan, Erik Selsing and Janet Stavnezer J Immunol 2007; 179:6064-6071; ; doi: 10.4049/jimmunol.179.9.6064 Downloaded from http://www.jimmunol.org/content/179/9/6064 References This article cites 51 articles, 21 of which you can access for free at: http://www.jimmunol.org/ http://www.jimmunol.org/content/179/9/6064.full#ref-list-1 Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists by guest on September 27, 2021 • Fast Publication! 4 weeks from acceptance to publication *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2007 by The American Association of Immunologists All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology Activation-Induced Cytidine Deaminase-Dependent DNA Breaks in Class Switch Recombination Occur during G1 Phase of the Cell Cycle and Depend upon Mismatch Repair1 Carol E. -

Identification of Conserved Genes Triggering Puberty in European Sea
Blázquez et al. BMC Genomics (2017) 18:441 DOI 10.1186/s12864-017-3823-2 RESEARCHARTICLE Open Access Identification of conserved genes triggering puberty in European sea bass males (Dicentrarchus labrax) by microarray expression profiling Mercedes Blázquez1,2* , Paula Medina1,2,3, Berta Crespo1,4, Ana Gómez1 and Silvia Zanuy1* Abstract Background: Spermatogenesisisacomplexprocesscharacterized by the activation and/or repression of a number of genes in a spatio-temporal manner. Pubertal development in males starts with the onset of the first spermatogenesis and implies the division of primary spermatogonia and their subsequent entry into meiosis. This study is aimed at the characterization of genes involved in the onset of puberty in European sea bass, and constitutes the first transcriptomic approach focused on meiosis in this species. Results: European sea bass testes collected at the onset of puberty (first successful reproduction) were grouped in stage I (resting stage), and stage II (proliferative stage). Transition from stage I to stage II was marked by an increase of 11ketotestosterone (11KT), the main fish androgen, whereas the transcriptomic study resulted in 315 genes differentially expressed between the two stages. The onset of puberty induced 1) an up-regulation of genes involved in cell proliferation, cell cycle and meiosis progression, 2) changes in genes related with reproduction and growth, and 3) a down-regulation of genes included in the retinoic acid (RA) signalling pathway. The analysis of GO-terms and biological pathways showed that cell cycle, cell division, cellular metabolic processes, and reproduction were affected, consistent with the early events that occur during the onset of puberty. -

