“A Prospective Study of Non-Malignant Lesions of Larynx”
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pathology of Head and Neck
Pathology of Head and Neck • Pathology of Oral cavity • Pathology of Nose, and Nasopharynx • Pathology of Larynx • Pathology of Neck • Pathology of Salivary gland ผูชวยศาสตราจารย แพทยหญิง จุลินทร สําราญ Pathology of Oral cavity Inflammations and infections • Inflammations and infections • Herpes simplex virus infections • Reactive lesions • Aphthous ulcer ( Canker sores ) • Oral manifestations of systemic disease • Oral candidiasis ( Thrush ) • Glossitis • Tumors and precancerous lesions • Xerostomia 1 Herpes simplex virus infections • Etiology ; HSV1 • Clinical feature ; – Acute herpetic gingivostomatitis in young children , severe diffuse involvement of the oral and pharyngeal mucosa, tongue and gingiva ,and spontaneously clear in 3-4 weeks • Morphology – Recurrent herpetic stomatitis in young adult , – Gross ; Small vesicles to bullae painful, red- milder form involving lip, nasal orifices and buccal rimmed, shallow ulceration mucosa and spontaneously clear in 1-2 weeks – Histo ; Acantholysis and presence of intranuclear inclusion with multinucleated giant cells 2 Aphthous ulcer ( Canker sores ) • Morphology ; – Gross ; single or multiple, shallow, hyperemic ulceration with red-rimmed and thin exudate covering – Histo ; mainly mononuclear cell infiltration • Common superficial ulceration of oral mucosa and neutrophilic infiltration when has • Most in first decade of life secondary bacterial infection • Clinical feature; painful and recurrent ulceration and clear within a week Oral candidiasis ( Thrush ) • The most common fungal infection -
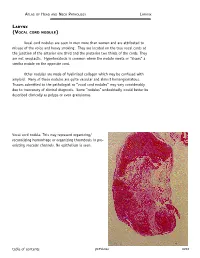
Larynx (Vocal Cord Nodule)
ATLAS OF HEAD AND NECK PATHOLOGY LARYNX LARYNX (VOCAL CORD NODULE) Vocal cord nodules are seen in men more than women and are attributed to misuse of the voice and heavy smoking. They are located on the true vocal cords at the junction of the anterior one third and the posterior two thirds of the cords. They are not neoplastic. Hyperkeratosis is common where the nodule meets or “kisses” a similar nodule on the opposite cord. Other nodules are made of hyalinized collagen which may be confused with amyloid. Many of these nodules are quite vascular and almost hemangiomatous. Tissues submitted to the pathologist as “vocal cord nodules” may vary considerably due to inaccuracy of clinical diagnosis. Some “nodules” undoubtedly would better be described clinically as polyps or even granulomas. Vocal cord nodule. This may represent organizing/ recanalizing hemorrhage or organizing thrombosis in pre- existing vascular channels. No epithelium is seen. table of contents previous next ATLAS OF HEAD AND NECK PATHOLOGY LARYNX Vocal cord nodule, similar to the prior nodule. Recent hemorrhage and granulation tissue (double arrows) cov- ered with thick layer of squamous epithelium (arrow) and some keratin (triangle). Laryngeal papilloma. This specimen was submitted as a “nodule” but represents a laryngeal squamous papilloma of the human papilloma virus type and likely will recur. Koilocytosis is indicated by arrow. It is not what the clinician or pathologist would call a vocal cord nodule. table of contents previous next ATLAS OF HEAD AND NECK PATHOLOGY LARYNX Vocal cord nodule. Epithelium of a vocal cord nodule typically shows no dysplasia and a distinct basement membrane. -

1 K. J. Lee: Essential Otolaryngology and Head and Neck Surgery (Iiird Ed) Chapter 15: the Larynx Embryology of the Larynx (See
