Emerging Medical Treatment for Hypertrophic Cardiomyopathy
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-
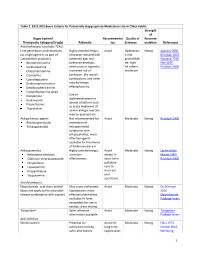
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

And Its Obstructive Form, Idiopathic Hypertrophic Subaortic Stenosis (IHSS), in Pediatrics
Asymmetric septal hypertrophy (ASH) and its obstructive form, idiopathic hypertrophic subaortic stenosis (IHSS), in pediatrics ALBERT K. HARVEY, DD. Oklahoma City, Oklahoma IHSS. The father had no siblings, but two uncles had Although idiopathic hypertrophic died suddenly of heart disease at early ages. subaortic stenosis usually occurs in Case 1 adults, the possibility of its presence in children must not be overlooked. It An 18-year-old white girl said she had not experienced dyspnea, exercise intolerance, syncope, or chest pain. She has been reported even as early as was a senior in high school and had participated in dra- infancy and in stillborn fetuses. The matic and athletic activities. Physical examination condition appears to be genetically showed the pulse rate to be 74 and the blood pressure transmitted, with the natural history 110/64 mm. Hg. Pulses on the upper and lower ex- one of progressive disease. The tremities were strong and symmetric. The point of atypical location of an aortic stenosis maximum intensity (PMI) was not enlarged, and no type murmur is a clue to early thrill or precordial heave was perceptible. There was a diagnosis. Echocardiography is Grade 2/6 harsh systolic ejection murmur along the lower confirmative of a diagnosis. Four case left sternal border, which was transmitted well to the reports are presented. apex. No diastolic component was present. The phono- cardiogram showed an intermittent fourth heart sound. An x-ray film of the chest showed the heart size and vascularity of the lung field to be normal. An elec- trocardiogram (EKG) revealed left ventricular hyper- trophy with marked ST and T wave changes in the left precordial leads. -

Heart & Vascular Institute
Sydell and Arnold Miller Family Heart & Vascular Institute 9500 Euclid Avenue, Cleveland, OH 44195 ClevelandClinic.org 2016 Outcomes 17-OUT-413 108369_CCFBCH_Cov_acg.indd 1 8/31/17 12:22 PM Measuring Outcomes Promotes Quality Improvement This project would not have been possible without the commitment and expertise of a team led by Umesh Khot, MD; Mouin Abdallah, MD; Sandra Hays; and Jagina McIntyre. Graphic design and photography were provided by Brian Kohlbacher and Cleveland Clinic’s Center for Medical Art and Photography. © The Cleveland Clinic Foundation 2017 108369_CCFBCH_Cov_acg.indd 2 9/19/17 10:57 AM Measuring and understanding outcomes of medical treatments promotes quality improvement. Cleveland Clinic has created a series of Outcomes books similar to this one for its clinical institutes. Designed for a physician audience, the Outcomes books contain a summary of many of our surgical and medical treatments, with a focus on outcomes data and a review of new technologies and innovations. The Outcomes books are not a comprehensive analysis of all treatments provided at Cleveland Clinic, and omission of a particular treatment does not necessarily mean we do not offer that treatment. When there are no recognized clinical outcome measures for a specific treatment, we may report process measures associated with improved outcomes. When process measures are unavailable, we may report volume measures; a relationship has been demonstrated between volume and improved outcomes for many treatments, particularly those involving surgical and -

