New Product Information Wording – Extracts from PRAC Recommendations on Signals Adopted at the 11-14 May 2020 PRAC
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
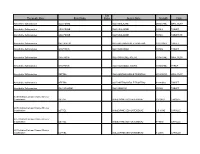
Therapeutic Class Brand Name P a Status Generic
P A Therapeutic Class Brand Name Status Generic Name Strength Form Absorbable Sulfonamides AZULFIDINE SULFASALAZINE 250MG/5ML ORAL SUSP Absorbable Sulfonamides AZULFIDINE SULFASALAZINE 500MG TABLET Absorbable Sulfonamides AZULFIDINE SULFASALAZINE 500MG TABLET DR Absorbable Sulfonamides BACTRIM DS SULFAMETHOXAZOLE/TRIMETHO 800-160MG TABLET Absorbable Sulfonamides GANTRISIN SULFISOXAZOLE 500MG TABLET Absorbable Sulfonamides GANTRISIN SULFISOXAZOLE ACETYL 500MG/5ML ORAL SUSP Absorbable Sulfonamides GANTRISIN SULFISOXAZOLE ACETYL 500MG/5ML SYRUP Absorbable Sulfonamides SEPTRA SULFAMETHOXAZOLE/TRIMETHO 200-40MG/5 ORAL SUSP Absorbable Sulfonamides SEPTRA SULFAMETHOXAZOLE/TRIMETHO 400-80MG TABLET Absorbable Sulfonamides SULFADIAZINE SULFADIAZINE 500MG TABLET ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 10-20MG CAPSULE ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 2.5-10MG CAPSULE ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 5-10MG CAPSULE ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 5-20MG CAPSULE P A Therapeutic Class Brand Name Status Generic Name Strength Form ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 5-40MG CAPSULE ACE Inhibitor/Calcium Channel Blocker Combination LOTREL AMLODIPINE BESYLATE/BENAZ 10-40MG CAPSULE Acne Agents, Systemic ACCUTANE ISOTRETINOIN 10MG CAPSULE Acne Agents, Systemic ACCUTANE ISOTRETINOIN 20MG CAPSULE Acne Agents, Systemic ACCUTANE -

Clinical Efficacy of Hormonal and Nonhormonal Agents in The
https://doi.org/10.6118/jmm.20026 J Menopausal Med 2021;27:15-23 pISSN: 2288-6478, eISSN: 2288-6761 ORIGINAL ARTICLE Clinical Efficacy of Hormonal and Nonhormonal Agents in the Treatment of Vulvovaginal Atrophy Gokcen Ilhan1, Mehmet Musa Aslan2, Arif Serhan Cevrioglu3, Muzaffer Yıldırım4, Unal Erkorkmaz5 1Department of Obstetrics and Gynecology, Haydarpasa Numune Training and Research Hospital, Istanbul, Turkey, 2Department of Obstetrics and Gynecology, Sakarya Training and Research Hospital, Ministry of Health, Sakarya University, Sakarya, Turkey, 3Department of Obstetrics and Gynecology, Sakarya University School of Medicine, Sakarya, Turkey, 4Department of Pathology, Sakarya University School of Medicine, Sakarya, Turkey, 5Department of Biostatistics, Sakarya University School of Medicine, Sakarya, Turkey Objectives: Symptomatic local treatment of vaginal atrophy (VA) in menopausal women includes hormonal and nonhormonal preparations. Some women may be reluctant to use vaginal estradiol preparations because of the concern for developing breast cancer and endometrial hyperplasia. Therefore, it is necessary to compare the therapeutic effectiveness of alternative vaginal drugs, such as promestriene, an estrogen agonist, and sodium hyaluronate (NaH), a nonhormonal, water-based agent. Methods: Ninety-one postmenopausal women diagnosed with symptomatic VA were divided into three groups and treated for 12 weeks; 30 women with vaginal estradiol (VE), 30 women with promestriene, and 31 women with NaH. Composite scoring, vaginal maturation index (VMI), pH, frequency of sexual activity, serum hormone levels, and endometrial thickness were evaluated VA before and after treatment. Results: In the comparison of VA examination findings composite scoring, VMI, and vaginal pH values, three different drugs were found to be effective in the treatment (P < 0.05). -