Ubiquitination/Deubiquitination and Acetylation/Deacetylation
Acta Pharmacologica Sinica (2011) 32: 139–140 npg © 2011 CPS and SIMM All rights reserved 1671-4083/11 $32.00 www.nature.com/aps Research Highlight Ubiquitination/deubiquitination and acetylation/ deacetylation: Making DNMT1 stability more coordinated Qi HONG, Zhi-ming SHAO* Acta Pharmacologica Sinica (2011) 32: 139–140; doi: 10.1038/aps.2011.3 n mammals, DNA methylation plays important role in human cancers[7, 8]. abundance of DNMT1 mutant lacking Ia crucial role in the regulation of Ubiquitinproteasome pathway is sig the HAUSP interaction domain, but not gene expression, telomere length, cell nificant in the stability of DNMT1[8], but the fulllength protein. These results differentiation, X chromosome inactiva ubiquitinmediated protein degradation show the coordination between ubiquit tion, genomic imprinting and tumori can be enhanced or attenuated by some ination of DNMT1 by UHRF1 and deu genesis[1]. DNA methylation patterns modifications like acetylation/deacety biquitination by HAUSP. Furthermore, are established de novo by DNA meth lation, protein methylation/demethyla they found that knockdown of HDAC1 yltransferases (DNMTs) 3a and 3b, tion, phosphorylation and Snitrosy increased DNMT1 acetylation, and whereas DNMT1 maintains the parent lation[9–11]. Estève et al demonstrated reduced DNMT1 abundance. Addition specific methylation from parental cells that SET7mediated lysine methy lation ally, acetyltransferase Tip60 which was to their progeny[2]. After DNA replica of DNMT1 decreased DNMT1 level found to acetylate DNMT1 promoted its tion, the new DNA strand is unmethy by ubiquitinmediated degradation[10]. ubiquitination, then destabilized it. At lated. Thus with the mother methylated Furthermore, an early study[12] showed last, Tip60 and HAUSP were found to strand, the DNA is hemimethylated. -
1 AGING Supplementary Table 2
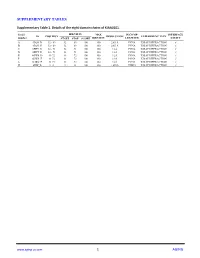
SUPPLEMENTARY TABLES Supplementary Table 1. Details of the eight domain chains of KIAA0101. Serial IDENTITY MAX IN COMP- INTERFACE ID POSITION RESOLUTION EXPERIMENT TYPE number START STOP SCORE IDENTITY LEX WITH CAVITY A 4D2G_D 52 - 69 52 69 100 100 2.65 Å PCNA X-RAY DIFFRACTION √ B 4D2G_E 52 - 69 52 69 100 100 2.65 Å PCNA X-RAY DIFFRACTION √ C 6EHT_D 52 - 71 52 71 100 100 3.2Å PCNA X-RAY DIFFRACTION √ D 6EHT_E 52 - 71 52 71 100 100 3.2Å PCNA X-RAY DIFFRACTION √ E 6GWS_D 41-72 41 72 100 100 3.2Å PCNA X-RAY DIFFRACTION √ F 6GWS_E 41-72 41 72 100 100 2.9Å PCNA X-RAY DIFFRACTION √ G 6GWS_F 41-72 41 72 100 100 2.9Å PCNA X-RAY DIFFRACTION √ H 6IIW_B 2-11 2 11 100 100 1.699Å UHRF1 X-RAY DIFFRACTION √ www.aging-us.com 1 AGING Supplementary Table 2. Significantly enriched gene ontology (GO) annotations (cellular components) of KIAA0101 in lung adenocarcinoma (LinkedOmics). Leading Description FDR Leading Edge Gene EdgeNum RAD51, SPC25, CCNB1, BIRC5, NCAPG, ZWINT, MAD2L1, SKA3, NUF2, BUB1B, CENPA, SKA1, AURKB, NEK2, CENPW, HJURP, NDC80, CDCA5, NCAPH, BUB1, ZWILCH, CENPK, KIF2C, AURKA, CENPN, TOP2A, CENPM, PLK1, ERCC6L, CDT1, CHEK1, SPAG5, CENPH, condensed 66 0 SPC24, NUP37, BLM, CENPE, BUB3, CDK2, FANCD2, CENPO, CENPF, BRCA1, DSN1, chromosome MKI67, NCAPG2, H2AFX, HMGB2, SUV39H1, CBX3, TUBG1, KNTC1, PPP1CC, SMC2, BANF1, NCAPD2, SKA2, NUP107, BRCA2, NUP85, ITGB3BP, SYCE2, TOPBP1, DMC1, SMC4, INCENP. RAD51, OIP5, CDK1, SPC25, CCNB1, BIRC5, NCAPG, ZWINT, MAD2L1, SKA3, NUF2, BUB1B, CENPA, SKA1, AURKB, NEK2, ESCO2, CENPW, HJURP, TTK, NDC80, CDCA5, BUB1, ZWILCH, CENPK, KIF2C, AURKA, DSCC1, CENPN, CDCA8, CENPM, PLK1, MCM6, ERCC6L, CDT1, HELLS, CHEK1, SPAG5, CENPH, PCNA, SPC24, CENPI, NUP37, FEN1, chromosomal 94 0 CENPL, BLM, KIF18A, CENPE, MCM4, BUB3, SUV39H2, MCM2, CDK2, PIF1, DNA2, region CENPO, CENPF, CHEK2, DSN1, H2AFX, MCM7, SUV39H1, MTBP, CBX3, RECQL4, KNTC1, PPP1CC, CENPP, CENPQ, PTGES3, NCAPD2, DYNLL1, SKA2, HAT1, NUP107, MCM5, MCM3, MSH2, BRCA2, NUP85, SSB, ITGB3BP, DMC1, INCENP, THOC3, XPO1, APEX1, XRCC5, KIF22, DCLRE1A, SEH1L, XRCC3, NSMCE2, RAD21. -

