Additional Tables.Xlsx
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Implications in Parkinson's Disease
Journal of Clinical Medicine Review Lysosomal Ceramide Metabolism Disorders: Implications in Parkinson’s Disease Silvia Paciotti 1,2 , Elisabetta Albi 3 , Lucilla Parnetti 1 and Tommaso Beccari 3,* 1 Laboratory of Clinical Neurochemistry, Department of Medicine, University of Perugia, Sant’Andrea delle Fratte, 06132 Perugia, Italy; [email protected] (S.P.); [email protected] (L.P.) 2 Section of Physiology and Biochemistry, Department of Experimental Medicine, University of Perugia, Sant’Andrea delle Fratte, 06132 Perugia, Italy 3 Department of Pharmaceutical Sciences, University of Perugia, Via Fabretti, 06123 Perugia, Italy; [email protected] * Correspondence: [email protected] Received: 29 January 2020; Accepted: 20 February 2020; Published: 21 February 2020 Abstract: Ceramides are a family of bioactive lipids belonging to the class of sphingolipids. Sphingolipidoses are a group of inherited genetic diseases characterized by the unmetabolized sphingolipids and the consequent reduction of ceramide pool in lysosomes. Sphingolipidoses include several disorders as Sandhoff disease, Fabry disease, Gaucher disease, metachromatic leukodystrophy, Krabbe disease, Niemann Pick disease, Farber disease, and GM2 gangliosidosis. In sphingolipidosis, lysosomal lipid storage occurs in both the central nervous system and visceral tissues, and central nervous system pathology is a common hallmark for all of them. Parkinson’s disease, the most common neurodegenerative movement disorder, is characterized by the accumulation and aggregation of misfolded α-synuclein that seem associated to some lysosomal disorders, in particular Gaucher disease. This review provides evidence into the role of ceramide metabolism in the pathophysiology of lysosomes, highlighting the more recent findings on its involvement in Parkinson’s disease. Keywords: ceramide metabolism; Parkinson’s disease; α-synuclein; GBA; GLA; HEX A-B; GALC; ASAH1; SMPD1; ARSA * Correspondence [email protected] 1. -

Understanding the Molecular Pathobiology of Acid Ceramidase Deficiency
Understanding the Molecular Pathobiology of Acid Ceramidase Deficiency By Fabian Yu A thesis submitted in conformity with the requirements for the degree of Doctor of Philosophy Institute of Medical Science University of Toronto © Copyright by Fabian PS Yu 2018 Understanding the Molecular Pathobiology of Acid Ceramidase Deficiency Fabian Yu Doctor of Philosophy Institute of Medical Science University of Toronto 2018 Abstract Farber disease (FD) is a devastating Lysosomal Storage Disorder (LSD) caused by mutations in ASAH1, resulting in acid ceramidase (ACDase) deficiency. ACDase deficiency manifests along a broad spectrum but in its classical form patients die during early childhood. Due to the scarcity of cases FD has largely been understudied. To circumvent this, our lab previously generated a mouse model that recapitulates FD. In some case reports, patients have shown signs of visceral involvement, retinopathy and respiratory distress that may lead to death. Beyond superficial descriptions in case reports, there have been no in-depth studies performed to address these conditions. To improve the understanding of FD and gain insights for evaluating future therapies, we performed comprehensive studies on the ACDase deficient mouse. In the visual system, we reported presence of progressive uveitis. Further tests revealed cellular infiltration, lipid buildup and extensive retinal pathology. Mice developed retinal dysplasia, impaired retinal response and decreased visual acuity. Within the pulmonary system, lung function tests revealed a decrease in lung compliance. Mice developed chronic lung injury that was contributed by cellular recruitment, and vascular leakage. Additionally, we report impairment to lipid homeostasis in the lungs. ii To understand the liver involvement in FD, we characterized the pathology and performed transcriptome analysis to identify gene and pathway changes. -