PEMD-91-12BR Off-Label Drugs: Initial Results of a National Survey
11 1; -- __...._-----. ^.-- ______ -..._._ _.__ - _........ - t Ji Jo United States General Accounting Office Washington, D.C. 20648 Program Evaluation and Methodology Division B-242851 February 25,199l The Honorable Edward M. Kennedy Chairman, Committee on Labor and Human Resources United States Senate Dear Mr. Chairman: In September 1989, you asked us to conduct a study on reimbursement denials by health insurers for off-label drug use. As you know, the Food and Drug Administration designates the specific clinical indications for which a drug has been proven effective on a label insert for each approved drug, “Off-label” drug use occurs when physicians prescribe a drug for clinical indications other than those listed on the label. In response to your request, we surveyed a nationally representative sample of oncologists to determine: . the prevalence of off-label use of anticancer drugs by oncologists and how use varies by clinical, demographic, and geographic factors; l the extent to which third-party payers (for example, Medicare intermediaries, private health insurers) are denying payment for such use; and l whether the policies of third-party payers are influencing the treatment of cancer patients. We randomly selected 1,470 members of the American Society of Clinical Oncologists and sent them our survey in March 1990. The sam- pling was structured to ensure that our results would be generalizable both to the nation and to the 11 states with the largest number of oncologists. Our response rate was 56 percent, and a comparison of respondents to nonrespondents shows no noteworthy differences between the two groups. -

Postmenopausal Pharmacotherapy Newsletter
POSTMENOPAUSAL PHARMACOTHERAPY September, 1999 As Canada's baby boomers age, more and more women will face the option of Hormone Replacement Therapy (HRT). The HIGHLIGHTS decision can be a difficult one given the conflicting pros and cons. M This RxFiles examines the role and use of HRT, as well as newer Long term HRT carries several major benefits but also risks SERMS and bisphosphonates in post-menopausal (PM) patients. which should be evaluated on an individual and ongoing basis MContinuous ERT is appropriate for women without a uterus HRT MWomen with a uterus should receive progestagen (at least 12 HRT is indicated for the treatment of PM symptoms such as days per month or continuous low-dose) as part of their HRT vasomotor disturbances and urogenital atrophy, and is considered MLow-dose ERT (CEE 0.3mg) + Ca++ appears to prevent PMO primary therapy for prevention and treatment of postmenopausal MBisphosphinates (e.g. alendronate, etidronate) and raloxifene are osteoporosis (PMO).1 Contraindications are reviewed in Table 2. alternatives to HRT in treating and preventing PMO Although HRT is contraindicated in women with active breast or M"Natural" HRT regimens can be compounded but data is lacking uterine cancer, note that a prior or positive family history of these does not necessarily preclude women from receiving HRT.1 Comparative Safety: Because of differences between products, some side effects may be alleviated by switching from one product Estrogen Replacement Therapy (ERT) 2 to another, particularly from equine to plant sources or from oral to Naturally secreted estrogens include: topical (see Table 3 - Side Effects & Their Management). -

Genitourinary Syndrome of Menopause in Breast Cancer Survivors: Are We Facing New and Safe Hopes?
Review Genitourinary Syndrome of Menopause in Breast Cancer Survivors: Are We Facing New and Safe Hopes? Nicoletta Biglia,1 Valentina E. Bounous,1 Luca G. Sgro,1 Marta D’Alonzo,1 Silvia Pecchio,1 Rossella E. Nappi2 Abstract Breast cancer survivors (BCSs) often suffer from menopausal symptoms induced by systemic treatments, with a consequent negative effect on quality of life. Since the introduction of aromatase inhibitors as the standard therapy for hormone-dependent tumors, genitourinary syndrome of menopause (GSM) has become a main problem for BCSs. This new terminology refers to the wide range of vaginal and urinary symptoms related to menopause, which can be relieved by estrogen therapy. Unfortunately, systemic hormone therapy is contraindicated for BCSs and also vaginal estrogens at standard dosage might influence the risk of recurrence because they cause a significant increase of circulating estrogens. Nonhormonal vaginal moisturizers or lubricants are the first choice for BCSs but only have limited and short-term efficacy. New strategies of management of GSM are now available, including: (1) low-dose or ultra low-dose vaginal estrogens; (2) oral selective estrogen receptor modulators (ospemifene); (3) androgen therapy; (4) physical treatment with vaginal laser; and (5) psychosocial interventions. In this review we discuss and analyze these different options. Clinical Breast Cancer, Vol. -, No. -, --- ª 2015 Elsevier Inc. All rights reserved. Keywords: BCS, GSM, Iatrogenic menopause, Treatment, Vulvovaginal atrophy (VVA) Introduction vasomotor symptoms are the most common side effects, affecting Breast cancer affects 1 of 8 women who live up to the age of 85 approximately 65% of BCSs.3 Even vulvovaginal atrophy (VVA) is years in Western countries. -

