CODA.Org: Accreditation Standards for Pediatric Dentistry
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Scientific Article
Scientific Article Prosthodontic and surgical considerations for pediatric patients requiring maxillectomy Jack W. Martin, DDS, MS Mark S. Chambers, DMD, MS James C. Lemon, DDS Bela B. Toth, MS, DDS John F. Helfrick, DDS, MS Abstract head and neck tumors of the maxillofacial region. In The quality of treatment and rehabilitation for the head such diseases, the principal treatment option is surgi- and neck cancer patient, especially the pediatric patient, cal resection of the maxilla (maxillectomy), which may has progressed markedly over the years due to the coopera- produce pronounced deficits and cosmetic deformi- tion of specialists involved in the total care of the patient. ties. Consequently, when a maxillectomy is required Defects of the oral cavity caused by trauma or removal of for treating benign or malignant disease, the maxillofa- malignant or benign tissue require special treatment con- cial prosthodontist must be included in the assessment siderations with the pediatric patient. Aside from radiation of the patient prior to surgery. Many articles describe and chemotherapy, other forms of adjuvant therapy, such the surgical and prosthodontic management of the adult as physical therapy, and patient and family counseling, are maxillectomy patient, but little information exists about needed for proper rehabilitation. In addition, oral hygiene management of the pediatric maxillectomy patient. This is essential in the overall rehabilitative process. Pediatric article discusses preoperative evaluation, and surgical dental, orthodontic, prosthodontic, and oral and maxillofa- and prosthodontic considerations of children diagnosed cial surgery specialties become integrated in treating the with maxillary cancer or benign disease. Postsurgical pediatricpatient. The concentrated multidisciplinary treat- care and growth considerations also are presented. -

Pediatric Clerkship Manual Se Campus-Fargo
PEDIATRIC CLERKSHIP MANUAL SE CAMPUS-FARGO 1 | P a g e Table of Contents Curriculum and Objectives 3 Introduction-Inpatient, Outpatient, Subsp. Clinic, NNN, CTC 4 Pediatric Clerkship Requirements 9 Inpatient H&P Outline 10 Inpatient Progress Note Outline 17 Outpatient Write-Up Outline 19 Oral Case Primer 21 Oral Case Template 33 Professor Rounds – OPCRS Rating For m 35 Midclerkship Feedback 39 Aquifer Pediatrics/Radiology (CLIPP/CORE) Cases 40 Pediatric Grand Rounds 40 Grading Policy and Honors Designation Guidelines 42 2 | P a g e PEDIATRIC CLERKSHIP UND SCHOOL OF MEDICINE AND HEALTH SCIENCES SOUTHEAST CAMPUS – FARGO Welcome to the 3rd year Pediatric Clerkship where “The care of children is the finest privilege!” We hope that your eight-week experience in Pediatrics will provide you with a broad and exciting introduction to the care of infants, children, and adolescents. While rotating through Pediatrics, you will have the opportunity to work as part of a team comprised of community attending physicians, nurses, and paramedical personnel. Our commitment to you: The faculty of the Southeast Campus is composed of volunteer faculty pediatricians under the leadership of Dr. Chris DeCock, pediatric clerkship director. You will be provided prompt feedback to ensure you to optimize your learning experience on Pediatrics. We expect that as third year medical students you come to the Pediatric Clerkship prepared to give 100% to each patient encounter. We also expect you will conduct yourself in a professional manner. If you have any concerns or problems during your rotation feel free to contact Dr. Chris DeCock, pediatric clerkship director or Kathy Kraft, clerkship coordinator. -