K. J. Lee: Essential Otolaryngology and Head and Neck Surgery (IIIrd Ed) Chapter 15: The Larynx Embryology of the Larynx (see Chap. 11, pages 306-310) Anatomy Anatomy The larynx consists of a framework of cartilages, held in position by an intrinsic and extrinsic musculature, and lined by mucous membrane which is arranged in characteristic folds. The larynx is situated in front of the fourth, fifth, and sixth cervical vertebrae. The upper portion of the larynx, which is continuous with the pharynx above, is almost triangular in shape; the lower portion leading into trachea presents a circular appearance. Laryngeal Cartilages The laryngeal cartilages form the main framework of the larynx and consist of: 1. Thyroid cartilage (unpaired). 2. Cricoid cartilage (unpaired). 3. Epiglottis (unpaired). 4. Arytenoid cartilage (paired). 5. Corniculate cartilage (paired). 6. Cuneiform cartilage (paired). Thyroid Cartilage The thyroid cartilage (hyaline cartilage) is the largest and encloses the larynx anteriorly and laterally, thus shielding it from all but the most forceful blows. This cartilage is composed of two alae which meet anteriorly, dipping down from above to form the thyroid notch before meeting at the protuberance of the Adam's apple. Posteriorly, each wing has a superior cornu, extending upward about 2 cm, and a much shorter inferior cornu which articulates with the cricoid cartilage below. This is the only direct articulation of the thyroid cartilage, all other relationships with contiguous structures being maintained by muscles or ligaments. Cricoid Cartilage The cricoid cartilage (hyaline cartilage) lies directly below the thyroid cartilage. It is the strongest of the laryngeal cartilages, and is shaped like a signet ring. -

A Study of Stroboscopic Parameters in Vocal Cord Pathologies
Original Research Article A study of stroboscopic parameters in vocal cord pathologies Sheetal Shelke1, Nilam Sathe2, Hetal Marfatia3, Asmita Madhavi4* 1Assistant Professor, Department of ENT, MIMSR Medical College, Latur, INDIA. 2Associate Professor, 2Professor, 3Assistant Professor, Department of ENT, Seth G.S. Medical College, Mumbai, INDIA. Email: [email protected] Abstract Background: Speech is one of the unique qualities that sets man apart from all other living organism. Voice disorders isolate a person from the society but could also have deep impact on emotional and occupational aspect of life. Stroboscopy has evolved as the most practical and useful technique for the clinical evaluation of the visco-elastic properties of the phonatory mucosa. It provides useful, real-time information concerning the nature of vibration, an image to detect vocal pathology, and a permanent video record of the examination. Aim: To study the stroboscopic parameters in vocal cord pathologies. Material and Methods: A total of 30 cases (18-60 years) presented with complaints of change in voice and hoarseness of voice in Department of ENT, KEM Hospital Mumbai were examined. Stroboscopic examination was carried for these patients. All parameters of stroboscopy including symmetry, amplitude of vibration, mucosal wave, glottis closure and periodicity were observed in these patients. Results: All patients those had vocal cord cysts (2) and polyps (6) underwent microlaryngoscopic surgery showed symmetry of vocal cords in all patients (100%). Increased in amplitude was not observed in any patient. Vocal cord mucosal wave was normal in all patients with sulcus (2), vocal cord palsy (5), spasmodic dysphonia (1) and anterior commissure web (1). -

Biphasic Stridor Related to a Congenital Vallecular Cyst Konjenital Vallekula Kisti Ile İlgili Bifazik Stridor