Supplemental Information
Supplemental information Dissection of the genomic structure of the miR-183/96/182 gene. Previously, we showed that the miR-183/96/182 cluster is an intergenic miRNA cluster, located in a ~60-kb interval between the genes encoding nuclear respiratory factor-1 (Nrf1) and ubiquitin-conjugating enzyme E2H (Ube2h) on mouse chr6qA3.3 (1). To start to uncover the genomic structure of the miR- 183/96/182 gene, we first studied genomic features around miR-183/96/182 in the UCSC genome browser (http://genome.UCSC.edu/), and identified two CpG islands 3.4-6.5 kb 5’ of pre-miR-183, the most 5’ miRNA of the cluster (Fig. 1A; Fig. S1 and Seq. S1). A cDNA clone, AK044220, located at 3.2-4.6 kb 5’ to pre-miR-183, encompasses the second CpG island (Fig. 1A; Fig. S1). We hypothesized that this cDNA clone was derived from 5’ exon(s) of the primary transcript of the miR-183/96/182 gene, as CpG islands are often associated with promoters (2). Supporting this hypothesis, multiple expressed sequences detected by gene-trap clones, including clone D016D06 (3, 4), were co-localized with the cDNA clone AK044220 (Fig. 1A; Fig. S1). Clone D016D06, deposited by the German GeneTrap Consortium (GGTC) (http://tikus.gsf.de) (3, 4), was derived from insertion of a retroviral construct, rFlpROSAβgeo in 129S2 ES cells (Fig. 1A and C). The rFlpROSAβgeo construct carries a promoterless reporter gene, the β−geo cassette - an in-frame fusion of the β-galactosidase and neomycin resistance (Neor) gene (5), with a splicing acceptor (SA) immediately upstream, and a polyA signal downstream of the β−geo cassette (Fig. -

Mir-17-92 Fine-Tunes MYC Expression and Function to Ensure
ARTICLE Received 31 Mar 2015 | Accepted 22 Sep 2015 | Published 10 Nov 2015 DOI: 10.1038/ncomms9725 OPEN miR-17-92 fine-tunes MYC expression and function to ensure optimal B cell lymphoma growth Marija Mihailovich1, Michael Bremang1, Valeria Spadotto1, Daniele Musiani1, Elena Vitale1, Gabriele Varano2,w, Federico Zambelli3, Francesco M. Mancuso1,w, David A. Cairns1,w, Giulio Pavesi3, Stefano Casola2 & Tiziana Bonaldi1 The synergism between c-MYC and miR-17-19b, a truncated version of the miR-17-92 cluster, is well-documented during tumor initiation. However, little is known about miR-17-19b function in established cancers. Here we investigate the role of miR-17-19b in c-MYC-driven lymphomas by integrating SILAC-based quantitative proteomics, transcriptomics and 30 untranslated region (UTR) analysis upon miR-17-19b overexpression. We identify over one hundred miR-17-19b targets, of which 40% are co-regulated by c-MYC. Downregulation of a new miR-17/20 target, checkpoint kinase 2 (Chek2), increases the recruitment of HuR to c- MYC transcripts, resulting in the inhibition of c-MYC translation and thus interfering with in vivo tumor growth. Hence, in established lymphomas, miR-17-19b fine-tunes c-MYC activity through a tight control of its function and expression, ultimately ensuring cancer cell homeostasis. Our data highlight the plasticity of miRNA function, reflecting changes in the mRNA landscape and 30 UTR shortening at different stages of tumorigenesis. 1 Department of Experimental Oncology, European Institute of Oncology, Via Adamello 16, Milan 20139, Italy. 2 Units of Genetics of B cells and lymphomas, IFOM, FIRC Institute of Molecular Oncology Foundation, Milan 20139, Italy. -

Epigenetic Regulation of DNA Repair Genes and Implications for Tumor Therapy ⁎ ⁎ Markus Christmann , Bernd Kaina
Mutation Research-Reviews in Mutation Research xxx (xxxx) xxx–xxx Contents lists available at ScienceDirect Mutation Research-Reviews in Mutation Research journal homepage: www.elsevier.com/locate/mutrev Review Epigenetic regulation of DNA repair genes and implications for tumor therapy ⁎ ⁎ Markus Christmann , Bernd Kaina Department of Toxicology, University of Mainz, Obere Zahlbacher Str. 67, D-55131 Mainz, Germany ARTICLE INFO ABSTRACT Keywords: DNA repair represents the first barrier against genotoxic stress causing metabolic changes, inflammation and DNA repair cancer. Besides its role in preventing cancer, DNA repair needs also to be considered during cancer treatment Genotoxic stress with radiation and DNA damaging drugs as it impacts therapy outcome. The DNA repair capacity is mainly Epigenetic silencing governed by the expression level of repair genes. Alterations in the expression of repair genes can occur due to tumor formation mutations in their coding or promoter region, changes in the expression of transcription factors activating or Cancer therapy repressing these genes, and/or epigenetic factors changing histone modifications and CpG promoter methylation MGMT Promoter methylation or demethylation levels. In this review we provide an overview on the epigenetic regulation of DNA repair genes. GADD45 We summarize the mechanisms underlying CpG methylation and demethylation, with de novo methyl- TET transferases and DNA repair involved in gain and loss of CpG methylation, respectively. We discuss the role of p53 components of the DNA damage response, p53, PARP-1 and GADD45a on the regulation of the DNA (cytosine-5)- methyltransferase DNMT1, the key enzyme responsible for gene silencing. We stress the relevance of epigenetic silencing of DNA repair genes for tumor formation and tumor therapy. -