Clinical Pharmacists' Role in Paediatric Patients' Medical Care
International Journal of Contemporary Pediatrics Balakrishnan RP et al. Int J Contemp Pediatr. 2020 Dec;7(12):2416-2420 http://www.ijpediatrics.com pISSN 2349-3283 | eISSN 2349-3291 DOI: https://dx.doi.org/10.18203/2349-3291.ijcp20205110 Review Article Clinical pharmacists’ role in paediatric patients’ medical care Raveena Pachal Balakrishnan1*, Rajganesh Ravichandran1, Jaya Shree Dillibatcha1, Abrana Lakshmi Ravi1, Nikhil Cherian Sam1, Ramya Nuthalapati2 1Department of Pharmacy Practice, C. L. Baid Metha college of Pharmacy, The Tamil Nadu Dr. M. G. R. Medical University, Chennai, Tamil Nadu, India 2Clinical Pharmacist, Gleneagles Global Health City, Perumbakkam, Chennai Tamil Nadu, India Received: 11 October 2020 Accepted: 13 November 2020 *Correspondence: Dr, Raveena Pachal Balakrishnan, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Clinical pharmacists give valuable administrations to adult patients, however, their advantages for pediatric and neonatal patients are less characterized. Many studies state that medication errors in children are more common than in adults with a greater risk of death.Clinical Pharmacists are accepted as the primary source for providing evidence-based information and advice, to ensure the delivery of correct, safest, and most effective medication to patients. This paper presents a review of the role of clinical pharmacists in the pediatric unit and emphasis the importance of clinical pharmacists for all patients, especially in the pediatric age group. -

Pediatrics Community About the Residency Recruitment Process May 19, 2021
APPD/COMSEP/AMSPDC/FuturePedsRes/NextGenPediatricians Letter to Our Pediatrics Community About the Residency Recruitment Process May 19, 2021 The leadership of APPD, COMSEP, AMSPDC, FuturePedsRes, and NextGenPediatricians have been working collaboratively with Undergraduate Medical Education (UME) and Graduate Medical Education (GME) leaders and learners to optimize the recruitment process for applicants and programs. Through this process, we have sought substantial input from applicants, program leaders, chairs, and the greater community including other subspecialties. In addition, we have reviewed and appreciate the recommendations from the Coalition for Physician Accountability. Our primary goal is to optimize the recruitment process for both learners and programs by: (1) Helping learners find programs that match their career goals while providing an atmosphere conducive to their learning styles. (2) Creating a fair and equitable application process for both learners and programs. This past interview season has opened our eyes to ways of improving equity in our processes. In addition, there continues to be uncertainty due to the COVID‐19 pandemic, with some regions still experiencing surges and travel restrictions. Given that many are most focused on the types of interviews we will be doing this coming year, we present that recommendation up front, and then go into the additional recommendations below. Following many conversations and surveys with each of our organizations, we strongly recommend only offering virtual interviews for the 2021‐2022 recruitment cycle for several reasons: (1) Effective assessment: The majority of applicants and programs highlighted that they thought the assessment of applicants was sufficient using virtual interviews in the 2020‐ 2021 cycle. (2) Equity: Virtual interviews are more equitable for applicants and programs, both in terms of cost savings and in terms of any remaining restrictions from the COVID‐19 pandemic. -

Former General Pediatrics Fellows
Former General Pediatrics Fellows Alumni, 2007–2017 2007 Name: Copeland-Linder, Nikeea Prior Training: PhD (Psychology), University of Michigan Years In Program: 2005-2007 Mentors: Tina Cheng, Nick Lalongo Research Area: Youth violence prevention, child stress and mental health Current Position: Child psychologist, Ellicott City 2008 Name: Garg, Arvin Prior Training: MD: Boston University School of Medicine; MPH: Boston University School of Public Health; Pediatric Residency: Univ. of Connecticut School of Medicine Years In Program: 2004-2008 Mentors: Janet Serwint, Arlene Butz Research Area: Addressing social determinants of health within pediatric primary care Associate Professor, Boston University School of Medicine; Associate Director Current Position: of Medical Student Education for Pediatrics Name: Kuo, Dennis Prior Training: MD: University of Pennsylvania; Pediatric Residency, University of North Years In Program: Carolina Degrees Earned: 2005-2008 Mentors: MHS, Johns Hopkins University Bloomberg School of Public Health Research Area: Cynthia Minkovitz Current Position: Associate Professor and Chief, General Pediatrics, University at Buffalo, and Medical Director of Primary Care Services at Women & Children‘s Hospital of Buffalo 2009 Name: Dodge, Rachel Prior Training: MD: University of Maryland; Pediatric Residency: Rainbow Babies and Children’s Hospital, Cleveland, OH Years In Program: 2005-2009 Degrees Earned: MPH: Johns Hopkins University Bloomberg School of Public Health Mentors: Anne Duggan, Tina Cheng, Tracy King, Megan Bair-Merritt Research Area: Primary care based interventions to promote positive parenting Current Position: Pediatrician, Dundalk Pediatric Association (Johns Hopkins Medicine) Name: Murray, Kantahyaneee Prior Training: PhD (Public Health): University of Maryland Years In Program: 2007-9 Mentors: Tina Cheng, Megan Bair-Merritt Research Area: Role of primary care in youth violence prevention Current Position: Senior Research Associate, Annie E. -