NORPACE- Disopyramide Phosphate Capsule, Gelatin Coated
NORPACE- disopyramide phosphate capsule, gelatin coated Carilion Materials Management ---------- Norpace disopyramide phosphate capsules Norpace CR disopyramide phosphate extended- release capsules ® ® DESCRIPTION Norpace (disopyramide phosphate) is an antiarrhythmic drug available for oral administration in immediate-release and controlled-release capsules containing 100 mg or 150 mg of disopyramide base, present as the phosphate. The base content of the phosphate salt is 77.6%. The structural formula of Norpace is: Norpace is freely soluble in water, and the free base (pKa 10.4) has an aqueous solubility of 1 mg/ml. The chloroform:water partition coefficient of the base is 3.1 at pH 7.2. Norpace is a racemic mixture of and isomers. This drug is not chemically related to other antiarrhythmic drugs. d-l- Norpace CR (controlled-release) capsules are designed to afford a gradual and consistent release of disopyramide. Thus, for maintenance therapy, Norpace CR provides the benefit of less-frequent dosing (every 12 hours) as compared with the every-6-hour dosage schedule of immediate-release Norpace capsules. Inactive ingredients of Norpace include corn starch, edible ink, FD&C Red No. 3, FD&C Yellow No. 6, gelatin, lactose, talc, and titanium dioxide; the 150-mg capsule also contains FD&C Blue No. 1. Inactive ingredients of Norpace CR include corn starch, D&C Yellow No. 10, edible ink, ethylcellulose, FD&C Blue No. 1, gelatin, shellac, sucrose, talc, and titanium dioxide; the 150-mg capsule also contains FD&C Red No. 3 and FD&C Yellow No. 6. CLINICAL PHARMACOLOGY Mechanisms of Action Norpace (disopyramide phosphate) is a Type 1 antiarrhythmic drug (i.e., similar to procainamide and quinidine). -

Surgical Septal Myectomy Outcome for Obstructive Hypertrophic Cardiomyopathy After Alcohol Septal Ablation
1065 Original Article Surgical septal myectomy outcome for obstructive hypertrophic cardiomyopathy after alcohol septal ablation Qiulan Yang1^, Changsheng Zhu1, Hao Cui2, Bing Tang3, Shengwei Wang3, Qinjun Yu4, Shihua Zhao5, Yunhu Song1, Shuiyun Wang1 1Department of Cardiovascular Surgery, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing, China; 2Department of Cardiovascular Surgery, Mayo Clinic, Rochester, MI, USA; 3Department of Cardiac Surgery, Beijing Anzhen Hospital, Capital Medical University & Beijing Institute of Heart, Beijing, China; 4Department of Anesthesiology, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing, China; 5Department of Magnetic Resonance Imaging, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing, China Contributions: (I) Conception and design: S Wang; (II) Administrative support: C Zhu, H Cui, B Tang, S Wang, S Zhao; (III) Provision of study materials or patients: C Zhu; (IV) Collection and assembly of data: Q Yang; (V) Data analysis and interpretation: C Zhu, H Cui, B Tang, S Wang, S Zhao; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Shuiyun Wang. Department of Cardiovascular Surgery, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, Beilishi Road 167, Xicheng District, Beijing 100037, China. Email: [email protected]. Background: Although surgical treatment of residual obstruction after alcohol septal ablation (ASA) is often challenging in patients with obstructive hypertrophic cardiomyopathy (OHCM) there are very few relevant clinical reports. Thus, outcomes of surgical septal myectomy (SSM) in this subgroup of patients remain to be determined. -