DOI: 10.4274/atfm.galenos.2019.25743 CASE REPORT / OLGU SUNUMU Journal of Ankara University Faculty of Medicine 2019;72(3):367-369 DAHİLİ TIP BİLİMLERİ / INTERNAL MEDICAL MEDICINE Biphasic Stridor Related to a Congenital Vallecular Cyst Konjenital Vallekula Kisti ile İlgili Bifazik Stridor Fatih Günay1, Nisa Eda Çullas İlarslan1, Serhan Özcan2, Tanıl Kendirli2, Alican Akaslan3, Süha Beton3, Nazan Çobanoğlu4 1Ankara University Faculty of Medicine, Department of Pediatrics, Ankara, Turkey 2Ankara University Faculty of Medicine, Department of Pediatrics, Division of Pediatric Intensitive Care, Ankara, Turkey 3Ankara University Faculty of Medicine, Department of Otolaryngology, Ankara, Turkey 4Ankara University Faculty of Medicine, Department of Pediatrics, Division of Pediatric Pulmonology, Ankara, Turkey Abstract Congenital vallecular cyst (VC) is a rare but potentially fatal pathology in neonates and infants. It usually manifests with symptoms such as stridor, apnea and cyanosis that develop shortly after birth. Stridor is the most common encountered symptom. VC is frequently accompanied by laryngomalacia (LM) and LM is the most common cause of stridor in infants. Diagnosis can be made by flexible laryngoscopy or bronchoscopy. Surgery is the mainstay for VC treatment. Here we present an infant who had respiratory distress, biphasic stridor and cyanosis worsened during feeding and crying, and diagnosed VC. The respiratory symptoms of the patient recovered rapidly after surgical resection. Key Words: Flexible Bronchoscopy, Infant, Respiratory Distress, Stridor, Vallecular Cyst Öz Konjenital vallekula kisti (VK) yenidoğanlarda ve bebeklerde nadir görülen ancak potansiyel olarak ölümcül bir patolojidir. Genellikle doğumdan kısa bir süre sonra ortaya çıkan stridor, apne ve siyanoz gibi semptomlarla kendini gösterir. Stridor en sık karşılaşılan semptomdur. -

Congenital Laryngeal Cyst
Global Journal of Otolaryngology ISSN 2474-7556 Case Report Glob J Otolaryngol Volume 20 Issue 2 - June 2019 Copyright © All rights are reserved by Khdim Mouna DOI: 10.19080/GJO.2019.20.556032 Congenital Laryngeal Cyst Khdim Mouna*, Douimi Loubna, Choukry Karim, Rouadi Sami, Abada Reda, Roubal Mohammed and Mahtar Mohammed EN Department 20 august 1953 Hospital, Casablanca, Morocco Submission: May 24, 2019; Published: June 04, 2019 *Corresponding author: Khdim Mouna, EN Department 20 august 1953 Hospital, Casablanca, Morocco Abstract Benign congenital laryngeal cysts are a rare clinical entity, with potential for severe airway obstruction, leading sometimes to severe In this report, a 10-month-old infant with a severe respiratory distress caused by congenital laryngeal cyst is presented. respiratory distress and death. They oftenly arise from the vallecula, the aryepiglottic fold, and the saccule ventricle, and rarely from the epiglottis. Keywords: Congenital Laryngeal Cyst; Respiratory Distress; Stridor Introduction Congenital laryngeal cysts are rare, but easily managed once the diagnosis is made. Delay in making a correct diagnosis may lead to serious and fatal consequences. Clinical presentation consists of inspiratory stridor, and varying degrees of upper airway obstruction that usually present soon after birth or during by laryngoscopy. In fact, there is no consensus on the optimal the first weeks or mouths of life. They are usually diagnosed treatment, however several surgical procedures are proposed: endoscopic excision, needle aspiration, de-roofing, external describes the case of 10 mouths year old infant with a severe laryngofissure, and lateral pharyngotomy. The following report airway distress and stridor caused by a congenital laryngeal cyst. -

The Impact of Gastroesophageal Reflux in the ENT Pathology