A Pediatric Role in Enhancing Development in Young Children
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Power of Play: A Pediatric Michael Yogman, MD, FAAP,a Andrew Garner, MD, PhD, FAAP, b Jeffrey Hutchinson, MD, FAAP, c RoleKathy Hirsh-Pasek, in PhD, Enhancing d Roberta Michnick Golinkoff, PhD, Development e COMMITTEE ON PSYCHOSOCIAL inASPECTS Young OF CHILD AND FAMILY Children HEALTH, COUNCIL ON COMMUNICATIONS AND MEDIA Children need to develop a variety of skill sets to optimize their development abstract and manage toxic stress. Research demonstrates that developmentally appropriate play with parents and peers is a singular opportunity to promote the social-emotional, cognitive, language, and self-regulation skills that build executive function and a prosocial brain. Furthermore, play aDepartment of Pediatrics, Harvard Medical School, Harvard University and Mount Auburn Hospital, Cambridge, Massachusetts; bDepartment supports the formation of the safe, stable, and nurturing relationships with of Pediatrics, School of Medicine, Case Western Reserve University and University Hospitals Medical Practices, Cleveland, Ohio; cDepartment all caregivers that children need to thrive. of Pediatrics, F. Edward Hebert School of Medicine, Uniformed Services University, Bethesda, Maryland; dDepartment of Psychology, Brookings Play is not frivolous: it enhances brain structure and function and promotes Institution and Temple University, Philadelphia, Pennsylvania; and executive function (ie, the process of learning, rather than the content), eSchool of Education, University -

36 Dept .Of Pediatrics, "Obstetrics and Phillpps -University ,355 Marburg/L. ,FRG &I. KIM C M (9) 11
T.M.Strom*, J. Weil*, A. Timnic*, D. Knorr, C.G.D.Brook F..A.~ivese~': F. Bidlingmaier 38 The Middlesex Hospit~l,Mortimer Street, London W1. Depart. of Paediatrics, University of Munich and CROW'LII AND CROWD1 IIOIIMONE (CII) TRMTMENT FOI.I.OIIING IUUlOTIICIL$PY 35 Institute of Clinical Biochemistry, University of Bonn OF BRAIN TUEIOURS. FRGl EIND~NCSITES FOR ATRIAL NATRlURETlC PEPTIDE Of a cohort of 132 children .,live and well following treatment of brain (ANP) ON PLATELETS IN PATIENTS WITH HIGH tumours renlote from the hypothalasus or pituitaly with radrotherapy, 96% tiad PLASMA ANP LEVELS. evidence of GI1 abnornwlity. 32 had campleLctl their Growth. 14 who had received craniospinal irradiation, had final height SDS -2.03 (range, -3.7 to +O.O9), In our first study we found binding sites for ANP on human sitting height (SH) SbS -3.22 and subischinl leg letlgtl; (SILL) SDS -0.61. 18 platelets. Binding studies on these easily accessible cells could treated with cranial irradiation aloac liad final height SDS -0.93 (range, -7.6 be a useful model to investigate receptor-status in patients with to +2.07), SH SUS -1.24 and ST1.L SDS -0.53. llius the crfect of spin.il elevated ANP plasma levels. We reported high ANP levels in irradiation on final height was considerable. neonates and in patients with heartfailure. Therefore we studied 40 children were treated with GH for periods of 1-4 years. 32 had the number of binding sites on platelets in venous umbilical blood received craniospinal irradiation and 8 cranial irradiation alone. -