Asymmetric Septal Hypertrophy in Patients with Aortic Stenosis: an Adaptive Mechanism Or a Coexistence of Hypertrophic Cardiomyopathy?
View metadata, citation and similar papers at core.ac.uk brought to you by CORE J AM cou,providedCARDIOl by Elsevier - Publisher783 Connector 1983.1(3)783-9 Asymmetric Septal Hypertrophy in Patients With Aortic Stenosis: An Adaptive Mechanism or a Coexistence of Hypertrophic Cardiomyopathy? OTTO M. HESS, MD, JAKOB SCHNEIDER, MD, MARCO TURINA, MD, JOHN D. CARROLL, MD, FACC, MARTIN ROTHLIN, MD, HANS P. KRAYENBUEHL, MD Zurich, Switzerland Myocardial histologic features andventricular left dy• 1 and 2 (26.5 versus 29.1IJ.; NS), but muscle fiber di• namics were assessed in 24 patients with severe aorticameter of the septum in group 1 was significantlysmaller stenosis, 12 with (group 1) and 12 without (group(24.4 2) IJ.; P < 0.01) than that ofanterolateral the wall in associated asymmetric septalhypertrophy.In 10patients group 2. No morphologic abnormalities typical for hy• from group 1,echocardiographyshowed a septal/pos• pertrophic cardiomyopathy (fiberdisarray)were seen in teriorwall ratio of 1.5; in the other 2, asymmetric septalsamples from the patients in either group. By 18 months hypertrophywas diagnosed by direct inspection at thepostoperatively, septal wall thickness had decreased sig• time of surgery. Septal myectomy in all 12 patientsnificantly in from 2.0 to 1.5 em< (p0.01) and posterior group 1 was completed at the time of aortic valvewall re• thickness from 1.4 to 1.2 cm< (p0.05) in group 1. In group 2, septal wall thickness decreased from 1.5 placement. Septal histologicfeatures were assessedfrom to 1.3 em (NS) and posterior wall thickness from 1.4 to surgical specimens in 10 patients in groupTransseptal 1. -

Septal Myectomy for Obstructive Hypertrophic Cardiomyopathy Joseph A
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector Septal Myectomy for Obstructive Hypertrophic Cardiomyopathy Joseph A. Dearani, MD, and Gordon K. Danielson, MD ransaortic septal myectomy is currently considered to tion of the LVOT gradient is important so that a compar- Tbe the most appropriate surgical treatment for pa- ison can be made with postmyectomy measurements. tients with obstructive hypertrophic cardiomyopathy Standard cardiopulmonary bypass with mild to moderate (HCM) and severe symptoms unresponsive to medical hypothermia (30-34°C) is used and the left heart is vented therapy.1-18 However, there is a significant learning curve with a catheter inserted through the right superior pulmo- for this procedure, and early surgical experience was as- nary vein. Myocardial protection, especially important be- sociated with complications of complete heart block, ven- cause of the severe ventricular hypertrophy, is begun with tricular septal defect, injury to the aortic or mitral valves, a generous infusion of cold blood cardioplegia (800-1000 and incomplete relief of obstruction. Current surgical re- mL) into the aortic root followed by additional doses given sults are vastly improved, although the reported experi- selectively into the left and right coronary ostia every 20 ence in North America is limited to a few centers. minutes. For more complex and lengthy procedures, top- ical cooling with ice-cold saline is applied, and an insulat- Surgical Technique ing pad is placed behind the left ventricle. After the extended left ventricular septal myectomy is Over the last three decades, our technique of septal myec- performed, the resected area can be deepened with a ron- tomy has evolved from the classic Morrow myectomy (Fig geur. -

Data Element Specifications
California CABG Outcomes Reporting Program (CCORP) Data Element Specifications Version 7.1 May 5, 2019 California CABG Outcomes Reporting Program Data Element Specifications Version 7.1, dated May 5, 2019 (1) Medical Record Number: (A) Format: Alphanumeric, length 12 (B) Valid Values: Free text (C) Category: Demographics (D) Definition/Description: Indicate the patient's medical record number at the hospital where surgery occurred. (2) Type of Coronary Artery Bypass Graft (CABG): (A) Format: Numeric, length 1 (B) Valid Values: 1 = Isolated CABG; 3 = CABG + Valve; 4= Other non-isolated CABG (C) Category: Operative (D) Definition/Description: Indicate the type of CABG. (i) Type of CABG should be coded Isolated CABG if none of the procedures listed in this subsection was performed concurrently with the coronary artery bypass surgery. (a) Valve repairs or replacements (b) Operations on structures adjacent to heart valves (papillary muscle, chordae tendineae, traebeculae carneae cordis, annuloplasty, infundibulectomy) (c) Ventriculectomy when diagnosed preoperatively as a rupture, aneurysm or remodeling procedure. Excludes 1) sites intra-operatively diagnosed, 2) patch applications for site oozing discovered during surgery and 3) prophylactic patch applications to reduce chances of future rupture (d) Repair of atrial and ventricular septa, excluding closure of patent foramen ovale (e) Excision of aneurysm of heart (f) Head and neck, intracranial endarterectomy (g) Other open heart surgeries, such as aortic arch repair, pulmonary endarterectomy -