Estradiol-17Β Pharmacokinetics and Histological Assessment Of
animals Article Estradiol-17β Pharmacokinetics and Histological Assessment of the Ovaries and Uterine Horns following Intramuscular Administration of Estradiol Cypionate in Feral Cats Timothy H. Hyndman 1,* , Kelly L. Algar 1, Andrew P. Woodward 2, Flaminia Coiacetto 1 , Jordan O. Hampton 1,2 , Donald Nickels 3, Neil Hamilton 4, Anne Barnes 1 and David Algar 4 1 School of Veterinary Medicine, Murdoch University, Murdoch 6150, Australia; [email protected] (K.L.A.); [email protected] (F.C.); [email protected] (J.O.H.); [email protected] (A.B.) 2 Faculty of Veterinary and Agricultural Sciences, University of Melbourne, Melbourne 3030, Australia; [email protected] 3 Lancelin Veterinary Hospital, Lancelin 6044, Australia; [email protected] 4 Department of Biodiversity, Conservation and Attractions, Locked Bag 104, Bentley Delivery Centre 6983, Australia; [email protected] (N.H.); [email protected] (D.A.) * Correspondence: [email protected] Received: 7 September 2020; Accepted: 17 September 2020; Published: 21 September 2020 Simple Summary: Feral cats (Felis catus) have a devastating impact on Australian native fauna. Several programs exist to control their numbers through lethal removal, using tools such as baiting with toxins. Adult male cats are especially difficult to control. We hypothesized that one way to capture these male cats is to lure them using female cats. As female cats are seasonal breeders, a method is needed to artificially induce reproductive (estrous) behavior so that they could be used for this purpose year-round (i.e., regardless of season). -

Exposure to Female Hormone Drugs During Pregnancy
British Journal of Cancer (1999) 80(7), 1092–1097 © 1999 Cancer Research Campaign Article no. bjoc.1998.0469 Exposure to female hormone drugs during pregnancy: effect on malformations and cancer E Hemminki, M Gissler and H Toukomaa National Research and Development Centre for Welfare and Health, Health Services Research Unit, PO Box 220, 00531 Helsinki, Finland Summary This study aimed to investigate whether the use of female sex hormone drugs during pregnancy is a risk factor for subsequent breast and other oestrogen-dependent cancers among mothers and their children and for genital malformations in the children. A retrospective cohort of 2052 hormone-drug exposed mothers, 2038 control mothers and their 4130 infants was collected from maternity centres in Helsinki from 1954 to 1963. Cancer cases were searched for in national registers through record linkage. Exposures were examined by the type of the drug (oestrogen, progestin only) and by timing (early in pregnancy, only late in pregnancy). There were no statistically significant differences between the groups with regard to mothers’ cancer, either in total or in specified hormone-dependent cancers. The total number of malformations recorded, as well as malformations of the genitals in male infants, were higher among exposed children. The number of cancers among the offspring was small and none of the differences between groups were statistically significant. The study supports the hypothesis that oestrogen or progestin drug therapy during pregnancy causes malformations among children who were exposed in utero but does not support the hypothesis that it causes cancer later in life in the mother; the power to study cancers in offspring, however, was very low. -