Medical Terminology Abbreviations Medical Terminology Abbreviations
34 MEDICAL TERMINOLOGY ABBREVIATIONS MEDICAL TERMINOLOGY ABBREVIATIONS The following list contains some of the most common abbreviations found in medical records. Please note that in medical terminology, the capitalization of letters bears significance as to the meaning of certain terms, and is often used to distinguish terms with similar acronyms. @—at A & P—anatomy and physiology ab—abortion abd—abdominal ABG—arterial blood gas a.c.—before meals ac & cl—acetest and clinitest ACLS—advanced cardiac life support AD—right ear ADL—activities of daily living ad lib—as desired adm—admission afeb—afebrile, no fever AFB—acid-fast bacillus AKA—above the knee alb—albumin alt dieb—alternate days (every other day) am—morning AMA—against medical advice amal—amalgam amb—ambulate, walk AMI—acute myocardial infarction amt—amount ANS—automatic nervous system ant—anterior AOx3—alert and oriented to person, time, and place Ap—apical AP—apical pulse approx—approximately aq—aqueous ARDS—acute respiratory distress syndrome AS—left ear ASA—aspirin asap (ASAP)—as soon as possible as tol—as tolerated ATD—admission, transfer, discharge AU—both ears Ax—axillary BE—barium enema bid—twice a day bil, bilateral—both sides BK—below knee BKA—below the knee amputation bl—blood bl wk—blood work BLS—basic life support BM—bowel movement BOW—bag of waters B/P—blood pressure bpm—beats per minute BR—bed rest MEDICAL TERMINOLOGY ABBREVIATIONS 35 BRP—bathroom privileges BS—breath sounds BSI—body substance isolation BSO—bilateral salpingo-oophorectomy BUN—blood, urea, nitrogen -

Osseointegrated Dental Implants As Alternative Therapy to Bridge
SCIENTIFIC ARTICLE Osseointegrateddental implants as alternative therapy to bridge construction or orthodonticsin youngpatients: sevenyears of clinical experience Philippe D. Ledermann,DDS Thomas M. Hassell, DDS,PhD Arthur F. Hefti, DDS,PD Abstract Youngpatients often require fixed bridgeworkor orthodontictherapy in cases of traumatic tooth loss or congenitally missing teeth. Dentalimplants represent an alternative to the moreconventional treatment methods.We report positive experienceover a seven-year period with 42 titanium Ha-Ti implants in 34 patients aged 9 to 18 years. Fourteen implants were placed into preparedtooth sockets immediatelyafter traumatic luxation of anterior teeth in 12 patients aged9 to 18 years (medianage 16). Anadditional 22 patients (medianage 15.5, range 11 to 18) also received implants (N = 28), but these wereplaced only after healing of extraction sites, or as substitutes for congenitally missing teeth. Implants remainedin situ for an averageof 7.7 monthsbefore loading. Duringthe healing period, three implants were lost due to additional traumaand one becameinfected. The 38 remainingimplants osseointegrated and since have been loaded for five to 79 monthsin successful function. There was no difference between immediateand delayed implants in clinical success. These experiences demonstratethat appropriate, versatile, osseointegrated implants can provide a successful treatment methodfor youngpatients, without damagingadjacent teeth. (Pediatr Dent 15:327-33, 1993) Introduction Edentulous spaces often exist in children -