PEX5 Regulates Autophagy Via the Mtorc1-TFEB Axis During Starvation
Eun et al. Experimental & Molecular Medicine (2018) 50:4 DOI 10.1038/s12276-017-0007-8 Experimental & Molecular Medicine ARTICLE Open Access PEX5 regulates autophagy via the mTORC1-TFEB axis during starvation So Young Eun1,JoonNoLee2,In-KooNam2, Zhi-qiang Liu1,Hong-SeobSo 1, Seong-Kyu Choe1 and RaeKil Park2 Abstract Defects in the PEX5 gene impair the import of peroxisomal matrix proteins, leading to nonfunctional peroxisomes and other associated pathological defects such as Zellweger syndrome. Although PEX5 regulates autophagy process in a stress condition, the mechanisms controlling autophagy by PEX5 under nutrient deprivation are largely unknown. Herein, we show a novel function of PEX5 in the regulation of autophagy via Transcription Factor EB (TFEB). Under serum-starved conditions, when PEX5 is depleted, the mammalian target of rapamycin (mTORC1) inhibitor TSC2 is downregulated, which results in increased phosphorylation of the mTORC1 substrates, including 70S6K, S6K, and 4E- BP-1. mTORC1 activation further suppresses the nuclear localization of TFEB, as indicated by decreased mRNA levels of TFEB, LIPA, and LAMP1. Interestingly, peroxisomal mRNA and protein levels are also reduced by TFEB inactivation, indicating that TFEB might control peroxisome biogenesis at a transcriptional level. Conversely, pharmacological inhibition of mTOR resulting from PEX5 depletion during nutrient starvation activates TFEB by promoting nuclear localization of the protein. In addition, mTORC1 inhibition recovers the damaged-peroxisome biogenesis. These data suggest that PEX5 may be a critical regulator of lysosomal gene expression and autophagy through the mTOR-TFEB- autophagy axis under nutrient deprivation. 1234567890():,; 1234567890():,; Introduction Mitochondrial antiviral-signaling protein (MAVS) func- Peroxisome is an essential cellular organelle for per- tions as an antiviral signaling platform to induce the forming various metabolic activities, including oxidation interferon-independent signaling pathways4. -

GM2 Gangliosidoses: Clinical Features, Pathophysiological Aspects, and Current Therapies
International Journal of Molecular Sciences Review GM2 Gangliosidoses: Clinical Features, Pathophysiological Aspects, and Current Therapies Andrés Felipe Leal 1 , Eliana Benincore-Flórez 1, Daniela Solano-Galarza 1, Rafael Guillermo Garzón Jaramillo 1 , Olga Yaneth Echeverri-Peña 1, Diego A. Suarez 1,2, Carlos Javier Alméciga-Díaz 1,* and Angela Johana Espejo-Mojica 1,* 1 Institute for the Study of Inborn Errors of Metabolism, Faculty of Science, Pontificia Universidad Javeriana, Bogotá 110231, Colombia; [email protected] (A.F.L.); [email protected] (E.B.-F.); [email protected] (D.S.-G.); [email protected] (R.G.G.J.); [email protected] (O.Y.E.-P.); [email protected] (D.A.S.) 2 Faculty of Medicine, Universidad Nacional de Colombia, Bogotá 110231, Colombia * Correspondence: [email protected] (C.J.A.-D.); [email protected] (A.J.E.-M.); Tel.: +57-1-3208320 (ext. 4140) (C.J.A.-D.); +57-1-3208320 (ext. 4099) (A.J.E.-M.) Received: 6 July 2020; Accepted: 7 August 2020; Published: 27 August 2020 Abstract: GM2 gangliosidoses are a group of pathologies characterized by GM2 ganglioside accumulation into the lysosome due to mutations on the genes encoding for the β-hexosaminidases subunits or the GM2 activator protein. Three GM2 gangliosidoses have been described: Tay–Sachs disease, Sandhoff disease, and the AB variant. Central nervous system dysfunction is the main characteristic of GM2 gangliosidoses patients that include neurodevelopment alterations, neuroinflammation, and neuronal apoptosis. Currently, there is not approved therapy for GM2 gangliosidoses, but different therapeutic strategies have been studied including hematopoietic stem cell transplantation, enzyme replacement therapy, substrate reduction therapy, pharmacological chaperones, and gene therapy. -