Romanian Journal of Rhinology, Vol. 6, No. 23, July - September 2016 DOI: 10.1515/rjr-2016-0016 LITERATURE REVIEW The impact of gastroesophageal reflux in the ENT pathology Violeta Melinte1,2,3, Codrut Sarafoleanu1,2,3 1“Carol Davila” University of Medicine and Pharmacy, Bucharest, Romania 2CESITO Centre, “Sfanta Maria” Hospital, Bucharest, Romania 3ENT&HNS Department, “Sfanta Maria” Hospital, Bucharest, Romania ABSTRACT Frequently encountered in medical practice, the gastroesophageal reflux (GER) is a chronic condition characterized by the passage of gastric acid or gastric contents into the esophagus. In otorhinolaryngology, the diagnosis of pharyngo-laryngeal or rhinosinusal inflammatory conditions secondary to GER is one of exclusion and it is based on a detailed anamnesis in which we are interested in symptoms, behavioural and medical risk factors, on the ENT clinical examination, the laryngo-fibroscop- ical assessment, the phoniatric examination, the barite pharyngo-esogastric exam, the upper gastrointestinal endoscopy and the esophageal manometry. The authors are making a systematization of the contribution of the gastroesophageal reflux has in the ENT pathology, em- phasising the sympytoms and the most frequent associated pathological entities. KEYWORDS: gastroesophageal reflux, extraesophageal reflux, chronic laryngitis, rhinosinusitis, post nasal drip INTRODUCTION crease in incidence in adults over 40 years can be no- ticed4. Frequently encountered in medical practice, the Between 6 and 10% of patients presenting in an gastroesophageal reflux is a chronic condition charac- ENT service are diagnosed with gastroesophageal re- terized by the passage of gastric acid or gastric con- flux. In 1995, Rival et al. found that 73% of patients * tents into the esophagus, without being accompanied with various complaints in the cervical region (n=216) by nausea or vomiting. -

Original Article Hoarseness of Voice
Bangladesh J Otorhinolaryngol 2017; 23(1): 47-51 Original Article Hoarseness of Voice : An Etiological Study Salah Uddin Ahmmed1, AKM Asaduzzaman2, Mohammed Ahmed Ahsan3, Md Zakir Hossain2, Mohammad Ali Azad2, Mohammed Iftekharul Alam2 Abstract: Hoarseness of voice is one of the commonest symptom in otolaryngological practice and it indicates diseases ranging from totally benign condition to the most malignant condition. The aim of this study was to analyze clinical profile, to find out common etiological factors and association of common predisposing factors leading to hoarseness of voice. The study was carried out in the department of ENT, CMB, BAF Dhaka, from February 2014 to July 2016. A total of 130 patients having hoarseness of voice were selected coming to the OPD. All the patients then underwent a detailed history, ENT examinations and investigations to reach a diagnosis. Out of total 130 patients 76(58.47 %) were males and 54 (41.53) were females. Male predominance was observed with male female ratio of 1.49: 1. Common age group involved was 31- 40 years in 29 (20.7%) cases. Common etiology included chronic laryngitis in 37 (28.46%) cases, vocal nodules in 20 (15.38%), vocal cord polyp in 18 (13.84%), acute laryngitis in 10 (7.69%), vocal cord cyst in 9 (6.92%), hypothyroidism in 7 (5.38%) and Carcinoma larynx in 6 (4.61%) patients. Most of the etiopathological factors found in this study were treatable disease. So, early diagnosis can reduce the morbidity and mortality. Key words: Hoarseness of Voice, aetiology, fiber optic laryngoscopy. Introduction: or lower pitch. -

Is It Possible to Say Gastroesophageal Reflux Disease and Laryngopharyngeal Reflux Are Different?