ACT Early Milestone Moments
Milestone Moments Learn the Signs. Act Early. Learn the Signs. Act Early. www.cdc.gov/milestones 1-800-CDC-INFO Adapted from CARING FOR YOUR BABY AND YOUNG CHILD: BIRTH TO AGE 5, Fifth Edition, edited by Steven Shelov and Tanya Remer Altmann © 1991, 1993, 1998, 2004, 2009 by the American Academy of Pediatrics and You can follow your child’s development by watching how he or BRIGHT FUTURES: GUIDELINES FOR HEALTH SUPERVISION OF INFANTS, CHILDREN, AND ADOLESCENTS, Third she plays, learns, speaks, and acts. Edition, edited by Joseph Hagan, Jr., Judith S. Shaw, and Paula M. Duncan, 2008, Elk Grove Village, IL: American Academy of Pediatrics. Special acknowledgements to Susan P. Berger, PhD; Jenny Burt, PhD; Margaret Greco, MD; Katie Green, MPH, Look inside for milestones to watch for in your child and how you CHES; Georgina Peacock, MD, MPH; Lara Robinson, PhD, MPH; Camille Smith, MS, EdS; Julia Whitney, BS; and can help your child learn and grow. Rebecca Wolf, MA. Centers for Disease Centers for Disease Control and Prevention Control and Prevention www.cdc.gov/milestones www.cdc.gov/milestones 1-800-CDC-INFO 1-800-CDC-INFO 220788 Milestone Moments How your child plays, learns, speaks, and acts offers important clues about your child’s development. Developmental milestones are things most children can do by a certain age. The lists that follow have milestones to look for when your child is: 2 Months ............................................................... page 3 – 6 Check the milestones your child has reached at each age. 4 Months ............................................................... page 7 –10 Take this with you and talk with your child’s doctor at every visit about the milestones your child has reached and what to 6 Months .............................................................. -

Pediatric and Orthodontic Dental Specialists
Top 10 Things You Must Know Before Choosing Your Pediatric And Orthodontic Dental Specialists Roxbury Orthodontics & Pediatric Dentistry The Top 10 Things You Must Know Before Choosing Your Dental Care Provider! Welcome Letter from Your Pediatric and Orthodontic Dental Specialty Team Dear Friend, If you are researching orthodontists and pediatric dentists for yourself or your child, then you are in the right place! You should know that just like all teeth are different, every dental care practice is different, too. In your search to find the right provider for your family, you will most likely find similar treatment options. It’s important to know, however, that all treatment is not the same. At Roxbury Orthodontics & Pediatric Dentistry, our mission is to serve others by changing lives, supporting our community, and taking a patient-centric approach to care. Our team works hard to offer the highest quality care in a friendly, comforta-ble, environment. With our “patient-first” approach, our biggest reward is seeing how happy our patients are with their new smiles after treatment. To help support our mission and to help you choose the right practice, we invite you to read our report, “The Top 10 Things You Must Know Before Choosing Your Dental Care Provider” Each section addresses an important question to consider as you research options for your and your family’s treatment. While many providers fit a few of the criteria, I strongly encourage you to settle for nothing less than the complete package. It’s what you and your teeth deserve! We hope you find our report to be informative and helpful as you begin your exciting journey toward your ideal, healthy smile. -
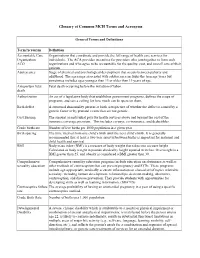
Glossary of Common MCH Terms and Acronyms
Glossary of Common MCH Terms and Acronyms General Terms and Definitions Term/Acronym Definition Accountable Care Organizations that coordinate and provide the full range of health care services for Organization individuals. The ACA provides incentives for providers who join together to form such ACO organizations and who agree to be accountable for the quality, cost, and overall care of their patients. Adolescence Stage of physical and psychological development that occurs between puberty and adulthood. The age range associated with adolescence includes the teen age years but sometimes includes ages younger than 13 or older than 19 years of age. Antepartum fetal Fetal death occurring before the initiation of labor. death Authorization An act of a legislative body that establishes government programs, defines the scope of programs, and sets a ceiling for how much can be spent on them. Birth defect A structural abnormality present at birth, irrespective of whether the defect is caused by a genetic factor or by prenatal events that are not genetic. Cost Sharing The amount an individual pays for health services above and beyond the cost of the insurance coverage premium. This includes co-pays, co-insurance, and deductibles. Crude birth rate Number of live births per 1000 population in a given year. Birth spacing The time interval from one child’s birth until the next child’s birth. It is generally recommended that at least a two-year interval between births is important for maternal and child health and survival. BMI Body mass index (BMI) is a measure of body weight that takes into account height.