Assessment of a Targeted Gene Panel for Identification of Genes Associated with Movement Disorders
Supplementary Online Content Montaut S, Tranchant C, Drouot N, et al; French Parkinson’s and Movement Disorders Consortium. Assessment of a targeted gene panel for identification of genes associated with movement disorders. JAMA Neurol. Published online June 18, 2018. doi:10.1001/jamaneurol.2018.1478 eMethods. Supplemental methods. eTable 1. Name, phenotype and inheritance of the genes included in the panel. eTable 2. Probable pathogenic variants identified in a cohort of 23 patients with cerebellar ataxia using WES analysis. eTable 3. Negative cases in a cohort of 23 patients with cerebellar ataxia studied using WES analysis. eTable 4. Variants of unknown significance (VUSs) identified in the cohort. eFigure 1. Examples of pedigrees of cases with identified causative variants. eFigure 2. Pedigrees suggesting mendelian inheritance in negative cases. eFigure 3. Examples of pedigrees of cases with identified VUSs. eResults. Supplemental results. This supplementary material has been provided by the authors to give readers additional information about their work. © 2018 American Medical Association. All rights reserved. Downloaded From: https://jamanetwork.com/ on 10/02/2021 eMethods. Supplemental methods Patients selection In the multicentric, prospective study, patients were selected from 25 French, 1 Luxembourg and 1 Algerian tertiary MDs centers between September 2014 and July 2016. Inclusion criteria were patients (1) who had developed one or several chronic MDs (2) with an age of onset below 40 years and/or presence of a family history of MDs. Patients suffering from essential tremor, tic or Gilles de la Tourette syndrome, pure cerebellar ataxia or with clinical/paraclinical findings suggestive of an acquired cause were excluded. -

Peroxisomal Disorders and Their Mouse Models Point to Essential Roles of Peroxisomes for Retinal Integrity
International Journal of Molecular Sciences Review Peroxisomal Disorders and Their Mouse Models Point to Essential Roles of Peroxisomes for Retinal Integrity Yannick Das, Daniëlle Swinkels and Myriam Baes * Lab of Cell Metabolism, Department of Pharmaceutical and Pharmacological Sciences, KU Leuven, 3000 Leuven, Belgium; [email protected] (Y.D.); [email protected] (D.S.) * Correspondence: [email protected] Abstract: Peroxisomes are multifunctional organelles, well known for their role in cellular lipid homeostasis. Their importance is highlighted by the life-threatening diseases caused by peroxisomal dysfunction. Importantly, most patients suffering from peroxisomal biogenesis disorders, even those with a milder disease course, present with a number of ocular symptoms, including retinopathy. Patients with a selective defect in either peroxisomal α- or β-oxidation or ether lipid synthesis also suffer from vision problems. In this review, we thoroughly discuss the ophthalmological pathology in peroxisomal disorder patients and, where possible, the corresponding animal models, with a special emphasis on the retina. In addition, we attempt to link the observed retinal phenotype to the underlying biochemical alterations. It appears that the retinal pathology is highly variable and the lack of histopathological descriptions in patients hampers the translation of the findings in the mouse models. Furthermore, it becomes clear that there are still large gaps in the current knowledge on the contribution of the different metabolic disturbances to the retinopathy, but branched chain fatty acid accumulation and impaired retinal PUFA homeostasis are likely important factors. Citation: Das, Y.; Swinkels, D.; Baes, Keywords: peroxisome; Zellweger; metabolism; fatty acid; retina M. Peroxisomal Disorders and Their Mouse Models Point to Essential Roles of Peroxisomes for Retinal Integrity. -