Targeting Alcohol Septal Ablation in Patients with Obstructive
Journal of Clinical Medicine Article Targeting Alcohol Septal Ablation in Patients with Obstructive Hypertrophic Cardiomyopathy Candidates for Surgical Myectomy: Added Value of Three-Dimensional Intracoronary Myocardial Contrast Echocardiography Giovanni La Canna 1,*, Iside Scarfò 1, Irina Arendar 1, Antonio Colombo 2, Lucia Torracca 3, Davide Margonato 4, Matteo Montorfano 4 and Ottavio Alfieri 5 1 Applied Diagnostic Echocardiography Unit, IRCCS Humanitas Clinical and Research Center, 20089 Rozzano, Italy; [email protected] (I.S.); [email protected] (I.A.) 2 Interventional Cardiology Unit, IRCCS Humanitas Clinical and Research Center, 20089 Rozzano, Italy; [email protected] 3 Cardiac Surgery, IRCCS Humanitas Clinical and Research Center, 20089 Rozzano, Italy; [email protected] 4 Interventional Cardiology Unit, IRCCS San Raffaele Scientific Institute, 20132 Milan, Italy; [email protected] (D.M.); [email protected] (M.M.) 5 Cardiac Surgery Unit, IRCCS San Raffaele Scientific Institute, 20132 Milan, Italy; ottavio.alfi[email protected] * Correspondence: [email protected]; Tel.: +39-33-5674-4319 Citation: La Canna, G.; Scarfò, I.; Abstract: Background: Myocardial contrast two-dimensional echocardiography (MC-2DE) is widely Arendar, I.; Colombo, A.; Torracca, L.; Margonato, D.; Montorfano, M.; used to address alcohol septal ablation (ASA) in obstructive hypertrophic cardiomyopathy (HCM). Alfieri, O. Targeting Alcohol Septal Owing to its limited cut-planes, MC-2DE may inaccurately identify the contrast misplacement Ablation in Patients with Obstructive associated with an unsuccessful or complicated ASA outcome. Objective: The aim of this study Hypertrophic Cardiomyopathy was to assess the added value of myocardial contrast three-dimensional echocardiography (MC- Candidates for Surgical Myectomy: 3DE) compared with MC-2DE to identify the appropriate matching between the target septal zone Added Value of Three-Dimensional (TSZ) and coronary artery branch for safe and long-term effective ASA in HCM patients. -

Hypertrophic Cardiomyopathy 2011 Pocket Guide
ACCF/AHA Pocket Guideline Adapted from the 2011 ACCF/AHA Guideline for the Diagnosis and Treatment of Hypertrophic Cardiomyopathy November 2011 Developed in Collaboration With the American Association for Thoracic Surgery, American Society of Echocardiography, American Society of Nuclear Cardiology, Heart Failure Society of America, Heart Rhythm Society, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons © 2011 by the American College of Cardiology Foundation and the American Heart Association, Inc. The following material was adapted from the 2011 ACCF/AHA Guidelines for the Diagnosis and Treatment of Hypertrophic Cardiomyopathy (J Am Coll Cardiol 2011;XX:XX–XX). This pocket guideline is available on the World Wide Web sites of the American College of Cardiology (www.cardiosource. org) and the American Heart Association (my.americanheart.org). For copies of this document, please contact Elsevier Inc. Reprint Department, e-mail: [email protected]; phone: 212-633-3813; fax: 212-633-3820. Permissions: Multiple copies, modification, alteration, enhancement, and/ ordistribution of this document are not permitted without the express permission of the American College of Cardiology Foundation. Please contact Elsevier’s permission department at [email protected]. Contents 1. Introduction .........................................................................................3 2. Clinical Definition ................................................................................6 3. Genetic -