Global Journal of Otolaryngology ISSN 2474-7556 Research Article Glob J Otolaryngol Volume 16 Issue 3 - June 2018 Copyright © All rights are reserved by Ergun Sevil DOI: 10.19080/GJO.2018.16.555938 Is it Possible to Say Gastroesophageal Reflux Disease and Laryngopharyngeal Reflux are Different? Ergun Sevil1*, Togay Muderris2 and Muzaffer Kiris3 1Department of Otorhinolaryngology, Karaman State Hospital, Turkey 2Department of Otorhinolaryngology, Bozyaka Training and Research Hospital, Turkey 3Department of Otorhinolaryngology, Gulhane Training and Research Hospital, Turkey Submission: June 11, 2018; Published: June 27, 2018 *Corresponding author: Ergun Sevil, Karaman State Hospital, Department of Otorhinolaryngology Head and Neck Surgery, 70000, Karaman, Turkey, Fax:903382263309, Tel: ; Email: Abstract Objective: Methods: To find out the differences and similarities between these two diseases in the aspect of symptoms and findings. We compared symptoms and laryngeal findings of 110 patients with laryngopharyngeal complaints and physical findings suggesting laryngopharyngeal reflux LPR (LPR group) and 86 patients who underwent esophagogastroscopy and diagnosed as lower esophageal sphincterResults: (LES) incompetency and/or esophagitis (Gastroesophageal reflux disease (GERD) group). The most common complaints in LPR group were hoarseness in 98 (89%) patients, chronic throat clearing in 96 (87.2%) patients, sore throat in 92 (83.9%) patients, globus in 82 (74.5%) patients and dysphagia in 78 (70.9%) patients. In GERD group, common complaints -

Ent Superbill Daniel Todd, Md, Facs Facility: Svh Mck Sfsc Va Clinic
ENT SUPERBILL DANIEL TODD, MD, FACS FACILITY: SVH MCK SFSC VA CLINIC PT NAME_______________________________________ DOB_____________________________ DATE____________________________ NEW PATIENT EST PATIENT LOW 99202 LOW 99212 MED 99203 MOD 99213 HIGH 99204 HIGH 99214 OUT PATIENT CONSULT INPATIENT CONSULT IN CONSULT SUBSEQUENT LOW 99242 MEDIUM 99252 LOW 99231 MODERATE 99243 HIGH 99253 MEDIUM 99232 HIGH 99244 COMPLEX 99254 HIGH 99233 HOSPITAL ADMISSIONS HOSPITAL SUBSEQUENT HOSPITAL DISCHARGE LOW 99221 LOW 99231 LOW 99238 MEDIUM 99222 MEDIUM 99232 HIGH 99239 HIGH 99223 HIGH 99233 NASAL PROCEDURES ORAL/PHARYNX EAR PROCEDURES SKIN BIOPSY 11100 TONGUE BX 41110 CERUMEN 69210 EXC BENIGN <0.5 11440 VEST BX 40808 EXT EAR BX 69100 EXC CANCER <0.5 11640 FOM BX 41116 EXC LESION EAR 69110 COMPLEX REPAIR 13150 OP BX 42800 EAC LESION EXC 69145 RIDGID ENDO 31231 LIP BX 40490 MASTOID CLEAN 69220 FDE 31276 DL 31525 PET 69436 SEPTO 30520 DL WITH MICRO 31526 REMOVAL PET 69424 TE 31255 DL/MICRO/BX 31536 T-PLASTY 69631/20926-59 MA WITH TISSUE 31267 DL/MICRO/EXC 31541 TYMPMASTIOD 69641 AE 31254 FRENULOPLAST 41520 MYRINGOTOMY 69421 SPHENOID 31287 FLEXIBLE 31575 STAPES 69660 MA 31256 BRONCH 31622 MICRODISSECT 69990 SUBMUC TURB 30140 ESOPH 43200 MEE 69440 CONCHA BULL 31240 T&A <12 42820 NECK PROCEDURES POLYP/DEBRIDE 31237 T&A >12 42821 NECK NODE 38510 SEPTORHINO 30420 TONSIL >12 42826 NECK DISSECT. 38724 RHINO 30410 UP3 42145 SUBMAX 42440 NASAL VALVE 30465 ADENOID <12 42830 SUP. PAROTID 42415 OPEN RED FX 21335 ADENOID >12 42831 SUPRAHYOID 38700 SEPTAL GRAFT 20912(spreaders) -

Identification and Remediation of Pediatric Fluency and Voice