Supplementary Table S4. FGA Co-Expressed Gene List in LUAD
Supplementary Table S4. FGA co-expressed gene list in LUAD tumors Symbol R Locus Description FGG 0.919 4q28 fibrinogen gamma chain FGL1 0.635 8p22 fibrinogen-like 1 SLC7A2 0.536 8p22 solute carrier family 7 (cationic amino acid transporter, y+ system), member 2 DUSP4 0.521 8p12-p11 dual specificity phosphatase 4 HAL 0.51 12q22-q24.1histidine ammonia-lyase PDE4D 0.499 5q12 phosphodiesterase 4D, cAMP-specific FURIN 0.497 15q26.1 furin (paired basic amino acid cleaving enzyme) CPS1 0.49 2q35 carbamoyl-phosphate synthase 1, mitochondrial TESC 0.478 12q24.22 tescalcin INHA 0.465 2q35 inhibin, alpha S100P 0.461 4p16 S100 calcium binding protein P VPS37A 0.447 8p22 vacuolar protein sorting 37 homolog A (S. cerevisiae) SLC16A14 0.447 2q36.3 solute carrier family 16, member 14 PPARGC1A 0.443 4p15.1 peroxisome proliferator-activated receptor gamma, coactivator 1 alpha SIK1 0.435 21q22.3 salt-inducible kinase 1 IRS2 0.434 13q34 insulin receptor substrate 2 RND1 0.433 12q12 Rho family GTPase 1 HGD 0.433 3q13.33 homogentisate 1,2-dioxygenase PTP4A1 0.432 6q12 protein tyrosine phosphatase type IVA, member 1 C8orf4 0.428 8p11.2 chromosome 8 open reading frame 4 DDC 0.427 7p12.2 dopa decarboxylase (aromatic L-amino acid decarboxylase) TACC2 0.427 10q26 transforming, acidic coiled-coil containing protein 2 MUC13 0.422 3q21.2 mucin 13, cell surface associated C5 0.412 9q33-q34 complement component 5 NR4A2 0.412 2q22-q23 nuclear receptor subfamily 4, group A, member 2 EYS 0.411 6q12 eyes shut homolog (Drosophila) GPX2 0.406 14q24.1 glutathione peroxidase -
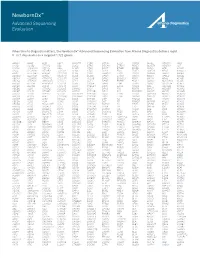
Cldn19 Clic2 Clmp Cln3
NewbornDx™ Advanced Sequencing Evaluation When time to diagnosis matters, the NewbornDx™ Advanced Sequencing Evaluation from Athena Diagnostics delivers rapid, 5- to 7-day results on a targeted 1,722-genes. A2ML1 ALAD ATM CAV1 CLDN19 CTNS DOCK7 ETFB FOXC2 GLUL HOXC13 JAK3 AAAS ALAS2 ATP1A2 CBL CLIC2 CTRC DOCK8 ETFDH FOXE1 GLYCTK HOXD13 JUP AARS2 ALDH18A1 ATP1A3 CBS CLMP CTSA DOK7 ETHE1 FOXE3 GM2A HPD KANK1 AASS ALDH1A2 ATP2B3 CC2D2A CLN3 CTSD DOLK EVC FOXF1 GMPPA HPGD K ANSL1 ABAT ALDH3A2 ATP5A1 CCDC103 CLN5 CTSK DPAGT1 EVC2 FOXG1 GMPPB HPRT1 KAT6B ABCA12 ALDH4A1 ATP5E CCDC114 CLN6 CUBN DPM1 EXOC4 FOXH1 GNA11 HPSE2 KCNA2 ABCA3 ALDH5A1 ATP6AP2 CCDC151 CLN8 CUL4B DPM2 EXOSC3 FOXI1 GNAI3 HRAS KCNB1 ABCA4 ALDH7A1 ATP6V0A2 CCDC22 CLP1 CUL7 DPM3 EXPH5 FOXL2 GNAO1 HSD17B10 KCND2 ABCB11 ALDOA ATP6V1B1 CCDC39 CLPB CXCR4 DPP6 EYA1 FOXP1 GNAS HSD17B4 KCNE1 ABCB4 ALDOB ATP7A CCDC40 CLPP CYB5R3 DPYD EZH2 FOXP2 GNE HSD3B2 KCNE2 ABCB6 ALG1 ATP8A2 CCDC65 CNNM2 CYC1 DPYS F10 FOXP3 GNMT HSD3B7 KCNH2 ABCB7 ALG11 ATP8B1 CCDC78 CNTN1 CYP11B1 DRC1 F11 FOXRED1 GNPAT HSPD1 KCNH5 ABCC2 ALG12 ATPAF2 CCDC8 CNTNAP1 CYP11B2 DSC2 F13A1 FRAS1 GNPTAB HSPG2 KCNJ10 ABCC8 ALG13 ATR CCDC88C CNTNAP2 CYP17A1 DSG1 F13B FREM1 GNPTG HUWE1 KCNJ11 ABCC9 ALG14 ATRX CCND2 COA5 CYP1B1 DSP F2 FREM2 GNS HYDIN KCNJ13 ABCD3 ALG2 AUH CCNO COG1 CYP24A1 DST F5 FRMD7 GORAB HYLS1 KCNJ2 ABCD4 ALG3 B3GALNT2 CCS COG4 CYP26C1 DSTYK F7 FTCD GP1BA IBA57 KCNJ5 ABHD5 ALG6 B3GAT3 CCT5 COG5 CYP27A1 DTNA F8 FTO GP1BB ICK KCNJ8 ACAD8 ALG8 B3GLCT CD151 COG6 CYP27B1 DUOX2 F9 FUCA1 GP6 ICOS KCNK3 ACAD9 ALG9 -

Lipid Deposition and Metabolism in Local and Modern Pig Breeds: a Review