Determination of 17 Hormone Residues in Milk by Ultra-High-Performance Liquid Chromatography and Triple Quadrupole Mass Spectrom
No. LCMSMS-065E Liquid Chromatography Mass Spectrometry Determination of 17 Hormone Residues in Milk by Ultra-High-Performance Liquid Chromatography and Triple Quadrupole No. LCMSMS-65E Mass Spectrometry This application news presents a method for the determination of 17 hormone residues in milk using Shimadzu Ultra-High-Performance Liquid Chromatograph (UHPLC) LC-30A and Triple Quadrupole Mass Spectrometer LCMS- 8040. After sample pretreatment, the compounds in the milk matrix were separated using UPLC LC-30A and analyzed via Triple Quadrupole Mass Spectrometer LCMS-8040. All 17 hormones displayed good linearity within their respective concentration range, with correlation coefficient in the range of 0.9974 and 0.9999. The RSD% of retention time and peak area of 17 hormones at the low-, mid- and high- concentrations were in the range of 0.0102-0.161% and 0.563-6.55% respectively, indicating good instrument precision. Method validation was conducted and the matrix spike recovery of milk ranged between 61.00-110.9%. The limit of quantitation was 0.14-0.975 g/kg, and it meets the requirement for detection of hormones in milk. Keywords: Hormones; Milk; Solid phase extraction; Ultra performance liquid chromatograph; Triple quadrupole mass spectrometry ■ Introduction Since 2008’s melamine-tainted milk scandal, the With reference to China’s national standard GB/T adulteration of milk powder has become a major 21981-2008 "Hormone Multi-Residue Detection food safety concern. In recent years, another case of Method for Animal-derived Food - LC-MS Method", dairy product safety is suspected to cause "infant a method utilizing solid phase extraction, ultra- sexual precocity" (also known as precocious puberty) performance liquid chromatography and triple and has become another major issue challenging the quadrupole mass spectrometry was developed for dairy industry in China. -

Title 16. Crimes and Offenses Chapter 13. Controlled Substances Article 1
TITLE 16. CRIMES AND OFFENSES CHAPTER 13. CONTROLLED SUBSTANCES ARTICLE 1. GENERAL PROVISIONS § 16-13-1. Drug related objects (a) As used in this Code section, the term: (1) "Controlled substance" shall have the same meaning as defined in Article 2 of this chapter, relating to controlled substances. For the purposes of this Code section, the term "controlled substance" shall include marijuana as defined by paragraph (16) of Code Section 16-13-21. (2) "Dangerous drug" shall have the same meaning as defined in Article 3 of this chapter, relating to dangerous drugs. (3) "Drug related object" means any machine, instrument, tool, equipment, contrivance, or device which an average person would reasonably conclude is intended to be used for one or more of the following purposes: (A) To introduce into the human body any dangerous drug or controlled substance under circumstances in violation of the laws of this state; (B) To enhance the effect on the human body of any dangerous drug or controlled substance under circumstances in violation of the laws of this state; (C) To conceal any quantity of any dangerous drug or controlled substance under circumstances in violation of the laws of this state; or (D) To test the strength, effectiveness, or purity of any dangerous drug or controlled substance under circumstances in violation of the laws of this state. (4) "Knowingly" means having general knowledge that a machine, instrument, tool, item of equipment, contrivance, or device is a drug related object or having reasonable grounds to believe that any such object is or may, to an average person, appear to be a drug related object. -