UHRF1 Depletion Suppresses Growth of Gallbladder Cancer Cells Through Induction of Apoptosis and Cell Cycle Arrest
ONCOLOGY REPORTS 31: 2635-2643, 2014 UHRF1 depletion suppresses growth of gallbladder cancer cells through induction of apoptosis and cell cycle arrest YIYU QIN1, JIANDONG WANG1, WEI GONG1, MINGDI ZHANG1, ZHAOHUI TANG1, JUN ZHANG2 and ZHIWEI QUAN1 1Department of General Surgery and 2Ministry of Education-Shanghai Key Laboratory of Children's Environmental Health, Xinhua Hospital Affiliated to Shanghai Jiaotong University School of Medicine, Shanghai 200092, P.R. China Received December 28, 2013; Accepted February 21, 2014 DOI: 10.3892/or.2014.3145 Abstract. Ubiquitin-like containing PHD and RING finger proliferation and migration of GBC cells and may serve as a domains 1 (UHRF1), overexpressed in various human biomarker or even a therapeutic target for GBC. malignancies, functions as an important regulator in cell proliferation and epigenetic regulation. Depletion of UHRF1 Introduction has shown potential antitumor activities in several types of cancer. However, the role of UHRF1 in gallbladder cancer Gallbladder cancer (GBC) represents the most frequent and (GBC) has not been investigated. RT-PCR, western blotting aggressive type among biliary tract malignancies. Although and immunohistochemistry were performed to examine recent advances have been made in the diagnosis and treatment, UHRF1 expression at mRNA and protein levels in GBC tissues GBC has a poor overall prognosis with a 5-year survival rate and cell lines. UHRF1 siRNA and UHRF1 shRNA were used <10% (1). Currently, radical resection remains the mainstay of to deplete the expression of UHRF1. The results showed treatment for GBC. However, due to lacking typical symptoms that UHRF1 was overexpressed in GBC and its expression and specific biomarkers, most GBC patients are diagnosed correlated with advanced TNM stage and presence of lymph at advanced stages with unresectable tumors. -

Uhrf1-Mediated Tnf-Α Gene Methylation Controls
Uhrf1-Mediated Tnf-α Gene Methylation Controls Proinflammatory Macrophages in Experimental Colitis Resembling Inflammatory Bowel Disease This information is current as of September 30, 2021. Shanshan Qi, Yongkui Li, Zheng Dai, Mengxi Xiang, Guobin Wang, Lin Wang and Zheng Wang J Immunol published online 14 October 2019 http://www.jimmunol.org/content/early/2019/10/12/jimmun ol.1900467 Downloaded from Supplementary http://www.jimmunol.org/content/suppl/2019/10/12/jimmunol.190046 Material 7.DCSupplemental http://www.jimmunol.org/ Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication by guest on September 30, 2021 *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2019 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. Published October 14, 2019, doi:10.4049/jimmunol.1900467 The Journal of Immunology Uhrf1-Mediated Tnf-a Gene Methylation Controls Proinflammatory Macrophages in Experimental Colitis Resembling Inflammatory Bowel Disease Shanshan Qi,*,1 Yongkui Li,*,1 Zheng Dai,* Mengxi Xiang,* Guobin Wang,*,† Lin Wang,*,‡ and Zheng Wang*,† Macrophages drive the pathological process of inflammatory bowel diseases (IBD) mostly by secreting proinflammatory cytokines, such as Tnf-a. -

Genome-Wide DNA Methylation Analysis Reveals Molecular Subtypes of Pancreatic Cancer
www.impactjournals.com/oncotarget/ Oncotarget, 2017, Vol. 8, (No. 17), pp: 28990-29012 Research Paper Genome-wide DNA methylation analysis reveals molecular subtypes of pancreatic cancer Nitish Kumar Mishra1 and Chittibabu Guda1,2,3,4 1Department of Genetics, Cell Biology and Anatomy, University of Nebraska Medical Center, Omaha, NE, 68198, USA 2Bioinformatics and Systems Biology Core, University of Nebraska Medical Center, Omaha, NE, 68198, USA 3Department of Biochemistry and Molecular Biology, University of Nebraska Medical Center, Omaha, NE, 68198, USA 4Fred and Pamela Buffet Cancer Center, University of Nebraska Medical Center, Omaha, NE, 68198, USA Correspondence to: Chittibabu Guda, email: [email protected] Keywords: TCGA, pancreatic cancer, differential methylation, integrative analysis, molecular subtypes Received: October 20, 2016 Accepted: February 12, 2017 Published: March 07, 2017 Copyright: Mishra et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC-BY), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. ABSTRACT Pancreatic cancer (PC) is the fourth leading cause of cancer deaths in the United States with a five-year patient survival rate of only 6%. Early detection and treatment of this disease is hampered due to lack of reliable diagnostic and prognostic markers. Recent studies have shown that dynamic changes in the global DNA methylation and gene expression patterns play key roles in the PC development; hence, provide valuable insights for better understanding the initiation and progression of PC. In the current study, we used DNA methylation, gene expression, copy number, mutational and clinical data from pancreatic patients. -