animals Review Lipid Deposition and Metabolism in Local and Modern Pig Breeds: A Review Klavdija Poklukar 1 , Marjeta Candek-Potokarˇ 1,2 , Nina Batorek Lukaˇc 1 , Urška Tomažin 1 and Martin Škrlep 1,* 1 Agricultural Institute of Slovenia, Ljubljana SI-1000, Slovenia; [email protected] (K.P.); [email protected] (M.C.-P.);ˇ [email protected] (N.B.L.); [email protected] (U.T.) 2 University of Maribor, Faculty of Agriculture and Life Sciences, HoˇceSI-2311, Slovenia * Correspondence: [email protected]; Tel.: +386-(0)1-280-52-34 Received: 17 February 2020; Accepted: 29 February 2020; Published: 3 March 2020 Simple Summary: Intensive selective breeding and genetic improvement of relatively few pig breeds led to the abandonment of many low productive local pig breeds. However, local pig breeds are more highly adapted to their specific environmental conditions and feeding resources, and therefore present a valuable genetic resource. They are able to deposit more fat and have a distinct lipogenic capacity, along with a better fatty acid composition than modern breeds. Physiological, biochemical and genetic mechanisms responsible for the differences between fatty and lean breeds are still not fully clarified. The present paper highlights important associations to better understand the underlying mechanisms of lipid deposition in subcutaneous and intramuscular fat between fatty and lean breeds. Abstract: Modern pig breeds, which have been genetically improved to achieve fast growth and a lean meat deposition, differ from local pig breeds with respect to fat deposition, fat specific metabolic characteristics and various other properties. The present review aimed to elucidate the mechanisms underlying the differences between fatty local and modern lean pig breeds in adipose tissue deposition and lipid metabolism, taking into consideration morphological, cellular, biochemical, transcriptomic and proteomic perspectives. -

Mouse Model of GM2 Activator Deficiency Manifests Cerebellar Pathology and Motor Impairment
Proc. Natl. Acad. Sci. USA Vol. 94, pp. 8138–8143, July 1997 Medical Sciences Mouse model of GM2 activator deficiency manifests cerebellar pathology and motor impairment (animal modelyGM2 gangliosidosisygene targetingylysosomal storage disease) YUJING LIU*, ALEXANDER HOFFMANN†,ALEXANDER GRINBERG‡,HEINER WESTPHAL‡,MICHAEL P. MCDONALD§, KATHERINE M. MILLER§,JACQUELINE N. CRAWLEY§,KONRAD SANDHOFF†,KINUKO SUZUKI¶, AND RICHARD L. PROIA* *Section on Biochemical Genetics, Genetics and Biochemistry Branch, National Institute of Diabetes and Digestive and Kidney Diseases, ‡Laboratory of Mammalian Genes and Development, National Institute of Child Health and Development, and §Section on Behavioral Neuropharmacology, Experimental Therapeutics Branch, National Institute of Mental Health, National Institutes of Health, Bethesda, MD 20892; †Institut fu¨r Oganische Chemie und Biochemie der Universita¨tBonn, Gerhard-Domagk-Strasse 1, 53121 Bonn, Germany; and ¶Department of Pathology and Laboratory Medicine, and Neuroscience Center, University of North Carolina, Chapel Hill, NC 27599 Communicated by Stuart A. Kornfeld, Washington University School of Medicine, St. Louis, MO, May 12, 1997 (received for review March 21, 1997) ABSTRACT The GM2 activator deficiency (also known as disorder, the respective genetic lesion results in impairment of the AB variant), Tay–Sachs disease, and Sandhoff disease are the the degradation of GM2 ganglioside and related substrates. major forms of the GM2 gangliosidoses, disorders caused by In humans, in vivo GM2 ganglioside degradation requires the defective degradation of GM2 ganglioside. Tay–Sachs and Sand- GM2 activator protein to form a complex with GM2 ganglioside. hoff diseases are caused by mutations in the genes (HEXA and b-Hexosaminidase A then is able to interact with the activator- HEXB) encoding the subunits of b-hexosaminidase A. -

Ion Channels