Drug Name Plate Number Well Location % Inhibition, Screen Axitinib 1 1 20 Gefitinib (ZD1839) 1 2 70 Sorafenib Tosylate 1 3 21 Cr
Drug Name Plate Number Well Location % Inhibition, Screen Axitinib 1 1 20 Gefitinib (ZD1839) 1 2 70 Sorafenib Tosylate 1 3 21 Crizotinib (PF-02341066) 1 4 55 Docetaxel 1 5 98 Anastrozole 1 6 25 Cladribine 1 7 23 Methotrexate 1 8 -187 Letrozole 1 9 65 Entecavir Hydrate 1 10 48 Roxadustat (FG-4592) 1 11 19 Imatinib Mesylate (STI571) 1 12 0 Sunitinib Malate 1 13 34 Vismodegib (GDC-0449) 1 14 64 Paclitaxel 1 15 89 Aprepitant 1 16 94 Decitabine 1 17 -79 Bendamustine HCl 1 18 19 Temozolomide 1 19 -111 Nepafenac 1 20 24 Nintedanib (BIBF 1120) 1 21 -43 Lapatinib (GW-572016) Ditosylate 1 22 88 Temsirolimus (CCI-779, NSC 683864) 1 23 96 Belinostat (PXD101) 1 24 46 Capecitabine 1 25 19 Bicalutamide 1 26 83 Dutasteride 1 27 68 Epirubicin HCl 1 28 -59 Tamoxifen 1 29 30 Rufinamide 1 30 96 Afatinib (BIBW2992) 1 31 -54 Lenalidomide (CC-5013) 1 32 19 Vorinostat (SAHA, MK0683) 1 33 38 Rucaparib (AG-014699,PF-01367338) phosphate1 34 14 Lenvatinib (E7080) 1 35 80 Fulvestrant 1 36 76 Melatonin 1 37 15 Etoposide 1 38 -69 Vincristine sulfate 1 39 61 Posaconazole 1 40 97 Bortezomib (PS-341) 1 41 71 Panobinostat (LBH589) 1 42 41 Entinostat (MS-275) 1 43 26 Cabozantinib (XL184, BMS-907351) 1 44 79 Valproic acid sodium salt (Sodium valproate) 1 45 7 Raltitrexed 1 46 39 Bisoprolol fumarate 1 47 -23 Raloxifene HCl 1 48 97 Agomelatine 1 49 35 Prasugrel 1 50 -24 Bosutinib (SKI-606) 1 51 85 Nilotinib (AMN-107) 1 52 99 Enzastaurin (LY317615) 1 53 -12 Everolimus (RAD001) 1 54 94 Regorafenib (BAY 73-4506) 1 55 24 Thalidomide 1 56 40 Tivozanib (AV-951) 1 57 86 Fludarabine -
Efficacy of Ethinylestradiol Re-Challenge for Metastatic Castration-Resistant Prostate Cancer
ANTICANCER RESEARCH 36: 2999-3004 (2016) Efficacy of Ethinylestradiol Re-challenge for Metastatic Castration-resistant Prostate Cancer TAKEHISA ONISHI1, TAKUJI SHIBAHARA1, SATORU MASUI1, YUSUKE SUGINO1, SHINICHIRO HIGASHI1 and TAKESHI SASAKI2 1Department of Urology, Ise Red Cross hospital, Ise, Japan; 2Department of Urology, Mie University Graduate School of Medicine, Tsu, Japan Abstract. Background: There has recently been renewed corticosteroids, estrogens, sipuleucel T and, more recently, interest in the use of estrogens as a treatment strategy for CYP17 inhibitor (abirateron acetate) and androgen castration-resistant prostate cancer (CRPC). The purpose of receptor antagonist (enzaltamide) (2-7). Treatment with this study was to evaluate the feasibility and efficacy of estrogens was used as a palliative therapy for advanced ethinylestradiol re-challenge (re-EE) in the management of prostate cancer, however, the discovery of luteinizing CRPC. Patients and Methods: Patients with metastatic CRPC hormone-releasing hormone (LH-RH) agonists led them to who received re-EE after disease progression on prior EE become less common and they stopped being used in most and other therapy were retrospectively reviewed for prostate- countries in the 1980s (8). One of the reasons for reduction specific antigen (PSA) response, PSA progression-free in their use is the risk of cardiovascular and survival (P-PFS) and adverse events. Results: Thirty-six re- thromboembolic events during therapy. However, several EE treatments were performed for 20 patients. PSA response reports demonstrated the positive oncological results of to the initial EE treatment was observed in 14 (70%) patients. therapy with estrogens, such as diethylstilbestrol (DES) PSA response to re-EE was 33.3% in 36 re-EE treatments. -

Hormone Replacement Therapy and Osteoporosis
This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or a basis for reimbursement and coverage policies. AHRQ or U.S. Department of Health and Human Services endorsement of such derivative products may not be stated or implied. AHRQ is the lead Federal agency charged with supporting research designed to improve the quality of health care, reduce its cost, address patient safety and medical errors, and broaden access to essential services. AHRQ sponsors and conducts research that provides evidence-based information on health care outcomes; quality; and cost, use, and access. The information helps health care decisionmakers— patients and clinicians, health system leaders, and policymakers—make more informed decisions and improve the quality of health care services. Systematic Evidence Review Number 12 Hormone Replacement Therapy and Osteoporosis Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 2101 East Jefferson Street Rockville, MD 20852 http://www.ahrq.gov Contract No. 290-97-0018 Task Order No. 2 Technical Support of the U.S. Preventive Services Task Force Prepared by: Oregon Health Sciences University Evidence-based Practice Center, Portland, Oregon Heidi D. Nelson, MD, MPH August 2002 Preface The Agency for Healthcare Research and Quality (AHRQ) sponsors the development of Systematic Evidence Reviews (SERs) through its Evidence-based Practice Program. With guidance from the third U.S. Preventive Services Task Force∗ (USPSTF) and input from Federal partners and primary care specialty societies, two Evidence-based Practice Centers—one at the Oregon Health Sciences University and the other at Research Triangle Institute-University of North Carolina—systematically review the evidence of the effectiveness of a wide range of clinical preventive services, including screening, counseling, immunizations, and chemoprevention, in the primary care setting.