Newyork-Presbyterian 2017 Outcomes and Quality Report in Cardiovascular Services
NewYork-Presbyterian Cardiovascular Services 2017 Outcomes and Quality Report NewYork-Presbyterian Cardiology and Heart Surgery ranks #3 in the nation. NewYork-Presbyterian Cardiovascular Services 2017 Outcomes and Quality Report Welcome 1 Measures of Distinction 2 Innovations at a Glance 3 Complex Cardiac Care Adult Congenital Heart Disease 4 Advanced Heart Failure 6 Arrhythmias 10 Coronary Artery Disease 12 Hypertrophic Cardiomyopathy 15 Pulmonary Hypertension 16 Valve Disease 18 Aortic Disease 23 NewYork-Presbyterian Today 26 3D fl uorescence deconvolution micrograph of stacked images showing adrenergic receptors (red) clustered around the nucleus of a myofi bril in the heart tissue of a heart failure patient For More Information nyp.org/amazingadvances Welcome Dear Colleague: We are pleased to bring you our 2017 Outcomes and Quality Report in Cardiovascular Services. The strength of our cardiology, interventional cardiology, and cardiac surgery programs is derived from the exceptional clinical, scientic, and educational resources made possible by the partnership of NewYork-Presbyterian, Columbia University Medical Center, and Weill Cornell Medicine. These programs are among the largest and most comprehensive in the nation, bringing together faculty that have made transformative contributions to their specialties – from adult congenital heart disease to advanced heart failure and complex valve disease. Our patients benet from exceptional heart teams, whose multispecialty members provide Dr. Steven J. Corwin collaborative and integrated care that optimizes their outcomes. Our physicians treat the most challenging cases, applying expertise that crosses and often combines the skills of cardiologists, interventionalists, and surgeons to meet the unique needs of each patient. This collegiality is a hallmark of our cardiology and heart surgery programs and a key factor in being ranked #1 in New York State for the past 17 years and #3 in the nation since 2013 by U.S.News & World Report. -

Disopyramide for Obstructive Hypertrophic Cardiomyopathy Symptoms and Gradient Resistant to First-Line Medical Therapy Approxima
Disopyramide for Obstructive Hypertrophic Cardiomyopathy Symptoms and Gradient Resistant to First‐Line Medical Therapy Approximately 2/3 of patients with hypertrophic cardiomyopathy (HCM) have left ventricular outflow tract (LVOT) obstruction either at rest or after physiologic provocation. Besides left ventricular hypertrophy (LVH), such patients have either resting, or provocable LVOT gradient > 30mmHg which contributes to their symptoms of exercise intolerance, dyspnea, angina or syncope. Moreover, resting gradient is associated with decreased survival. The most common cause of LVOT obstruction is due to systolic anterior motion of the mitral valve (SAM) and mitral‐septal contact. The underlying cause of SAM is an altered internal geometry of the LV, leading to an overlap between the inflow and outflow portions of the LV. Besides septal hypertrophy, this overlap is caused by anterior displacement of the mitral apparatus (papillary muscles and mitral leaflets) and mitral slack. Drag, the pushing force of flow is the dominant hydrodynamic force that causes SAM; flow gets behind the mitral leaflets and sweeps them into the septum. LVOT obstruction is associated with increased systolic LV work, decreased diastolic aortic perfusion pressure, supply‐demand ischemia, load‐related impairment in diastolic relaxation and a mid‐systolic drop in instantaneous LV ejection flow velocities and flow 1 A unique feature of obstructive HCM is the provocable gradient. Obstruction worsens after physiologic stimuli that reduce preload and afterload and increase contractility such as Valsalva maneuver, standing, after eating and particularly after exercise. Unfortunately, the more widely used cardiac medications, such as ACE‐inhibitors, ARBs, vasodilators, and nitrates are deleterious in exactly this way and increase gradient because of their vasodilatory properties.