UC Davis UC Davis Previously Published Works Title THE CONCISE GUIDE TO PHARMACOLOGY 2019/20: Ion channels. Permalink https://escholarship.org/uc/item/1442g5hg Journal British journal of pharmacology, 176 Suppl 1(S1) ISSN 0007-1188 Authors Alexander, Stephen PH Mathie, Alistair Peters, John A et al. Publication Date 2019-12-01 DOI 10.1111/bph.14749 License https://creativecommons.org/licenses/by/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California S.P.H. Alexander et al. The Concise Guide to PHARMACOLOGY 2019/20: Ion channels. British Journal of Pharmacology (2019) 176, S142–S228 THE CONCISE GUIDE TO PHARMACOLOGY 2019/20: Ion channels Stephen PH Alexander1 , Alistair Mathie2 ,JohnAPeters3 , Emma L Veale2 , Jörg Striessnig4 , Eamonn Kelly5, Jane F Armstrong6 , Elena Faccenda6 ,SimonDHarding6 ,AdamJPawson6 , Joanna L Sharman6 , Christopher Southan6 , Jamie A Davies6 and CGTP Collaborators 1School of Life Sciences, University of Nottingham Medical School, Nottingham, NG7 2UH, UK 2Medway School of Pharmacy, The Universities of Greenwich and Kent at Medway, Anson Building, Central Avenue, Chatham Maritime, Chatham, Kent, ME4 4TB, UK 3Neuroscience Division, Medical Education Institute, Ninewells Hospital and Medical School, University of Dundee, Dundee, DD1 9SY, UK 4Pharmacology and Toxicology, Institute of Pharmacy, University of Innsbruck, A-6020 Innsbruck, Austria 5School of Physiology, Pharmacology and Neuroscience, University of Bristol, Bristol, BS8 1TD, UK 6Centre for Discovery Brain Science, University of Edinburgh, Edinburgh, EH8 9XD, UK Abstract The Concise Guide to PHARMACOLOGY 2019/20 is the fourth in this series of biennial publications. The Concise Guide provides concise overviews of the key properties of nearly 1800 human drug targets with an emphasis on selective pharmacology (where available), plus links to the open access knowledgebase source of drug targets and their ligands (www.guidetopharmacology.org), which provides more detailed views of target and ligand properties. -

ASAH1 Variant Causing a Mild SMA Phenotype with No Myoclonic Epilepsy: a Clinical, Biochemical and Molecular Study
European Journal of Human Genetics (2016) 24, 1578–1583 & 2016 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 1018-4813/16 www.nature.com/ejhg ARTICLE ASAH1 variant causing a mild SMA phenotype with no myoclonic epilepsy: a clinical, biochemical and molecular study Massimiliano Filosto*,1, Massimo Aureli2, Barbara Castellotti3, Fabrizio Rinaldi1, Domitilla Schiumarini2, Manuela Valsecchi2, Susanna Lualdi4, Raffaella Mazzotti4, Viviana Pensato3, Silvia Rota1, Cinzia Gellera3, Mirella Filocamo4 and Alessandro Padovani1 ASAH1 gene encodes for acid ceramidase that is involved in the degradation of ceramide into sphingosine and free fatty acids within lysosomes. ASAH1 variants cause both the severe and early-onset Farber disease and rare cases of spinal muscular atrophy (SMA) with progressive myoclonic epilepsy (SMA-PME), phenotypically characterized by childhood onset of proximal muscle weakness and atrophy due to spinal motor neuron degeneration followed by occurrence of severe and intractable myoclonic seizures and death in the teenage years. We studied two subjects, a 30-year-old pregnant woman and her 17-year-old sister, affected with a very slowly progressive non-5q SMA since childhood. No history of seizures or myoclonus has been reported and EEG was unremarkable. The molecular study of ASAH1 gene showed the presence of the homozygote nucleotide variation c.124A4G (r.124a4g) that causes the amino acid substitution p.Thr42Ala. Biochemical evaluation of cultured fibroblasts showed both reduction in ceramidase activity and accumulation of ceramide compared with the normal control. This study describes for the first time the association between ASAH1 variants and an adult SMA phenotype with no myoclonic epilepsy nor death in early age, thus expanding the phenotypic spectrum of ASAH1-related SMA.