ORIGINAL ARTICLE Identification and P Remediation of H Pediatric Fluency C and Voice Disorders Barbara M. Baker, PhD, CCC-SLP, & Patricia B. Blackwell, PhD, CCC-SLP When children cannot communicate well, the difficulty often is because they have articulation or language disorders, but other difficulties also may adversely affect children’s abilities to express themselves. Prob- lems with fluency (stuttering or cluttering) and voice quality can impair communication. Pediatric nurse practitioners need to be prepared to re- spond to parents’ questions about voice and fluency issues and, when appropriate, to make referrals for evaluation and possible treatment. This article presents a basic overview of the nature of fluency and voice disorders and provides guidelines for identifying children who should be referred, and to whom. ABSTRACT FLUENCY DISORDERS Early identification of pediatric dis- fluency and voice disorders is advis- Two different terms relate to fluency disorders. The more frequent and best able because these disorders may known is stuttering, which may include repetitions of words or parts of progress to lifelong communicative words, prolongations of sounds, and/or the temporary blockage of speech. impairments if left untreated. Espe- A second type of disfluency, cluttering, occurs far less frequently than cially with disfluency or stuttering, it stuttering, and results in speech that is “rapid, dysrhythmic, sporadic, is critical that an informed differen- unorganized, and frequently unintelligible” (Daly, 1992, p. 107). Arapid rate tial diagnosis be made to determine and lack of organization of ideas distinguishes cluttering from stuttering. whether a speech pattern represents Because stuttering is considerably more common, with a prevalence of normal disfluency or actual stutter- approximately 1% of the pediatric population (Guitar, 1998), it will be the ing. -

PDF Hosted at the Radboud Repository of the Radboud University Nijmegen
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. https://hdl.handle.net/2066/226629 Please be advised that this information was generated on 2021-09-26 and may be subject to change. OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY NECK AND HEAD AND LARYNGOLOGY IN SURGERY ENDOSCOPIC OFFICE-BASED OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY IMPROVING QUALITY OF CARE AND EFFICIENCY THROUGH INNOVATIVE TECHNIQUES DAVID WELLENSTEIN J. DAVID DAVID J. WELLENSTEIN OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY NECK AND HEAD AND LARYNGOLOGY IN SURGERY ENDOSCOPIC OFFICE-BASED OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY IMPROVING QUALITY OF CARE AND EFFICIENCY THROUGH INNOVATIVE TECHNIQUES DAVID WELLENSTEIN J. DAVID DAVID J. WELLENSTEIN OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY IMPROVING QUALITY OF CARE AND EFFICIENCY THROUGH INNOVATIVE TECHNIQUES David J. Wellenstein 549724-L-sub01-bw-Wellenstein Processed on: 21-10-2020 PDF page: 1 Office-based endoscopic surgery in laryngology and head and neck oncology Improving quality of care and efficiency through innovative techniques David Jonathan Wellenstein ISBN XXXX Copyright © David J. Wellenstein, 2020 Design by Bregje Jaspers, ProefschriftOntwerp.nl Printed by Ipskamp drukkers Printing of this thesis was financially supported by: Pentax Medical, Soluvos Medical, Lumenis, Medical Disposables Store, Laservision, Mylan, Atos Medical, ALK and Radboud university medical center/Radboud University Nijmegen 549724-L-sub01-bw-Wellenstein Processed on: 21-10-2020 PDF page: 2 OFFICE-BASED ENDOSCOPIC SURGERY IN LARYNGOLOGY AND HEAD AND NECK ONCOLOGY IMPROVING QUALITY OF CARE AND EFFICIENCY THROUGH INNOVATIVE TECHNIQUES Proefschrift ter verkrijging van de graad van doctor aan de Radboud Universiteit Nijmegen op gezag van de rector magnificus prof.