M Phase Phosphorylation of the Epigenetic Regulator UHRF1 Regulates Its Physical Association with the Deubiquitylase USP7 and Stability
M phase phosphorylation of the epigenetic regulator UHRF1 regulates its physical association with the deubiquitylase USP7 and stability Honghui Maa,1, Hao Chena,1, Xue Guoa,1, Zhentian Wanga, Mathew E. Sowab, Lijuan Zhenga, Shibin Hua, Pingyao Zenga, Rui Guoa, Jianbo Diaoa, Fei Lanc, J. Wade Harperb, Yujiang Geno Shia,d, Yanhui Xua,e,2, and Yang Shia,b,f,g,2 aLaboratory of Epigenetics, Institute of Biomedical Sciences, and Department of Biochemistry, Fudan University Medical School, 138 Yixue Yuan Road, Shanghai 200032, China; bDepartment of Cell Biology, Harvard Medical School, 77 Avenue Louis Pasteur, Boston, MA 02115; cConstellation Pharmaceuticals, 215 First Street, Cambridge, MA 02140; dEndocrinology Division, Brigham and Women Hospital, Harvard Medical School, Boston, MA 02115; eState Key Laboratory of Genetic Engineering, School of Life Sciences, Fudan University, Shanghai 200433, China; fDepartment of Biochemistry, Fudan University Medical School, 138 Yixue Yuan Road, Shanghai 200032, China; and gDivision of Newborn Medicine and Program in Epigenetics, Department of Medicine, Children’s Hospital, Harvard Medical School, 300 Longwood Avenue, Boston, MA 02115 Edited by Tony Hunter, The Salk Institute for Biological Studies, La Jolla, CA, and approved January 27, 2012 (received for review October 7, 2011) UHRF1 (Ubiquitin-like, with PHD and RING finger domains 1) plays question, we have recently undertaken a proteomics approach an important role in DNA CpG methylation, heterochromatin and identified a cell cycle signaling-regulated physical interaction function and gene expression. Overexpression of UHRF1 has been of UHRF1 with the deubiquitylase USP7 (HAUSP) (8, 9) and suggested to contribute to tumorigenesis. However, regulation of demonstrated that it is important for protecting UHRF1 from UHRF1 is largely unknown. -

P90 and UHRF1, Two Novel Regulators of the P53 Signaling Pathway
p90 and UHRF1, Two Novel Regulators of the p53 Signaling Pathway Chao Dai Submitted in partial fulfillment of the Requirements for the degree of Doctor of Philosophy in the Graduate School of Arts and Sciences COLUMBIA UNIVERSITY 2014 ©2013 Chao Dai All Rights Reserved ABSTRACT p90 and UHRF1, Two Novel Regulators of the p53 Signaling Pathway Chao Dai To ensure proper and differentiated regulation of stress response pathways, the p53 tumor suppressor calls for an intricate network of control of activation and fine tuning of transcription activity, which is offered largely through post- translational modifications. Accumulating evidence supports the indispensability of acetylation in the activation of p53 function and indicates modulation of cell fate decision; however the underlying molecular mechanisms are not well understood and identification of the regulatory mechanisms controlling p53 acetylation remains an important step in furthering the understanding of p53 regulation in vivo. In this study we identify p90 and UHRF1 as two novel members of the p53 regulatory network upstream of TIP60-mediated p53 acetylation. Through biochemical purification, p90 was identified as a unique regulator for p53. p90 (also called CCDC8, coiled-coil domain containing 8) interacts with p53 both in vitro and in vivo. Depletion of p90 by RNAi has no obvious effect on p53 stability or p53-mediated activation of p21, but specifically abrogates PUMA activation. Moreover, p90 also interacts with the TIP60 acetyltransferase and stimulates TIP60-dependent Lys120 acetylation of p53, therefore enhancing the apoptotic response of p53. These data reveal p90 as an upstream regulator of the Tip60-p53 interaction and demonstrate that p90 is specifically required for p53- mediated apoptosis upon DNA damage.